Psychoactive substances are an important public health issue, especially with the upward trend in the number of cases in recent years. The COVID-19 pandemic, with its major impact on lifestyle, has brought an additional level of stress to the population and, thus, has led to changes in substance use-related caseloads in terms of number of admissions, but especially in terms of severity of symptoms at the time of presentation to mental health services. These changes accentuate the need to increase the capacity of substance abuse services to prepare the healthcare system for an increasing number of new cases with severe symptoms at presentation, including potential somatic, sometimes life-threatening problems. The lack of specific treatment, with the exception of opioids, means that a multidisciplinary specialist approach is required for the management of drug use cases and raises the need for specialized staff and the establishment of drug addiction wards across the country where there is currently no such coverage.
Internările consumatorilor de droguri în spitalele de psihiatrie din România (2018-2021)
Admissions of psychoactive substance users in Romanian psychiatric hospitals (2018-2021)
First published: 30 iunie 2022
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Psih.69.2.2022.6627
Abstract
Rezumat
Substanţele psihoactive reprezintă o problemă importantă de sănătate publică, în special ţinând cont de trendul ascendent al numărului de cazuri din ultimii ani. Pandemia de COVID-19, prin impactul major asupra stilului de viaţă, a adus un nivel suplimentar de stres la nivelul populaţiei şi astfel a determinat modificări în ceea ce priveşte cazuistica legată de consumul de substanţe ca număr de internări, dar mai ales ca severitate a simptomatologiei din momentul prezentării în serviciile de sănătate mintală. Aceste modificări accentuează nevoia de a suplimenta capacitatea serviciilor de toxicomanii în vederea pregătirii sistemului medical cu un număr tot mai crescut de cazuri noi şi cu simptomatologii severe la prezentare, inclusiv cu potenţiale probleme somatice, uneori ameninţătoare de viaţă. Lipsa unui tratament specific, cu excepţia opioidelor, face ca pentru managementul cazurilor de consum să fie necesară o abordare multidisciplinară de specialitate şi ridică nevoia personalului specializat şi de înfiinţare a secţiilor de toxicomanii pe teritoriul ţării, acolo unde nu există momentan acoperire în acest sens.
Introduction
One of the public health problems worldwide is the use of psychoactive substances, in particular because of the constant increase in consumption and the diversity of substances used and their effects on health. According to the United Nations Office on Drugs and Crime (UNODC)(1), the number of drug users is increasing worldwide, with estimates currently putting the number of users at around 270 million, an increase of 22% since 2010.
The COVID-19 pandemic has brought significant changes in the trafficking and use of psychoactive substances. Even though drug trafficking decreased significantly at the beginning of the pandemic, it has surpassed the pre-pandemic level and managed to circumvent the restrictions imposed in this context. Another pandemic change in drug use is the increasing use of cannabis and sedatives for self-medication in the context of pandemic stress and government restrictions(2). Also, the economic implications of the pandemic and the conflict in Ukraine increase the risk of future illicit drug use, especially in low‑ and middle-income countries(1).
Drug use has increased or at least stagnated in most countries during the pandemic, but there are exceptions, such as that for some psychoactive substances, in some countries, a decrease in use has been observed, with the only almost constant increases being noted for sedatives and pharmaceutical opioids(3).
These changes are putting additional pressure on health systems worldwide, especially in low- and middle-income countries that are already stretched by the pandemic. An estimated 36 million people suffer from drug-related mental disorders and this number is expected to increase in the coming years(4). However, the treatments available are limited, to date the only substances with specific treatment being opioids, the pathology generated by the rest being treated symptomatically.
In the present study, we aim to analyze the evolution of the number of psychoactive substance users admitted to psychiatric services in Romania and the average duration of hospitalization (DMS) as an indirect indicator of the severity of their mental pathology.
Methodology
Data were taken from the Center for Health Services Research and Evaluation’s 2018-2022 national public database(5). Diagnostic groups according to the current DRG classification in Romania were used, and data were reported quarterly, from quarter 1 (Q1) to quarter 4 (Q4) of each year.
For the purpose of this article, two DRG groups were selected:
V3041 – Opioid use disorder and dependence.
V3050 – Other drug use disorders and dependence.
For these groups, the number of cases per quarter and the average length of stay (ALS) were analyzed.
Data analysis was performed using the Excel application from the Microsoft Office 2021 package.
Results
In Romania, in the last four years, 2657 patients were hospitalized with mental pathology caused by psychoactive substances. The overall direction of the number of cases is decreasing, with two minimum points, both in the initial period of the pandemic (Q2 of 2020), when the state of emergency was instituted, followed by Q4, which coincided with the second wave of the pandemic.
The average duration of hospitalization followed a relatively constant trend, including in the initial period of the pandemic, but with an increase during 2021, with a peak in Q4 of the same year.
Opioids
Opioid use has seen a general downward trend from 2018 – 271 cases admitted (an average of 22.6 cases per month) to 151 cases (12.6 cases per month) in 2021. The period with the lowest number of admissions in the context of opioid consumption was in quarters 2 and 4 of 2020, with an average of 8.7 admissions per month.
In terms of the average length of stay, it remained approximately constant during 2018-2019 (4.42 days per hospitalization), but increased in the pandemic years (9.59 days per hospitalization). The lowest average length of stay can be observed in the second quarter of 2019 and the highest in the last quarter of 2021.
Non-opioid psychoactive substance
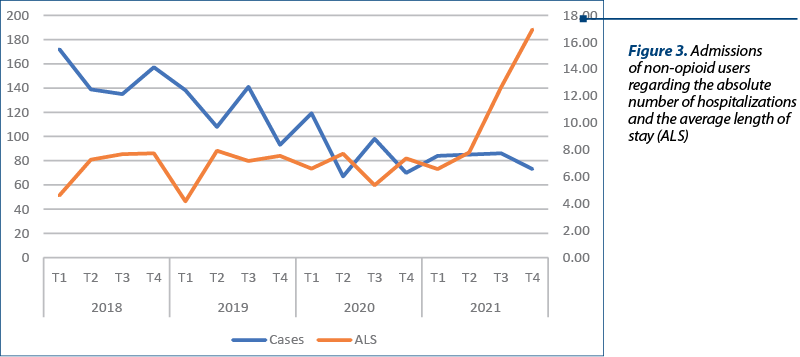
The number of cases hospitalized with a diagnosis due to the use of other psychoactive substances shows a similar trend to the use of opioids. In 2018, the average number of cases was 50.25 per month, this average decreasing steadily until 2021, when the average number of admissions was 27.33 per month. Unlike opioid use, in this case, a period with a low number of admissions cannot be delimited, but in the second quarter of 2020 there was registered the lowest number of admissions – 67 per quarter, an average of 22.33 per month.
The average length of stay for non-opioid psychoactive substances other than opioids remained relatively constant over the period studied, averaging 6.83 days per hospitalization. During quarters 3 and 4 of 2021, the average length of stay increased to 14.80 days per hospitalization, peaking at 16.95 days per hospitalization in quarter 4.
Discussion and conclusions
The use of psychoactive substances is constantly changing, both in general and in terms of specific substances. In recent years, a general trend of increasing cannabis use has been observed, probably due to legalization in various countries, but also to the increasing perception of cannabis as an easy drug or even as a medicinal plant without negative effects. At the same time, the use of opioids, especially prescription opioids, is on a downward trend worldwide(4).
The results obtained in our study are confirmed by the worldwide decrease in opioid consumption. However, the same decrease can be observed for other psychoactive substances. Although the number of cannabis users may be increasing in our country, it may not be pronounced enough to increase the total number of admissions to psychiatric services. Also, the fact that patients who are admitted present severe symptoms, often of psychotic intensity, raise the question of comorbidity between psychoactive substance abuse/dependence and major psychiatric disorders (schizophrenia, bipolar disorder). In this situation, it is possible to underdiagnose substance use, especially in situations where there are no anamnestic sources to determine the definite substance use and the patient does not cooperate in testing by available means, often urine tests(5).
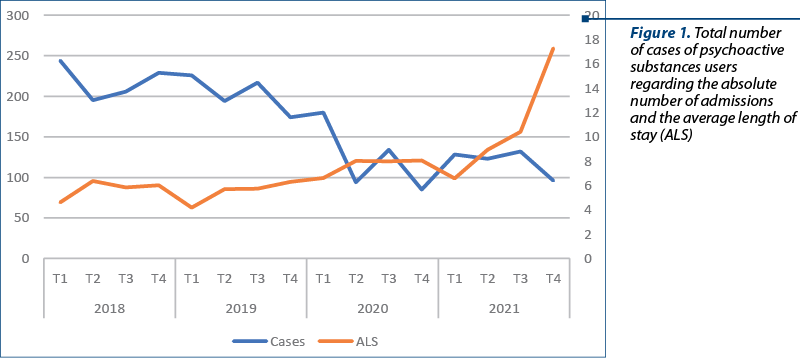
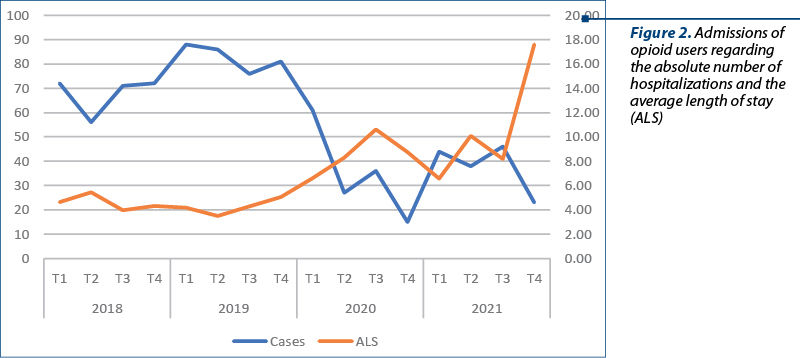
At the beginning of the pandemic, in quarters 2-4 of 2020, we observed a marked decrease in the number of admissions with diagnoses related to opioid use, followed by a slight increase but not reaching pre-pandemic levels. This decrease could be due to restrictions imposed during the early period of the pandemic, limiting the mobility of users, but also the mobility and access to medical services of patients who obtained opioids on prescription due to associated somatic pathologies(6).
Although the overall trend in the number of admissions is decreasing, the average length of stay has shown a marked increase, especially in 2021, for both opioids and other psychoactive substances. This steep increase, up to twofold, in the average length of stay denotes an increase in the severity of healthcare attendance. The period with the highest increase in hospitalization duration, the fourth quarter of 2021, coincided with the relaxation of the restrictions imposed so far during the pandemic, but also with a marked “psychological relaxation” of the general population, despite the legislation, followed by the resumption of social events and a general increase in mobility and, therefore, access to psychoactive substances(7).
Given that detoxification services are located in hospitals, state or private, the severity of cases of mental disorders resulting from substance use includes intoxication and addiction, so in the following period there is the possibility of a wave of withdrawal pathologies. Even though in the case of opioids there is a specific treatment for this pathology, in the case of other psychoactive substances there is a deficit, so that the implications of substance intoxication, especially those with unknown structures, can have a major impact on somatic health, with possible life-threatening complications. Also, in the context of intoxication with unknown substances, the therapeutic approach is very limited, not knowing the possible drug interactions that may occur with the consumed substances.
The situation of the number of psychoactive substance users requiring admission to psychiatric services is relatively balanced in Romania with a constant downward trend in the last four years, a trend accentuated as a result of the pandemic. However, the severity of the pathology, indirectly indicated by the average length of stay, raises concerns, increasing steeply in the last two quarters of 2021 for both opioids and non-opioid psychoactive substances.
Given that the pathology caused by intoxication does not require a long duration of hospitalization, improving in the first days, we can infer that the average duration of hospitalization is increased due to withdrawal from psychoactive substances or psychotic disorders caused by them. Thus, there is a possibility that this increase is a result of an increase in consumption but which has not produced symptoms requiring hospitalization. In this situation, we can assume the persistence of an increased level of consumption of active substances in the general population which will lead to an increasing number of cases hospitalized in the future as a result of pathologies caused by these substances.
Changes in the pattern of use and the severity of substance use disorders have a significant potential to overburden and destabilize the mental health systems in Romania, especially in regions where there are major deficits in drug-related health services. It is, therefore, necessary to implement an action plan to prevent a future wave of pathologies caused by the consumption of psychoactive substances, through the establishment of profile centers, the overspecialization of medical staff to optimize the management of patients, and a well-conceptualized prevention project to have a significant impact on the general population.
Bibliografie
-
UNODC I. World Drug Report. United Nations, New York, NY. 2021.
-
Blithikioti C, Nuño L, Paniello B, Gual A, Miquel L. Impact of COVID-19 lockdown on individuals under treatment for substance use disorders: Risk factors for adverse mental health outcomes. Journal of Psychiatric Research. 2021 Jul 1;139:47-53.
-
Farhoudian A, Radfar SR, Mohaddes Ardabili H, Rafei P, Ebrahimi M, Khojasteh Zonoozi A, De Jong CA, Vahidi M, Yunesian M, Kouimtsidis C, Arunogiri S. A global survey on changes in the supply, price, and use of illicit drugs and alcohol, and related complications during the 2020 COVID-19 pandemic. Frontiers in Psychiatry. 2021;12:646206.
-
Ignaszewski MJ. The epidemiology of drug abuse. The Journal of Clinical Pharmacology. 2021 Aug;61:S10-7.
-
Smith MJ, Thirthalli J, Abdallah AB, Murray RM, Cottler LB. Prevalence of psychotic symptoms in substance users: a comparison across substances. Comprehensive Psychiatry. 2009 May 1;50(3):245-50.
-
Reinstadler V, Ausweger V, Grabher AL, Kreidl M, Huber S, Grander J, Haslacher S, Singer K, Schlapp-Hackl M, Sorg M, Erber H. Monitoring drug consumption in Innsbruck during coronavirus disease 2019 (COVID-19) lockdown by wastewater analysis. Science of the Total Environment. 2021 Feb 25;757:144006.
-
Harris LC. Breaking lockdown during lockdown: a neutralization theory evaluation of misbehavior during the Covid 19 pandemic. Deviant Behavior. 2020 Dec; 22:1-5.
Articole din ediţiile anterioare
Spitalul de Psihiatrie Voila - Câmpina – studiu de caz
În contextul economico-social şi legislativ de astăzi, managerul unui spital de psihiatrie are, dincolo de atribuţiile și obligaţiile din contractu...
Trauma psihică a expunerii la infecţia cu SARS-CoV-2
După mai mult de un an de expunere globală la COVID-19, la consecinţele acesteia asupra stării de sănătate şi la măsuri variabile de limitare a răs...
Riscul de suicid în timpul pandemiei de COVID-19
The sensitive topic of suicide risk during the COVID-19 pandemic entails two relevant components.
Adicţiile în perspectiva pragmatică a ICD-11
Se inventariază modificările aduse de noua ediţie a ICD faţă de ediţia precedentă, precum şi în comparaţie cu predecesorul său temporal, DSM-5 (201...