Skin cancers are the most common type of cancer worldwide, with increasing incidence and prevalence in the past decades. It has been aimed to determine the recurrence rates after different treatment options, and the results proved that surgical excision and radiotherapy had the lowest relapse rates, whereas curettage and photodynamic therapy resulted in five-year relapse rates of up to 70%(1). The axial paramedian forehead is the flap of choice for extensive nose defects reconstruction due to its great variability in terms of size and shape of the donor and recipient site. When used as a three-dimensional pattern flap, it will restore not only the dimensions of the defect, but also the proportion and contour of the nose by replacing skin with tissue of similar color, texture and thickness.
Reconstrucţia unui defect extensiv la nivelul nasului cu lambou frontal paramedian după excizii seriate pentru recidivă locală de carcinom bazocelular
Nasal reconstruction of extensive defect using axial paramedian forehead flap after staged excision for relapsed basal cell carcinoma
First published: 30 noiembrie 2018
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Orl.41.4.2018.2119
Abstract
Rezumat
Cancerele de piele sunt cele mai frecvente tipuri de cancer, cu o creştere semnificativă a incidenţei şi prevalenţei în ultimele decenii. S-a încercat determinarea ratelor de recidivă locală după diferite metode de tratament, iar rezultatele au dovedit că excizia chirurgicală cu margini de siguranţă oncologică şi radioterapia au avut cele mai mici rate de recurenţă, pe când chiuretajul şi terapia fotodinamică au fost încadrate la rate de recidivă la cinci ani de aproximativ 70%(1). Lamboul frontal paramedian este lamboul de elecţie pentru reconstrucţia defectelor extensive de la nivelul nasului, în principal datorită marii variabilităţi în privinţa formei şi dimensiunii zonelor donoare şi receptoare. Când este gândit ca pattern tridimensional, lamboul restabileşte nu numai dimensiunile defectului, dar şi proporţiile şi conturul nasului, înlocuind pielea cu ţesut similar în ceea ce priveşte textura, culoarea şi grosimea.
Case presentation
A 50-year-old male patient presented to our Plastic and Reconstructive Surgery Department for nodulo-ulcerative lesions on the nose, developed on scarred tissue surrounded by skin desquamation without well defined margins. The first assessment of the patient determined that the lesion was local basal cell carcinoma recurrence. The initial lesion was biopsied and cauterized twice in the last three years.
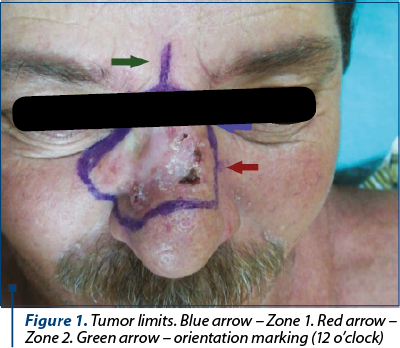
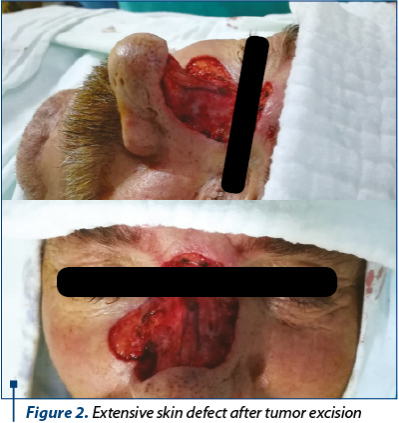
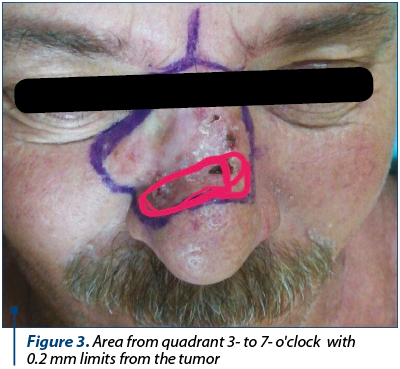
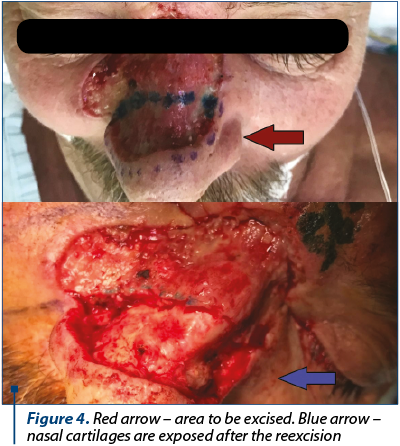
After the dermoscopic examination the limits were marked, resulting a lesion which included both Zone 1 and Zone 2 of the nose, the right lateral nose side wall, the superior one-third of the nose ala and part of the cheek (Figure 1). Following the preoperative markings, under local anesthesia, the tumor was excised with 3 mm safety margins. The depth of the excision reached the orbicularis muscle, SMAS (superficial muscular aponeurotic system) of the cheek and nasal muscle (Figure 2). We carefully ensured hemostasis and secured the wound with neutral ointment dressing. The excised sample, labeled at 12-o’clock position, underwent histopathological examination and the result showed infiltrative sclerodermiform basal cell carcinoma invading the deep dermis with 0.2 mm demarcation limits in depth from quadrant 3- to 7-o’clock (Figure 3). The area with inframillimetric limits from the tumor was reexcised (Figure 4, Figure 5). After thoroughly assessing the size and shape of the defect, along with the nasal cartilage exposure, we decided to use a combined “V-Y” nasolabial flap for the cheek region and paramedian forehead flap for nasal reconstruction (Figure 6). The advancement of the “V-Y” flap reduced the cheek defect. The forehead flap was harvested with a 2-centimeter vascular pedicle and rotated over the nose defect (Figure 7). We used primary closure for the donor site in the cheek region and skin grafting for the forehead area (Figure 8). At the 7-day follow-up, the flap was completely integrated, with no local complications (Figure 9).
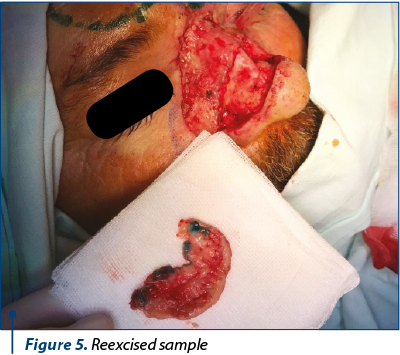
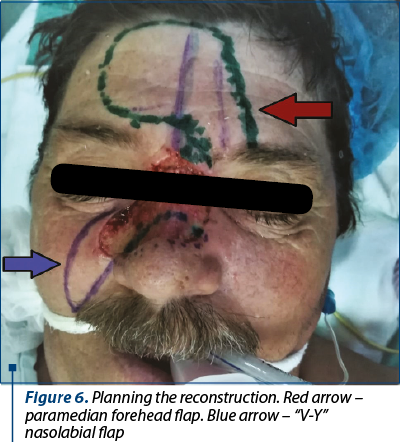
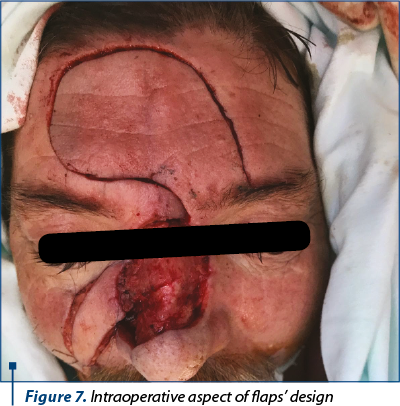
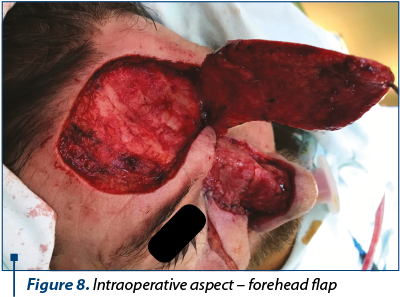
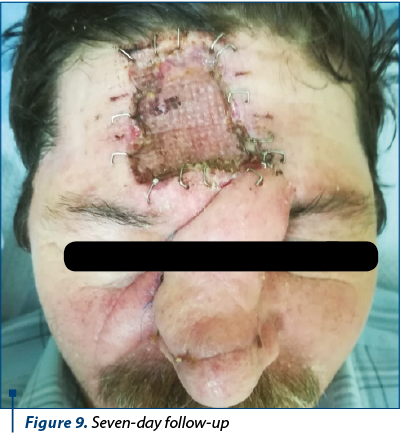
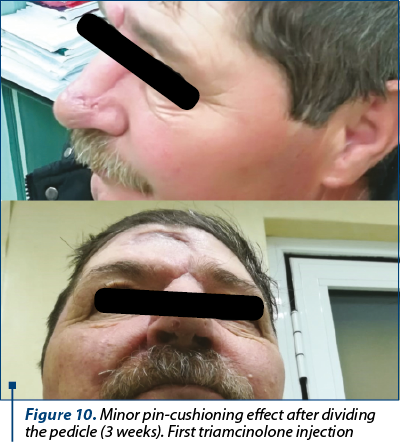
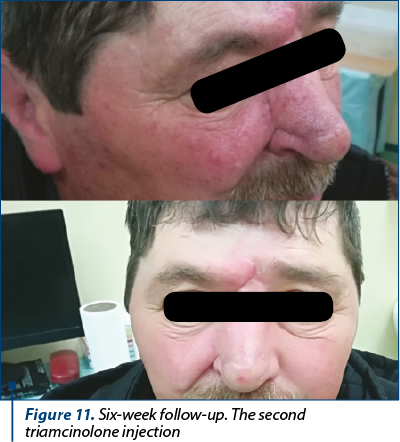
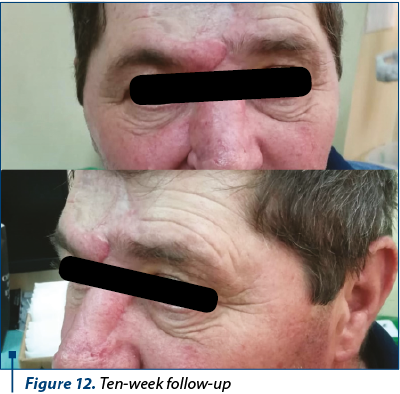
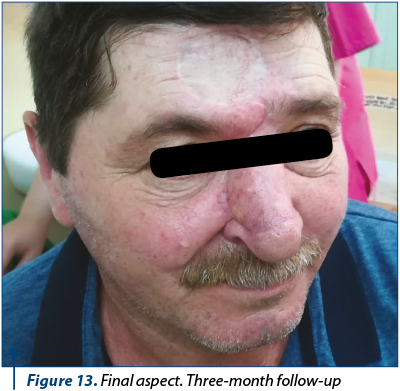
The patient underwent the second stage of the surgery three weeks after the first one, when the forehead flap’s pedicle has been divided, under local anesthesia. Minor complications included pin-cushioning effect (Figure 10), which was satisfyingly reduced by locally injecting triamcinolone, in three sessions, each at three weeks apart (Figure 11, Figure 12).
Discussion
The forehead flap is the work horse for large nose defects due to the following characteristics: it is easy to raise, it has a reliable pedicle, it can be raised in various sizes and shapes, it provides tissue similar in color and texture with the nasal skin. The disadvantages of using this flap are: it is a two-stage flap, it requires patient compliance for the three weeks between stages and for the following 6 to 12 months during which surgical and/or nonsurgical procedures might become necessary in order to obtain maximum esthetic results.
The current literature cites surgical and nonsurgical treatment options for skin carcinomas(2). With so many options available, we obviously face the question what and when to use one or another.
Mohs and slow Mohs surgery are now the gold standard for surgical treatment of high-risk skin carcinomas that feature the following characteristics: location in the central face, size less than 2 centimeters, poor clinical definition of tumor margins, recurrent lesions, histologically confirmed morphoeic, infiltrative, micronodular, basosquamos types or perineural and perivascular involvement.
By far, the most frequently used nonsurgical option is cauterization after curettage of the tumor. Studies cited in literature proved that curettage and cauterization is a good treatment for low-risk skin carcinomas, but should not be used for high-risk tumors(3).
We consider the case presented to be illustrative of how treatment options should be judged. We support tumor biopsy before taking any decision because histological high-risk features can definitely guide us towards the correct treatment option.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Bøgelund FS, Philipsen PA, Gniadecki R. Factors Affecting the Recurrence Rate of Basal Cell Carcinoma. Acta Derm Venereol. 2007; 87: 330–334.
- Telfer NR, Colver GB, Morton CA. Guidelines for the management of basal cell carcinoma. Br J Dermatol. 2008 Jul; 159(1):35-48.
- American Cancer Society. Cancer Facts & Figures 2018. Atlanta: American Cancer Society; 2018.
Articole din ediţiile anterioare
Reconstrucţia de vestibul nazal şi aripă nazală cu cartilaj auricular şi lambou cutanat latero-nazal după excizia unui carcinom bazocelular
Numărul în continuă creştere al cancerelor cutanate diagnosticate, dintre care un procent important localizat la nivelul feţei, a determinat chir...
Reconstrucţia unui defect complex ce cuprinde multiple subunităţi nazale cu lambou insular după chirurgia oncologică a carcinomului bazocelular
Aproximativ 85% dintre carcinoamele bazocelulare apar la nivelul feţei(1). În regiunea nazală, zonele includ pereţii nazali, dorsum nasi, cartilaje...
Urmărirea pacienţilor cu carcinom bazocelular
Tegumentul poate fi afectat de tumori maligne, cu preponderenţă carcinomul bazocelular, urmat de cel spinocelular şi melanomul malign. Patol...