A case of extrapulmonary sarcoidosis mimicking metastatic disease
Un caz de sarcoidoză extrapulmonară ce mimează boala metastatică
Abstract
Sarcoidosis is a multisystemic inflammatory disease of unknown cause, characterized by the presence of noncaseous granulomas and T4 helper CD4 lymphocytic inflammation. It mainly affects the lungs and the intrathoracic lymph nodes, the skin and the eyes, but any organ can be involved. In extrapulmonary forms, sarcoidosis most commonly has the appearance of metastatic or lymphomatous disease. In these rare cases, intralesional or lymphadenopathy biopsy puncture and histopathological examination allow the positive diagnostic. We present the case of a 14-year-old patient hospitalized in the Fundeni Clinical Institute, Bucharest, for epistaxis and arterial hypertension (HTA), with a high level of renin. The CT examination performed to elucidate the cause of arterial hypertension revealed hepatosplenomegaly, a hepatic nodule in association with multiple conglomerate abdominal lymphadenopathies and the presence of multiple bilateral renal nodules. Pulmonary radiography was within normal limits. Given the bilateral renal nodular lesions and the multiple lymphadenopathies, a biopsy puncture was performed in one of the renal nodules and in the adenopathic mass, the histopathological result being suggestive for extrapulmonary sarcoidosis lesions. Conclusions. In the presence of multiple plurivisceral nodular lesions in association with adenopathic masses, extrapulmonary sarcoidosis must be included in the list of differential diagnoses, the final confirmation being made by histopathological examination after intralesional biopsy.Keywords
extrapulmonary sarcoidosisCTMRImetastatic diseaseRezumat
Sarcoidoza este o boală inflamatorie multisistemică de cauză necunoscută, caracterizată prin prezenţa de granuloame necazeificate şi inflamaţie limfocitară T helper CD4. Afectează predominant plămânii şi ganglionii limfatici intratoracici, pielea şi ochii, dar orice organ poate fi implicat. În formele extrapulmonare, sarcoidoza îmbracă cel mai frecvent aspectul unor determinări metastatice sau limfomatoase. În aceste cazuri rare, puncţia-biopsie intralezională sau din adenopatii şi examenul histopatologic permit diagnosticul de certitudine. Prezentăm cazul unei paciente de 14 ani, internată în Institutul Clinic Fundeni, Bucureşti, pentru epistaxis şi hipertensiune arterială (HTA), cu un nivel crescut al reninei plasmatice. Examinarea CT efectuată pentru elucidarea cauzei HTA evidenţiază hepatosplenomegalie, un nodul hepatic în asociere cu multiple adenopatii abdominale conglomerate şi prezenţa de noduli renali multipli bilaterali. Radiografia pulmonară este în limite normale. Având în vedere leziunile nodulare renale bilaterale şi adenopatiile multiple, se realizează puncţie-biopsie într-unul din nodulii renali şi în masa adenopatică, rezultatul histopatologic fiind sugestiv pentru leziuni sarcoidotice extrapulmonare. Concluzii. În faţa unor leziuni nodulare pluriviscerale multiple în asociere cu mase adenopatice, în lista de diagnostice diferenţiale trebuie să fie inclusă şi sarcoidoza extrapulmonară, confirmarea finală realizându-se prin examen histopatologic postbiopsie intralezională.Cuvinte Cheie
sarcoidoză extrapulmonarăCTIRMboală metastaticăClinical history
A 14-year-old male patient presented with epistaxis and high blood pressure. His past medical history revealed Rolandic epilepsy since 2015. On admission, further investigations revealed normal cardiovascular examination, normal levels of creatinine and elevated plasmatic renin. A CT scan was performed to establish the cause of hypertension.
Imaging findings
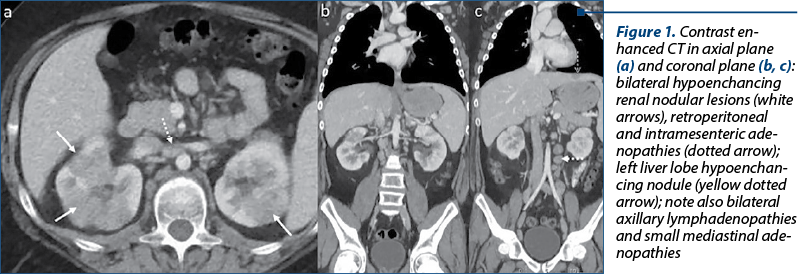
Unenhanced and enhanced abdominal multislice CT evaluation with coronal reconstructions (Figure 1) revealed hepatomegaly, a left liver lobe hypoenchancing nodule, splenomegaly, multiple abdominal lymphadenopathies and ill-defined multiple hypoenchancing lesions in both kidneys. The chest X-ray was normal (Figure 2).

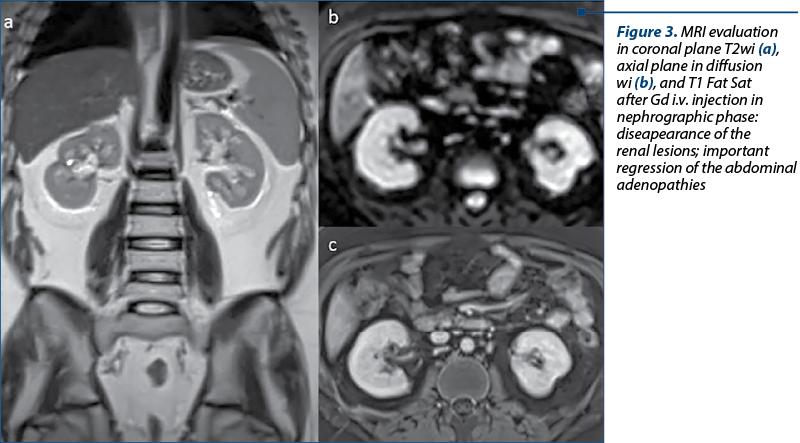
After two months, an abdominal MRI was performed in T1-weighted image with FatSat, SSFSE with short TE and long TE, diffusion and with extracellular paramagnetic gadolinium-based contrast i.v. injection using a 3D T1 FS acquisition in axial (Figure 3) and coronal plane. All renal lesions have disappeared, and also the retroperitoneal adenopathies were without any MRI pathological appearance.
Outcome
Taking into account the CT aspects, renal and lymph node biopsies were performed. The pathological analysis from the biopsied kidney lesion discovered granulomatous tubulointerstitial nephritis, while the biopsied lymph node pathological examination showed multiple non-caseating cell granulomas, suggesting the diagnosis of sarcoidosis. After the coticotherapy began, the clinical symptoms and the imaging findings improved.
Discussion
Sarcoidosis is a multisystemic inflammatory disease characterized by the existence of non-caseating granulomas which consist in masses with macrophages, mononuclear and epithelioid cells, along with T cells. The etiology of this disorder is unknown, but an abnormal immune response could be the cause(1,2). This disease is ubiquitous, with a higher prevalence in young and middle-aged patients, respectively with a slight female predominance(3). The lungs manifestations are the most frequent in sarcoidosis, along with skin, liver, spleen, lymph nodes, nervous system, heart and renal involvement(4).
The prevalence of sarcoidosis is less common in children and they often present with acute symptomatology and multisystemic involvement, such as hepatosplenomegaly, lymphadenopathy, lung disease and uveitis(5). Pediatric sarcoidosis has two forms, one that has an early onset, before 5 years old, and one with late onset which is characterized by multi-system disease(6).
Renal manifestations are rare in sarcoidosis, with no certain data about the prevalence in general population. The most common finding in biopsies in this cases is the granulomatous tubulointerstitial nephritis(7). Non-caseating cell granulomas can be found isolated or associated with extrarenal disorder(6).
Patients suspected of having sarcoidosis should have a chest radiography, which is the first imaging step used for pulmonary sarcoidosis, but for extrapulmonary disease there are often required ultrasound, CT and magnetic resonance (MR) imaging(8). Thin-section CT of the thoracic cavity highlights multiple well-defined perilymphatic micronodules in the pulmonary parenchyma and mediastinal adenopathy(8).
The most common ultrasound findings in abdominal sarcoidosis are hepatosplenomegaly, hypoechoic masses and enlarged lymph-nodes(9).
Regarding the renal lesions, they appear hypodense and hypovascular on CT scans, with multiple patterns of enhancement, from spotted or striated to mass-like lesions, less frequently. The kidneys can be atrophied or with an increased dimension(10). On MRI, ill-defined masses can be found, with homogenous or heterogenous structure, frequently isointense to the surrounding renal parenchyma on unenhanced T1 and T2-weighted sequences. After gadolinium-based intravenous contrast administration, the lesions demonstrate delayed and poor enhancement to the normal renal cortex(11).
The differential diagnosis list is made with: metastasis, lymphomas, infectious disease (e.g., tuberculosis), other granulomatous diseases.
Conclusions
The diagnosis of extrapulmonary sarcoidosis, in cases with normal chest X-ray or normal CT lungs, is possible correlating the clinical and imagistic findings with the histopathologic results of non-caseating granulomas on biopsy, the pathology remaining the gold standard examination, after the exclusion of other causes of granuloma formation, such as infectious diseases or neoplasms and, of course, taking into account the favorable evolution under the corticosteroid treatment.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
Ungprasert P, Ryu JH, Matteson EL. Clinical Manifestations, Diagnosis, and Treatment of Sarcoidosis. Mayo Clin Proc Innov Qual Outcomes. 2019;3(3):358–75.
-
Jain R, Yadav D, Puranik N, Guleria R, Jin JO. Sarcoidosis: Causes, diagnosis, clinical features, and treatments. J Clin Med. 2020;9(4).
-
Nunes H, Bouvry D, Soler P, Valeyre D. Sarcoidosis. Orphanet J Rare Dis. 2007;2(1):1–8.
-
Wessendorf TE, Bonella F, Costabel U. Diagnosis of Sarcoidosis. Clin Rev Allergy Immunol. 2015;49(1):54–62.
-
Klaus R, Jansson AF, Griese M, Seeman T, Amann K, Lange-Sperandio B. Case Report: Pediatric Renal Sarcoidosis and Prognostic Factors in Reviewed Cases. Front Pediatr. 2021;9(September):1–7.
-
Chotalia P, Pandya S, Srivastava P. Granulomatous nephritis: A rare presentation of juvenile-onset sarcoidosis. Mod Rheumatol Case Reports. 2021;(June):1–4.
-
Agrawal V, Crisi GM, D’Agati VD, Freda BJ. Renal sarcoidosis presenting as acute kidney injury with granulomatous interstitial nephritis and vasculitis. Am J Kidney Dis. 2012;59(2):303–8.
-
Ganeshan D, Menias CO, Lubner MG, Pickhardt PJ, Sandrasegaran K, Bhalla S. Sarcoidosis from head to toe: What the radiologist needs to know. Radiographics. 2018;38(4):1180–200.
-
Tana C, Schiavone C, Ticinesi A, Ricci F, Giamberardino MA, Cipollone F, et al. Ultrasound imaging of abdominal sarcoidosis: State of the art. World J Clin Cases. 2019;7(7):809–18.
-
Warshauer DM, Lee JKT. Imaging Manifestations of Abdominal Sarcoidosis. Am J Roentgenol. 2004;182(1):15–28.
-
Gezer NS, Başara I, Altay C, Harman M, Rocher L, Karabulut N, et al. Abdominal sarcoidosis: Cross-sectional imaging findings. Diagnostic Interv Radiol. 2015;21(2):111–7.



