MATERNAL-FETAL MEDICINE
Impactul parametrilor materni asupra restricţiei de creştere intrauterină
The impact of maternal parameters on intrauterine growth restriction
Abstract
The incidence of fetal growth restriction is variable, being known that is more frequent in resource-limited countries. The mechanism of fetal growth restriction is considered to be multifactorial, resulting from a combination of maternal, placental and fetal factors, the uteroplacental insufficiency being the dominant cause. Our purpose in this study was to determine the impact and the incidence of various maternal factors encountered among cases with fetal growth restriction delivered at term. The studied parameters were: the birth weight, the sex of the newborn, the way of delivery, the Apgar score at one minute, the maternal age, the maternal gestation and parity, the presence of presentation dystocia, the pregnancy monitoring by specialist, the presence of infectious factor, the presence of abnormal placental insertion or umbilical cord abnormalities, the status of the fetus and the presence of pregnancy-induced hypertension, preeclampsia or eclampsia. Results. During the 3-year period of the study, there were registered 12987 births in our hospital. The incidence of newborns with low birth weight at term was 1.5%. The average weight at birth was 2302 grams, with the lowest value 1750 grams, and the female fetuses were more affected (57.6%). The incidence of placental condition within the studied group was only 2%; also, the pregnancy-induced hypertension was present only in 6% of cases. Conclusion. Fetal growth restriction requires an accurate diagnosis with a clear distinction of constitutional small fetuses from the abnormal small ones. Ultrasound monitorization is mandatory for the diagnosis and the assessment of the fetal statusKeywords
growth restrictionmaternal factorsRezumat
Incidenţa restricţiei creşterii fetale este variabilă, fiind cunoscut faptul că este mai frecventă în ţările slab dezvoltate. Mecanismul restricţiei de creştere fetală este considerat a fi multifactorial, rezultând dintr-o combinaţie de factori materni, placentari şi fetali, insuficienţa uteroplacentară fiind cauza dominantă. Scopul nostru în acest studiu a fost de a determina impactul şi incidenţa diverşilor factori materni întâlniţi în cazurile cu restricţie de creştere fetală cu naştere la termen. Parametrii studiaţi au fost greutatea la naştere, sexul nou-născutului, calea naşterii, scorul Apgar la 1 minut, vârsta mamei, gestaţia maternă şi paritatea, prezenţa distociilor de prezentaţie, neinvestigarea sarcinii, prezenţa factorului infecţios, prezenţa anomaliilor de inserţie placentară sau a modificărilor cordonului ombilical, starea fătului şi prezenţa hipertensiunii induse de sarcină, a preeclampsiei sau a eclampsiei. Rezultate. Pe parcursul a 3 ani de studiu, în spitalul nostru au fost înregistrate 12987 de naşteri. Incidenţa nou-născuţilor la termen cu greutate mică la naştere a fost de 1,5%. Greutatea medie la naştere a fost de 2302 grame, cu cea mai mică valoare 1750 de grame, feţii de sex feminin fiind mai afectaţi (57,6%). Incidenţa anomaliilor placentare în cadrul grupului studiat a fost de numai 2%. De asemenea, hipertensiunea indusă de sarcină a fost prezentă doar în 6% din cazuri. Concluzie. Restricţia de creştere intrauterină necesită un diagnostic precis, cu o distincţie clară a feţilor mici constituţional de cei cu reală restricţie de creştere. Monitorizarea ecografică este obligatorie pentru clarificarea diagnosticului şi evaluarea statusului fetal.Cuvinte Cheie
restricţie de creşterefactori materniIntroduction
Intrauterine growth restriction is a constant actual topic due to the association of this condition with an increased fetal morbidity and mortality. The incidence of fetal growth restriction is variable, being known the fact that is more frequent in resource-limited countries. It is defined as infants with a birth weight below the 10th percentile for gestational age. The inconvenience of this definition is the impossibility of distinguishing pathologically the grown infants from those who are constitutionally small. The constitutionally small newborns are at the maximum of their normal growth potential (weight between the 5th and the 10th percentiles, with normal physiology, normal velocimetry of umbilical artery during pregnancy progression) with a favorable successive outcome. By distinguishing a true fetal growth restriction from a normal small constitutional fetus, the clinician can avoid unnecessary pregnancy interventions(1). The importance of the mentioned differences is supported by a large prospective observational trial(2) (PORTO); over 1100 pregnancies were studied with small fetuses (<10th percentile weight for gestational age on ultrasound examination), resulting a poor outcome for fetuses with the birth weight <3rd percentile and abnormal umbilical artery Doppler(2). Above that, most cases of intrauterine growth restriction remain undiagnosed until birth; regarding this affirmation, several maternal risk factors can lead to the suspicion of this condition.The mechanism of fetal growth restriction is considered to be multifactorial, resulting from a combination of maternal, placental and fetal factors, the uteroplacental insufficiency being the dominant cause. Several maternal non-pathological factors can reflect into an increased risk for fetal growth restriction, as height, pregnancy weight, parity, and ethnicity(3). Due to the fact that a strong association exists between congenital anomalies and intrauterine growth restriction in 20 to 60 percent of cases(4), close and detailed monitoring of fetal anatomy is required in all cases. An asymmetric fetal growth restriction in pregnancies after 24 weeks with normal fetal anatomy suggests an etiology most likely placental or maternal.
Fetal growth restriction can have an early onset, with an incidence percentage of 20-30% from all the fetal growth restriction cases(5), being associated with severe placental insufficiency and chronic fetal hypoxia prior to severe injury or fetal death before term(6). The late onset of fetal growth restriction characterizes 70-80% of cases and is considered to be of a rather benign nature, but a fetal deterioration before labor is always possible(7).
Regarding the management of pregnancies, when this condition is suspected, is based on few randomized trials(8); these pregnancies require a special monitoring, recommended gestational age for delivery and postnatal surveillance. The outcome of small fetuses can be predicted antenatally through several parameters, with no evidence that one is more suggestive than other.
- Umbilical artery has been accepted for almost 20 years to be the standard for predicting fetal growth restriction. Meta-analyses regarding this parameter have shown that a high value of umbilical artery Doppler has a positive impact on the mortality and perinatal outcome of fetuses with fetal growth restriction(9), but not as standalone criteria.
- Middle cerebral artery Doppler is essential for evaluating the presence of brain vasodilation, an indirect sign of hypoxia. Middle cerebral artery being a late manifestation with low sensitivity, is mostly an important predictor for late-onset fetal growth restriction outcome(10).
- Cerebroplacental ratio is an important diagnostic criterion, improving significantly the sensitivity of umbilical artery and middle cerebral artery alone; the values of this parameter are modified even when its components measured alone suffer minor modification(11).
- Ductus venous Doppler represents the most important parameter for predicting the proximal risk for fetal death in early-onset fetal growth restriction; its value is modified only in advanced compromised fetal status, reflecting at that point important hypoxia and acidosis(12).
- Another parameter used to appreciate the impact of early-onset of fetal growth restriction is the aortic isthmus Doppler that is associated with increased mortality and important neurological morbidity and precedes the impaired values of ductus venous with one week(13).
Material and method
Our purpose in this study was to determine the impact and the incidence of various maternal factors encountered among cases with fetal growth restriction delivered at term. We studied the births from the University Emergency Hospital of Bucharest for a period of three years, the target population being represented by the newborns delivered at term with the weight smaller than 2500 grams. The studied parameters were the birth weight, sex of the newborn, the way of delivery, the Apgar score at 1 minute, the maternal age, the maternal gestation and parity, the presence of presentation dystocia, the pregnancy monitoring by a specialist, the presence of infectious factor, the presence of abnormal placental insertion or umbilical cord abnormalities, the status of the fetus and the presence of pregnancy-induced hypertension, preeclampsia or eclampsia.Results
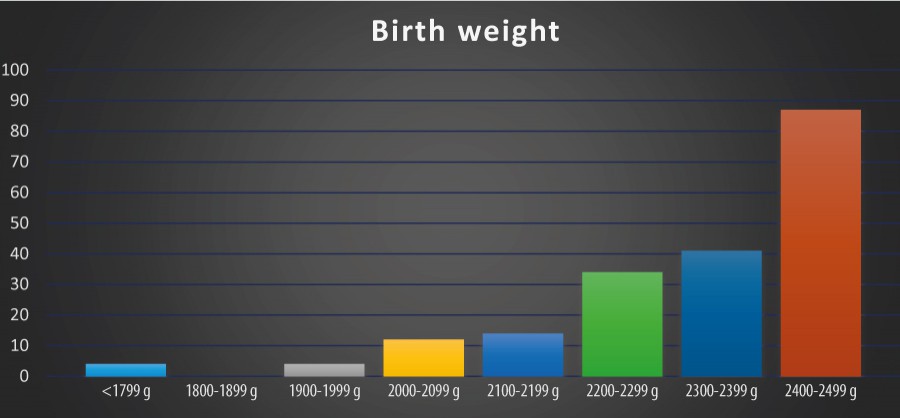
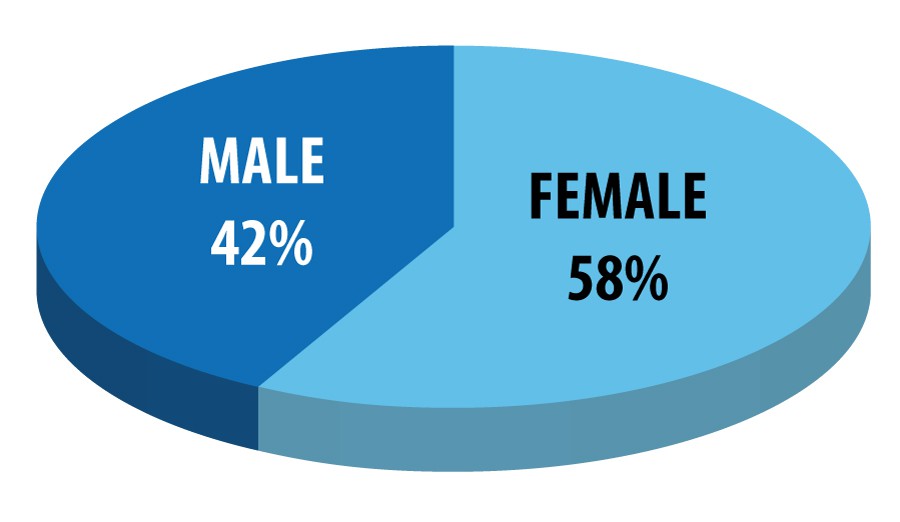
During the 3-year period of the study, 12987 births were registered in our hospital. The incidence of newborns with low birth weight was 1.5%, 196 cases being registered (Figure 1).The average weight at birth was 2302 grams, with the lowest value 1750 grams, and the female newborns were more affected (57.6%) – Figure 2.
Distribution by method of delivery: the delivery through C-section was predominant with 59% (Figure 3).
Regarding the fetal status at birth, 4 cases received a 1-minute Apgar score of 1 and only 7 cases were appreciated with the maximum Apgar score; above 55% of the newborns received an Apgar score at birth of 9 (Figure 4).
The average of maternal age was 28.5 years, with the maximum value 43 years, and the youngest patient was 14 years old.
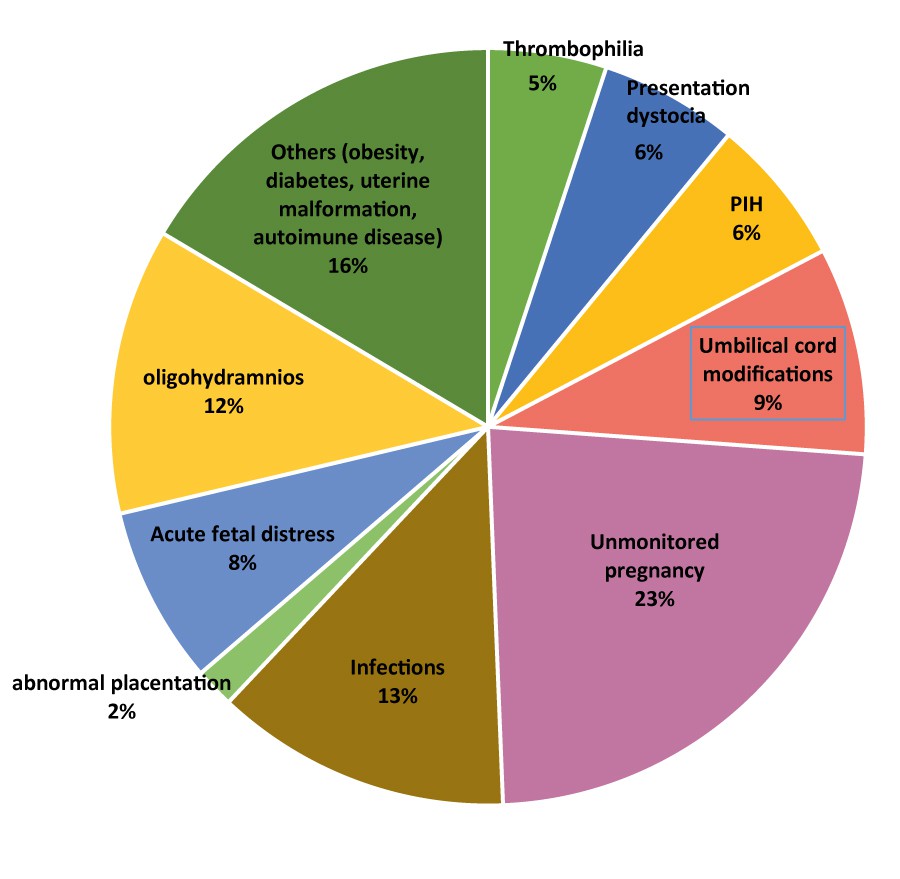
The pregnancies that were not followed by a specialist had an important proportion in our studied population. Also, conditions as obesity, diabetes, uterine malformation and autoimmune diseases were present in a significant percent. Above that, we considered important for study factors like thrombophilia, pregnancy-induced hypertension (PIH), umbilical cord modification (here were included true knot of the umbilical cord and double, triple or quadruple circular of the umbilical cord), abnormal placentation with placenta previa and adherent placenta, but the proportion of this enumerated condition was low (Figure 5).


Discussion and conclusion
No treatment is known to bring benefits in fetal growth restriction(14). A correct assessment of the fetal status and appropriate timing of delivery, alongside the recognition of factors that can lead to small fetuses represent the basis of the management. The worldwide incidence of fetal growth restriction is considered to be about 10 percent for small for gestational age newborns. In our study, we obtained a slightly low incidence of small for gestational age at term babies.
Only four newborns at term weighted at birth less than 1800 grams, the majority of our study population being rated as weighting between 2400-2499 grams.
There was a small difference between the ways of delivery, the C-section being predominant, with 59%. According to the latest suggestions for management in fetal growth restriction(15), labor induction is recommended at 40 weeks. From stage II to stage IV of fetal growth restriction, close monitoring at every 24-48 hours and delivery by caesarean section are recommended(15).
We expected for the extreme birth ages to influence the incidence of fetal growth restriction; however, the corresponding percentages of patients who gave birth at ages under 20 years or over 36 were low, 8.6% and 11.7%, respectively.
Surprisingly, the incidence of placental condition (placenta previa and adherent placenta) was only 2% within the studied group, also the pregnancy-induced hypertension was present only in 6% of cases.
The highest percentage (23%) among all registered associated conditions was represented by the unmonitored pregnancy (Figure 5). The suitable observation here is that for these pregnancies a proper differential diagnosis between constitutional small newborns and pathological small ones was impossible, considering the lack of any ultrasound monitorization during pregnancy and a poor social status involving nutritional deficiencies that could justify a late-onset of fetal growth restriction. The second in the order of decreasing prevalence were the maternal infections (13%), here being included beside classical urogenital infections with frequent appearance in pregnancy, the infection with HIV and the infection with hepatitis B and hepatitis C viruses.
The cases with oligohydramnios (12%) reflect a chronic fetal distress; a meta-analysis conducted by Chauhan SP et al.(16) concluded that a reduced amniotic fluid index is associated with an abnormal 5-minute Apgar score, but no association with perinatal death of small for gestational age was demonstrated.
In conclusion, fetal growth restriction requires an accurate diagnosis with a clear distinction of constitutional small fetuses by the abnormal small ones. Ultrasound monitoring is mandatory for the diagnosis and the assessment of the fetal status.
Bibliografie
1. Resnik R. Fetal growth restriction: Evaluation and management. Obstetrics & Gynecology 2002; 99(3)3: 490–496.
2. Unterscheider J, Daly S, Geary MP, et al. Optimizing the definition of intrauterine growth restriction: the multicenter prospective PORTO Study. Am J Obstet Gynecol 2013; 208:290.e1.
3. Gardosi J. New definition of small for gestational age based on fetal growth potential. Horm Res 2006; 65 Suppl 3:15.
4. Mendez H. Introduction to the study of pre- and postnatal growth in humans: a review. Am J Med Genet 1985; 20:63.
5. Crovetto F, et al. Performance of first-trimester integrated screening for early and late small for gestational age newborns. Ultrasound Obstet Gynecol 2013 (E-pub ahead of print).
6. Baschat AA, et al. Predictors of neonatal outcome in early-onset placental dysfunction. Obstet Gynecol 2007; 109:253-261.
7. Kady S, Gardosi J. Perinatal mortality and fetal growth restriction. Best Pract Res Clin Obstet Gynaecol 2004; 18:397-410.
8. Grivell RM, Wong L, Bhatia V. Regimens of fetal surveillance for impaired fetal growth. Cochrane Database Syst Rev 2012; CD007113.
9. Figueras F, et al. Predictiveness of antenatal umbilical artery Doppler for adverse pregnancy outcome in small-for-gestational-age babies according to customised birthweight centiles: a population-based study. BJOG 2008;115:590-594.
10. Eixarch E, et al. Neurodevelopmental outcome in 2-year-old infants who were small-for-gestational age term fetuses with cerebral blood flow redistribution. Ultrasound Obstet Gynecol 2008;32:894-899.
11. Gramellini D, et al. Cerebral-umbilical Doppler ratio as a predictor of adverse perinatal outcome. Obstet Gynecol 1992;79:416-420.
12. Hecher K, et al. Fetal venous, intracardiac, and arterial blood flow measurements in intrauterine growth retardation: relationship with fetal blood gases. Am J Obstet Gynecol 1995;173:10-15.
13. Fouron JC, et al. The relationship between an aortic isthmus blood flow velocity index and the postnatal neurodevelopmental status of fetuses with placental circulatory insufficiency. Am J Obstet Gynecol 2005; 192; 497-503.
14. Gulmezoglu AM, Hofmeyr GJ. Plasma volume expansion for suspected impaired fetal growth. Cochrane Database Syst Rev 2000; CD000167.
15. Figueras F., Gratacós E. Update on the Diagnosis and Classification of Fetal Growth Restriction and Proposal of a Stage-Based Management Protocol, Fetal Diagn Ther 2014; 36:86-98.
16. Chauhan SP, et al. Perinatal outcome and amniotic fluid index in the antepartum and intrapartum periods: a meta-analysis. Am J Obstet Gynecol 1999; 181:1473-1478.
Articole din ediția curentă
MATERNAL-FETAL MEDICINE
Screening pentru trombofilie ereditară al gravidelor internate în Spitalul Universitar de Urgenţă Bucureşti
Diana Ioana Voicu, Roxana-Elena Bohîlţea, Oana Bodean, Octavian Munteanu, Eugen Radu, Anda Băicuș, Irina Horhoianu, Elvira Brătilă, Sorin Vasilescu, Costin Berceanu, Oana Săndulescu, Livia Traşcă, Monica-Mihaela Cîrstoiu
Trombofilia reprezintă tendinţa crescută la hipercoagulabilitate. Patologia poate fi ereditară sau dobândită. În timpul sarcinii c...
EDITORIAL
PERINATOLOGIA, între evoluţia spectaculoasă, realitatea actuală și așteptările viitoare
Simona Vlădăreanu
Privind în ansamblul practicii obstetricale și neonatale, este evident faptul că, pentru mai bine de jumătate de secol, medicina materno-fetală a parcurs etape cu adevărat remarcabile....
CASE REPORT
Administrare minim invazivă de surfactant la nou-născutul cu greutate extrem de mică la naştere (ELBW) - prezentare de caz
Manuela Cucerea, Laura Suciu, Marta Simon
În ciuda numeroaselor controverse privind abordarea sindromului de detresă respiratorie prin deficit de surfactant (SDRDS) la prematurii ELBW, în scopul reducerii riscului de boală pulmonară cronică s...Articole din edițiile anterioare
MATERNAL-FETAL MEDICINE
Screening pentru trombofilie ereditară al gravidelor internate în Spitalul Universitar de Urgenţă Bucureşti
Diana Ioana Voicu, Roxana-Elena Bohîlţea, Oana Bodean, Octavian Munteanu, Eugen Radu, Anda Băicuș, Irina Horhoianu, Elvira Brătilă, Sorin Vasilescu, Costin Berceanu, Oana Săndulescu, Livia Traşcă, Monica-Mihaela Cîrstoiu
Trombofilia reprezintă tendinţa crescută la hipercoagulabilitate. Patologia poate fi ereditară sau dobândită. În timpul sarcinii c...
GYNECOLOGY
Evaluarea răspunsului imun postvaccinal anti-HPV la populația generală cu şi fără antecedente de infecție virală – review al literaturii
Robert Costin, Octavian Munteanu, Monica-Mihaela Cîrstoiu
Vaccinurile împotriva virusului papilomatozei umane (HPV) induc o protecție imună puternică și de lungă durată, reducând semnificativ bolile asociate cu HPV. ...
OBSTETRICS


