The practice of medicine has been constantly evolving throughout the course of human history. Treatments and therapies have been developed and abandoned as evidence and experimentation have shown us the errors and successes of various types of care. Less obvious, though, is the role of language and its influence on how care is administered throughout the world. This is especially true in the practice of hospice, palliative care, and in the practice of a relatively new concept: supportive care. This article aims to discuss the general history of the subspecialty known in the United States of America as hospice and palliative medicine, and the terminology that has been used to describe the spectrum of end-of-life care, terminal disease care, and the holistic approach to pain and symptom management in patients who have life-altering, chronic diseases. Research has begun to ask questions about how the language used in this field may inspire feelings of fear and hopelessness, in both patients and providers. Such bias and negative connotation may limit access to care which oncologic and palliative care organizations worldwide consider an essential component to best-practice delivery of medicine.
Îngrijire paliativă sau suportivă? O perspectivă istorică asupra utilizării limbajului în practică
Palliative or supportive care? A historical perspective on language in practice
First published: 14 decembrie 2019
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/OnHe.49.4.2019.2737
Abstract
Rezumat
Arta de practicare a medicinei a evoluat în permanenţă de-a lungul istoriei. Diferite tratamente şi terapii au fost folosite sau abandonate ca urmare a succesului sau eşecului diverselor metode de îngrijire medicală implementate. Un aspect mai puţin evident este rolul jucat de limbajul medical la nivel naţional şi internaţional, în special atunci când ne referim la îngrijirea paliativă, hospice şi îngrijirea suportivă, acesta din urmă fiind un termen relativ nou, devenit popular în Statele Unite ale Americii. Autorii articolului au analizat diferenţele de definire a îngrijirii paliative şi a celei suportive şi felul în care limbajul de adresare poate influenţa percepţia atât a pacienţilor, cât şi a medicilor despre îngrjirea paliativă, inducând sentimente de frică şi descurajare. Într-un final, aceste prejudecăţi şi conotaţii negative pot limita accesul pacienţilor la serviciile de îngrijire paliativă, pe care organizaţiile din domeniul oncologic şi din domeniul paliaţiei le consideră o componentă esenţială a celor mai bune practici de îngrijire medicală.
In the distant reaches of human history, when the expansion of civilization was limited by tribalism and geography, the care of the infirm and the dying was in the hands of the ill person’s family or their immediate local community. As the interpersonal connections of human beings expanded, with the rise of various religious groups and expectations of distant pilgrimage, so too rose a need to house and care for those travelers who were unable to complete their journeys(1). Thus were the first hospitals established.
Both the words hospital and hospice share a common linguistical root in the latin word hospes, meaning “guest” or “host”. The first documented use of the word hospice in American English, according to Merriam-Webster, was in 1818, in reference to a lodging for travelers, especially those maintained by a religious group or order(2). The modern hospice movement grew out of this ancient model of charity care and was continued by religious orders in the 18th and 19th centuries. This culminated in the work of Dr. Cicely Saunders, who founded the first hospice in the modern sense: a place for the care of the terminally ill that was not restricted to particular diseases, social classes, or religious beliefs(1).
During the initial development of hospice programs in North America, it was noted by Dr. Balfour Mount, a surgical oncologist and pioneer of end-of-life care in Canada, that the word hospice was already in frequent use in the French-speaking province of Quebec, where it designated a home for the elderly. Additionally, Dr. Mount felt that it would be difficult to acquire funding to start a hospice, at least in the traditional sense as a physical location for the terminally ill to receive care. It was Dr. Mount who then coined the phrase palliative care to describe his new ward for the dying at Royal Victoria Hospital in Montreal(3).
The phrase palliative care has also a root in Latin: pallium – a cloak(4). Thus, palliative care is that which cloaks or hides the manifestations of disease but does not cure it. Other English words with distressing connotations derive from the same Latin root, including pallbearer – a person charged with carrying a coffin during a burial. Given this linguistic history, there has been an increase in awareness of possible cultural and social biases among patients and caregivers in relation to the phrases “hospice” or “palliative care”, which may limit the adoption or consideration of such services(5-8).
Palliative care is defined by the World Health Organization (WHO) as “an approach that improves the quality of life of patients and their families facing the problem associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual”. WHO emphasizes that palliative care should not serve to “hasten or postpone death” and that palliative care is “applicable early in the course of illness, in conjunction with other therapies that are intended to prolong life, such as chemotherapy or radiation therapy, and includes those investigations needed to better understand and manage distressing clinical complications”. This definition serves as a succinct clarification that palliative care is holistic, team-based and focused on guiding a patient and their family through the challenges of pain, distressing symptoms, and complications of treatment. It is not, in the view of WHO, completely synonymous with end-of-life care, but a complement to standard care for any patient facing a potentially life-threatening disease and a means to ensure comfort and support in the event an illness progresses to a terminal state(9).
WHO has also developed a supplemental definition for palliative care for the pediatric population, which highlights concepts to emphasize when providing care to children. WHO recommends a focus on multidisciplinary and holistic “mind-body-spirit” support for the child and their family that is initiated regardless of care setting or resource limitations, at the time of diagnosis and continued throughout the course of disease regardless of the treatment plan for the underlying condition(9).
The European Association for Palliative Care (EAPC) defined the same field of medicine as: “Palliative care is the active, total care of the patient whose disease is not responsive to curative treatment. Control of pain, of other symptoms, and of social, psychological and spiritual problems is paramount. Palliative care is interdisciplinary in its approach and encompasses the patient, the family and the community in its scope. In a sense, palliative care is to offer the most basic concept of care – that of providing for the needs of the patient wherever he or she is cared for, either at home or in the hospital. Palliative care affirms life and regards dying as a normal process; it neither hastens nor postpones death. It sets out to preserve the best possible quality of life until death”(10).
These two definitions are illustrative of a problem in the language used to describe the care provided to a patient with a potentially life-limiting disease. Classically – and as suggested by the definition provided by EAPC –, the palliative care concept may be interpreted as care for the patient who is not yet dying but has a disease that will progress to end of life and cannot be cured. Yet, as noted in the WHO definition, palliative care should be initiated early and in conjunction with disease modifying therapy. The limitations of terminology have resulted in confusion for both providers and the lay public(7).
Seemingly in response to this problem, a fairly new term, supportive care, has emerged in this domain of medicine and was enthusiastically embraced by many palliative care programs in the Unites States. Many hospitals are now using “supportive care” or “supportive medicine” in their department or division naming schemes. This initiative prompted many queries on what made “supportive care” a unique concept and why it had such traction at national and international levels.
The Multinational Association for Supportive Care in Cancer (MASCC) has defined supportive care in cancer as “the prevention and management of the adverse effects of cancer and its treatment. This includes management of both physical and psychological symptoms and side effects across the continuum of the cancer experience from diagnosis, through anticancer treatment, to post-treatment care. Enhancing rehabilitation, secondary cancer prevention, survivorship, and end-of-life care are integral to supportive care”. MASCC has suggested that, by expanding the traditional palliative care model into early management and survivorship, providers can ensure an improved quality of life through better symptom management, can promote improved tolerance of therapy and toxicities, and can lessen the emotional burden of cancer for the patient and their family(11).
The National Cancer Institute (NCI) has defined supportive care as “care given to improve the quality of life of a patient who have a serious or life-threatening disease. The goal of supportive care is to prevent or treat as early as possible the symptoms of a disease, side effects caused by treatment of a disease, and psychological, social and spiritual problems related to a disease or its treatment. Also called comfort care, palliative care, and symptom management”(12). Therefore, according to NCI, these three terms are used interchangeably. The European Society for Medical Oncology (ESMO) has developed similar guidelines in supportive and palliative care. The organization also describes “supportive care” and “palliative care” as interchangeable terms. The ESMO Guidelines in Supportive and Palliative Care include recommendations for the management of cancer pain in adult population, constipation and diarrhea, delirium, nausea and vomiting, dyspnea and other symptoms commonly encountered in palliative medicine covered by the aforementioned guidelines(13).
EAPC recognizes that the phrases supportive care and palliative care are often used interchangeably and with significant overlap, though it is also recognized that supportive care is often used in the context of adverse symptoms of cancer and associated treatments and lacks the generality of palliative care(10).
Our institution, City of Hope National Medical Center, within its patient-facing online educational materials explicitly states that the phrases “supportive care” and “palliative care” have similar meaning, but notes that other institutions may consider each to be a distinct service. It provides an example of supportive care as services offered to patients for prevention and treatment of symptoms of cancer – including the psychosocial and spiritual ones – or side effects from the cancer treatments. This is contrasted with palliative care as a specialized medical service for patients with serious or life-threatening illness, with its main focus on relieving pain and other symptoms to prevent suffering.
The National Comprehensive Cancer Network (NCCN) has explicitly developed guidelines in supportive care, utilizing the phrase as a general descriptor with additional subcategories of guidelines for palliative care, adult cancer pain, antiemesis, cancer-related fatigue, distress management and survivorship, among others. In this approach to the terminology, one may come to the conclusion that palliative care is a part or subset of supportive care(14).
Several articles by the palliative care group at MD Anderson Cancer Center dedicated to integration of palliative care into oncological care and at similarities and differences between palliative care and supportive care concluded that:
1. Hospice care is a form of medical care aimed at patients at the end of their life and their families that represents a community-based form of palliative care and an integral part of the palliative care.
2. Palliative care represents medical services offered to patients with advanced cancer in both hospital and community settings, with palliative care being a subdivision of supportive care.
3. Supportive care represents all services offered to patients from the moment of diagnosis throughout their cancer journey until end of life or survivorship and intended to address these patients’ informational, emotional, spiritual, social and physical needs(15-17).
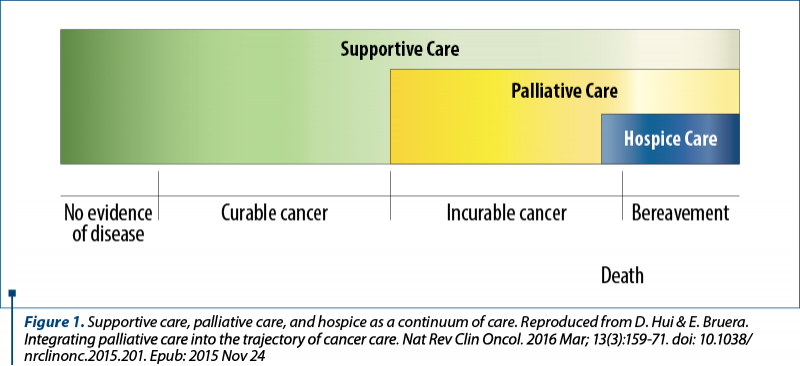
The relationship between these three terms is presented in Figure 1.
A review of the literature suggests that the term “supportive care” has gained significant traction through both patient and provider preferences. This has prompted several trials in implementation of the term as a replacement for care traditionally described as palliative care, with positive results in both provider and lay groups(5-8,17-19).
A common theme across these analyses – whether sourced from a patient, lay caregiver, or healthcare professional – is an inappropriate expectation that palliative care is equivalent to end-of-life care, or that the recommendation of initiating palliative care is a signal of lost hope. From the perspective of the patient or their caregivers, the recommendation of palliative care may suggest a change for the worse or that other treatments may be withheld(5). Maciasz et al. have concluded that supportive care is a term perceived more favorably than palliative care in patients with advanced cancer, and the fact that palliative care is perceived as end-of-life care may be one of the explanations why patients with cancer receive palliative care in the later stage of their disease, especially when this misunderstanding is not addressed by their oncologists(7). Another study that surveyed a sample of 103 oncology patients mentioned that patients who were convinced that palliative care was reserved only for end-of-life cases were more likely to feel hopeless or frightened. The same study mentioned that patients were more likely to accept palliative care services if they were told these services were not for end of life(5). Another study concluded, based on the observation that patients were also unaware that pastoral care, social work, psychology and bereavement were also part of the palliative care services or that palliative care services extend beyond the end-of-life care, that patient education was crucial for a successful integration of palliative care services in oncology(5).
From the providers point of view, several articles have mentioned that the term palliative care may act as a barrier to early patient referral in oncology because it may be perceived as causing distress and hopelessness in patients and their families; therefore, oncologists are more likely to refer patients to services called “supportive care”(7,18). Maciasz et al. note that subspecialty training within this field in the United States is governed by the Board of Hospice and Palliative Medicine; the researchers speculate that the name of the board and subspecialty training may be contributing factors to the perceived equivalency of palliative care and end-of-life care. They also suggest that, if the term “supportive medicine” continues to gain wide acceptance, a change in the name of this subspecialty may be considered in the future(7).
The idea that palliative care is reserved solely for end-of-life cases is untenable and must be aggressively addressed. Maciasz and his team concluded that the lack of familiarity with the similarities and differences between palliative and supportive care presents itself as an opportunity for the palliative care providers to properly introduce their services and subspecialty to both patients and oncologists. He argues that adequate delivery of palliative or supportive care throughout the world is dependent on recognition of both(7). The misconceptions about palliative care, triggered by lack of education or even by fear, may hinder early integration of palliative care in oncology that would go against literature showing that early use of palliative care can enhance patients’ quality of life, mood, understanding of their prognostic or utilization of resources at the end of life. Such gaps in evidence-based good practice are against recent recommendations from organizations such as NCCN, ESMO, and the Institute of Medicine. In its most recent recommendations, The American Society for Clinical Oncology (ASCO) stated that “patients with advanced cancer, whether inpatient or outpatient, should receive dedicated palliative care services, early in the disease course, concurrent with active treatment. Referring patients to interdisciplinary palliative care team is optimal, and services may complement existing programs”(7,20).
It is self-evident that words and language can provoke emotional and visceral reactions which may vary widely depending on context, culture, prior experiences, and expectations of the medical system. Knowing this, it is imperative of the worldwide medical community to appreciate how language will affect the physical and mental health of patients and their families in all stages of the disease. The education of the lay public and healthcare providers is certainly a priority, but so is the acceptance of one of the greatest advances in modern medicine: that change in the face of supporting evidence is for the good of the patient. Linguistic status quo for the sake of tradition or the honor of past discovery should fall away to language that is both understood and appreciated by those who are most affected by it.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Lutz S. The History of Hospice and Palliative Care. Curr Probl Cancer. 2011; 35(6):304-309. doi:10.1016/j.currproblcancer.2011.10.004
- Hospice. Merriam-Webster. https://www.merriam-webster.com/dictionary/hospice. Published 2019. Accessed November 7, 2019.
- Duffy A. A Moral Force: The Story of Dr. Balfour Mount. The Ottawa Citizen. https://web.archive.org/web/20130528195548/http://www.canada.com/ottawacitizen/story.html?id=896d005a-fedd4f50-a2d9-83a95fc56464&p=2. Published April 25, 2005.
- Palliate. Definition of Palliate by Merriam-Webster. https://www.merriam-webster.com/dictionary/palliate. Accessed November 19, 2019.
- Chosich B, Burgess M, Earnest A, et al. Cancer patients’ perceptions of palliative care. Support Care Cancer. June 2019; doi:10.1007/s00520-019-04917-8
- Taber JM, Ellis EM, Reblin M, Ellington L, Ferrer RA. Knowledge of and beliefs about palliative care in a nationally-representative U.S. sample. Graetz I, ed. PLoS One. 2019; 14(8):e0219074. doi:10.1371/journal.pone.0219074
- Maciasz RM, Arnold RM, Chu E, et al. Does it matter what you call it? A randomized trial of language used to describe palliative care services. Support Care Cancer. 2013; 21(12):3411-3419. doi:10.1007/s00520-013-1919-z
- Zimmermann C, Swami N, Krzyzanowska M, et al. Perceptions of palliative care among patients with advanced cancer and their caregivers. CMAJ. 2016; 188(10):E217-E227. doi:10.1503/cmaj.151171
- https://www.who.int › cancer › palliative › definition
- Radbruch L, Payne S. White paper on standards and norms for hospice and palliative care in Europe: Part 1. Eur J Palliat Care. 2009; 16(6):278-289.
- https://www.mascc.org/mascc-strategic-plan
- https://www.cancer.gov › publications › dictionaries › cancer-terms › definitions
- https://www.esmo.org/Guidelines/Supportive-and-Palliative-Care
- https://www.nccn.org › professionals › physician_gls
- Hui D, Bruera E. Integrating palliative care into the trajectory of cancer care. Nat Rev Clin Oncol. 2016 Mar; 13(3):159-71. doi: 10.1038/nrclinonc.2015.201. Epub 2015 Nov 24.
- Bruera E, Hui D. Conceptual models for integrating palliative care at cancer centers. J Palliat Med. 2012 Nov; 15(11):1261-9. doi: 10.1089/jpm.2012.0147. Epub 2012 Aug 27.
- Hui D, Bruera E. Models of integration of oncology and palliative care. Ann Palliat Med. 2015 Jul; 4(3):89-98. doi: 10.3978/j.issn.2224-5820.2015.04.01.
- Fadul N, Elsayem A, Palmer JL, et al. Supportive versus palliative care: What’s in a name? Cancer. 2009; 115(9):2013-2021. doi:10.1002/cncr.24206
- Rhondali W, Burt S, Wittenberg-Lyles E, Bruera E, Dalal S. Medical oncologists’ perception of palliative care programs and the impact of name change to supportive care on communication with patients during the referral process. A qualitative study. Palliat Support Care. 2013; 11(5):397-404. doi:10.1017/S1478951512000685
- Ferrel BR, Temel JS, Temin S, Alesi ER, Balboni TA, Basch EM, Firn JI, Paice JA, Pepercorn JM, Phillips T, Stovall EL, Zimmermann C, Smith TJ, Integration of Palliative Care Into Standard Oncology Care: American Society of Clinical Oncology Clinical Practice Guideline Update. J Clin Oncol. 2017 Jan; 35(1):96-112. Epub 2016 Oct 28.
Articole din ediţiile anterioare
Îngrijirile paliative – prezent şi viitor
Îngrijirile paliative iau o amploare din ce în ce mai mare în întreaga lume, iar pandemia de COVID-19 a accentuat nevoia pentru astfel de îngrijiri.
Importanţa îngrijirilor paliative în oncologia medicală – utilizarea scalei IPOS
Acest articol prezintă succint argumentele care determină nevoia de integrare a oncologiei medicale cu îngrijirile paliative, accentuând necesi...
Îngrijirile paliative în stadiul de sfârşit al vieţii în bolile oncologice
Starea terminală este un capitol al îngrijirilor paliative care suscită interes pentru lumea ştiinţifică, dar şi în cadrul practicii medicale. Exis...