Introduction. Morphological anomalies of the cardiovascular system represent a major cause of neonatal mortality and morbidity worldwide. A routine fetal ultrasound can easily miss the diagnosis of this tetralogy of Fallot due to its normal appearance in the four-chamber ultrasound view. Method. The article describes a multidisciplinary retrospective study performed in the first and second departments of obstetrics and gynecology in association with the neonatology and pediatry departments of the “Pius Brînzeu” Emergency Clinical County Hospital. It presents the patterns of evolution of live newborns diagnosed before and after birth with tetralogy of Fallot in the last three years. Conclusions. Tetralogy of Fallot is a condition that requires special medical attention after birth, so prenatal detection is critical as it places the pregnant women in a high-risk group. The management of this cardiac malformation can be a challenge after birth and it can have an intricate way of evolution until surgical correction. Although a feared pathology in the past, tetralogy of Fallot’s surgical treatment has an excellent prognostic.
Managementul prenatal şi postnatal în tetralogia Fallot
Tetralogy of Fallot prenatal and postnatal management
First published: 18 aprilie 2019
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/ObsGin.67.1.2019.2293
Abstract
Rezumat
Introducere. Anomaliile morfologice ale aparatului cardiovascular reprezintă o cauză majoră de morbiditate şi mortalitate neonatală. O ecografie fetală de rutină poate omite uşor diagnosticul de tetralogie Fallot, din cauza aspectului normal al cordului fetal în secţiunea de patru camere. De fapt, utilizarea strictă a acestei secţiuni identifică doar un procent redus din cazurile cu cardiopatii congenitale. Metodă. Articolul prezintă un studiu retrospectiv multidisciplinar efectuat de Departamentul de obstetrică şi ginecologie în asociere cu Departamenul de neonatologie şi pediatrie al Spitalului Clinic Judeţean de Urgenţă „Pius Brînzeu” din Timişoara. Studiul descrie modelele de evoluţie a nou-născuţilor diagnosticaţi antenatal şi postnatal cu tetralogie Fallot în ultimii trei ani. Concluzii. Tetralogia Fallot este o patologie care necesită o conduită specială după naştere, astfel încât detectarea prenatală este critică, plasând pacienta în grupul gravidelor cu risc. Managementul acestei malformaţii cardiace complexe poate reprezenta o provocare după naştere, având o evoluţie intricată până la corecţia chirurgicală. Deşi îngrijorătoare în trecut, tetralogia Fallot are un prognostic excelent după tratamentul chirurgical.
Introduction
The morphologic anomalies of the cardiovascular system represent an important cause of neonatal morbidity and mortality worldwide, the reported death rate in the first 27 days after birth being 4.2%(1). Congenital heart disease is still the most frequent cause of congenital anomalies(2). The literature cites an incidence of heart defects that varies from 0.8-1% in case of term newborns to 8.3% in case of premature newborns(2).
The prenatal diagnosis is based on identifying sonographic images that will raise the suspicion of anomalous heart. The International Society of Ultrasound in Obstetrics and Gynecology (ISOUG) recommends the morphologic evaluation of the heart between 18 and 22 weeks of gestation(3). This screening is based on the evaluation of the situs of the heart, the four-chamber view, the ejection tract of the right and left ventricle, and the three-vessel view. In case of a low risk of a gravida with a positive ultrasound screening for cardiac anomalies, an expertise evaluation must be done by a practitioner specialized in fetal medicine(3). Irrespective of the reason, high-risk gravidas must be evaluated in a fetal medicine center(3). As far as the prenatal rate detection of congenital heart defects is concerned, the literature reports a rate of 82.1% in case of specialists in fetal medicine.
The most frequent congenital heart diseases are ventricular septal defect (prevalence of 6.23), tetralogy of Fallot (prevalence of 2.66), and atrio-ventricular septal defect (prevalence of 1.89)(4). Tetralogy of Fallot is defined as a combination of: ventricular septal defect, overriding of the aorta, pulmonary artery stenosis, and right ventricular hypertrophy(4). Despite the simplicity of the postnatal ultrasound diagnosis, the prenatal diagnostic rates are quite low, ranging from 30% to 60%(5).
Materials and method
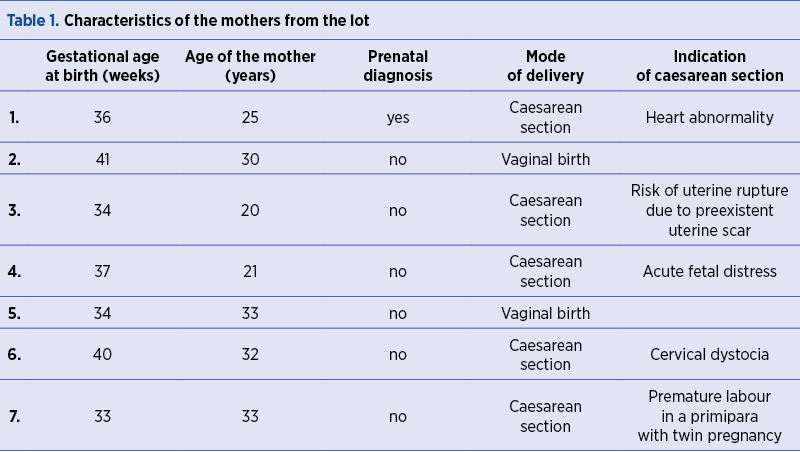
The paper presents a multidisciplinary retrospective study performed in the first and second departments of obstetrics and gynecology in association with the neonatology and pediatry departments of the “Pius Brînzeu” Emergency Clinical County Hospital, Timişoara. The study followed the pregnancies with fetal tetralogy of Fallot, the prenatal rate of diagnosis of this cardiac pathology, the delivery mode, as well as short- and long-term management of the neonates. During the studied period (2016-2018), 7828 births were registered in our clinics. Out of these, seven neonates were diagnosed with tetralogy of Fallot. The prenatal detection rate was 1/7. The characteristics of the studied lot are presented in Table 1 and Table 2.

Results
A routine fetal ultrasound can easily miss the diagnosis of tetralogy of Fallot, due to the normal aspect of the heart in the four-chamber view. Actually, using strictly this sonographic heart section, the chance of diagnosing a potential heart defect is only 30%(7).
In order to raise the suspicion of tetralogy of Fallot, there are necessary additional sonographyc heart sections: the five-chamber view that shows a discontinuation of the ventricular septum with the medial wall of the aorta, a lateral view of the heart that shows the ventricular septal defect (with color Doppler confirmation), as well as the three-vessel view that shows the dilated aorta. The prenatal detection rate of these anomalies usually depends on the gestational age of the fetus and the severity of the disease(8). Right ventricular hypertrophy develops rarely in the prenatal life, mostly because of the presence of the foramen ovale and the arterial duct that are responsible for reducing the pressure in the right ventricle(9). In our study, one fetus was diagnosed with this cardiac anomaly. Out of the seven pregnant women, only three had regular obstetrical check-ups during pregnancy, and only one was evaluated (and diagnosed) by a specialist in fetal medicine. Although some articles describe maternal alcohol, anticonvulsivants or retinoic acid intake, as well as hyperphenylalaninemia and phenylketonuria as risk factors for tetralogy of Fallot, no evident maternal risk factors for this condition were found(10).
Discussion
Whenever a suspicion of heart anomaly is suspected, genetic testing, as well as expertise morphologic ultrasound evaluation are recommended, hence 17% of cases are accompanied by chromosomal abnormalities(11). The literature reports a higher incidence of tetralogy of Fallot in fetuses with DiGeorge syndrome, trisomy 21 and trisomy 18.
Other cited extracardiac anomalies frequently associated with this pathology are: absence or hypoplastic thymus, right aortic arch, and anomalous subclavian artery(10).
Other studies reported a higher incidence of talipes, traheo-oesophagian fistula, abdominal wall defects, as well as ventriculomegaly(12). In our study, no genetic tests had been performed during pregnancy, however after birth the neonatology team requested genetic testing in two cases; in both cases, DiGeorge syndrome was diagnosed. Other extracardiac abnormalities identified in our study lot after birth included low inserted ears, facial asymmetry, retrognatia, syndactilily, and talipes.
Prenatal diagnosis of tetralogy of Fallot is important, as it places the pregnant woman in the high-risk pregnancy group. The further management of this case should be made in a third-degree level maternity by a complex team that will decide the mode of delivery, as well as the newborn’s treatment. As far as the prenatal management is concerned, the options are scarce and not specific. Due to the relatively equal pressure of the fetal systemic and pulmonary systems, usually there are no repercussions on fetal growth. However, in cases diagnosed with absence of the pulmonary valve, severe pulmonary regurgitation with fetal cardiac failure and fetal hydrops can appear(13). In our study, most of the women delivered at term; nevertheless, in three situations, premature labour was installed. As far as the mode of delivery is concerned, two patients delivered vaginally and in the rest of the cases the mode of delivery was through caesarean section. There appears to be no significant link between the mode of delivery and the immediate extrauterine adjustment of the neonates. The immediate extrauterine adjustion was difficult for the majority of the neonates: most of the patients had a one-minute Apgar score of 7 or less (five out of seven neonates). The weight of the babies varied between 1700 and 3070 grams, but when evaluated on the growth chart, only one neonate was considered small for gestational age.
If severe obstruction of the left ventricular tract is diagnosed, immediate prostaglandins administration after birth is indicated, as it prevents the closure of the arterial duct and consequently ameliorates the right to left shunt. In our study, one neonate benefited from continuous administration of prostaglandins until surgical correction that was performed four weeks after delivery.
The outcome of a case with tetralogy of Fallot depends on the degree of severity, on the association with extracardiac anomalies and on the postnatal treatment. In the absence of treatment, 35% of the children will die in the first year of life, and 50% will die in the first three years from birth(14). With appropriate surgical treatment, the survival reported rates are 97-100% in the first year of life, and 87.5% in the first ten years(14). Regarding the long-term evolution, only four cases from our lot are still under observation. Three infants already had complete surgical correction. With the exception of one baby, the rest were treated in specialized pediatric surgery centers in Romania, with a favorable immediate result. Until present time, all patients have a favorable outcome; however, in one case, stenosis of the conduct appeared and a new surgical session is considered. One infant is still on medical treatment, though he is also scheduled for surgery.
Conclusions
Tetralogy of Fallot is a condition that requires special medical attention after birth, so prenatal detection is critical, as it places the pregnant woman in a high-risk group. All women diagnosed prenatally should deliver in a third-level maternity, as it is beneficial for the immediate management of the neonate. The management of this cardiac malformation can be a challenge after birth, and it can have an intricate evolution until surgical correction. Although a feared pathology in the past, tetralogy of Fallot’s surgical treatment has an excellent prognostic in the short and long term.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
2. Moons P, Sluysmans T, De Wolf D. Congenital heart disease in 111,225 births in Belgium: birth prevalence, treatment and survival in the 21st century. Acta Paediatr. 2009; 98:472–477.
3. International Society of Ultrasound in Obstetrics and Gynecology; Carvalho JS, Allan LD, Chaoui R, et al. ISUOG Practice Guidelines (updated): sonographic screening examination of the fetal heart. Ultrasound Obstet Gynecol. 2013; 41: 348–359.
4. Xie D, Fang J, Liu Z, Wang H, Yang T, Sun Z, Wang A, Xiong L. Epidemiology and major subtypes of congenital heart defects in Hunan Province, China Donghua. Medicine (Baltimore). 2018; 97(31): e11770.
5. Hill GD, Block JR, Tanem JB, Frommelt MA. Disparities in the prenatal detection of critical congenital heart disease. Prenat Diagn. 2015; 35:859–863.
6. Chew C, Halliday JL, Riley MM, Penny DJ. Population-based study of antenatal detection of congenital heart disease by ultrasound examination. Ultrasound Obstet Gynecol. 2007; 29:619–624.
7. van Velzen CL, Clur A, Rijlaarsdam MEB et al. Prenatal diagnosis of congenital heart defects: accuracy and discrepancies in a multicenter cohort. Ultrasound Obstet Gynecol. 2016; 47(5):616-22.
8. Pepas LP, Savis A, Jones A, Sharland GK, Tulloh RM, Simpson JM. An echocardiographic study of tetralogy of Fallot in the fetus and infant. Cardiol Young. 2003; 13(3):240-7
9. Becker R, Schmitz L, Guschmann M, Wegner RD, Stiemer B, Entezami M. Prenatal diagnosis of familial absent pulmonary valve syndrome: case report and review of the literature. Ultrasound Obstet Gynecol. 2001; 17:263–267.
10. Bailliard F, Anderson RH. Tetralogy of Fallot. Orphanet J Rare Dis. 2009; 4:2.
11. Poon LC, Huggon IC, Zidere V, Allan LD. Tetralogy of Fallot in the fetus in the current era. 2007;29(6):625-7.
12. Bronshtein M, Siegler E, Yoffe N, Zimmer EZ. Prenatal diagnosis of ventricular septal defect and overriding aorta at 14 weeks’ gestation, using transvaginal sonography. Prenat Diagn. 1990; 10(11):697-702.
13. Hirsch JC, Mosca RS, Bove EL. Complete repair of tetralogy of Fallot in the neonate: results in the modern era. Ann Surg. 2000; 232:508–514.
14. Yong MS, Yim D, Brizard CP, Robertson T, Bullock A. Long-term outcomes of patients with absent pulmonary valve syndrome: 38 years of experience. Ann Thorac Surg. 2014; 97(5):1671-7.
Articole din ediţiile anterioare
Prognosticul în cazul pentalogiei lui Cantrell
Pentalogia lui Cantrell este un sindrom congenital rar, considerat letal, care asociază în forma sa completă următoarele cinci defecte: defect la n...
Fibroamele uterine asociate sarcinii – este fezabilă miomectomia în sarcină? Review şi prezentare de caz
Mioamele uterine afectează 2-10% dintre femeile însărcinate. Sunt tumori dependente hormonal şi, în consecinţă, 30% dintre ele vor creşte ca răspun...
Sarcina cicatricială după operaţia cezariană – o continuă dilemă terapeutică. Serie de cazuri şi review al literaturii
Sarcina cicatricială după operaţie cezariană (CSP) este o tulburare iatrogenă care pune viaţa în pericol, cu o incidenţă tot mai mare, din cauza cr...
Consilierea în agenezia ductului venos secundară venei cave inferioare întrerupte
The ultrasound (US) examination of the fetal venous system has exposed a wide spectrum of malformations.