Uterine fibroids are benign tumors which may alter the implantation process. The present study aims to examine the impact of medium-sized (3-5 cm) intramural fibroids without contact with the endometrial cavity on implantation rates in patients following in vitro fertilization (IVF) protocols. Materials and method. Thirty-one patients with intramural fibroids and 65 patients with normal uterine cavity undergoing IVF were recruited for the study groups and retrospectively evaluated. Results. Statistically significant differences were observed only regarding endometrial thickness between the two groups, and not regarding pregnancy rates. Conclusions. Intramural fibroids do not seem to decrease pregnancy rates in patients undergoing IVF with the long protocol.
Impactul fibromului intramural asupra reproducerii la pacienţii supuşi procedurilor de FIV
The impact of intramural fibroids on reproductive outcome in patients undergoing IVF procedures
First published: 17 decembrie 2019
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/ObsGin.67.4.2019.2767
Abstract
Rezumat
Fibromul uterin este o tumoră benignă cu potenţial de alterare a procesului implantaţional. În acest studiu ne-am propus să examinăm impactul pe care fibroamele intramurale de dimensiuni intermediare (3-5 cm) care nu amprentează cavitatea uterină îl pot avea asupra ratei de implantare la pacientele intrate în protocolul de fertilizare in vitro (FIV). Materiale şi metodă. Un număr de 31 de paciente cu fibrom intramural, respectiv 65 de paciente cu cavitate uterină normală, aflate în protocolul FIV, au fost evaluate retrospectiv. Rezultate. S-au constatat diferenţe semnificative doar în privinţa grosimii endometrului, însă nu şi a ratei de sarcini. Concluzii. Fibromul uterin intramural nu pare a afecta rata de sarcini la pacientele intrate în protocolul lung de FIV.
Introduction
Uterine fibroids are benign tumors of the uterine wall which may influence the implantation process. There is a large variety of phenotypes that uterine fibroids may express. Currently, submucous fibroids or intramural fibroids larger than 7 cm are chiefly incriminated in the reduction of fertility(1,2).
The mechanisms by which the fibroid impacts fertility are various and they include: distorting the uterine cavity, alteration of the subendometrial blood flow, impairment of uterine contractility, changes in cervical or tubal ostia anatomy, as well as maintaining a local inflammatory environment(2-4).
For these patients, surgery is in most cases the first step before resorting to other infertility treatments.
Unfortunately, surgical interventions – especially those performed by abdominal access – impact the overlying endometrium and require a period of at least 6 months for the cure of the uterine scar, which may be a real issue for infertile patients of advanced age (>40 years)(3).
Moreover, these interventions carry further subsidiary risks (adhesions formation, endometrial damage) which may represent auxiliary iatrogenic impediments. For this reason, care should be taken in the selection of cases suitable for surgical management.
In the present paper, we aimed to examine the impact that medium-sized uterine fibroids (3 to 5 cm) which do not impact the uterine cavity may have on implantation rates of in vitro fertilization (IVF) patients.
Materials and method
This is a retrospective study conducted in the Assisted Reproduction Department of the First Obstetrics and Gynecology Clinic, Cluj-Napoca, Romania, between January 2018 and October 2019.
A number of 128 patients, considered as normoresponsive and undergoing IVF protocols, were selected for the present study. The following exclusion criteria were used: presence of adenomyosis, uterine fibroids larger than 5 cm, fibroids which were in contact with the uterine cavity or conditions with possible endometrial impact (endometriosis).
The patients undergoing the antagonist protocol were also excluded for a better homogeneity of the groups. Patients aged under 25 years old or over 37 years old, and those with a body mass index (BMI) above 30 kg/m2 were not eligible for participation in the study.
Ovarian stimulation protocols, oocytes retrieval and embryo transfer
The starting gonadotrophin doses (urinary/recombinant FSH) were adjusted according to patient age, BMI, antimüllerian hormone (AMH) levels and previous IVF procedures. The patients received gonadotropin-releasing hormone (GnRH) agonist treatment (triptorelin, 0.1 mg) for downregulation in a long protocol. Follicle sizes were evaluated by successive ultrasound examinations. At the time when three ovarian follicles larger than 17 mm were identified, human chorionic gonadotrophin (hCG) (Ovitrelle®, 250 µg) was administered to enhance final oocyte maturation. Oocytes retrieval was performed 34-38 hours after the hCG day. Embryo transfer was performed on day three or five following oocyte retrieval. One or two embryos were transferred and the remaining embryos were frozen. Luteal phase support was achieved by progesterone administrated (Lutinus®, intravaginally, 100 mg, t.i.d.). The pregnancy was diagnosed by serum beta-hCG testing 14 days after oocyte pick-up.
We divided the patients into two groups: patients with 2-5 cm intramural fibroids which did not alter the uterine cavity (Group 1 – 31 patients), respectively patients without uterine pathology – the control group (Group 2 – 65 patients).
We analyzed the age, the BMI and the duration of infertility of these patients, the type of response to ovarian stimulation (number of oocytes >14 mm, the number of oocytes retrieved, the number of resulting embryos, the pregnancy rates, and the endometrial thickness on the hCG day).
Statistical analysis
The statistical analysis was performed using OpenEpi v.3.03 and StatsDirect v.2.7.2 statistical packages to generate descriptive statistics, Pearson (r) correlation coefficients, and linear regression models. For variables with normal distribution, we used the t (Student) test, and for those with non-uniform distribution or ranks, we used the non-parametric Mann-Whitney (U) test. The statistical significance was defined as a=0.05 (5%). To evaluate the correlation between two continuous variables with normal (uniform) distribution, we used the Pearson (r) correlation coefficient, and for variables with non-uniform distribution, we used the Spearman coefficient for rank correlation (r).
Results
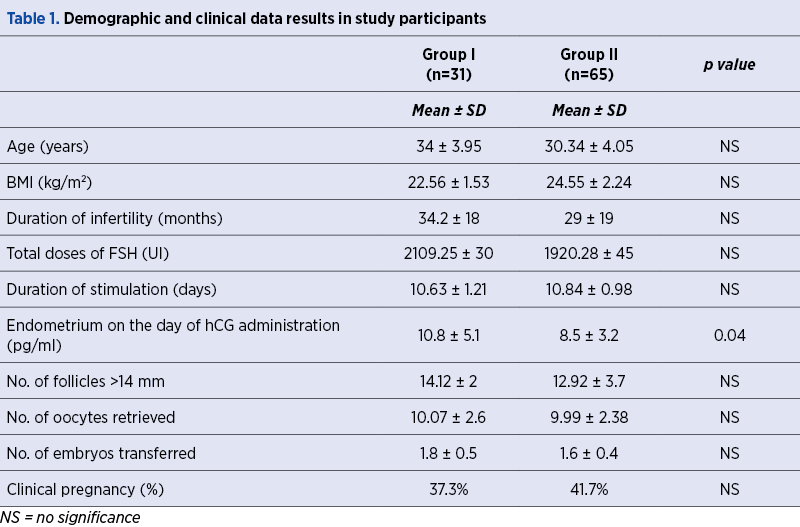
The study participants’ demographic and clinical characteristics are described in Table 1. There were no statistical differences regarding age, BMI, duration of stimulation, the FSH doses required, number of oocytes or the number/quality of embryos transferred. A significant statistical difference was described regarding endometrial thickness. There was a difference in terms of pregnancy rate, but without clinical relevance.
Discussion
The impact of intramural fibroids on fertility remains uncertain. Data provided by the current study identified a larger thickness of the susceptible endometrium in uterine fibroid patients, but with similar pregnancy rates between groups.
Currently available literature on this topic is surprisingly sparse, considering the relatively large frequency of this type of tumor(6,7). The results provided by these studies are largely concentrated in a series of meta-analyses whose conclusions are similar: subserous fibroids do not alter pregnancy rates, while submucous fibroids are detrimental to fertility. Regarding intramural fibroids, studies report much lower pregnancy rates, but which do not improve following myomectomy(6-8).
When analyzing the implantation process, we must take into consideration a series of aspects involved in this process. A series of main pillars have been nominated, which are strongly interconnected and whose function is crucial for implantation: production of local steroid metabolism, the immune system, the integrin system (interleukins, adhesins), the oxide-reductive system or the functionality of the junctional zone. Furthermore, uterine fibroids are estrogen dependent and may be associated with primary alterations in other factors implicated in this process, independently from the actual impact derived from the presence of the tumor. In this respect, excessive endometrial aromatase production, alterations of natural killer cells or alterations of the junctional zone may represent independent factors which alter implantation rates(3,5).
The results of our study come to somewhat contradict literature(9) reports in the sense that pregnancy rates were similar between the two groups. This may be explained by the use of the long protocol for stimulation and consequently a more expressed ovarian suppression with lower estrogen levels.
As such, the dysfunctions described previously were in part controlled by this strategy. In this regard, there is a series of studies which prove that GnRH agonists improve the aforementioned dysfunctions.
In conclusion, patients with intramural fibroids who do not exhibit endometrial consequences may be managed conservatively without repercussions on their success rates.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
2. Bulun SE. Uterine fibroids. The New England Journal of Medicine. 2013; 369(14):1344–1355.
3. Van Heertum K, Barmat L. Uterine fibroids associated with infertility. Women’s Health. 2014; 10(6):645–653.
4. Pritts EA. Fibroids and infertility: a systematic review of the evidence. Obstetrical and Gynecological Survey. 2001; 56(8):483–491.
5. Pritts EA, Parker WH, Olive DL. Fibroids and infertility: an updated systematic review of the evidence. Fertility and Sterility. 2009; 91(4):1215–1223.
6. Sunkara SK, Khairy M, El-Toukhy T, Khalaf Y, Coomarasamy A. The effect of intramural fibroids without uterine cavity involvement on the outcome of IVF treatment: a systematic review and meta-analysis. Human Reproduction. 2010; 25(2):418–429.
7. Zepiridis LI, Grimbizis GF, Tarlatzis Basil C, et al. Infertility and uterine fibroids. Best Practice Research Clinical Obstetrics Gynaecology. 2016; 34:66–73.
8. Somigliana E, De Benedictis S, Vercellini P, et al. Fibroids not encroaching the endometrial cavity and IVF success rate: A prospective study. Human Reproduction. 2011; 26(4):834–839.
9. Oliveira FG, Abdelmassih VG, Diamond MP, Dozortsev D, Melo NR, Abdelmassih R. Impact of subserosal and intramural uterine fibroids that do not distort the endometrial cavity on the outcome of in vitro fertilization-intracytoplasmic sperm injection. Fertil Steril. 2004; vol. 81 582-587.
Articole din ediţiile anterioare
Frumoasa şi bestia: medicaţia utilizată pentru stimularea ovariană creṣte riscul de cancere genitale pe termen lung? Un review extensiv
Stimularea ovariană pentru inducerea ovariană şi fertilizarea in vitro (FIV) sunt utilizate frecvent la nivel mondial de multe cupluri infertile.
Semnificaţia instabilităţii microsatelitare în cancerul endometrial
Cancerul endometrial reprezintă cea mai frecventă patologie ginecologică malignă din ţările dezvoltate, atât ratele de incidenţă, cât şi cele de mo...
Tratamentul laparoscopic al bolilor pelvine inflamatorii şi implicaţiile infertilităţii
Infecţiile genitale, atât la bărbaţi, cât şi la femei, pot provoca leziuni funcţionale permanente ale aparatului reproductiv, care pot duce la apa...
Fibroamele uterine asociate sarcinii – este fezabilă miomectomia în sarcină? Review şi prezentare de caz
Mioamele uterine afectează 2-10% dintre femeile însărcinate. Sunt tumori dependente hormonal şi, în consecinţă, 30% dintre ele vor creşte ca răspun...