Prostate cancer is an important health public issue. Magnetic Resonance Imaging (MRI) is the best imaging modality for evaluating the prostate and accurately diagnose the prostatic carcinoma, especially in cases with aggressive and larger volume tumors. The main objectives of this article are: to review the multiparametric MRI assessment technique used in prostate pathology, to list and illustrate the most common MRI features in prostate cancer, and to present the role of the multidisciplinary team in the diagnosis and management of patients with prostate tumoral pathology.
Imagistica multiparametrică de rezonanţă magnetică în diagnosticul cancerului de prostată: o necesitate
Multiparametric Magnetic Resonance Imaging in prostate cancer diagnosis: a must
First published: 29 decembrie 2018
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/OnHe.45.4.2018.2168
Abstract
Rezumat
Cancerul de prostată reprezintă o importantă problemă de sănătate publică. Imagistica prin rezonanţă magnetică (IRM) este cea mai bună modalitate de evaluare a prostatei şi de a diagnostica cancerul de prostată, mai ales în cazurile în care tumora este voluminoasă şi agresivă. Principalele obiective ale acestui articol sunt: revizuirea tehnicii utilizate în evaluarea IRM multiparametrică în patologia prostatei, prezentarea şi ilustrarea principalelor aspecte IRM întâlnite în cancerul de prostată şi prezentarea rolului abordului multidisciplinar în diagnosticul şi managementul pacienţilor cu patologie tumorală prostatică.
Objectives
To describe the optimal Magnetic Resonance Imaging (MRI) protocol used to detect prostate carcinoma. To become familiar with the MRI features of prostate cancer. To delineate the importance of the multidisciplinary team in the diagnosis and management of patients with prostate cancer.
Introduction
Epidemiology. Prostate cancer is the most common solid neoplasm in Europe and the second leading cause of male cancer deaths in USA and UK. Approximately 30% of men in their 50’s have microscopic foci of prostate cancer, but most of them never progress. Age is the most important risk factor(1-3).
Histopathology. Allmost all prostate cancers are adenocarcinomas. Gleason score grade 2-4 corresponds to a well differentiated prostatic tumor; grade 5-7 is a moderately differentiated tumor, and 8-10 signifies a poorly differentiated prostatic cancer(3).
Prognostic indicators. TNM stage is the most important prognostic variable. The 5-year disease specific survival for patients with metastasis (M1) is approximately 30%. The Gleason score is an independent prognostic indicator; the 10-year disease survival for clinically localized disease is 87% for well and moderately differentiated tumors, dropping to 34% for poorly differentiated tumors(1-3). Prostate specific antigen (PSA) is primarily used in the diagnosis and detection of disease recurrence. High levels is correlated with advanced TNM stage at diagnosis(3).
Indications of MRI evaluation in prostate cancer:
1. Detection (localization) – detection and characterization protocol.
2. Staging protocol: tumor extension, presence of node and bone metastasis.
3. Follow-up of a known prostatic tumor.
4. Recurrences (after treatment).
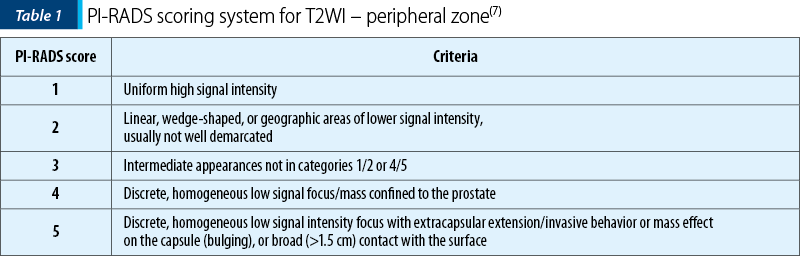
PI-RADS (Prostate Imaging Reporting and Data System) was published in February 2012 by The European Society of Urogenital Radiology (ESUR) with the purpose to standardize reporting in the MRI of the prostate(4). A scale from 1 to 5, stratifying a focal prostatic abnormality according to the MRI findings, obtained with different MRI sequences, improves the reproducibility of radiologists reports and the communication with referring physicians(5-9).
Multiparametric (MP) MRI evaluation of the prostatic tumors. MP MRI in prostatic carcinoma (PC) diagnosis is based on morphological acquisitions focused on T2WI and functional acquisitions which include diffusion weighted image (DWI) and perfusion 3DT1 with paramagnetic contrast(4-9).
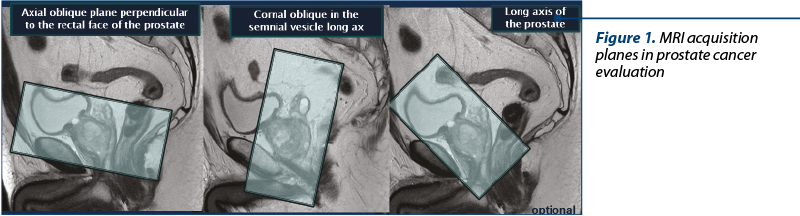
Other sequences and technical requirements. The prostate and seminal vesicles must be covered entirely (slice thickness: 3 mm). Imaging, parallel to the prostate, perpendicular to the rectal face of the prostate, or oblique into the seminal vesicles plane are essential to evaluate extraprostatic extension (Figure 1).
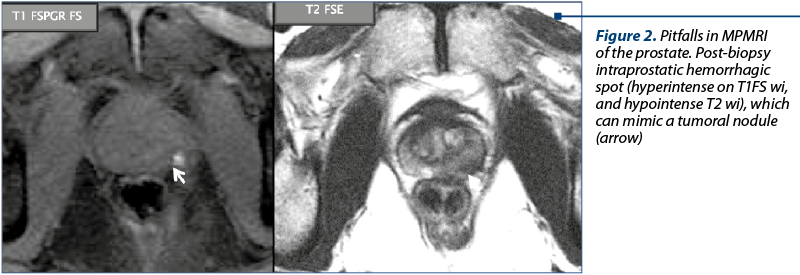
T1-wi SE are useful for detecting enlarged pelvic lymph nodes (slices from the pubic symphysis till the aortic bifurcation), bone metastases and post biopsy hemorrhage. T1 FSPGR Fat Sat (FS) is used to visualize post-biopsy prostate hemorrhage focus (Figure 2). The interpretation is based on an attentive qualitative and quantitative analysis of each sequence(4-9).
It is very important that the slices obtained on T2 wi, diffusion, dynamic T1 after gadolinium (Gd) injection have the same plane (centering), slices number, slice thickness and identical interslice space for a correct and easy analysis. Using b values ≥1500, it is possible to differentiate PC from prostatitis and stromal benign prostatic hypertrophy (BPH); PC remains bright and the apparent diffusion coefficient (ADC) value decrease. Different publications and studies regarding the correlation between ADC value on diffusion-weighted MR imaging and the Gleason score in prostate cancer have demonstrated that ADC values are lower in aggressive PC and correlated with the Gleason score(9-11).
MP MRI features
T2 hyposignal in the peripheral zone (PZ) and transition zone (TZ). Prostate cancer located in the PZ corresponds to an area of low signal intensity (Figure 3 and Table 1). But T2 hyposignal in the peripheral zone may be present also in noncancerous conditions(12): inflammation, biopsy-related hemorrhage (blood products may persist 4-6 weeks or longer after prostate biopsy), post-radiation therapy fibrosis, and changes after hormone deprivation therapy (Figure 2).
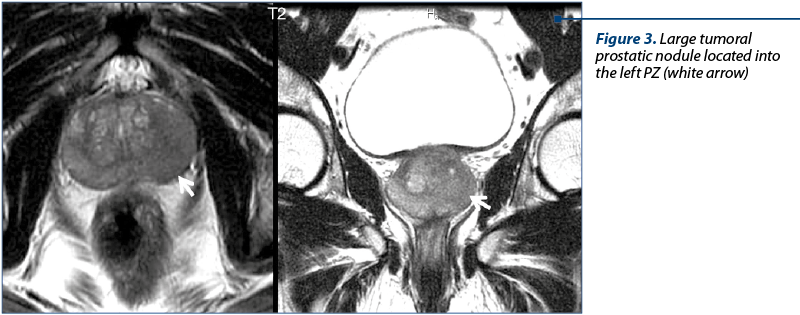
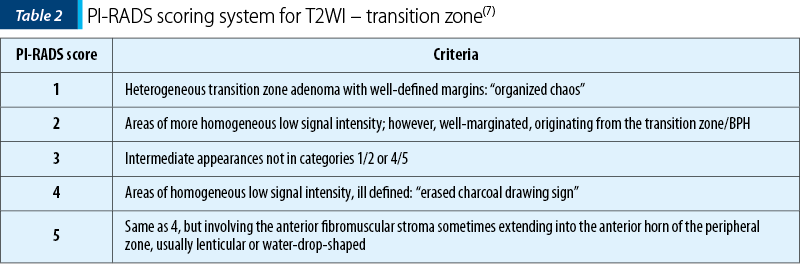
T2-wi has significant limitations for depicting cancer involving the TZ and CZ (Table 2): cancer and normal tissues have both low signal intensity(4-9).
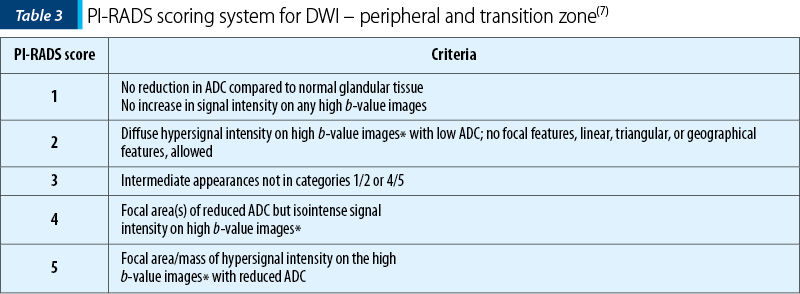
Diffusion weighted images (DWI; Table 3). The diffusion properties of tissue are related to the amount of interstitial free water and permeability(10,11). The b factor values: 0; 100; 800; 1000; 1500; 2000 s/mm² (trace image).
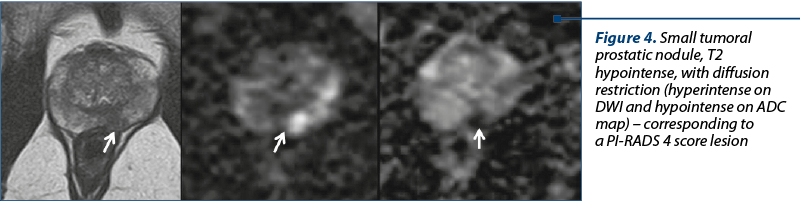
Cancer tends to have more restricted diffusion than does normal tissue because of the high cell densities and the abundance of intra-/and intercellular membranes (Figure 4).
Dynamic contrast-enhanced (DCE) – perfusion MRI (Table 4)

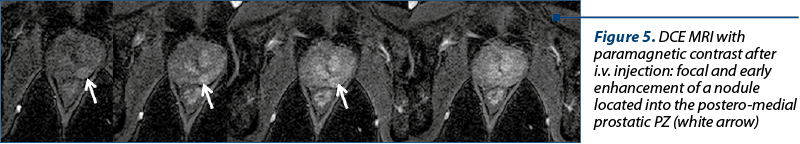
In many studies, it has been shown that the values of contrast enhancement parameters – mean transit time, blood flow, permeability surface area and interstitial volume – are significantly greater in cancerous tissue than in normal tissue (Figure 5). DCE is useful in cases when T2 and DWI are unclear(13-15).
Anterior-posterior cancer appears as an homogeneous area in T2 hyposignal lenticular form, blurred contours, no cyst, without capsule, with restricted diffusion(4,14,15).
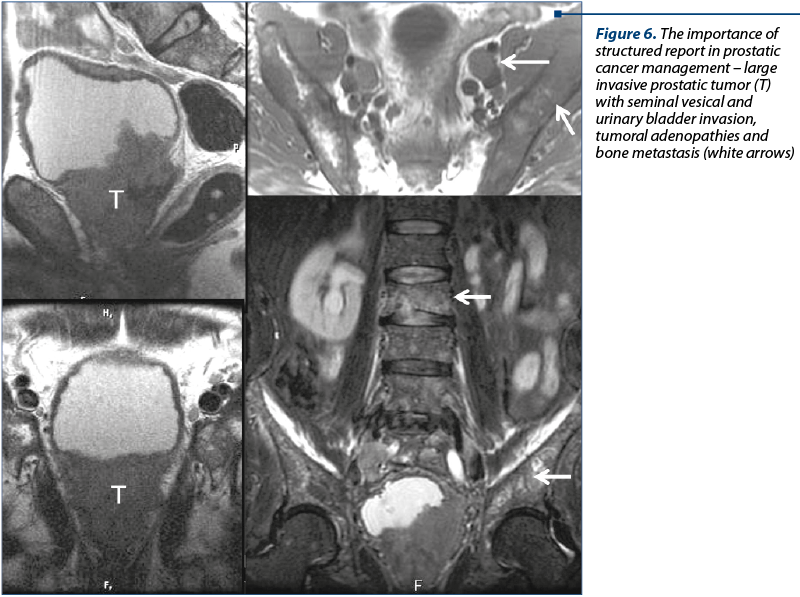
Staging. MP MRI is very useful for evaluating the tumoral (T) stage, confined to the prostatic gland (≤T2 disease) or extending beyond the gland (≥T3 disease). The apex of the prostate should be carefully analyzed, as well as the external urethral sphincter. Extraprostatic extension (EPE) is based on the existence of a bulging prostatic contour, an irregular or spiculated margin, obliteration of the recto-prostatic angle, a tumor‐capsule interface greater than 1 cm, breach of the capsule with evidence of direct tumor extension or bladder wall, involvement of the neurovascular bundle (asymmetry, enlargement), and seminal vesicle (SV) invasion. The tumoral invasion of SV include the demonstration of direct tumor extension from the base of the prostate into the VS, focal or diffuse hypointense T2W image and/or abnormal contrast enhancement within or along the SV, restricted diffusion, obliteration of the angle between the base of the prostate and the SV. The analysis of pelvic and retroperitoneal lymph nodes is obligatory. Abnormal lymph nodes on MRI take into account the size, morphology, shape, and the enhancement pattern. Lymph nodes over 8 mm in short axis dimension are suspicious. Nodal groups necessary to be evaluated include: common femoral, obturator, external iliac, internal iliac, common iliac, pararectal, presacral, paracaval and paraaortic to the level of the aortic bifurcation. Bone metastases assessment is also required (Figure 6).
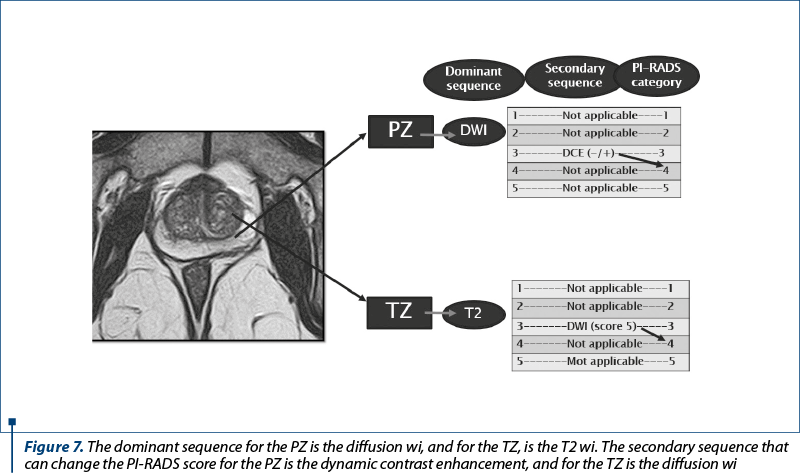
In summary, DWI is the best sequence for the PZ. T2 represents the best sequence for the TZ (Figure 7).
The MRI report must contain: antecedents/specific laboratory data, MRI technique, whether the MP MRI of the prostate is normal or not, the location of each lesion, the description of the signs in favor of malignancy, the tumoral (T) staging correlated to the extraprostatic extension, the involvement of the adjacent structures, the presence of adenopathies and metastasis.
In uncertain cases, the imaging report must contain the recommendations regarding what to do next: biopsy (fusion US-MRI), or follow-up based on a multidisciplinary team approach (urologist, radiologist, laboratory doctor, histopathologist, oncologist, radiotherapist).
Conflict of interests: The author declares no conflict of interests.
Bibliografie
- National Comprehensive Cancer Network NCCN. Clinical practice guidelines in oncology: prostate cancer. 2012; Fort Washington, PA. http://www.nccn.com/files/cancer-guidelines/ prostate.
- European Association of Urology (EAU). Guidelines on prostate cancer. 2012; Arnhem, The Netherlands (http://www.uroweb.org).
- Chodak GW, Krupski TL, et al. Prostate Cancer Workup. 2018; available at: https://emedicine.medscape.com/article/196773.
- Barentsz JO, Richenberg J, Clements R, et al. ESUR prostate MR guidelines 2012. Eur Radiol. 2012; 22(4):746–757.
- Rosenkrantz AB, Kim S, Lim RP, et al. Prostate cancer localization using multiparametric MR imaging: comparison of Prostate Imaging Reporting and Data System (PI-RADS) and Likert scales. Radiology. 2013; 269; 482–492.
- Hamoen EH, de Rooij M, Witjes JA, Barentsz JO, Rovers MM. Use of the prostate imaging reporting and data system (PIRADS) for prostate cancer detection with multiparametric magnetic resonance imaging: a diagnostic meta-analysis. Eur Urol. 2015; 67(6):1112–112.
- PI-RADS™ Prostate Imaging – Reporting and Data System 2015 version 2. Available at: https://www.acr.org/-/media/ACR/Files/RADS/Pi-RADS/PIRADS-V2.pdf
- Vargas HA, Hötker AM, Goldman DA, et al. Updated prostate imaging reporting and data system (PIRADS v2) recommendations for the detection of clinically significant prostate cancer using multiparametric MRI: critical evaluation using whole-mount pathology as standard of reference. Eur Radiol. 2016; 26 (6):1606-12.
- Litjens GJS, Barentsz JO, Karssemeijer N. Clinical evaluation of a computer-aided diagnosis system for determining cancer aggressiveness in prostate MRI. Eur Radiol. 2015; 25:3187–3199.
- Donati OF, Mazaheri Y, Afaq A, et al. Prostate cancer aggressiveness: assessment with whole-lesion histogram analysis of the apparent diffusion coefficient. Radiology. 2014; 271(1):143–152.
- Bae H, Yoshida S, Matsuoka Y, et al. Apparent diffusion coefficient value as a biomarker reflecting morphological and biological features of prostate cancer. Int Urol Nephrol. 2014; 46(3):555–561.
- Quon JS, Bardia Moosavi B, Khanna M, et al. False positive and false negative diagnoses of prostate cancer at multi-parametric prostate MRI in active surveillance. Insights Imaging. 2015; 6:449–463.
- Tan CH, Hobbs BP, Wei W, et al. Dynamic contrast enhanced MRI for the detection of prostate cancer: meta-analysis. Am J Roentgenol. 2015; 204: W439–48.
- Hassanzadeh E, Glazer DI, Dunne RM, et al. Prostate imaging reporting and data system version 2 (PI-RADS v2): a pictorial review. Abdom Radiol. 2017; 42:278–289.
- Furlan A, Borhani AA, Westphalen AC. Multiparametric MR imaging of the Prostate Interpretation Including Prostate Imaging Reporting and Data System Version 2. Radiol Clin N Am. 2018, 56: 223–238.
Articole din ediţiile anterioare
Managementul cancerului de prostată rezistent la castrare
Cancerul de prostată rezistent la castrare (CRPC) este un aspect important al practicii noastre clinice în fiecare zi. Pentru o perioadă foarte lun...
Evaluarea IRM multiparametrică în hiperplazia benignă de prostată – o adevărată provocare în excluderea cancerului de prostată
Evaluarea IRM multiparametrică este un instrument de nepreţuit în depistarea, localizarea şi caracterizarea leziunilor de prostată, una dintre ...
Aspecte IRM ale leziunilor PI-RADS 5 – experienţa unui centru terţiar
Cancerul de prostată este una dintre cele mai frecvente afecţiuni maligne în rândul bărbaţilor, pentru care se depun eforturi sporite, cu scop...