Although representing no threat in the majority of patients, thrombocytopenia in pregnancy may result from a range of pathologic conditions requiring closer monitoring and therapy. Occasionally, a low platelet count in pregnancy may be part of a more complex and life threatening condition. There is a vast range of conditions directly related to pregnancy or just coexistent, which manifest with a low platelet count. A correct diagnostic and management must be ensured in order to avoid serious consequences for both mother and newborn. This review article focuses on the clinical characteristics and management of gestational thrombocytopenia and its distinction from primary immune thrombocytopenia and thrombotic microangiopathies of pregnancy.
Trombocitopenia maternă în sarcină
Maternal Thrombocytopenia in Pregnancy
First published: 15 martie 2015
Editorial Group: MEDICHUB MEDIA
Abstract
Rezumat
Cu toate că de cele mai multe ori nu pune în pericol viaţa pacientei, trombocitopenia în sarcină poate fi expresia unei serii de patologii care necesită monitorizare strictă şi terapie promptă. Ocazional, un număr scăzut de trombocite prezent în timpul sarcinii poate face parte din tabloul vast al unor boli ameninţătoare de viaţă. O parte din aceste patologii sunt legate de sarcină, altele sunt preexistente sarcinii şi se pot agrava în momentul suprapunerii peste perioada de gestaţie. În aceste situaţii, un diagnostic corect şi un management adecvat sunt necesare pentru evitarea consecinţelor grave asupra mamei şi fătului. Acest articol de tip review se axează pe caracteristicile clinice şi conduita în trombocitopenia gestaţională şi diferenţierea acesteia de trombocitopenia autoimună primară şi microangiopatiile trombotice din sarcină.
Introduction
Thrombocytopenia defined as a total platelet count of less than 150,000/mm3 (<150 x 109/L) is a common finding during pregnancy(1). It is the second most common hematological abnormality encountered during pregnancy, exceeded only by anemia. A mild thrombocytopenia is quite frequent during pregnancy and it usually has no consequences for mother and fetus. Approximately 7-10% of pregnancies may evolve with this disorder that has many causes, some of them strictly related to pregnancy itself(2). Although most cases are mild, occasionally a low platelet count may be part of a more complex and life threatening condition. The main type of thrombocytopenia (75%) is gestational thrombocytopenia, 15-20% is secondary to hypertensive disorders, 4% is caused by immune processes and 1-2% is rare constitutional thrombocytopenia, or is induced by infections or by malignancy(3).
This article is a review that focuses on the clinical characteristics and management of gestational thrombocytopenia and its distinction from primary immune thrombocytopenia and thrombotic microangiopathies of pregnancy.
Investigating thrombocytopenia in pregnancy
Most studies report a reduction in platelet count during pregnancy with 10% compared to a non-pregnant woman (Boehln et al., 2000, Abbassi-Ghanavati et al., 2006, Jensen et al, 2011). The majority of women will still have levels within the normal range, but if pre-pregnancy levels are borderline, they may fall below normal range during pregnancy(4-6). Women with multiple gestations have lower platelet count compared to singleton pregnancies.
The pathophysiological mechanisms causing low platelet count during pregnancy are: dilutional effects and accelerated destruction of platelets passing through the placenta.
Diagnosis of thrombocytopenia in pregnancy should rely on data obtained from the following fields:
-
Patient’s history of any previous obstetric events, response to treatment, family history of bleeding, autoimmune disorders;
-
Physical examination: bleeding manifestations, high blood pressure, abdominal pain;
-
Laboratory tests (depending on pregnancy stage). Blood count is assessed monthly or more frequent according to findings, blood film to exclude microangiopathy and to confirm thrombocytopenia. Coagulation profile, liver function, renal function, screening for autoimmune disorders or hereditary macrothrombopathies.
Studies state that in women with platelet counts >100 x 109/L a monthly check is sufficient. If blood count is below 80 x 109/L or if there is bleeding or bruising, the patient should refer to a haematology clinic(7).
In the first and second trimesters low platelet counts could be due to immune processes or to platelet production defects(8). In these cases, a multidisciplinary approach is needed. Obstetricians, haematologists, neonatologists and anesthetists must be involved into taking decisions for optimal care. The aim of antenatal management would be maintaining a safe platelet number, rather than a normal one.
Gestational thrombocytopenia
Gestational thrombocytopenia is the most common thrombocytopenia encountered in pregnancy. It is usually mild and does not cause adverse events for mother and newborn. It occurs in late pregnancy, mostly mid-second trimester or third trimester. Platelet levels drop <70 x109/l or lower but it does not seem to increase the risk of severe bleeding at delivery. Most specialists do not indicate epidural anesthesia due to an increased risk of hematoma.
Gestational thrombocytopenia is a diagnosis of exclusion and it may be confounded with immune thrombocytopenia.
The main characteristics of gestational thrombocytopenia are:
-
It is a mild thrombocytopenia (usually PLT>70 x 109/L).
-
There is no specific diagnosis test.
-
Is not associated with maternal bleeding.
-
No past history of thrombocytopenia outside pregnancy.
-
Occurs in late pregnancy (mid second or third trimester).
-
Not associated with fetal thrombocytopenia.
-
May reappear in the following pregnancies.
-
Spontaneously disappears after delivery.
Primary immune thrombocytopenia
Primary Immune Thrombocytopenia (ITP) is the most common cause of low platelet count in the first and second trimesters of pregnancy. It occurs in 1/1000-1/10000 pregnancies.
A platelet count <100 x 109 /L defines ITP as recommended by a consensus group meeting (Provan et al., 2010)(9). One third of patients are diagnosed for the first time during pregnancy. There is no specific diagnostic test, therefore ITP is a diagnosis of exclusion that turns to be quite difficult to put when a difference between ITP and other causes of thrombocytopenia in pregnancy must be made.
The presence of other autoimmune phenomena or a low platelet count prior to pregnancy may help. Scientists report conflicting results about maternal and perinatal outcomes.
Some studies report a significant association with: hypertensive disorders, diabetes mellitus, preterm delivery and perinatal mortality in comparison with patients without ITP(10).

The primary treatment options for primary immune thrombocytopenia are corticosteroids and intravenuous immunoglobulins (IVIG), depending on how urgent the platelet increment is, the required duration of the increment and the potential side effects. The treatment scheme must be applied accordingly to the specificity of each case. ITP is not an indication for cesarean delivery. Mode of delivery is based on obstetric indications, with avoidance of procedures associated with increased hemorrhagic risk to the fetus (forceps, vacuum extraction). The risk of conversion to cesarean section is present in every labor and some authors recommend aiming for a platelet level of at least 50 x 10 9/L before that(11,12).
In ITP patients with moderate/severe thrombocytopenia (<20-30 x109/L), the first-line treatment are corticosteroids. Their main side effects for the mother include inducing or exacerbating gestational diabetes, hypertension, osteoporosis, weight gain and psychosis. ITP patients with very severe thrombocytopenia (≤10 x 109/L) or important bleeding must receive IVIG. Duration of response is short, usually of 2-3 weeks. In life threatening bleeding a combination therapy with platelet transfusion, IVIG and a pulse of corticosteroids (methylprednisolone) is recommended (Provan et al., 2010). In refractory ITP cases some authors reported the use of: Ciclosporin A, Azathioprine, Rituximab, splenectomy(13-15), but data is poor.
Hypertensive and microangyopathic disorders in pregnancy
Preeclampsia, HELLP syndrome (Haemolysis. Elevated Liver enzymes, Low Platelets), haemolytic uraemic syndrome and thrombotic thrombocytopenic purpura (TTP) have common aspects and an overlap between them and some features of thrombocytopenia and microangiopahy may cause considerable diagnostic difficulties.
All the conditions may be present in the postnatal period, but a delay in diagnostic is life threatening (especially in TTP). The patient must immediately be referred to a center with expertise for consideration of plasma exchange.
Preeclampsia is defined as new-onset of hypertension (≥140/90mmHg) after 20 weeks of gestation together with proteinuria (ACOG 2002). Thrombocytopenia is the most common abnormality. It occurs in half cases and its severity correlates directly to the severity of preeclampsia. Thrombocytopenia in preeclampsia is unlikely to be confused with other causes but when HELLP syndrome is superposed, difficulties may occur. The syndrome may occur without proteinuria or without hypertension and then the diagnostics can be missed. Clinical manifestations can be vague, with upper abdominal pain and nausea. The maternal and fetal outcomes are severe if HELLP syndrome is not being promptly recognized. Medical stabilization with blood products, followed by delivery is indicated if HELLP syndrome occurs after 34 weeks of gestation or if the fetal and/or maternal statuses deteriorate.
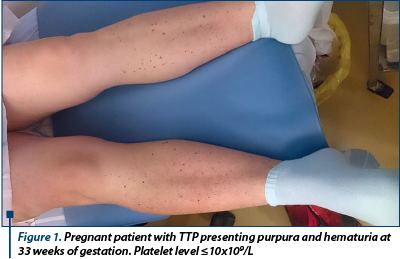
Thrombotic thrombocytopenic purpura (TTP) is a life threatening condition characterized by microangiopatic haemolytic anaemia, thrombocytopenia, appearance of bruising (purpura) or ecchymoses, fever, neurological abnormalities and renal disfunction due to a deficiency of von Willebrand factor cleaving protein (Figure 1). TTP is more frequent in women and nearly half cases occur at childbearing age. It is not specific to pregnancy but it occurs in approximately 1/25000 pregnancies, mostly in the second trimester(16-18). Plasma exchange should be initiated immediately. Where possible, delivery is the treatment of choice in pregnancy-associated microangiopathies, although it does not guarantee remission(19-20).
Conclusion
Thrombocytopenia is a common occurrence in pregnancy. Diagnosis depends on timing of its onset, severity and association of other disorders. Mild isolated thrombocytopenia may not require any medical treatment, as it does not involve any risks for mother and fetus. Thrombocytopenia associated with hypertensive disorders or microangiopathies may be severe, with important outcomes for both mother and newborn. Awareness of the complex disorders in which thrombocytopenia occurs is essential for a prompt diagnosis. The patients with such rare conditions must be immediately transferred to a center with expertise in order to ensure the correct approach. A team of obstetricians, haematologists, neonatologists and anesthetists must evaluate each case in order to offer proper care and management.
Bibliografie
2. Verdy E, Bessous V, Dreyfus M, Kaplan C, Tchernia G, Uzan S. Longitudinal analysis of platelet count and volume in normal pregnancy. Thrombosis and Haemostasis 1997(77):806–7.
3. Myers B. Diagnosis and management of maternal thrombocytemia in pregnancy. Brit J Haemat 2012, 158:3-15.
4. Abbassi-Ghanavati M, Greer LG, Cunningham FG. Pregnancy and laboratory administrative data, a reference table for clinicians. Obst Gynec, 2006, 114:1326–31.
5. Boehlen F, Hohlfeld H, Extermann P, Perneger T, de Moerloose P. Platelet count at term pregnancy: a reappraisal of the threshold. Obst Gynec 2000, 95:30.
6. Jensen JF, Wiedmeier SE, Henry E, Silver RM, Christensen RD. Linking maternal platelet counts with neonatal platelet counts and outcomes using the data repositories of a multihospital health care system. Am J Perinat, 2011,28:597–604.
7. Baili L, Khellaf M, Languille L, Bieling P, Godeau B, Michel M. Impact of pregnancy on the course of thrombocytopenic purpura: an observational study on 44 cases. Blood, 2009, 114:1320.
8. Koyama S, Tomimatsu T, Kanagawa T, Kumasawa K, Tsutsui T, Kimura T. Reliable predictors of neonatal immune thrombocytopenia in pregnant women with idiopathic thrombocytopenic purpura. Am J Hematol,2012;87(1):15-21.
9. Provan D, Stasi R, Newland A, Blanchette VS, Bolton-Maggs P, Bussel JB, Chong B, Cines D, Gernsheimer T, Godeau B, Grainger J, Greer I, Hunt B, Imbach P, Lyons G, McMillan R, Rodeghiero F, Sanz M, Tarantino M, Watson S, Young J, Kuter D. International consensus report on the investigation and management of primary immune thrombocytopenia. Blood, 2010, 115:168–86.
10. Belkin A, Levy A, Sheiner E. Perinatal outcomes and complications of pregnancy in women with immune thrombocytopenic purpura. J Maternal-Fetal & Neonatal Medicine, 2009(22/11):1081–5.
11. Webert KE, Mittal R, Sigouin C, Heddle NM, Kelton JG. A retrospective 11-year analysis of obstetric patients with idiopathic thrombocytopenic purpura. Blood. 2003; 102(13):4306-11.
12. Neunert C, Lim W, Crowther M, Cohen A, Solberg L Jr, Crowther MA. The American Society of Hematology 2011 evidence-based practice guideline for immune thrombocytopenia. Blood. 2011;117(16):4190-207.
13. Gall B, Yee A, Berry B, Birchman D, Hayashi A, Dansereau J, Hart J. Rituximab for management of refractory pregnancy-associated immune thrombocytopenic purpura. Journal of Obstetrics and Gynaecology Canada, 2010(32):1167–71.
14. Reddy D, Murphy SJ, Kane SV, Present DH, Kornbluth AA. Relapses of inflammatory bowel disease during pregnancy: in-hospital management and birth outcomes. Am J Gastroent, 2008(103):1203–9.
15. Schmid J, Piroth D, Buhrlen M, Maass N, Brummendorf TH, Galm O. Successful rituximab treatment of refractory immune thrombocytopenia during pregnancy. Onkologie, 2011, 34(Suppl 6):240, 378–584 .
16. Sadler JE. Von Willebrand factor, ADAMTS 13 and thrombotic thrombocytopenic purpura. Blood, 2008(112):11–8.
17. Scully M, Hunt BJ, Benjamin S, Liesner R, Rose P, Peyvandi F, Cheung B, Machin S J. Guidelines on the diagnosis and management of thrombotic thrombocytopenic purpura and other thrombotic microangiopathies. Brit J Haemat, 2012.
18. Vesely SK, Li X, McMinn JR, Terrell DR, George JN. Pregnancy outcomes after recovery from thrombotic thrombocytopenic purpura-hemolytic uremic syndrome. Transfusion, 2004(44):1149–58.
19. Hovinga JA, Meyer SC. Current management of thrombotic thrombocytopenic purpura. Current Opinion in Hematology, 2008(15):445–50.
20. Mirza FG, Cleary KL. Pre-eclampsia and the kidney. Seminars in Perinatology, 2009(33):173–8.
Articole din ediţiile anterioare
Implicaţii şi consecinţe ale sarcinii la adolescente
Context. Numărul sarcinilor în rândul adolescentelor este în continuă creştere la nivel global, ca urmare a schimbărilor sociale şi libertăţii sexu...
Actualităţi privind deficitul de acizi graşi esenţiali omega-3 în sarcină şi riscurile asupra fătului
Alimentaţia gravidei trebuie să fie variată şi echilibrată, deficitul unor nutrienţi putând avea repercusiuni grave asupra dezvoltării fătulu...
Principii de tratament cu metotrexat al sarcinii extrauterine necomplicate
Sarcina extrauterină reprezintă o urgenţă ginecologică severă care, în lipsa unui diagnostic stabilit corect şi rapid, precum şi a unei intervenţii...
Restaurarea coronară directă cu pivot din fibră de sticlă în sarcină - prezentare de caz
În cadrul tratamentelor dentare care sunt necesare în cursul perioadei de sarcină, situațiile clinice în care pacienta prezintă o distrucție corona...