Coronavirus spectrum infections (especially with SARS-CoV-2) particularly influence the thyroid axis, with both thyrotoxicosis as well as suppression of thyroid function, thus determining severe pregnancy and perinatal outcomes. However, the role of the thyroid autoimmunity and SARS-CoV-2 viral load in COVID-19-related thyroid dysfunction is unclear.
Rezultate la gravidele care asociază tiroidită autoimună şi COVID-19
Outcomes in pregnant women associating autoimmune thyroiditis and COVID-19
First published: 22 martie 2021
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Gine.31.1.2021.4326
Abstract
Rezumat
Infecţiile cu agenţii patogeni din familia Coronaviridae (în special SARS-CoV-2) influenţează cu precădere axul tiroidian, manifestându-se atât prin tireotoxicoză, cât şi prin suprimarea funcţiei tiroidiene, cu rezultate severe perinatale. Cu toate acestea, rolul autoimunităţii tiroidiene şi al încărcăturii virale de SARS-CoV-2 în disfuncţia tiroidiană legată de COVID-19 nu este clar.
Introduction
The women who are positive for thyroid autoimmunity (TAI) display antibodies as markers of an immune disease and have also a predisposition to a faulty thyroid function during gestation(1).
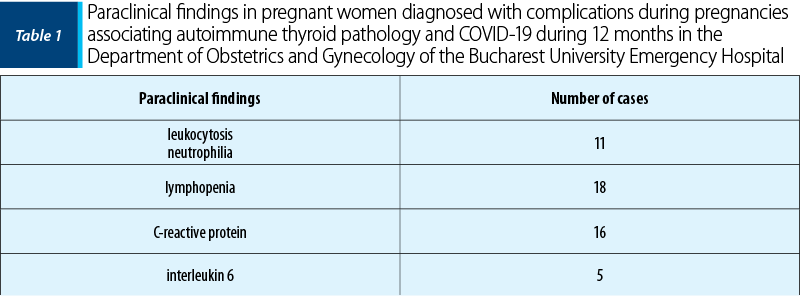
During pregnancy, specific physiological and immunological changes cause an increased susceptibility to viral infections, including to those with SARS-CoV-2. Regarding the paraclinical changes, in the case of pregnant women, there could be identified as markers leukocytosis accompanied by an elevated neutrophil ratio and lymphopenia. In many cases, a high level of C-reactive protein (CRP) has been noticed. Other results revealed by laboratory tests were elevated interleukin 6 levels and low albumin levels(2).
Hence, the inclusion criteria were: evaluation of the thyroid function and biochemical, immunological and inflammatory markers in a cohort of pregnant women, with the severity of COVID-19 ranging from mild to moderate.
Thyroid hormones are implicated in the regulation of innate immune response(3). Therefore, the excess or deficiency of thyroid hormones levels observed in thyroid disease will lead to dysregulation of innate immune response. Meanwhile, the innate immune response is also thought to contribute significantly in the pathogenesis of COVID-19, in the front lines of body defense systems to fight against SARS-CoV-2. The dysregulation of innate immune response, as evidenced by higher levels of neutrophils, increased levels of CD14b monocytes and macrophages, decreased levels of NK cells and by increased levels of complement, was significantly associated with severe forms of COVID-19(4). Increased levels of proinflammatory cytokines, such as TNF-alfa and IL-6 were observed in patients with thyroid diseases(5,6). Increased levels of these cytokines were also observed in patients with severe COVID-19 and correlated with the development of severe outcomes(7). Finally, some patients, especially those suffering from subacute thyroiditis, were taking corticosteroids as part of their medications(8), and meta-analyses showed that corticosteroid treatment in COVID-19 patients was associated with higher mortality, longer length of hospital stay, and higher rate of bacterial infections.
Materials and method
We conducted a retrospective observational study focused on pregnant women with autoimmune thyroiditis evaluated in our Department of Obstetrics and Gynaecology, who were also associating the infection with SARS-CoV-2, during 12 months. The studied population consisted in 20 pregnancies, out of which nine were marked by thyroid pathology.
A diagnosis of SARS-CoV-2 infection was considered if the patient had a positive polymerase chain reaction (PCR) test on samples collected from the respiratory system.
The presence of thyroid antibodies (ATAs), anti-thyroglobulin (anti-TG) and anti-thyroid peroxidase (TPOAb) was also taken into account when analyzing the pregnant patients suffering from COVID-19. We also measured serum levels of thyroid stimulation hormone (TSH), free thyroxine (fT4), and free T3 (fT3).
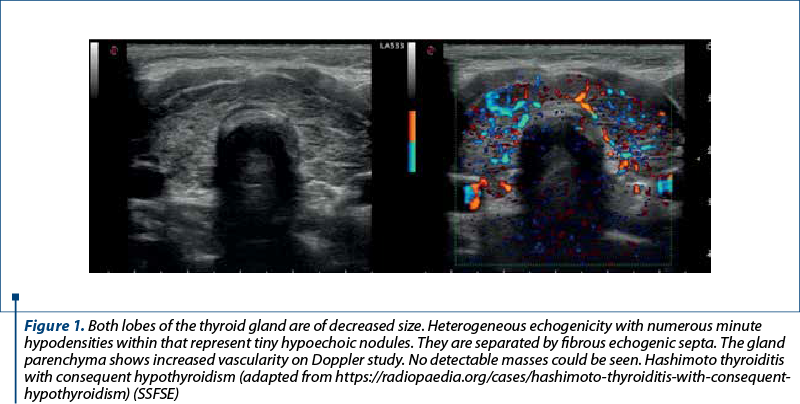
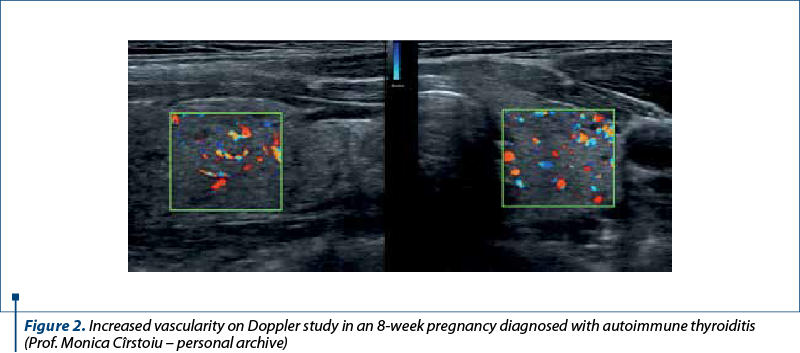
The thyroid was monitored periodically throughout the pregnancy using also ultrasound, though no changes were observed after contracting the infection with SARS-CoV-2. We used the measurement of the thyroid volume, thus providing an early diagnosis of diffuse pathologies and the detection and characterization of nodular lesions. Determining the volume of the thyroid is one of the most common purposes for which it is resorted to thyroid ultrasound, hypertrophy of the thyroid gland being the most common thyroid pathology in our geographical area. Regarding the diagnosis of diffuse thyroid diseases, thyroiditis occupies the first place. In acute and subacute thyroiditis, the clinical picture is suggestive of the diagnosis, the importance of ultrasound consisting in monitoring the evolution of the disease under treatment.
When collecting the data from the electronic health records, we took into account the comorbidities, the clinical characteristics of the infection and the laboratory tests data. The informed consent was obtained from all patients.
Results
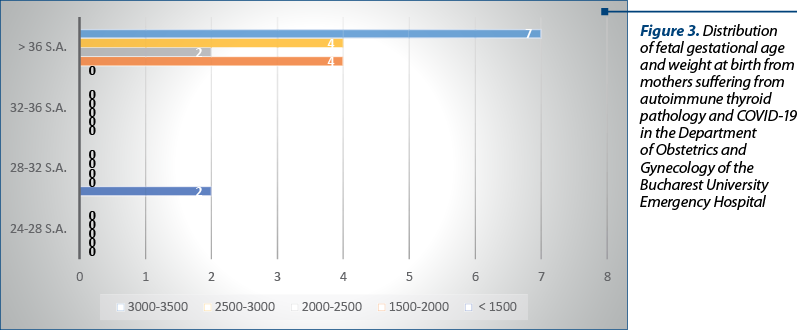
We identified 20 women with COVID-19 between the 1st of January 2020 and the 31st of January 2020. In the first stage of statistical evaluation, descriptive tests were applied while monitoring the presence of risk factors and complications in the studied groups. The main parameters analyzed were: the fetal weight at birth and the Apgar score, to assess the impact on the fetal outcome (Figure 3), as well as the risk of developing preeclampsia, intrauterine growth restriction, preterm prelabour rupture of membranes, length of hospitalization, dexamethasone and/or supplementary oxygen requirements, and premature birth.
The pregnancy outcomes observed were as follows:
-
preterm birth (<37 weeks of gestation) = 5 cases
-
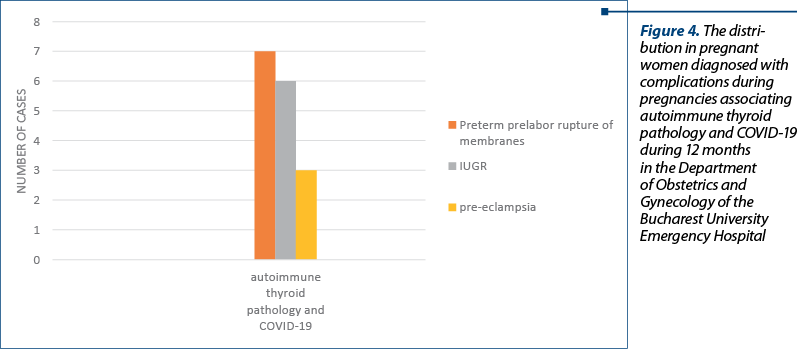
preeclampsia = 3 cases
-
preterm prelabor rupture of membranes = 7 cases
-
fetal growth restriction = 6 cases
-
caesarean mode of delivery = 13 cases.
-
The perinatal outcomes observed were:
-
Apgar score <7 = 7 cases
-
admission to the Neonatal Intensive Care Unit = 5 cases
-
perinatal death, including both stillbirth and neonatal birth = 2 cases.
Discussion
Regarding the statistics of the two pathologies affecting the pregnant woman, the data collected in our study are scarced. The study we conducted has several limitations:
-
retrospective single-center study
-
small sample – 20 patients
-
a short period of time.
Also, another limitation is the fact that the hospital in which we conducted our research is not primary designated to treat exclusively pregnant women with COVID-19.
The particular situation of pregnant women requires that the hospital units adopt the ISUOG recommendations in case of SARS-CoV-2 infections(9): the management of pregnant women with confirmed COVID-19 in designated tertiary hospitals; the setup of a negative-pressure isolation rooms for safe labor, delivery and postpartum care; the inclusion of CT scan in the workup of pregnant women with suspected, probable or confirmed COVID-19; the treatment of suspected/probable cases in isolation and the management of confirmed cases in a negative-pressure isolation room; the management by a multidisciplinary team of COVID-19 pregnant women; the individualization of timing and mode of delivery according to the clinical status of the patient, gestational age and fetal condition; the separation of the mother and the newborn if the first one is severely or critically ill, or stopping the breastfeeding and colocation if the patient is asymptomatic or mildly affected.
Any preexisting autoimmune pathology causes an increased vulnerability to respiratory viral infections, leading to an evolution with severe forms of the disease. The acute viral infections during pregnancy expose both the mother and the fetus to a wide range of side effects. There is an increased risk of vertical transmission in the presence of a severe form of the disease that can lead to miscarriage, premature birth, intrauterine growth restriction and maternal morbidity. The fear is that even in the absence of vertical transmission, the mother’s immune response to the infection could trigger a fetal inflammatory response, resulting in the damage of the central nervous system and the respiratory system of the fetus.
The information currently available is insufficient to outline the consequences of the disease on pregnancy and, conversely, the consequences of pregnancy on how the disease would further evolve(10).
Conclusions
The negative effect of autoimmune pathologies, more precisely of autoimmune thyroiditis, on pregnancy is well known. It was important to note the changes in the pathological context and the consequences of contracting SARS-CoV-2.
The group of patients studied, with the aforementioned limitations, did not reveal elements to establish correlations about the consequences of autoimmune thyroiditis on pregnancy, following a SARS-CoV-2 infection.
Further extensive studies are needed in order to obtain relevant medical data on the two concomitant pathologies associated with pregnancy.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
Stagnaro-Green A. Thyroid antibodies and miscarriage: where are we at a generation later? J Thyroid Res. 2011;2011:841949.
-
WHO. Statement on the second meeting of the International Health Regulations (2005). Emergency Committee regarding the outbreak of novel coronavirus (2019-nCoV). Available at: https://www.who.int/news/item/23-01-2020-statement-on-the-meeting-of-the-international-health-regulations-(2005)-emergency-committee-regarding-the-outbreak-of-novel-coronavirus-(2019-ncov)
-
Montesinos MDM, Pellizas CG. Thyroid hormone action on innate immunity. Front Endocrinol. 2019;10:350.
-
McKechnie JL, Blish CA. The innate immune system: fighting on the front lines or fanning the flames of COVID-19? Cell Host Microbe. 2020;27(6):863-9.
-
Figueroa-Vega N, Alfonso-Perez M, Benedicto I, Sanchez-Madrid F, Gonzalez-Amaro R, Marazuela M. Increased circulating pro-inflammatory cytokines and Th17 lymphocytes in Hashimoto’s thyroiditis. J Clin Endocrinol Metab. 2010;95(2):953-62.
-
Lv L-F, Jia H-Y, Zhang H-F, Hu Y-X. Expression level and clinical significance of IL- 2, IL-6 and TGF-ß in elderly patients with goiter and hyperthyroidism. Eur Rev Med Pharmacol Sci. 2017;21(20):4680-6.
-
Monti S, Balduzzi S, Delvino P, Bellis E, Quadrelli VS, Montecucco C. Clinical course of COVID-19 in a series of patients with chronic arthritis treated with immunosuppressive targeted therapies. Ann Rheum Dis. 2020;79(5):667–8.
-
Stockman LJ, Bellamy R, Garner P. SARS: systematic review of treatment effects. PLoS Med. 2006;3(9):e343.
-
Poon LC, Yang H, Dumont S, Lee JCS, Copel JA, Danneels L, Wright A, Da Silva Costa F, Leung TY, Zhang Y, Chen D, Prefumo F. ISUOG Interim Guidance on coronavirus disease 2019 (COVID-19) during pregnancy and puerperium: information for healthcare professionals – an update. Ultrasound Obstet Gynecol. 2020;55(6):848-62.
-
Mullins E, Evans D, Viner RM, O’Brien P, Morris E. Coronavirus in pregnancy and delivery: rapid review. Ultrasound Obstet Gynecol. 2020;55(5):586-92.
Articole din ediţiile anterioare
Preeclampsia şi boala parodontală maternă
Preeclampsia este una dintre complicaţiile sarcinii. Anaerobii Gram-negativi din pungile parodontale ale gravidelor sugerează că boala parodontal...
Dorsalgia joasă la gravide şi lăuze. Principii de reabilitare medicală
Dorsalgia joasă asociată sarcinii reprezintă o patologie importantă, însă deseori neglijată, care poate avea un potenţial impact negativ asupra...
Trombocitopenia maternă în sarcină
Cu toate că de cele mai multe ori nu pune în pericol viaţa pacientei, trombocitopenia în sarcină poate fi expresia unei serii de patologii care nec...
Contracepţia de urgenţă, puţin cunoscută şi utilizată - studiu multicentric naţional
Contracepţia de urgenţă se referă la un grup de metode contraceptive care, folosite după contactul sexual neprotejat într-un interval definit de ti...