Semne ecografice timpurii în agenezia de corp calos
Early sonographic signs in agenesis of the fetal corpus callosum
Abstract
Objectives. Although the agenesis of corpus callosum is currently a second-trimester diagnosis, it is a worthwhile pursuit to lower the gestational age at which this pathology should be at least suggested, if not diagnosed. Materials and method. We performed an ultrasound examination (2D and 3D) on women with a sigleton or twin pregnancy at 12 to 14 weeks of gestation. Images with measurements of midbrain and falx cerebri were acquired and their ratio computed, along with 3D volume with power Doppler images of the pericallosal arteries. We also performed a follow-up scan at 20-22 weeks of gestation in order to confirm the absence of the corpus callosum. Results. Nineteen fetuses with high suspicion on the first trimester were found with agenesis of corpus callosum at the second-trimester scan. Conclusions. Ultrasound measurements of midbrain/falx cerebri with calculated ratio and pericallosal artery in the first trimester could be a matter of concern for agenesis of corpus callosum.Keywords
first-trimester scanagenesis of corpus callosummidbrainfalx cerebriratiopericallosal arteryRezumat
Obiective. Deşi agenezia de corp calos este un diagnostic stabilit în trimestrul al doilea, este un deziderat să scădem vârsta gestaţională pentru depistarea acestei patologii. Materiale şi metodă. S-au efectuat examinări ecografice 2D şi 3D la paciente gravide cu sarcină unică sau multiplă între săptămânile 12 şi 14. S-au obţinut măsurători ale mezencefalului şi falx cerebri şi s-a calculat raportul celor două, alături de examinarea power Doppler a arterei pericalosale. De asemenea, s-a confirmat, prin follow-up la 20-22 de săptămâni gestaţionale, absenţa corpului calos. Rezultate. Nouăsprezece feţi au fost descoperiţi cu diagnostic cert de agenezie de corp calos la morfologia de trimestrul al doilea. Concluzii. Măsurarea ecografică a mezencefalului/falx cerebri, calculul raportului celor două şi evidenţierea arterei pericalosale în trimestrul întâi pot prezice agenezia de corp calos, confirmată în trimestrul al doilea.Cuvinte Cheie
morfologie de trimestru întâiagenezie de corp calosdiencefalfalx cerebriraportarteră pericalosalăIntroduction
Corpus callosum is one of the most interesting and important yet unknown structures of the human brain. It is the one that interchanges sensory information between the left and the right hemispheres and connects them.
In the unlikely event of its absence (agenesis of corpus callosum), there are still some non-callosal commissures that apparently fulfill its function and therefore many individuals can be asymptomatic.
Because the corpus callosum is not fully formed until 19 to 21 weeks of gestation, the diagnosis of agenesis of corpus callosum by ultrasound before this period is very challenging.
The condition is suggested by the absence of cavum septum pellucidum (CSP) and the teardrop configuration of lateral ventricles with enlargement of the posterior horns between 18 and 37 weeks(1,2) (Figure 1).
The development of the corpus callosum begins between 12 and 18 weeks of gestation. It represents a thin band of white matter and it can be visualized in midsagittal or midcoronal views of the fetal brain(3).
Because most of the pregnant women with this pathology of the fetus choose the termination of pregnancy, we try to diagnose the agenesis of corpus callosum (ACC) as soon as possible, by measuring midbrain and falx cerebri diameters, computing their ratio, along with the discovery of the pericallosal artery at the end of the first trimester.
Materials and method
The study started in 2014 and included 12-14-week pregnant women who undertook first-trimester scan and also pregnancies with confirmed ACC during the second-trimester scan, where a midsagittal scan of the fetal brain(4) from the first trimester was available.
In the light of the results observed by Lachmann(5), where the midbrain diameter of ACC-confirmed cases was above the 95th percentile and the falx diameter was below the 5th percentile, we performed measurements of midbrain and falx cerebri diameter in mid sagittal view of the fetal brain, and we computed midbrain to falx cerebri ratio. Afterwards we performed descriptive statistics and stratified comparative analysis using the SPSS software package.

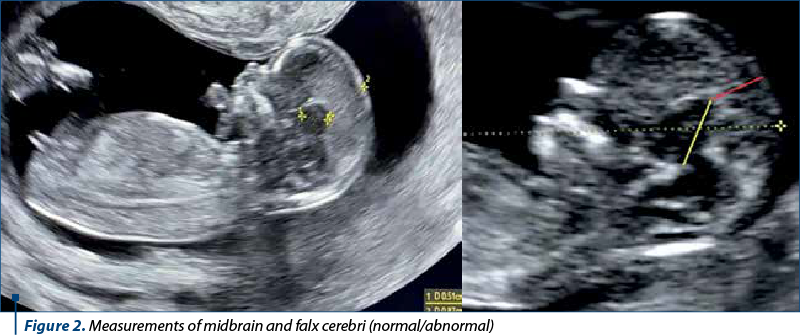
The examinations were performed by FMF certified sonographers in the 11-13 weeks scan on E8 Voluson GE machine. The measurements were represented by the diameter taken from the sphenoid bone to the echogenic falx for the midbrain, and the distance between the upper border of the midbrain and the skin of the fetal head for the falx (Figure 2). The ratio between the two structures was calculated.
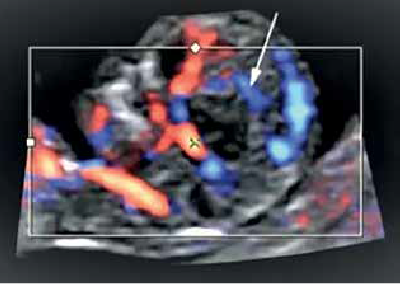
After this, the high-definition power Doppler was activated (set with a PRF of 0.3 kHz) and a 3D scan was performed to visualize the pericallosal arteries(6,7). Both mechanical and thermal indices were kept under 1 due to health and safety concerns (Figure 3).
Results
Overall, 1040 patients were included in the study, of which 23 were cases of confirmed agenesis of corpus callosum, with only 19 first-trimester scans available.
The crown-rump length (CRL) of the 19 fetuses was between 54 and 81 mm, with midbrain diameter from 6 to 10.5 mm and falx between 4.9 and 9.24 mm, with a higher than 1 ratio exceeding the normal limit, with one exception (0.93), in a case of a partial agenesis of the corpus callosum.
The whole length of the pericallosal artery was obtained (3.5 to 4.5 mm) in fetuses above 12 weeks of gestation who showed no evidence of abnormal brain findings(2).
The diagnosis of agenesis in all cases was made in the second trimester, between 21 and 24.5 weeks of gestation, as following: 15 complete ACC, 3 partial ACC, one hypoplastic CC, with 12 cases of associated pathology (CNS or extra CNS) and only 7 isolated ACC. We had a total of 15 births and 4 terminations of pregnancy (all of which had associated pathology).
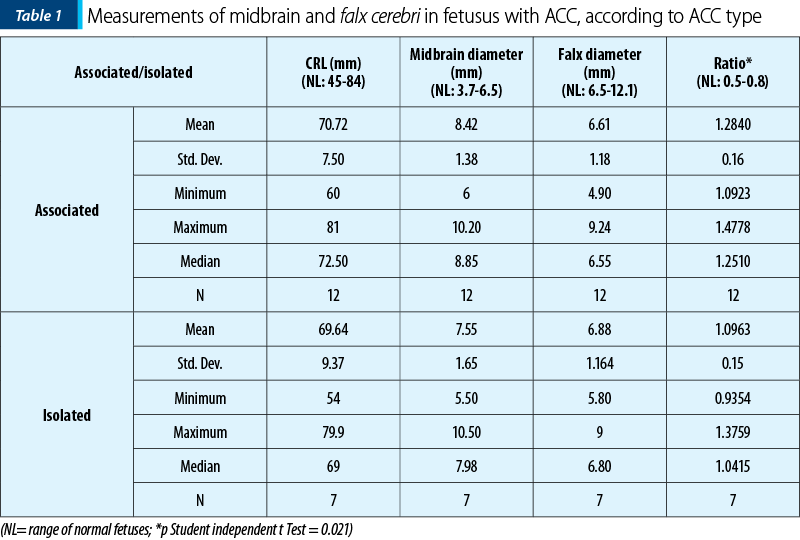
The midbrain/falx cerebri ratio of associated pathology cases of ACC was significantly (p=0.021) higher than those of isolated cases of ACC (1.28±0.16 versus 1.09±0.14), therefore the calculated ratio can be considered to predict the cases of associated pathology in agenesis of corpus callosum (Table 1).
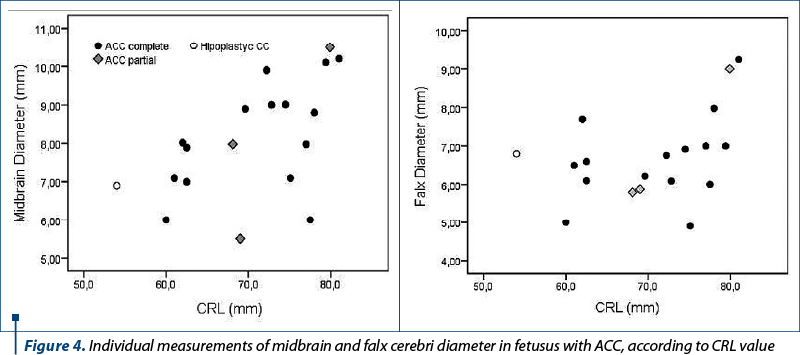
A medium significant positive correlation (r=0.566; p=0.011) was iddentified between CRL and midbrain diameter for all ACC cases. A significant correlation (r=0.523; p=0.045) was iddentified between CRL and midbrain diameter only for cases of complete ACC, and also a strong significant correlation (r=0.99; p=0.030) was found between CRL and falx diameter only for cases of partial ACC (Figure 4).
Discussion
Compared to normal fetuses, in fetuses with ACC the midbrain diameter is higher, the falx diameter is lower and midbrain to falx ratio is higher than 1.
The findings are compatible with the work of Lachmann et al., and we can say that in the midsagittal view of the brain in the first trimester there are measurable abnormalities that could suggest no forming of the corpus callosum.
On the other hand, we failed to observe the pericallosal artery in the first trimester, with good results in the second trimester, as we found a normally developed corpus callosum(8).
Although the presence of the feeding vessel should anticipate the development of the target organ, so the pericallosal artery should predict the appearance of corpus callosum. In our experience, this can be ambiguous and tricky.
Conclusions
Our study has shown that there are some structures and measurements that can suggest the abnormal development of the corpus callosum in the first trimester. We will continue our research in order to determine if these findings can be confidently accepted in this diagnosis.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
Paladini D, Pastore G, Cavallaro A, Massaro M, Nappi C. Agenesis of the fetal corpus callosum: sonographic signs change with advancing gestational age. Ultrasound Obstet Gynecol. 2013 Dec;42(6):687-690.
-
Pilu G, Sandri F, Perolo A, Pittalis MC, Grisolia G, Cocchi G, Foschini MP, Salvioli GP, Bovicelli L. Sonography of fetal agenesis of the corpus callosum: a survey of 35 cases. Ultrasound Obstet Gynecol. 1993 Sep;3(5):318-329.
-
Glass HC, Shaw GM, Ma C, Sherr EH. Agenesis of the corpus callosum in California 1983-2003: a population-based study. Am J Med Genet. 2008;146A(19):2495-2500.
-
Timor-Tritsch IE, Monteagudo A. Transvaginal fetal neurosonography: standardization of the planes and sections by anatomic landmarks. Ultrasound Obstet Gynecol. 1996 Jul;8(1):42-47.
-
Lachmann R, Sodre D, Barmpas M, Akolekar R, Nicolaides K. Midbrain and falx in fetuses with absent corpus callosum at 11-13 weeks. Fetal Dianosis and Therapy. 2012; 33(1):41-46.
-
Contuso R, Contro E, Belussi F, Youssef A, Pacella G, Marterlli F, Rizzo N, Pilu G, Ghi T. Demonstration of the Pericallosal Artery at 11-13 weeks of gestation using 3D Ultrasound. Fetal Diagnosis and Therapy. 2014;37(4):305-309.
-
Comănescu E, Cernea N, Tănase F, Comănescu C, Nedianu A, Alexandru D. Imaging the fetal corpus callosum in the routine examination – 2D versus 3D ultrasound. Ginecologia.ro. 2015;3(8):22-27.
-
Diaz-Guerrero L, Giugni-Chalbaud G, Sosa-Olavarria A. Assessment of pericallosal arteries by color Doppler ultrasonography at 11-14 weeks: an early marker of fetal corpus callosum development. Fetal Diagnosis and Therapy. 2013;34(2):85-89.





