Cunoaştere şi conştientizare privind virusul papiloma uman (HPV) în rândul adulţilor tineri – un studiu transversal
Knowledge and awareness of human papillomavirus (HPV) among young adults – a cross-sectional study
Abstract
Background. Human papillomavirus (HPV) infection is one of the most common sexually transmitted diseases and is incriminated in a large proportion of cervical, oral and other genital cancers. HPV vaccination was first introduced in 2004 in women, but recently there have been debates about extending the vaccination programme to men. Objective. To measure the knowledge and awareness of human papillomavirus infection among young adults. Subjects and method. The participants are medical students, selected from a larger sample, who completed an anonymous web-based survey measuring awareness and knowledge of HPV infection. The subsample contains 169 students in the age range 18-20 years old, with 32.5% men, who had fully completed the survey. Results. Overall, 70.4% of the sample had heard about HPV before. The awareness of HPV was similar between women (74.6%) and men (61.8%) (p=0.089), but was higher with seniority in medical studies (p=0.020). Among those who had heard about HPV before, while only 4.2% had been HPV vaccinated, 71% knew that the prevention of cervical cancer was possible through HPV vaccination. The highest knowledge score was 18 (out of 23), with a median of 11. The most missed answers were related to questions regarding the types of HPV included in the tetravalent vaccine (12/119 correct answers), and other types of cancer where HPV is incriminated (18/119 correct answers). Conclusions. Our survey indicates that medical students have poor knowledge of HPV and low HPV vaccination rates. These have important implications in prevention strategy. Increasing knowledge about the implications of HPV infection may encourage primary and secondary cervical cancer prevention programs.Keywords
HPV vaccinationcervical cancerknowledgeRezumat
Istoric. Infecţia cu papilomavirusul uman (HPV) este una dintre cele mai frecvente boli cu transmitere sexuală şi este incriminată pentru proporţiile mari de cancer de col uterin, oral şi de alte organe genitale. Vaccinarea HPV a fost introdusă pentru prima dată în 2004 la femei, dar recent au existat dezbateri despre extinderea programului de vaccinare la bărbaţi. Obiectiv. Măsurarea cunoştinţelor şi conştientizării infecţiei cu papilomavirusul uman la adulţii tineri. Subiecţi şi metodă. Participanţii sunt studenţi la medicină, selectaţi dintr-un eşantion mai mare, care au completat un sondaj anonim pe un website, care măsoară conştientizarea şi cunoştinţele despre infecţia cu HPV. Eşantionul conţine 169 de studenţi în intervalul de vârstă 18-20 de ani, cu 32,5% bărbaţi, care au finalizat complet sondajul. Rezultate. În general, 70,4% din eşantionul de studenţi au auzit de HPV înainte. Conştientizarea HPV a fost similară între femei (74,6%) şi bărbaţi (61,8%) (p=0,089), dar a fost mai mare cu vechimea în studiile medicale (p=0,020). Dintre cei care au auzit despre HPV înainte, în timp ce doar 4,2% au fost vaccinaţi cu HPV, 71% au ştiut că prevenirea cancerului de col uterin este posibilă prin vaccinarea HPV. Cel mai mare scor de cunoştinţe a fost 18 (din 23), cu o medie de 11. Cele mai multe răspunsuri greşite la întrebări au fost legate de tipurile de HPV incluse în vaccinul tetravalent (răspunsuri corecte 12/119) şi de alte tipuri de cancer în care HPV este incriminat (18/119 răspunsuri corecte). Concluzii. Sondajul nostru indică faptul că studenţii la medicină au cunoştinţe slabe despre HPV şi rate scăzute de vaccinare împotriva HPV. Acestea au implicaţii importante în strategia de prevenire. Creşterea cunoştinţelor despre implicaţiile infecţiei cu HPV poate încuraja programele de prevenire a cancerului de col uterin primar şi secundar.Cuvinte Cheie
vaccinare împotriva HPVcancer cervicalcunoştinţeIntroduction
Until recently, the high risk or oncogenic human papillomavirus (HPV) infection seemed to correlate exclusively with cervical carcinoma, the results of clinical investigations showing that it is primarily responsible for cancerous and precancerous lesions in the genital area, both in men and women. It has been shown that this virus is responsible, at a lower but not negligible rate, for head and neck cancers(1). HPV was incriminated to contribute up to 100% of cases of cervical cancer, to 88% of cases of anal cancer, to 43% of cases of vulvar cancer, to 70% of invasive vaginal carcinomas, and to 50% of all cancers of the penis worldwide(2). Instead, the exact proportion of head and neck cancer is unknown, but recent data have shown that the incidence of oropharyngeal squamous cell carcinoma is increasing in the UK at a rate of 15% per year. In the United States and Canada, approximately 70% of the oropharyngeal squamous cell carcinoma is considered to be HPV-related, and oropharyngeal cancer accounts for approximately one-third of over 9,000 cases of head and neck cancer reported annually in England and Wales(3).
Both bivalent and tetravalent vaccines are considered highly effective against cervical cancer and precancerous lesions caused by HPV 16 and 18. Both vaccines offer protection for HPV genotypes not included in the vaccine. This cross-protection for non-included strains is a very important remark, because strains not introduced in vaccination are responsible for approximately 30% of cervical cancer cases(4).
Nonavalent vaccination, including 9 strains, was approved by the US Food and Drug Administration (FDA) in 2014, and by the European Medicines Agency (EMA) in 2015.
Through this paper, we aim to highlight for the first time the level of knowledge and attitude of the young adult in Romania for human papillomavirus infection, because the acceptance of vaccination and other preventive measures are mainly related to the level of knowledge and understanding of the risk of HPV infection. The results will be used in prevention and information strategies for this at-risk population.
Subjects and method
The study was cross-sectional and the population was represented by students attending the “Victor Babeş” University of Medicine and Pharmacy of Timişoara, Romania. The sample included the answers of 169 students in the age range 18-20 years old, with 32.5% men, who had fully completed the survey and submitted complete questionnaires.
The questionnaire was created on a digital platform provided by Google forms. Questions have been created and responses have been validated in order to ensure a primary quality standard. Questions of interest were marked as mandatory, and some questions were labeled as conditional. Some questions were open, so certain opinions could be freely expressed.
The questionnaire evaluated the knowledge and perception of respondents about human papillomavirus infection, anti-HPV vaccination and general epidemiology knowledge. The respondents were asked to choose between “yes”, “not sure”, and “no”. The independent variables were age, year of study, and sex.
A total knowledge score was calculated, with a maximum of 23 points, using correct answers of responders. Each correct answer contributed equally to the final score.
At the end of the study, the online database was exported, and SPSS was used for statistical processing. Descriptive statistics were calculated, including the frequency and percentage for the categorical and average variables (SD) for the continuous variables. The p value less than 0.05 was considered statistically significant. For comparison of proportions, the Chi-square test, along with Mann-Whitney and Kruskal Wallis test were used.
Results
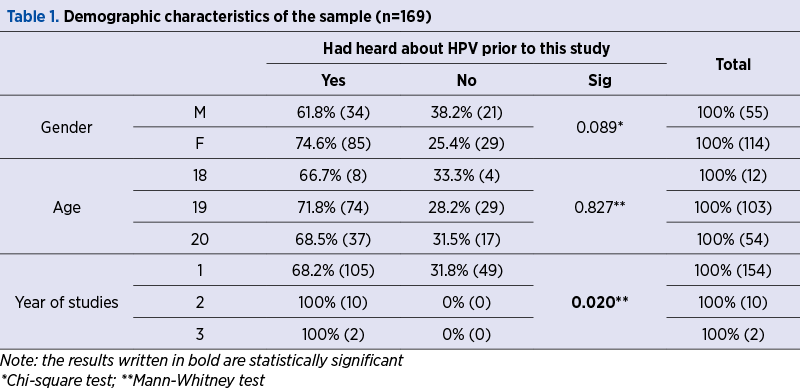
Prior to the participation in this study, 70.4% of the students had heard about HPV, and 29.6% had never heard before about HPV.
From the gender perspective, HPV awareness was similar (p=0.089) between women (74.6%) and men (61.8%), but higher with the year of study in medical science (p=0.020). Only students enrolled on the first year have never heard of HPV.
Using students who had heard previously about HPV (n=119), we have computed an average value of 11.87 and a standard deviation of 3.57 points. The highest score obtained by our responders was 18. Furthermore, the total score was transformed in tertiles. Table 2 contains intertertiles comparisons of demographic variables and the percentage of students who have responded correctly to questions.
The proportions of males/females, age and year of studies were not affected by tertiles. The vaccination rate was extremely low (5/114), and also without a relationship with tertiles of knowledge.
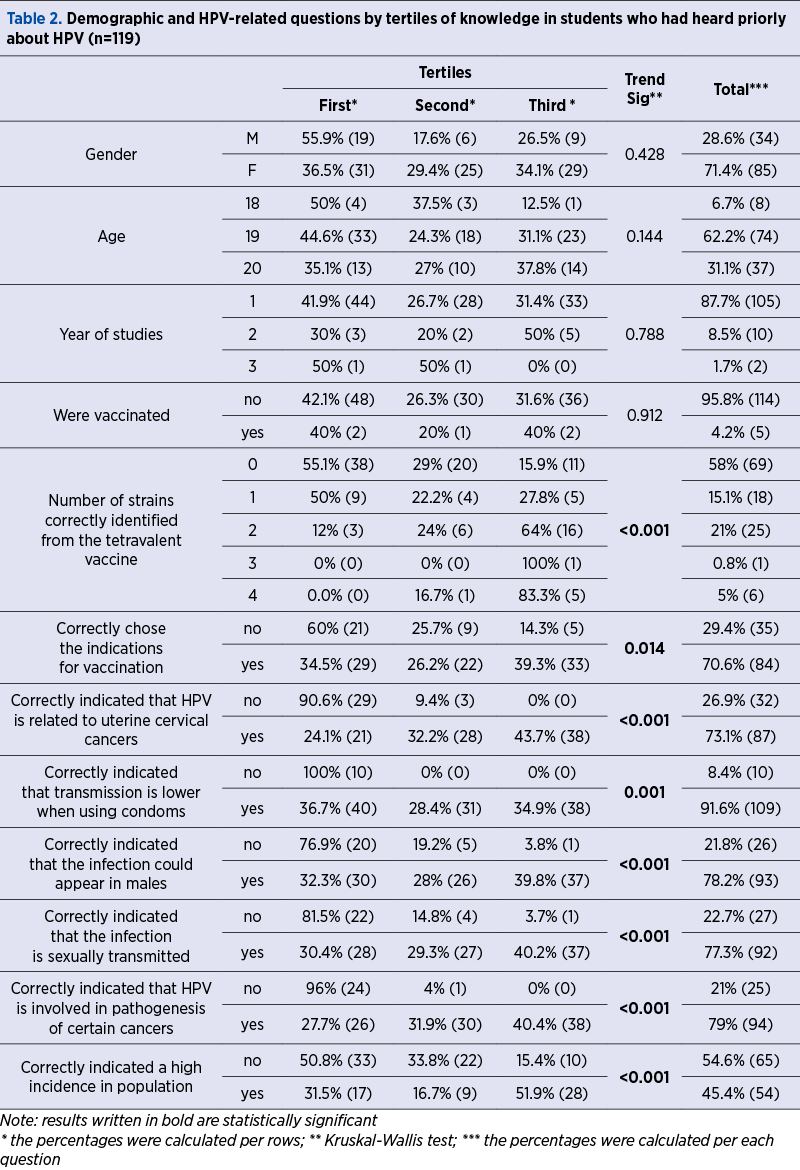
In all clinical questions about HPV, the trend is positive in tertiles, and statistically significant, higher rates of correct answers being observed in higher tertiles of knowledge.
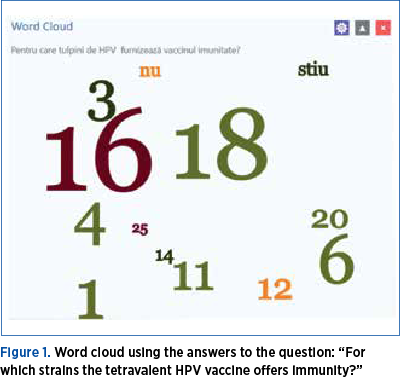
The most wrong answers were related to the types of HPV included in the tetravalent vaccine (12/119 correct answers), and other types of cancer where HPV is incriminated (18/119 correct answers) – Figure 1. Highest rates of correct answers were obtained for questions related to prevention by condoms (109/119 correct answers) and for the question if HPV infection could appear in males (93/119 correct answers).
Discussion
Human papillomavirus infection is the most common sexually transmitted disease worldwide. Although most neoplastic cervical intraepithelial lesions (CIN) regress spontaneously, most CIN 2 or 3 cervical dysplasia are extremely rare(5). Persistent HPV infection – the major risk factor for cervical cancer – is related to other factors, such as advanced age, HPV genotype, coexisting infections, immunosuppression and inflammation(5).
The present study was conducted to evaluate the students’ knowledge of HPV in medical specializations in Timişoara, Romania. Overall, the study showed that, except for a few questions, students had a low level of knowledge about HPV. However, despite attending medical specializations, only 70.4% had ever heard before about HPV, of which only 4.2% were vaccinated and only 5.4% correctly identified the strains present in the tetravalent vaccine, which was available on the market earlier this year.
Similar studies performed in different parts of the world had different prevalence levels of HPV consciousness. Thus, a study conducted at Keele University in England reported, similarly to our study, that nearly 75% of female participants had heard of HPV, but despite HPV awareness, only 27% knew that HPV is causing cervical cancer(6). Studies in developing countries have revealed lower percentages of HPV consciousness: in Pakistan, it was reported that nearly 57% of those investigated had heard of HPV prior to this study, and nearly 55% knew that HPV caused cervical cancer(7). Another study, conducted in Nigeria, showed that only 17.7% of female students were aware of HPV(8).
A study in Malaysia showed that about 80% of medical students knew that HPV was causing cervical disease, and nearly 54.6% reported that HPV could infect men and women equally. However, only 37% of them considered HPV as a common disease(9).
These results show that the lack of knowledge about HPV exists everywhere, and the inadequacy of HPV knowledge is a global issue.
Another important aspect of the present study is represented by the low HPV vaccination rates. The prevention of HPV infections is essential in the prophylaxis of cervical, oral and anal cancers. The emergence and application of the HPV vaccine have been a major event in the prevention of many cancers, so there should be a greater awareness of HPV prevention and HPV vaccination, as most of the study participants (95.8%) have not been vaccinated or do not know if they were vaccinated, and nearly 22.7% reported that HPV infection is not related to pathogenesis of cancers. A cause of the low prevalence of vaccination in this generation would be the false perceptions of vaccination, which could be caused by lack of knowledge, fear of having an adverse effect, and inadequate and insufficient preventive actions, such as advertising, brochures and information campaigns. Another reason could be the lack of medical professionals support and the lack of recommendation by general practitioners, which ultimately affect the perception and acceptability of vaccination by the general population and by the students, respectively.
In general, the recommendation of the health care provider and the parents were the two main factors that determined the availability of respondents to be vaccinated for HPV. These findings report a strong influence of friends, parents and health care professionals on the acceptability of HPV vaccination, which reaffirms the conclusions of previous studies(10).
The availability of effective HPV vaccines has led to a decrease in certain sequelae of HPV infections among women in the United States(11). In a meta-analysis of 20 eligible studies, investigators showed that in countries with female vaccine coverage of at least 50%, types 16 and 18 HPV infections decreased by 68% between the pre-vaccination and the post-vaccination periods, and anogenital warts decreased by 61% in girls aged 13-19 years old(12). In the United States, the prevalence trends for anogenital warts vary with age and gender. Among women aged 15 to 19 years old, the prevalence of HPV was stable between 2003 and 2007, but declined significantly over the period 2007-2010. Among women aged 20-24 years old, the anogenital prevalence of warts increased significantly between 2003 and 2007, was stable between 2007 and 2010, then declined in 2009-2010. The prevalence in females aged 25-39 years old (people who were not likely to be vaccinated) increased significantly over this period. For men aged 15 to 39 years old, the anogenital nursery prevalence for each 5-year age group increased in 2003-2009, but no increases were observed for 2010(13).
The rate of precancerous lesions decreased after the introduction of HPV vaccination; an analysis of the New Mexico HPV Papillomavirus Registry from 2007-2014 showed significant decreases in all stages of intraepithelial cervical neoplasia (CIN) for women aged 15-19 years old(14). Data from the HPV-IMPACT CDC project, a sentinel surveillance project, also demonstrated dramatic reductions in the incidence of cervical precancerous lesions between 2008 and 2012, for women aged 18-29 years old(15). It is important to note that screening recommendations have changed over this period, so that the decline in the disease may reflect both reduced screening and the impact of vaccination. At the same time, there was a significant decrease in the prevalence of precancerous lesions associated with HPV 16 and 18 in adult women who received at least one dose of HPV vaccine(15).
The absence of sexual activity remains the most reliable method for preventing genital HPV infection. Patients may decrease their chances of infection by consistently and correctly using condoms and by limiting the number of sexual partners. Although these interventions may not fully protect against HPV, they may reduce the chances of acquiring and transmitting HPV.
Conclusions
The results of this study revealed a low level of respondents’ awareness of HPV-related health problems, prevention and transmission. Nearly one-third of those investigated had not heard about human papillomavirus prior to this study, and among those who heard about it, the vaccination rate was very low, even though HPV vaccination was introduced in Romania in 2006.
Although the latest generation of nonavalent vaccine was launched in Romania in 2018, the proportion of medical students who correctly identified HPV strains in the tetravalent vaccine was extremely low, at 5.88%.
Patients’ counseling and education should cover the nature of HPV infection, the contagion issues and the risk reduction.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
1. Giuliano AR, Nyitray AG, Kreimer AR, et al. EUROGIN 2014 roadmap: Differences in human papillomavirus infection natural history, transmission and human papillomavirus-related cancer incidence by gender and anatomic site of infection. Int J Cancer. 2015; 136(12):2752-2760. doi:10.1002/ijc.29082.
2. Martel C De, Ferlay J, Franceschi S, et al. Global burden of cancers attributable to infectins in 2008: a review and synthetic analysis. Lancet. 2012; 379(9829):1851. doi:10.1016/S1470-2045(12)70137-7.
3. Jones TM. Tumour-infiltrating lymphocytes in the risk stratification of squamous cell carcinoma of the head and neck. Br J Cancer. 2014; 110(2):269-270. doi:10.1038/bjc.2013.746.
4. WHO. Human papillomavirus vaccines: WHO position paper, October 2014. World Heal Organ Wkly Epidemiol Rec. 2014; 89(43):465-492. doi:10.1186/1750-9378-2-15.Voir.
5. Wheeler CM. Natural History of Human Papillomavirus Infections, Cytologic and Histologic Abnormalities, and Cancer. Obstet Gynecol Clin North Am. 2008; 35(4):519-536. doi:10.1016/j.ogc.2008.09.006.
6. Sherman SM, Nailer E, Minshall C, Coombes R, Cooper J, Redman CWE. Awareness and knowledge of HPV and cervical cancer in female students: A survey (with a cautionary note). J Obstet Gynaecol (Lahore). 2016; 36(1):76-80. doi:10.3109/01443615.2015.1041886.
7. Khan TM, Buksh MA, Rehman IU, Saleem A. Knowledge, attitudes, and perception towards human papillomavirus among university students in Pakistan. Papillomavirus Res. 2016; 2:122-127. doi:10.1016/j.pvr.2016.06.001.
8. Makwe CC, Anorlu RI, Odeyemi KA. Human papillomavirus (HPV) infection and vaccines: Knowledge, attitude and perception among female students at the University of Lagos, Lagos, Nigeria. J Epidemiol Glob Health. 2012; 2(4):199-206. doi:10.1016/j.jegh.2012.11.001.
9. Rajiah K, Maharajan MK, Chin NS, Num KSF. Awareness and acceptance of human papillomavirus vaccination among health sciences students in Malaysia. Virus Disease. 2015; 26(4):297-303. doi:10.1007/s13337-015-0287-3.
10. Gamble HL, Klosky JL, Parra GR, Randolph ME. Factors influencing familial decision-making regarding human papillomavirus vaccination. J Pediatr Psychol. 2010; 35(7):704-715. doi:10.1093/jpepsy/jsp108.
11. Perkins RB, Legler A, Hanchate A. Trends in male and female genital warts among adolescents in a safety-net health care system 2004-2013: Correlation with introduction of female and male human papillomavirus vaccination. Sex Transm Dis. 2015; 42(12):665-668. doi:10.1097/OLQ.0000000000000369.
12. Drolet M, Bénard É, Boily M-C, et al. Population-level impact and herd effects following human papillomavirus vaccination programmes: a systematic review and meta-analysis. Lancet Infect Dis. 2015; 15(5):565-580. doi:10.1016/S1473-3099(14)71073-4.
13. Flagg EW, Schwartz R, Weinstock H. Prevalence of anogenital warts among participants in private health plans in the United States, 2003-2010: Potential impact of human papillomavirus vaccination. Am J Public Health. 2013; 103(8):1428-1435. doi:10.2105/AJPH.2012.301182.
14. Benard VB, Castle PE, Jenison SA, et al. Population-Based Incidence Rates of Cervical Intraepithelial Neoplasia in the Human Papillomavirus Vaccine Era. JAMA Oncol. 2016; 87131:1-5. doi:10.1001/jamaoncol.2016.3609.
15. Hariri S, Johnson ML, Bennett NM, et al. Population-based trends in high-grade cervical lesions in the early human papillomavirus vaccine era in the United States. Cancer. 2015; 121(16):2775-2781. doi:10.1002/cncr.29266.



