Tendinţe privind mastectomia pentru cancerul de sân în stadii incipiente: experienţa unui centru medical
Mastectomy trends for early-stage breast cancer: a single-center experience
Abstract
Breast cancer is a major public health problem in Romania, representing the first cause of mortality for women between 15 and 49 years old. Despite the latest developments in medication, surgery continues to represent a crucial role in breast cancer treatment. Studies analyzing mastectomy versus breast-conserving surgery (BCS) followed by radiation therapy show comparable overall survival rate and disease-free survival rate. However, the percentage of women electing BCS varies depending on country. Age is considered the most frequent sociodemographic factor affecting the choice of surgery. We studied a small lot of patients to assess whether the surgical choice of patients with breast cancer could be correlated with global trends. The patients were diagnosed with early-stages (IA-IIIA) breast cancer and underwent either BCS or mastectomy. The results show that 28 patients (32.94%) underwent breast-conserving surgery, while the remaining 57 patients (67.05%) had mastectomy, from a total of 85 women. There was no significant difference between the age groups in term of surgical choice. Patients aged younger than 50 years of age chose radical mastectomy in greater numbers compared to the ones who chose BCS: 65.63% (21 patients) had mastectomy while 34.38% (11 patients) had BCS. Regarding the 50 to 64 years old age group, mastectomy was performed on 25 patients (67.57%) versus 12 patients (32.43%) who had BCS. Patients older than 65 years old also predominately underwent mastectomy (11 patients; 68.75%), whilst 5 patients (31.25%) had BCS.Keywords
breast cancerBCSmastectomyageRezumat
Cancerul de sân este o problemă majoră de sănătate publică în România, reprezentând prima cauză de mortalitate pentru femeile între 15 şi 49 de ani. În ciuda ultimelor medicamente antitumorale recent introduse în terapeutică, intervenţia chirurgicală continuă să reprezinte un element crucial în tratamentul cancerului de sân. Studii care analizează mastectomia versus chirurgia de conservare a sânului (BCS) urmată de radioterapie relevă o rată de supravieţuire globală şi o rată de supravieţuire fără progresie comparabile. Cu toate acestea, procentul dintre femeile care aleg BCS variază în funcţie de ţară. Vârsta este considerată cel mai frecvent factor sociodemografic care afectează alegerea intervenţiei chirurgicale. Am studiat un lot de paciente pentru a evalua dacă alegerea chirurgicală a pacientelor cu cancer de sân ar putea fi în concordanţă cu tendinţele globale. Pacientele au fost diagnosticate cu stadii incipiente (IA-IIIA) de cancer de sân şi au efectuat fie BCS, fie mastectomie. Rezultatele arată că 28 de paciente (32,94%) au suferit intervenţii chirurgicale conservatoare, în timp ce restul de 57 de paciente (67,05%) au efectuat mastectomie, dintr-un total de 85 de femei. Nu a existat o diferenţă semnificativă între grupurile de vârstă privind alegerea tratamentului chirurgical. Pacientele cu vârsta mai mică de 50 de ani au ales mastectomia radicală, totuşi în număr mai mare comparativ cu cele care au ales BCS: 65,63% (21 de paciente) au efectuat mastectomie, în timp ce 34,38% (11 paciente) au efectuat BCS. În ceea ce priveşte grupa de vârstă cuprinsă între 50 şi 64 de ani, mastectomia a fost efectuată la 25 de paciente (67,57%), faţă de 12 paciente (32,43%) care au ales BCS. Pacientele cu vârsta de peste 65 de ani au efectuat predominant mastectomie (11 paciente; 68,75%), în timp ce 5 paciente (31,25%) au efectuat BCS.Cuvinte Cheie
cancer de sânBCSmastectomievârstăIntroduction
According to International Agency for Research on Cancer (IARC) statistics, 1 in 8 women in the European Union (27 member states) and the former member United Kingdom will develop breast cancer before the age of 85 years old. In Europe, an average of 20% of breast cancer cases occur in women younger than 50 years old; 36% appear between the ages of 50 and 64, while the remaining cases are reported above this age(1).
Breast cancer is considered to be the most frequent cancer among women across European Union countries, with more than 400,000 cases diagnosed each year. The most important risk factors for breast cancer are considered to be age, genetic predisposition, estrogen replacement therapy, and lifestyle factors, including obesity, physical inactivity, nutrition habits and alcohol consumption(2).
Breast cancer is a major public health problem in Romania, representing the first cause of mortality (8.68%) for women between 15 and 49 years old. According to Globocan 2018 statistics, Romania has an annual mortality comparable to the European average, although the reported incidence of breast cancer in Romania is 30% lower.
The long-term results of international, randomized clinical trials have described equivalent survival between the majority of patients with stage I or II breast cancer who had breast-conserving surgery (BCS) followed by radiation therapy (RT) and the group that underwent mastectomy(3,4). Although more data are required, some observational studies suggest possible improved survival and reduced recurrence rates with BCS(5-8).
An important aspect to be taken into consideration is that the risk of complications is almost twice as high for women who undergo mastectomy with reconstructive surgery compared to BCS plus radiation therapy(9). The reasons for BCS-eligible patients to choose mastectomy include reluctance to undergo radiation therapy after BCS and fear of disease recurrence(10-12). According to the data published so far, there are three categories of women who are more likely to undergo mastectomy: younger women (those under 40 years of age), patients with larger and/or more aggressive tumors, and those who live further from their treatment facility(13,14).
Due to the reduced risk of cancer recurrence (about 50% at 10 years) and the risk of breast cancer death (almost 20% at 15 years) for patients treated with radiation, BCS is typically followed by radiotherapy(4).
Given the particular importance of breast cancer in Romania, we studied a small lot of patients from our region to assess whether the surgical choice of patients with breast cancer could be correlated with global statistics.
Method
Patients treated for breast cancer at the Filantropia Clinical Hospital of Craiova, Romania, over a period of almost 10 years (between August 2007 and March 2017) were included in our retrospective study.
We have gathered data from 85 patients with breast cancer stages ranging from IA to IIIA. The participants were only female patients, there were no male patients whose data corresponded to our eligibility criteria.
The inclusion criteria were: patients age >18 years old, early-stages (I-IIIA) breast cancer diagnosed, which have underwent radical or breast conservatory surgery. IIIB and IV stages were excluded.
The following data were recorded for each patient: baseline information (age and sex), as well as diagnosis date, disease stage and TNM classification. The information about neoadjuvant chemo- and radiotherapy, adjuvant chemo- and radiotherapy were also recorded. We entered data regarding each patient surgery type: radical or conservatory. The informed consent was obtained from each patient. The analysis was performed with descriptive statistics – mean, relative frequency, standard deviation.
Results
From a total of 95 patients, 85 were included in the study after signing the informed consent. The remaining 10 patients (10.53%) were diagnosed with stages IIIB (8.42%) and IV (2.11%) breast cancer, and did not fulfill the inclusion criteria.
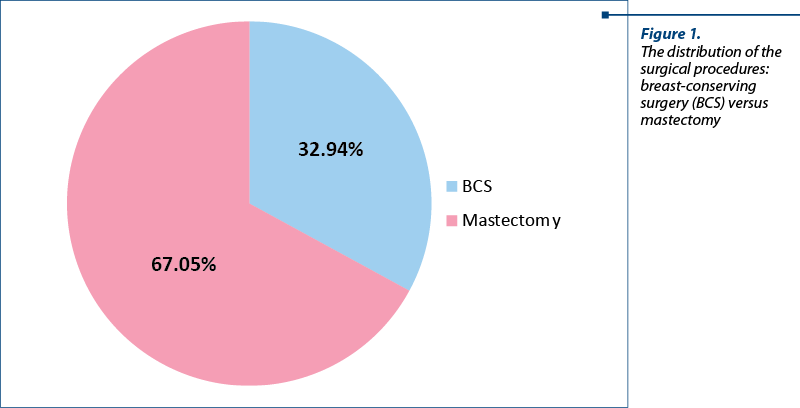
The mean age of the study population was 53 years old (range: 27-87 years old). The patients diagnosed with early stages (IA-IIIA) breast cancer underwent either BCS or mastectomy, as follows: 28 patients (32.94%) underwent breast-conserving surgery, while the remaining 57 patients (67.05%) had mastectomy (Figure 1). The median age of the subgroup of patients who underwent BCS and of the subgroup that had mastectomy is relatively close: 52.1 years old for BCS versus 53.4 years old – the average age of the mastectomy surgery.
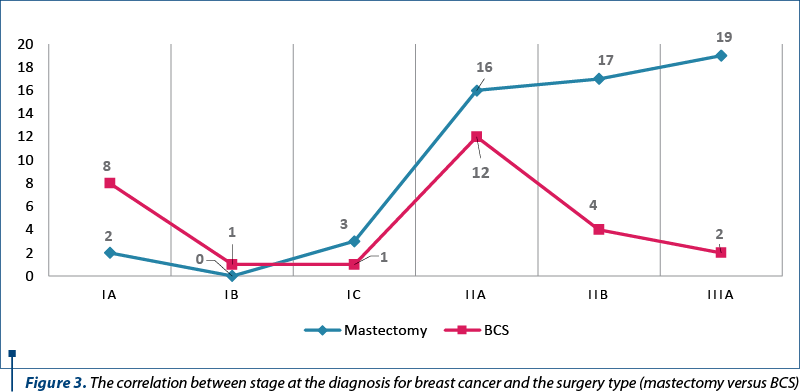
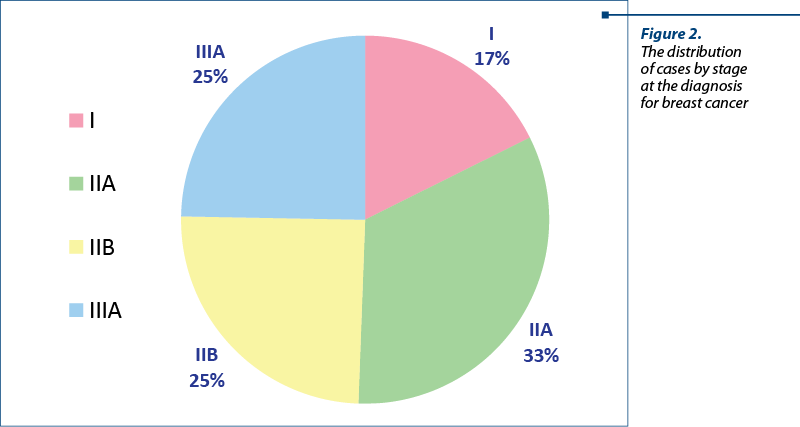
The distribution of cases by stage at diagnosis for breast cancer is presented in Figure 2, while the correlation between stages and the surgery type is depicted in Figure 3. More advanced stages were associated with higher rates of mastectomy.
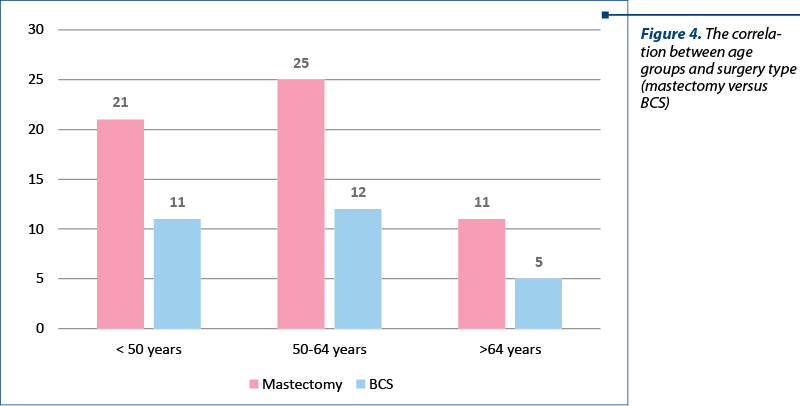
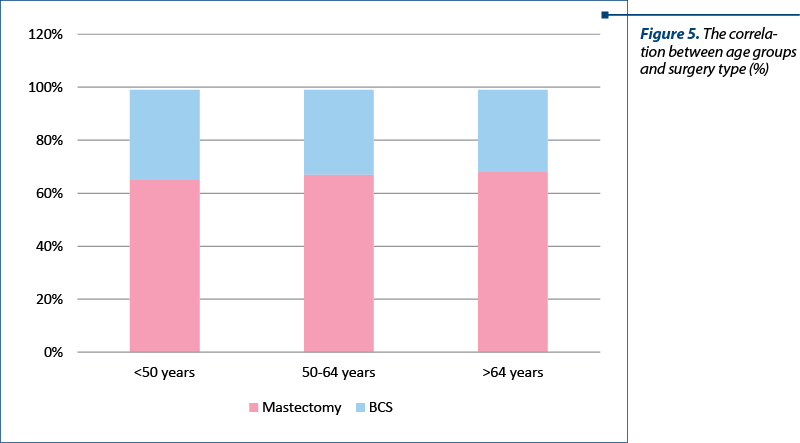
The patients were further divided into three categories depending on age: the young subgroup (<50 years old), middle-age subgroup (50-64 years old) and older subgroup (>64 years old). Patients younger than 50 years of age predominantly underwent mastectomy – 65.63% (21 patients), while 34.38% (11 patients) had BCS. Regarding the 50 to 64 years age group, mastectomy was performed on 25 patients (67.57%) versus 12 patients (32.43%) who had BCS. Patients older than 64 years old also generally underwent mastectomy: 11 patients (68.75%), whilst 5 patients (31.25%) had BCS (Figures 4 and 5). There was no significant difference between the age groups in terms of surgical choice.
Discussion
Surgery continues to represent a crucial component in breast cancer treatment, despite the latest developments in medication. Studies analyzing mastectomy versus BCS followed by radiation therapy show comparable overall survival rate and disease-free survival rate for the two operations(15,16). Additionally, BCS is followed by less surgical complications and increases cosmetic outcome for patients(17,18). As a result, this procedure is recommended by the US National Institutes for Health for early breast cancer stage and is chosen by 60% of patients in the USA(19). Globally, the percentage of women electing BCS varies. While Europe has similar high rate to USA (73% of patients receive BCS), China has a nationwide rate of 11%(20,21). Our regional study reveals a decreased rate of breast-conserving surgery (32.94%) compared to European countries and USA.
Studies assessing the sociodemographic factors affecting the choice of surgery reported age as the most frequent, offering multiple explanations as to how age influenced the patients’ decision(22). The most common results show a likelihood for the extremes of diagnostic age to undergo mastectomy. Specifically, increasing age is correlated with a decreasing probability of choosing BCS. Compared with a group of 65 to 69 years old, all older age groups including 70 to 74 years, 75 to 79 years, and 80+ years were less inclined to elect BCS(23). Moreover, the results from two other large studies suggest that younger women also tend to choose BCS. Patients aged less than 40 years and older than 64 years were more likely to undergo mastectomy than 40 to 46 years old age group(24). After analyzing a large cohort of over 100,000 patients, it was reported that women younger than 50 years old and those older than 65 years old elected mastectomy far often than those aged 50 to 64 years old(25). However, our study shows similar rates for mastectomy across all age groups.
The possible explanations for the reluctance of patients older than 60 to undergo BCS could be the decreased interest in cosmetic results and a greater concern over the effects of radiation therapy on their bodies(26). Overall, the main individual belief factors for women to undergo radical breast surgery were fear of cancer recurrence (mastectomy was considered the most reassuring option), a more expedient procedure (it provides a rapid treatment for employment, as well as domestic concerns), and avoiding the potential side effects of radiation therapy(24,27-30). Conversely, women choosing BCS mentioned body image concerns, equivalent long-term survival, and the lesser extent of the surgery(22).
Furthermore, the clinicopathological factors also play a significant role in the choice of treatment. Among them, a larger tumor size is frequently associated with a higher rate of radical breast surgery. Correspondingly, our study shows an association between more advanced stages and higher rates of mastectomy. The reasons behind this correlation are diverse and can potentially influence the surgeon recommendation. First, a large tumor requires a more challenging surgical procedure and can be associated with a higher rate of re-excision(31,32). Secondly, the risk of local recurrence increases with the size of the tumor(33-35). Also, the cosmetic outcome can be less satisfying. Regarding individual belief factors, a large tumor can alter the patients’ understanding of the severity of the neoplasm and their faith in the outcome of a breast-conserving surgery(22). In terms of physician-related factors, increased BCS rates are correlated with surgeons which possess the following characteristics: higher case number, training, as well as female gender(23).
The lack of data on whether the BCS-eligible patients were explicitly given the opportunity to choose between the procedures could have influenced the results of our study and could potentially explain the high rates of mastectomies. It is unclear to what extent the surgeon interfered in the decision-making process. Also, without a long postoperative follow-up interval on the patients, this study is unable to compare the overall survival rate and disease-free survival rate.
Conclusions
There was no significant difference between the age groups in term of surgical choice in the study population. Approximately two thirds of women underwent mastectomy compared to BCS followed by radiotherapy, with similar rates across all age groups. These results could suggest that Romania has lower rates of BCS for breast cancer compared with the European and American averages, while maintaining higher percentages in comparison to Asian countries.
Conflicts of interests: The authors declare no conflict of interests.
Bibliografie
- Forman D, Bray F, Brewster DH, Gombe Mbalawa C, Kohler B, Piñeros M, Steliarova-Foucher E, Swaminathan R, Ferlay J (editors). Cancer Incidence in Five Continents, Vol. X. IARC Scientific Publication. 2014; No. 164. Lyon: International Agency for Research on Cancer.
- Ferlay J, Colombet M, Soerjomataram I, Mathers C, Parkin D, Piñeros M, et al. Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. International Journal of Cancer. 2018; 144(8):1941-1953.
- Chen Y, Jiang L, Gao B, Cheng Z, Jin J, Yang K. Survival and disease-free benefits with mastectomy versus breast conservation therapy for early breast cancer: a meta-analysis. Breast Cancer Research and Treatment. 2016; 157(3):517-525.
- Early Breast Cancer Trialists’ Collaborative Group (EBCTCG), Darby S, McGale P, Correa C, Taylor C, Arriagada R, Clarke M, Cutter D, Davies C, Ewertz M, Godwin J, Gray R, Pierce L, Whelan T, Wang Y, Peto R. Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: meta-analysis of individual patient data for 10,801 women in 17 randomised trials. The Lancet. 2011; 378(9804):1707-1716.
- van Maaren M, de Munck L, de Bock G, Jobsen J, van Dalen T, Linn S et al. 10-year survival after breast-conserving surgery plus radiotherapy compared with mastectomy in early breast cancer in the Netherlands: a population-based study. The Lancet Oncology. 2016; 17(8):1158-1170.
- Hartmann-Johnsen O, Kåresen R, Schlichting E, Nygård J. Survival is Better After Breast Conserving Therapy than Mastectomy for Early Stage Breast Cancer: A Registry-Based Follow-up Study of Norwegian Women Primary Operated Between 1998 and 2008. Annals of Surgical Oncology. 2015; 22(12):3836-3845.
- Hwang E, Lichtensztajn D, Gomez S, Fowble B, Clarke C. Survival after lumpectomy and mastectomy for early stage invasive breast cancer. Cancer. 2013; 119(7):1402-1411.
- Agarwal S, Pappas L, Neumayer L, Kokeny K, Agarwal J. Effect of Breast Conservation Therapy vs Mastectomy on Disease-Specific Survival for Early-Stage Breast Cancer. JAMA Surgery. 2014; 149(3):267.
- Smith B, Jiang J, Shih Y, Giordano S, Huo J, Jagsi R, et al. Cost and Complications of Local Therapies for Early-Stage Breast Cancer. Journal of the National Cancer Institute. 2016; 109(1):djw178.
- Lautner M, Lin H, Shen Y, Parker C, Kuerer H, Shaitelman S, et al. Disparities in the Use of Breast-Conserving Therapy Among Patients With Early-Stage Breast Cancer. JAMA Surgery. 2015; 150(8):778.
- Kummerow K, Du L, Penson D, Shyr Y, Hooks M. Nationwide Trends in Mastectomy for Early-Stage Breast Cancer. JAMA Surgery. 2015; 150(1):9.
- McGuire K, Santillan A, Kaur P, Meade T, Parbhoo J, Mathias M et al. Are Mastectomies on the Rise? A 13-Year Trend Analysis of the Selection of Mastectomy Versus Breast Conservation Therapy in 5865 Patients. Annals of Surgical Oncology. 2009; 16(10):2682-2690.
- Bellavance E, Kesmodel S. Decision-Making in the Surgical Treatment of Breast Cancer: Factors Influencing Women’s Choices for Mastectomy and Breast Conserving Surgery. Frontiers in Oncology. 2016; 6:74.
- Freedman R, Virgo K, Labadie J, He Y, Partridge A, Keating N. Receipt of locoregional therapy among young women with breast cancer. Breast Cancer Research and Treatment. 2012; 135(3):893-906.
- Clarke M, Collins R, Darby S, Davies C, Elphinstone P, Evans V, Godwin J, Gray R, Hicks C, James S, MacKinnon E, McGale P, McHugh T, Peto R, Taylor C, Wang Y; Early Breast Cancer Trialists’ Collaborative Group (EBCTCG). Effects of radiotherapy and of differences in the extent of surgery for early breast cancer on local recurrence and 15-year survival: an overview of the randomised trials. The Lancet. 2005; 366(9503):2087-2106.
- Morris AD, Morris RD, Wilson JF, White J, Steinberg S, Okunieff P, et al. Breast conserving therapy versus mastectomy in early stage breast cancer: a meta-analysis of 10 year survival. Cancer J Sci Am. 1997; 3:6–12
- Al-Ghazal SK, Fallowfield L, Blamey R. Comparison of psychological aspects and patient satisfaction following breast conserving surgery, simple mastectomy and breast reconstruction. Eur J Cancer. 2000; 36:1938–43.
- Schain WS, D’Angelo TM, Dunn ME, Lichter AS, Pierce LJ. Mastectomy versus conservative surgery and radiation therapy: psychological consequences. Cancer. 1994; 73:1221–8.
- Lee MC, Rogers K, Griffith K, Diehl KA, Breslin TM, Cimmino VM, et al. Determinants of breast conservation rates: reasons for mastectomy at a comprehensive cancer center. Breast J. 2009; 15:34–40.
- Garcia-Etienne CA, Tomatis M, Heil J, Friedrichs K, Kreienberg R, Denk A et al; eusomaDB Working Group. Mastectomy trends for early-stage breast cancer: a report from the EUSOMA multi-institutional European database. Eur J Cancer. 2012; 48: 1947–1956.
- Li J, Zhang BN, Fan JH, Pang Y, Zhang P, Wang SL, et al. A nation-wide multicenter 10-year (1999-2008) retrospective clinical epidemiological study of female breast cancer in China. BMC Cancer. 2011; 11:364–74.
- Gu J, Groot G, Boden C, Busch A, Holtslander L, Hyun L. Review of Factors Influencing Women’s Choice of Mastectomy Versus Breast Conserving Therapy in Early Stage Breast Cancer: A Systematic Review. Clinical Breast Cancer. 2017; 18(4):e539-4
- Hershman DL, Buono D, Jacobson JS, et al. Surgeon characteristics and use of breast conservation surgery in women with early stage breast cancer. Ann Surg. 2009; 249:828-33.
- Olaya W, Wong JH, Morgan JW, Roy-Chowdhury S, Lum SS. Disparities in the surgical management of women with stage I breast cancer. Am Surg. 2009; 75:869-72.
- Boscoe FP, Johnson CJ, Henry KA, et al. Geographic proximity to treatment for early stage breast cancer and likelihood of mastectomy. Breast. 2011; 20:324-8.
- Chen R, You S, Yin Z, Zhu Q, Jiang C, Li S, Li Y, Zha X, Wang J. Non-doctoral factors influencing the surgical choice of Chinese patients with breast cancer who were eligible for breast-conserving surgery. World J Surg Oncol. 2019 Nov 11; 17(1):189.
- Schou I, Ekeberg O, Ruland CM, Karesen R. Do women newly diagnosed with breast cancer and consulting surgeon assess decision-making equally? Breast. 2002; 11:434-41.
- Caldon LJM, Collins KA, Wilde DJ, et al. Why do hospital mastectomy rates vary? Differences in the decision-making experiences of women with breast cancer. Br J Cancer. 2011; 104:1551-7.
- Lee CN, Chang Y, Adimorah N, et al. Decision making about surgery for early- stage breast cancer. J Am Coll Surg. 2012; 214:1-10.
- Osborn GD, Hodin M, Drew PJ, Fielder H, Vaughan-Williams E, Sweetland HM. Patient demographics and treatment for early breast cancer: an observational study. Breast. 2006; 15:377-81.
- Schiller DE, Le LW, Cho BCJ, Youngson BJ, McCready DR. Factors associated with negative margins of lumpectomy specimen: potential use in selecting patients for intraoperative radiotherapy. Ann Surg Oncol. 2008; 15:833-42.
- Chagpar AB, Martin RCG 2nd, Hagendoorn LJ, Chao C, McMasters KM. Lumpectomy margins are affected by tumor size and histologic subtype but not by biopsy technique. Am J Surg. 2004; 188:399-402.
- Mirza NQ, Vlastos G, Meric F, et al. Predictors of locoregional recurrence among patients with early-stage breast cancer treated with breast-conserving therapy. Ann Surg Oncol. 2002; 9:256-65.
- Cefaro GA, Genovesi D, Marchese R, et al. Predictors of local recurrence after conservative surgery and whole-breast irradiation. Breast Cancer Res Treat. 2006; 98:329-35.
- Fisher B, Redmond C, Poisson R, et al. Eight-year results of a randomized clinical trial comparing total mastectomy and lumpectomy with or without irradiation in the treatment of breast cancer. N Engl J Med. 1989; 320:822-8.





