Introduction. The basic guidelines provide the diagnosis of most anomalies or at least help the examiner observe there is something wrong and refer the case to a specialised unit. Fetal neurosonography is a complex examination that needs time and making it routinely in a complete form (with multiple coronal and sagittal sections) may not be cost-efficient. We analyzed if some elements of advanced neurosonography, together with color Doppler, would improve the examination, increase the diagnostic rate and decrease the referred case percentage, but also if they are feasible or prolong the examination time with minimal benefits. Materials and method. The new parameters used in our protocol were: sagittal image with the corpus callosum and vermis; color Doppler evaluation on a median approach with the pericallosal artery and Galen’s vein, and an axial approach with the circle of Willis, targeting the evaluation of vascular anomalies; acquiring a 3D volume of the fetal head for diagnostic purposes, but also for storing in a “3D volumes library”. Result. After the evaluation of 763 cases, we noticed an extension of the examination of about three minutes, and the target was achieved in over 90% of the cases, the most difficult being the vascular median view. The use of new techniques helped us demonstrate more anomalies or anatomic variants, among which a Galen’s vein aneurysm, and also offered the possibility of using the 3D volume library and offline examination for retrospective evaluation of certain cases. Conclusions. We believe that the new parameters had a good feasibility, they did not prolong the examination time, and brought new and more precise diagnosis. The benefits for the pathological cases were proved by the cases reported. Also, the existence of an ultrasound volume data base allows retrospective evaluation of cases and allows for new, sometimes better images, for later in pregnancy or even postnatally.
Extinderea examinării standard a sistemului nervos central fetal la ecografia de trimestrele doi şi trei
Extending the basic fetal CNS examination at the second and third trimester scan
First published: 21 mai 2019
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Gine.24.2.2019.2368
Abstract
Rezumat
Introducere. Protocolul de bază asigură diagnosticarea majorităţii anomaliilor sau cel puţin sesizarea prezenţei unei anormalităţi şi direcţionarea cazului către un for superior. Neurosonografia fetală este o examinare complexă care necesită timp şi introducerea ei în forma completă ar putea să nu fie considerată cost-eficientă. Am analizat modul în care introducerea unor secţiuni din protocolul extins recomandat de ISUOG ar îmbunătăţi calitatea examinării, ar creşte rata diagnosticelor şi rapiditatea formulării lor, dar şi măsura în care acestea sunt fezabile sau prelungesc timpul de examinare, cu beneficii minime. Materiale şi metodă. Parametrii noi introduşi au fost: a) secţiune sagitală – corp calos, vermis; b) evaluare Doppler color pe secţiune sagitală şi axială în scopul diagnosticului anomaliilor vasculare cerebrale; c) obţinerea unor volume 3D ale capului atât în scop diagnostic, cât şi în scopul realizării unei „biblioteci” de volume pentru evaluarea retrospectivă a cazurilor. Rezultate. În urma evaluării a 763 de cazuri am observat o prelungire a timpului de examinare cu aproximativ trei minute, iar targetul a fost atins în peste 90% din cazuri, cea mai dificilă fiind evaluarea vasculară sagitală. Adoptarea noilor tehnici ne-a ajutat să punem în evidenţă mai multe anomalii sau variante anatomice ale SNC, printre care un anevrism de venă Galen, dar şi evaluarea retrospectivă a cazurilor cu probleme, utilizând biblioteca de volume şi tehnici de evaluare offline. Concluzii. Considerăm că metodele adiţionale au avut o fezabilitate bună, nu au prelungit timpul de examinare şi au asigurat diagnostice suplimentare. Aportul adus în cazurile patologice a fost demonstrat de cazurile prezentate. De asemenea, existenţa unei baze de date de volume asigură evaluarea retrospectivă a cazurilor şi permite obţinerea de imagini noi, mai relevante, acolo unde se suspectează ceva ulterior în sarcină sau chiar postnatal.
Introduction
The basic protocol for central nervous system (CNS) evaluation recommended by ISUOG (for mid trimester) includes intact cranium, cavum septum pelucidum, midline falx, thalami, cerebral ventricles, cerebelum, and cisterna magna(1). In our unit, we use an ISUOG-based protocol illustrated in Table 1 and Table 2. This standardized examination assures the diagnosis of most anomalies or at least allows to observe if there is something wrong and refer the case to a specialised unit. Fetal neurosonography is a complex examination that needs time and making it routinely in a complete form (with multiple coronal and sagittal views) may not be cost-efficient. We analyzed if some elements of advanced neurosonography, together with color Doppler, would improve the examination, increase the diagnostic rate and decrease the referred cases percentage, but also if they are feasible or prolong the examination time with minimal benefits. We also analyzed the opportunity of acquiring 3D volumes of the fetal head. The study took place from July 2017 to July 2018, on 763 cases of second and third trimester pregnancies (465 cases of second trimester pregnancies, with an average gestational age of 22 weeks + 1 day, and 298 third trimester cases, with an average gestational age of 32 weeks + 3 days).


Materials and method
The new parameters used in our protocol were:
-
Sagittal image with the corpus callosum and vermis.
-
Color Doppler evaluation on a median approach with the pericallosal artery and Galen’s vein and on an axial approach with the circle of Willis, targeting the evaluation of vascular anomalies.
-
Acquiring a 3D volume of the fetal head for diagnostic purposes, but also for storing in a “3D volumes library”.
All the examinations were performed on a Voluson E8 expert ultrasound machine (GE Healthcare, Kretz Ultrasound, Zipf, Austria), using a RAB 6D 3D abdominal probe and a RIC 5-9D 3D transvaginal probe; the images were obtained transabdominally or transvaginally (if necessary and possible). Sometimes, sagittal images were obtained from a 3D volume, when 2D direct visualization was not possible. The settings for color Doppler were done as recommended in previous studies(2,3), using a PRF (pulse repetition frequency) of 2 to 4 MHz for routine examinations – however, in certain situations, we used a PRF as low as 0.6 MHz. The settings for second trimester volumes were made to a high 2D quality with an average angle of 50 (with a small variability according to gestational age). For the third trimester we chose a 70-degree angle with an image quality of max 1 or higher (if the fetus was still for enough period of time). We would like to mention that for the third trimester scan we used a special setting of the 2D with the specle reduction imaging (SRI) and the compound imaging (CRI) at level 1 and the dinamic contrast at level 4, for a better highlighting of the details of the cerebral tissue
Results and discussion
We analyzed four aspects of the utility of our methods: feasibility, the extra examination time needed, special cases in which the new parameters used were helpful, the need for a 3D volume data base.
Feasibility: we analyzed if the parameters were easy to obtain. Data shows (Table 3) that the parameters were obtained in over 90% of cases.
The extra examination time needed: we analyzed how much each examination took with or without the new parameters. This was evaluated separately for the second and third trimester scans, with an average of 41 minutes for every second trimester scan and 24 minutes for every third trimester scan – an extra 3 minutes for each type of examination compared to standard examinations.
Special cases in which the new parameters used were helpful
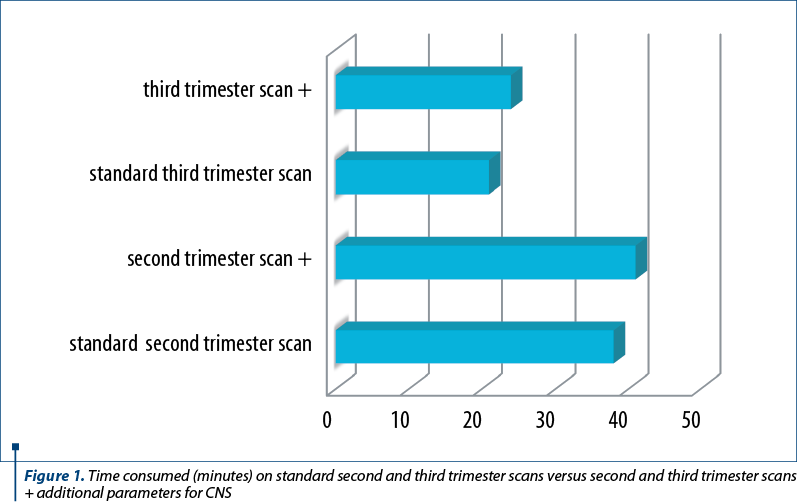
Case 1: Galen’s vein aneurysm
Galen’s vein aneurysm is a rare arteriovenous malformation that results from the abnormal communication between Galen’s venous sinus and branches of different cerebral arteries. It is associated with heart failure due to increased preload and may associate hydrocephaly due to compression of the aqueduct of Silvius(4,5). It is noticed on 2D ultrasound as a cyst-like structure and should be differentiated from other types of lesion such as arachnoid cysts, porencephaly, and cerebral hematomas. The use of color Doppler allows the visualization of a turbulent vascular flow (Figure 2). Due to the rare nature of the disease, there is no standard treatment protocol. There is, however, a consensus regarding the need for prenatal and/or postnatal MRI and the use of embolization as a first line of treatment(6), with good results on limited series. The patient was referred for a third trimester scan at 32 weeks for the suspicion of an arachnoid cyst – the use of color Doppler as part of our new screening protocol allowed a fast diagnosis of the cerebral malformation.
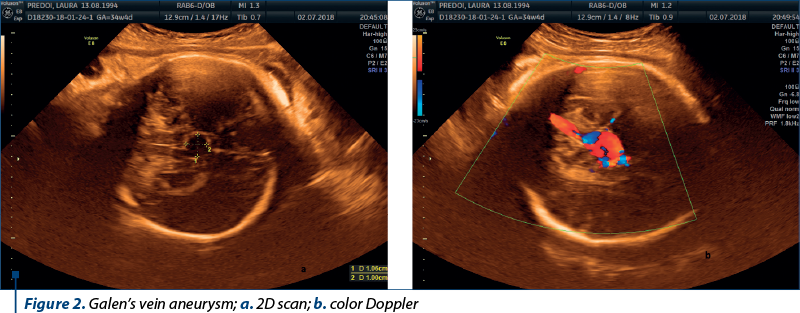
Case 2. Agenesis of the corpus callosum
Agenesis of the corpus callosum is the complete absence of the corpus callosum and has a prevalence of 1.4/10000 births. The diagnosis is based on direct and indirect signs that include the absence of the cavum septum pellucidi, abnormalities of the ventricles (colpocephaly), abnormal trajectory of the pericallosal artery, widening of the interhemispheric fissure, and radial disposition of the sulci on the internal side of the hemispheres(7). Our case was diagnosed at 22 weeks, after normal first trimester screening. The examination revealed the typical signs on axial images, but the definitive diagnosis was made on the sagittal scan, with the demonstration of an absent corpus callosum and an abnormal arterial disposition – only the anterior cerebral artery was seen, with branches ascending linearly. The patient opted for the termination of pregnancy; the karyotyping was normal.
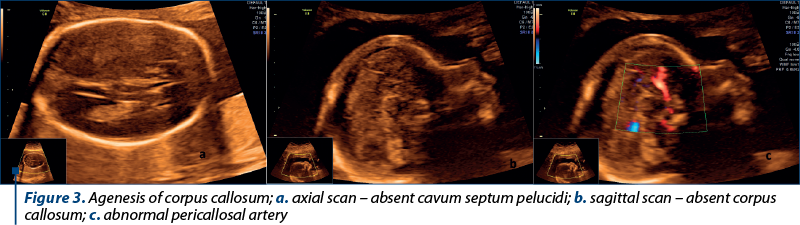
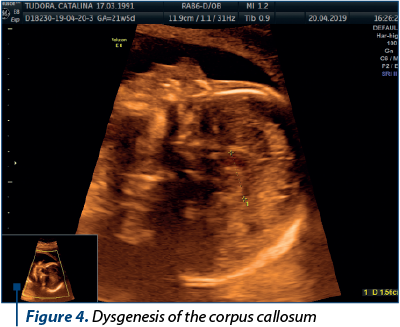
Case 3. Dysgenesis of the corpus callosum
The terminology of the corpus callosum pathology holds a wide spectrum. The dysgenesis of the corpus callosum, in the sense of incomplete development, covers partial agenesis and hypoplasia(8). The size of the corpus callosum can be measured from existing nomograms(9,10). The prognosis is unknown due to the limited number of cases reported. The association with genetic disease has been described(11). The case was referred to our unit for absent cavum septum pellucidi. The sagittal scan revealed a small corpus callosum – 15.1 mm to 17.1 mm on different measurements, compared to the normal range of 21.66-24.74 mm (95% CI). We recommended fetal MRI, karyotyping and microarray analysis. Unfortunately, the patient was lost from the follow-up.

Case 4: Abnormal trajectory of the pericallosal artery
Aberrant pericallosal artery has been described as part of the agenesis of the corpus callosum (partial or complete). However, due to the routine use of color Doppler, we found a case with a normal corpus callosum (size, thickness and normal dynamic throughout the pregnancy) with an aberrant pericallosal artery. We attributed it to a small lipoma adjacent to the corpus callosum and we counselled the patient to have a fetal MRI, but the patient decided not to do it. Since the case was at the beginning of our study, we have information from birth and postnatal follow-up. The patient gave birth to a 3420 g baby, with an Apgar score of 9, 9 and 10 at 1, 3 and 5 minutes, respectively. No neurological signs or seizures were registered in the third day of staying in the neonatal department. The 3-month and the 6-month evaluations revealed normal neuromotor development; no seizures or any abnormal signs were noticed.
Case 5. Cavum velum interpositi (normal variant/cyst)
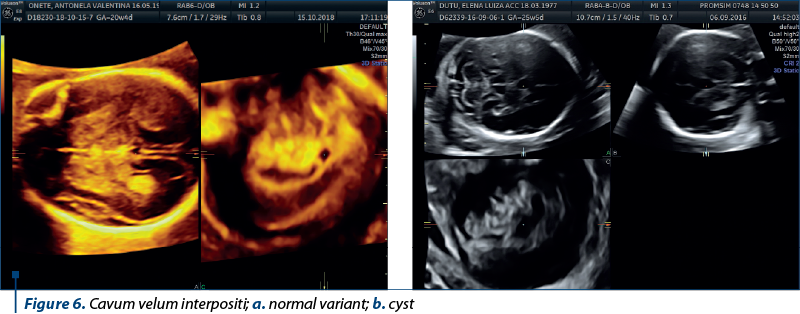
Cavum velum interpositi is located in the third ventricle, within the tela choroidea(12). When the structure is minimally fluid filled, just enough to make it visible, it is considered an anatomical variant, with no impact on fetal CNS. When the size is larger than 10 mm, it is described as a cavum velum interpositi cyst. When associated with a normal CNS scan, the prognosis is excellent(13). In this study, we found one case of cavum velum interpositi – normal variant (Figure 6a) and one case of cavum velum interpositi cyst (Figure 6b). Our cases were diagnosed at the mid trimester scan in patients of the low-risk group. 3D ultrasound proved especially useful in establishing the location of the cyst and in excluding other types of cystic structures. Color Doppler was used to exclude vascular malformations.
The 3D data base (our “library” of 3D volumes) proved useful in many situations, especially in patients who presented with ventriculomegaly later in pregnancy – the stored volumes allowed us to demonstrate the normal aspects on numerous axial sections. The offline volumes were accessed with the 4D view software.
Conclusions
We believe that the new parameters had a good feasibility, they did not prolong the examination time, and brought new and more precise diagnosis. The benefits for the pathological cases were proved by the cases reported. Also, the existence of an ultrasound volume data base allows a retrospective evaluation of cases and allows for new and sometimes better images, useful later in pregnancy or even postnatally.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Salomon LJ, Alfirevic Z, Berghella V, Bilardo C, Hernandez‐Andrade E, Johnsen SL, Kalache K, Leung K, Malinger G, Munoz H, Prefumo F, Toi A, Lee W. Practice guidelines for performance of the routine mid‐trimester fetal ultrasound scan. Ultrasound Obstet Gynecol. 2011; 7:116-26.
- Comănescu A, Cernea N, Tănase F, Comănescu C, Nedianu A, Alexandru D. Imaging the fetal corpus callosum in the routine examination – 2D versus 3D ultrasound. Ginecologia.ro. 2015; 3(8):22-7.
- Youssef A, Ghi T, Pilu G. How to image the fetal corpus callosum. Ultrasound Obstet Gynecol. 2013; 42:718-20.
- Heling KS, Chaoui R, Bollmann R. Prenatal diagnosis of an aneurysm of the vein of Galen with three‐dimensional color power angiography. Ultrasound Obstet Gynecol. 2000; 15:333-6.
- Vijayaraghavan SB, Vijay S, Kala MR, Neha D. Prenatal diagnosis of thrombosed aneurysm of vein of Galen. Ultrasound Obstet Gynecol. 2006; 27:81-3.
- Rodesch G, Hui F, Alvarez H, Tanaka A, Lasjaunias P. Prognosis of antenatally diagnosed vein of Galen aneurysmal malformations. Childs Nerv Syst. 1994;
- 10: 79–83.
- Santo S, D’Antonio F, Homfray T, Rich P, Pilu G, Bhide A, Thilaganathan B, Papageorghiou AT. Counseling in fetal medicine: agenesis of the corpus callosum. Ultrasound Obstet Gynecol. 2012; 40:513-21.
- Ghi T, Carletti A, Contro E, Cera E, Falco P, Tagliavini G, Michelacci L, Tani G, Youssef A, Bonasoni P, Rizzo N, Pelusi G, Pilu G. Prenatal diagnosis and outcome of partial agenesis and hypoplasia of the corpus callosum. Ultrasound Obstet Gynecol. 2010; 35:35-41.
- Cignini P, Padula F, Giorlandino M, Brutti P, Alfò M, Giannarelli D, Mastrandrea, ML, D’Emidio L, Vacca L, Aloisi A, Giorlandino C. Reference Charts for Fetal Corpus Callosum Length. J Ultrasound Med. 2014; 33:1065-78.
- Malinger G, Zakut H. The corpus callosum: normal fetal develop-ment as shown by transvaginal sonography. Am J Roentgenol. 1993; 161:1041–3.
- Paupe A, Bidat L, Sonigo P, Lenclen R, Molho M, Ville Y. Prenatal diagnosis of hypoplasia of the corpus callosum in association with non‐ketotic hyperglycinemia. Ultrasound Obstet Gynecol. 2002; 20:616-9.
- D’Addario V, Pinto V, Rossi AC, Pintucci A, Di Cagno L. Cavum veli interpositi cyst: prenatal diagnosis and postnatal outcome. Ultrasound Obstet Gynecol. 2009; 34:52-4.
- Kennedy A, Woodward P. P05.14: Cyst of the cavum veli interpositi in the fetus: anatomic variant not pathology. Ultrasound Obstet Gynecol. 2014; 44:211.
Articole din ediţiile anterioare
Evaluarea corpului calos fetal în examinarea de rutină - ecografie 2D versus ecografie 3D
În cadrul proiectul „Neurosonografia fetală - evaluarea potenţialului ecografiei 3D în examinarea de rutina” am analizat posibilităţile evaluării c...