Diagnosticul diferenţial al patologiilor selare şi paraselare – consideraţii anatomice și clinice
Differential diagnosis of sellar and parasellar pathologies – anatomic and clinical considerations
Abstract
The sellar and the parasellar regions can be affected by a wide variety of pathological processes, resulting in over 70 different entities. Although the most common are by far the pituitary adenomas, found in more than 80-90% of the cases, a differential diagnosis is mandatory before proceeding to treatment. The differential diagnosis can be sometimes difficult and in order to conduct it, a good understanding of the anatomy, of the possible pathologies involved and of the diagnostic significance of the clinical findings is essential. This article aims to review the anatomy of these regions and the pathologies encountered and will try to offer clues about the diagnostic significance of the clinical findings.Keywords
sellarparasellaranatomyclinicsdifferential diagnosisRezumat
Regiunea selară și cea paraselară pot fi afectate de o mare varietate de procese patologice, rezultând un număr de peste 70 de entități diferite. Deși cele mai frecvente sunt de departe adenoamele hipofizare, întâlnite în mai mult de 80-90% dintre cazuri, diagnosticul diferențial este obligatoriu înainte de a alege tratamentul. Diagnosticul diferențial poate fi uneori dificil, iar pentru a-l conduce este esențială o bună înțelegere a anatomiei, a posibilelor patologii implicate și a semnificației diagnostice a manifestărilor clinice. Acest articol își propune să treacă în revistă anatomia acestor regiuni și patologiile întâlnite și va încerca să ofere indicii despre semnificația diagnostică a manifestărilor clinice.Cuvinte Cheie
selarparaselaranatomieclinicădiagnostic diferențial
Introduction
Although the vast majority of the sellar and parasellar pathologies are represented by pituitary adenomas(1,2), the sellar and parasellar regions are complex areas that can be affected by a variety of lesions, ranging from benign and malignant tumors to developmental, vascular, inflammatory and infectious pathology(3,4). The preoperative etiological diagnosis of these pathologies isn’t always straightforward, because the clinical, biochemical and radiographic features of these lesions can mimic each other. However, some characteristics are specific or suggestive for certain lesions(2,5). A preoperative multidisciplinary assessment is necessary in order to orientate the diagnosis, to determine the right course of treatment and to improve the outcome(6).
Anatomy of the sellar and parasellar regions
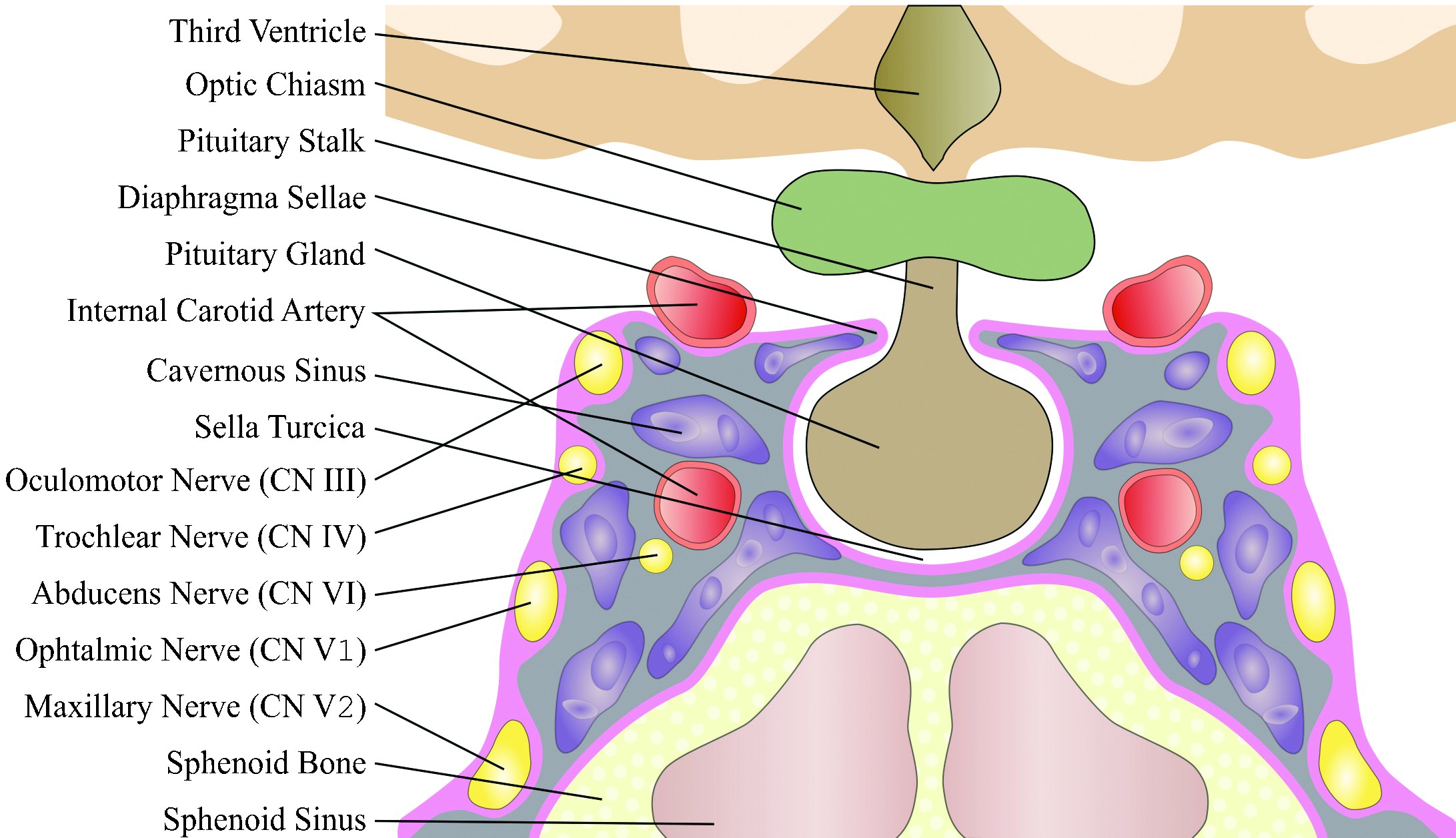
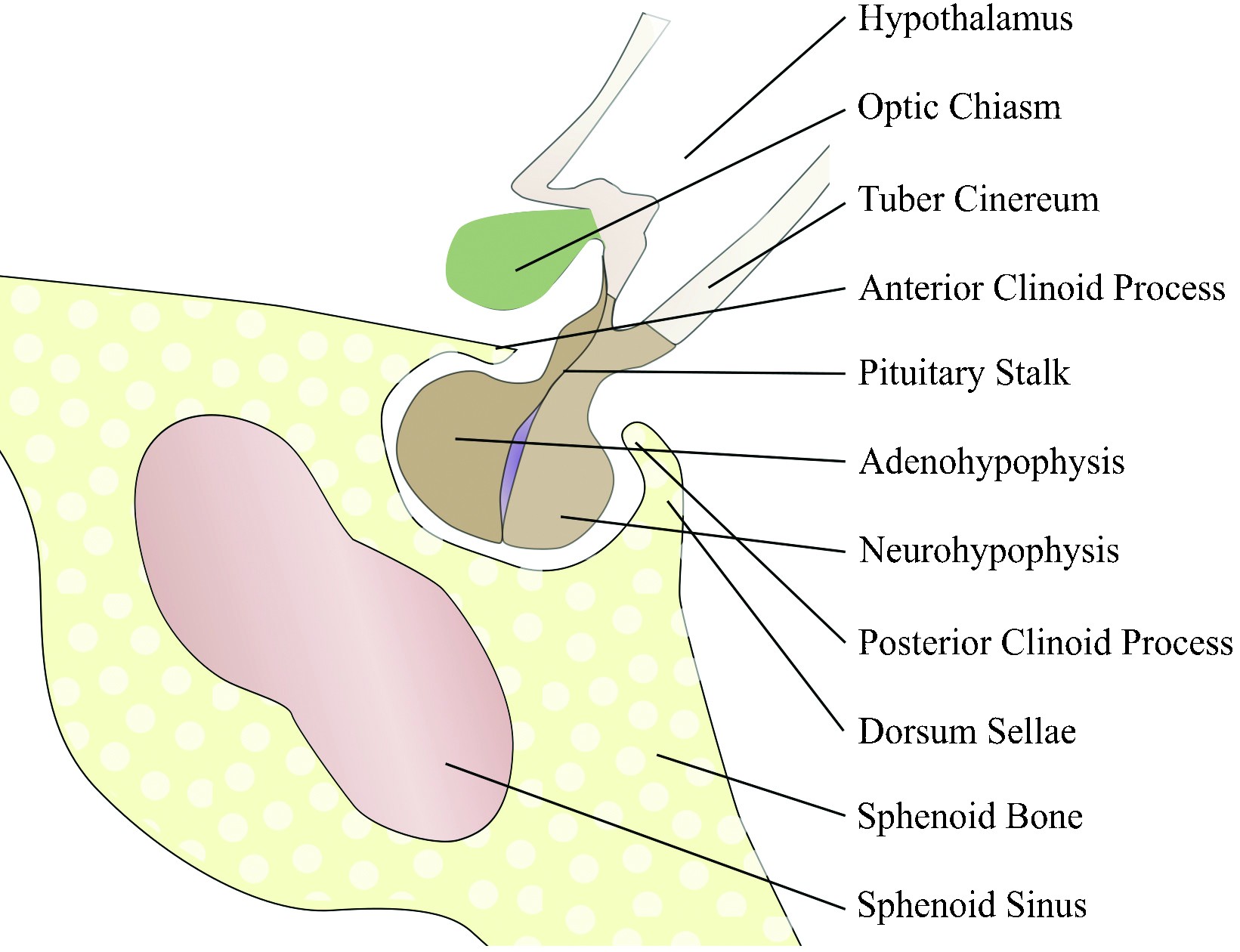
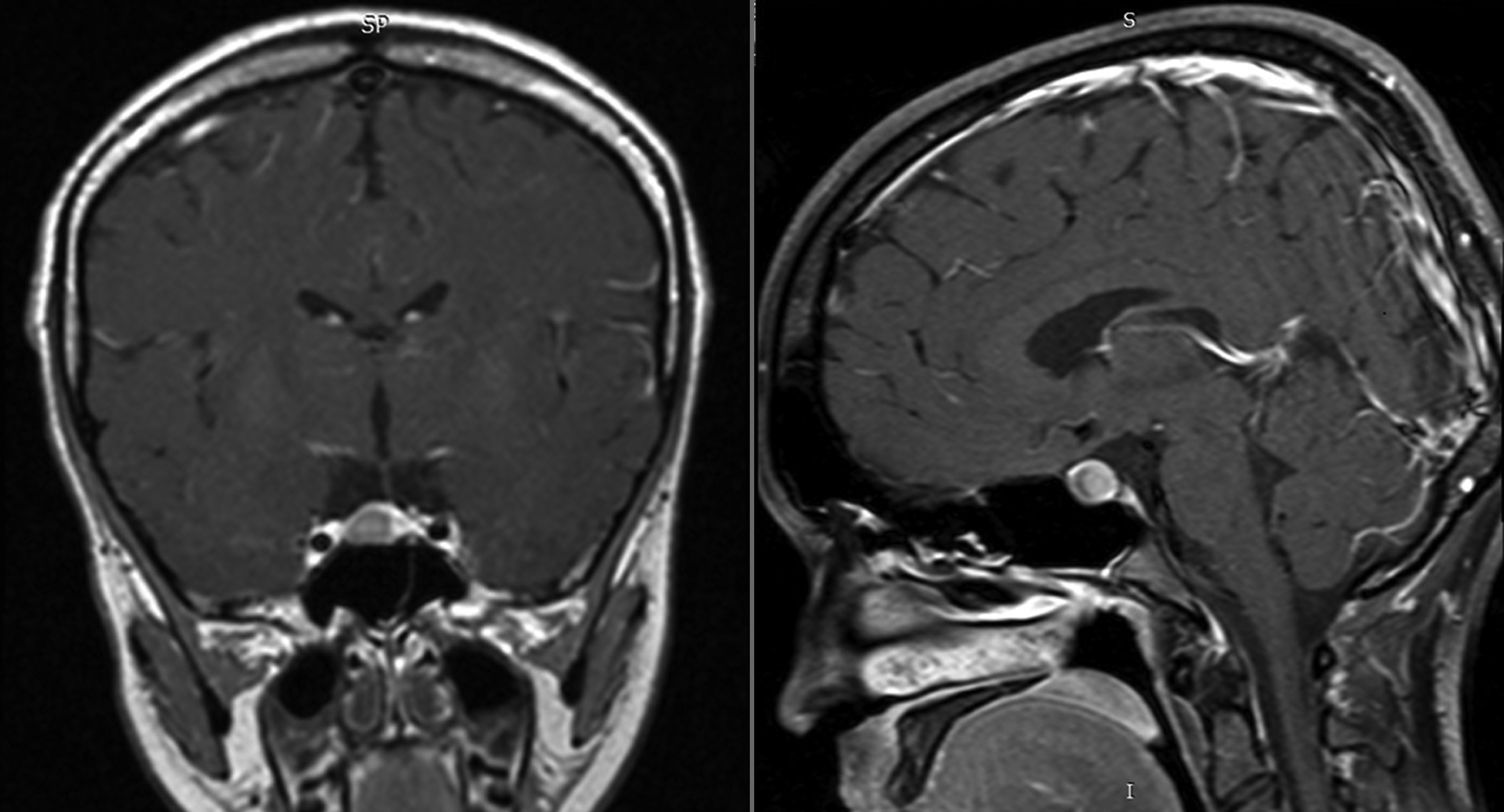
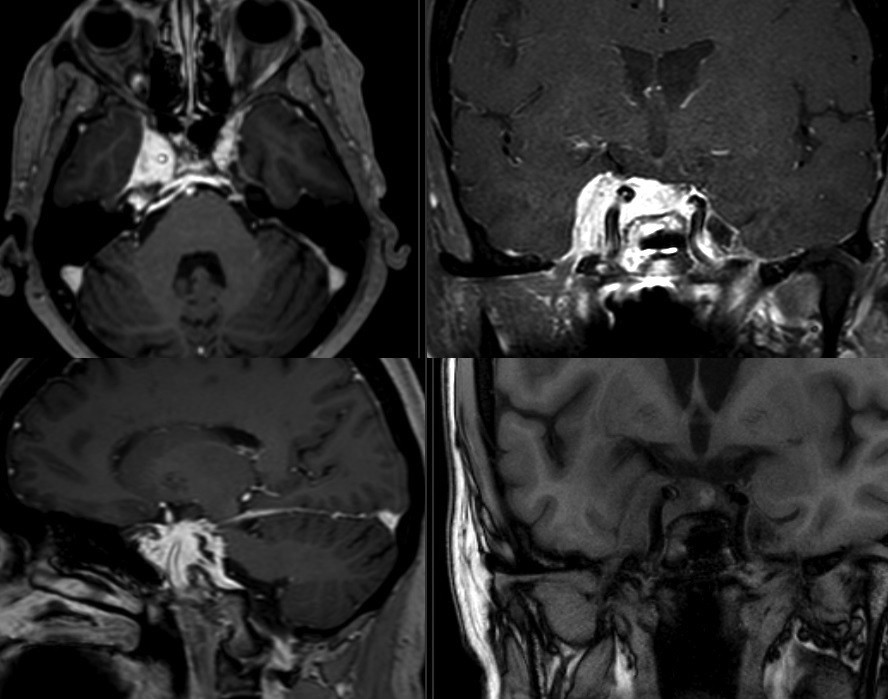
In order to understand the diverse pathology that can affect these areas and to conduct the differential diagnosis, it is essential to know the anatomy of these complex regions (Figure 1 and Figure 2) that contain numerous and important endocrine, neural and vascular structures found close one to another(7).
- The sella turcica, a bony depression of the sphenoid bone found on the midline, that has the following borders: the floor of the sella turcica (inferiorly), the diaphragma sellae (superiorly), the anterior clinoid processes and tuberculum sellae (anteriorly) and the posterior clinoid processes and dorsum sellae (posteriorly); the existence of a true lateral wall separating the sella turcica from the cavernous sinuses is controversial;
- The pituitary gland that lies within the sella, connected to the hypothalamus by the pituitary stalk and consisting of two different lobes: the adenohypophysis (that contains secretory cells which produce, under the control of the hypothalamus, growth hormone, adrenocortical-stimulating hormone, thyroid-stimulating hormone, prolactin, follicle-stimulating hormone and luteinizing hormone) and the neurohypophysis (that does not contain secretory cells, but only axons that stock and release the oxytocin and the vasopressin produced by the hypothalamus); the Rathke cleft resides between the adenohypophysis and the neurohypophysis(4,7-9).
- the sphenoid bone with the sphenoid sinuses;
- the cavernous sinuses that contain cranial nerves (III, IV, VI, V1 and V2) and the internal carotid artery;
- the suprasellar cistern (that contains the optic chiasm and nerves), the hypothalamus and the ventral inferior third ventricle(4,7,8).
Sellar and parasellar pathology
The diverse pathology affecting the sellar and the parasellar regions comprises tumoral, developmental, vascular, inflammatory and infectious pathology, resulting in more than 70 different entities that can involve the sellar and the parasellar regions (Table 1)(3,4,9-24). The most common are by far the pituitary adenomas, accounting for more than 80% to 90% of all the lesions found in these regions(1,2,11).Clinical findings
Although the sellar and parasellar pathologies often elicit similar symptoms and signs and besides the fact that an increasing numbers of patients present nowadays with incidentally discovered masses of this region, the clinical presentation including the signs and symptoms, the age at diagnosis, gender, the physiological and immunological status, the past and current medical history/treatments and the familial medical history are essential starting points in the differential diagnosis of these pathologies(3,4,25).
We divide here for didactic purposes the clinical findings in non-specific symptoms and signs, specific symptoms and signs and other clinical findings. This is not meant to be an all-inclusive list. Each case presents with its own unique constellation of findings that should be judged on an individual basis.
1. Non-specific symptoms and signs
The majority of the symptoms and signs are not specific for a certain lesion. They can be:
neurological (including headache, nausea, vomiting, dizziness, facial pain or facial numbness, cognitive complaints);
visual (including blurred vision, visual loss, diplopia, ptosis, visual field defects);
endocrine (including amenorrhea and galactorrhea caused by disconnection hyperprolactinemia, a wide range of symptoms caused by anterior pituitary deficiency, polyuria and polydipsia in diabetes insipidus);
general (including fatigue, fever and weakness(1,3,9,23).
Even though they are not specific, there are a number of studies that attempted to find if some of these symptoms and signs could be predictive for the type of lesion. Their finding are sometimes contradictory. For example, in a surgical series of 116 nonpituitary sellar lesions, Valassi et al. found that headache was the most common presenting symptom in both those with cysts (47%) and inflammatory lesions (20%), that diplopia/ptosis was the most common in those with malignancies (47%) and that blurred vision was the most common in those with benign tumors (28%)(1). Al-Aridi et al., in an analytical review that included 129 pathologically-confirmed sellar metastases, found that in more than 40% of the cases, the sellar metastasis was the first manifestation of cancer; the authors also found that diabetes insipidus was present in 59% of the cases of confirmed sellar metastasis and in none of the controls (the controls were represented by patients with nonfunctioning pituitary macroadenomas) and that abnormal eye motility was present in 84% of the cases of confirmed sellar metastasis, compared to 8% of the controls, and they concluded that diabetes insipidus and/or abnormal eye motility independently predict metastatic disease(26). In a series of 15 cases of lymphocytic hypophysitis, Heaney et al. found that 53% had diabetes insipidus(27), while Freda et al. found, in a series of 911 transsphenoidal surgical procedures, that the presence of diabetes insipidus strongly suggested that the sellar/parasellar mass was not of pituitary origin. Freda et al. also found that cranial neuropathy was more commonly encountered at presentation of nonpituitary sellar masses(2).
2. Specific symptoms and signs
Particularly important clinical differences can be found between hormonally inactive sellar/parasellar lesions and hormonally active pituitary adenomas, the last ones being usually accompanied by specific symptoms and signs caused by the hormonal hypersecretion:
Cushing’s syndrome in the case of adrenocorticotropic hormone hypersecretion;
gigantism/acromegaly in the case of growth hormone hypersecretion;
hyperthyroidism in the case of thyroid-stimulating hormone hypersecretion;
amenorrhea and galactorrhea or gynecomastia and hypogonadism (depending whether the affected subject is a woman or a man) in the case of prolactin hypersecretion;
ovarian hyperstimulation syndrome, testicular hyperstimulation syndrome or precocious puberty (depending on age and gender) in the case of active gonadotropin hormones hypersecretion (although most of the gonadotropin-secreting adenoma are particular and act as nonfunctioning adenomas)(3,8,9,28,29).
One important thing to bear in mind is that sometimes the symptoms and signs of hormonal hypersecretion can be subtle, so hormonal investigation in order to confirm or exclude a hormonally active pituitary adenoma should be performed(3,9).
Important clinical differences may also be found if the sellar/parasellar lesion is part of a systemic disease that elicits other symptoms and signs besides the ones produced by the sellar/parasellar lesion itself. Examples include:
granulomatous lesions of the sellar and parasellar regions: they can be part of systemic granulomatous diseases, whether the etiology is autoimmune (as for example in the case of granulomatosis with polyangiitis, known also as Wegener’s granulomatosis), infectious (as in the case of systemic mycosis or tuberculosis) or unknown (as in the case of sarcoidosis) or part of systemic histiocytosis (as in the case of Langerhans’ cell histiocytosis or of Erdheim-Chester disease)(13,22);
metastatic disease: the most frequently encountered metastases are from lung cancer in men and from breast cancer in women, although almost all types of malignancies can be involved; an important thing to bear in mind is that sometimes this metastasis can be the initial presentation of the malignancy(30-32);
other cases include lymphocytic hypophysitis if other autoimmune diseases are also present, amyloidosis and fibrous dysplasia(17,23).
3. Other clinical findings
Besides the symptoms and signs, there are other clinical findings that can help orientate the diagnosis:
age: the epidemiology of different lesions can vary greatly with age; for example, in children, craniopharyngioma is the most common sellar/parasellar tumor and not pituitary adenoma that is by far the most common entity encountered in adults, Langerhans’ cell histiocytosis is more frequent in children, meningioma is more common in middle age(3,22,25,33-35);
gender: some lesions have a gender preponderance (for example, metastases from lung cancer are found predominantly in men, metastases from breast cancer are found predominantly in women, lymphocytic hypophysitis is more frequent in women), while other lesions affect strictly one gender (for example, metastases from prostatic cancer are found exclusively in men)(3,22,26,31,32);
the physiological status: for example, during puberty, pregnancy and lactation, physiologic pituitary hyperplasia can occur(12,36);
the immunological status: immunocompromised patients are prone to certain infections and malignancies that can also affect the sellar and the parasellar regions(23,37);
the past and present medical history: for example, the existence of a systemic disease that can involve the sellar and the parasellar regions (systemic granulomatous diseases, neoplasms etc.), history of pituitary surgery/irradiation or sphenoid sinusitis that can predispose to pituitary abscess, primary hypothyroidism that can cause pituitary hyperplasia(12,13,19,22,26);
the medication: for example, the CTLA4-antibodies (ipilimumab and tremilimumab) used in the treatment of several cancers can produce hypophysitis(27).
Conclusion
The differential diagnosis of sellar and parasellar pathologies is sometimes difficult, but having a good understanding of the anatomy, of the variety of pathologies that can affect these regions and of the diagnostic significance of the clinical findings, is an essential first steps in orienting the diagnosis.
Bibliografie
- Valassi E, Biller BM, Klibanski A, Swearingen B. Clinical features of nonpituitary sellar lesions in a large surgical series. Clin Endocrinol (Oxf) 2010; 73:798-807.
- Freda PU, Wardlaw SL, Post KD. Unusual causes of sellar/parasellar masses in a large transsphenoidal surgical series. J Clin Endocrinol Metab 1996; 81:3455-9.
- Jagannathan J, Kanter AS, Sheehan JP, et al. Benign brain tumors: sellar/parasellar tumors. Neurol Clin 2007; 25:1231-49, xi.
- Chin BM, Orlandi RR, Wiggins III RH. Evaluation of the sellar and parasellar regions. Magn Reson Imaging Clin N Am 2012; 20:515-43.
- Shin JL, Asa SL, Woodhouse LJ, Smyth HS. Cystic Lesions of the Pituitary: Clinicopathological Features Distinguishing Craniopharyngioma, Rathke’s Cleft Cyst, and Arachnoid Cyst. J Clin Endocrinol Metab 1999; 84:3972-82.
- Moumen A, Meftah A, El Jadi H, et al. An unusual pituitary mass revealing a primary hypothyroidism! Clin Pract 2015; 5:733-5.
- Lucas JW, Zada G. Imaging of the Pituitary and Parasellar Region. Semin Neurol 2012; 32:320-31.
- Fenstermaker R, Abad A. Imaging of Pituitary and Parasellar Disorders. Continuum (Minneap Minn) 2016; 22:1574-94.
- Bresson D, Herman P, Polivka M, Froelich S. Sellar Lesions/Pathology. Otolaryngol Clin North Am 2016; 49:63-93.
- Chandrashekhara SH, Manjunatha YC, Muzumder S, et al. Multicentric sinus histicytosis (Rosai-Dorfman Disease): Computed tomography, magnetic resonance imaging findings. Indian J Med Paediatr Oncol 2011; 32:174-6.
- Al-Dahmani K, Mohammad S, Imran F, et al. Sellar Masses: An Epidemiological Study. Can J Neurol Sci 2016; 43:291-7.
- Glezer A, Paraiba DB, Bronstein MD. Rare sellar lesions. Endocrinol Metab Clin North Am 2008; 37:195-211.
- Basaria S, Ayala AR, Guerin C, Dobs AS. A rare pituitary lesion. J Endocrinol Invest 2000; 23:189-92.
- Hernandez-Estrada RA, Kshettry VR, Vogel AN, et al. Cholesterol granulomas presenting as sellar masses: a similar, but clinically distinct entity from craniopharyngioma and Rathke’s cleft cyst. Pituitary 2017; 20:325-32.
- Mendonca JL, Viana SL, Matsumine M, et al. Cavernous angioma of the cavernous sinus: imaging findings. Arq Neuropsiquiatr 2004; 62:1004-7.
- Doerfler A, Richter G. Lessions within and around the pituitary. Clin Neuroradiol 2008; 18:5-18.
- Kamel N, Ilgin SD, Gullu S, et al. Lymphocytic hypophysitis and infundibuloneurohypophysitis; clinical and pathological evaluations. Endocr J 1999; 46:505-12.
- Kumar J, Kumar A, Sharma R, Vashisht S. Magnetic Resonance Imaging of Sellar and Suprasellar Pathology: A Pictorial Review. Current Problems in Diagnostic Radiology 2007; 36:227-36.
- Connor SEJ, Penney CC. MRI in the Differential Diagnosis of a Sellar Mass. Clinical Radiology 2003; 58:20-31.
- Huang BY, Castillo M. Nonadenomatous tumors of the pituitary and sella turcica. Top Magn Reson Imaging 2005; 16:289-99.
- Orija IB, Weil RJ, Hamrahian AH. Pituitary incidentaloma. Best Pract Res Clin Endocrinol Metab 2012; 26:47-68.
- Carpinteri R, Patelli I, Casanueva FF, Giustina A. Pituitary tumours: inflammatory and granulomatous expansive lesions of the pituitary. Best Pract Res Clin Endocrinol Metab 2009; 23:639-50.
- Famini P, Maya MM, Melmed S. Pituitary magnetic resonance imaging for sellar and parasellar masses: ten-year experience in 2598 patients. J Clin Endocrinol Metab 2011; 96:1633-41.
- Batista RL, Ramos LS, Cescato VA, et al. Thickened Pituitary Stalk Associated with a Mass in the Sphenoidal Sinus: An Alarm to Suspect Hypophysitis by Immunoglobulin G4? Int Arch Otorhinolaryngol 2015; 19:273-6.
- Chumak J, Zarka A. Enhancing Sellar/Suprasellar Mass in an Adolescent. J Am Osteopath Coll Radiol 2013; 2:27-9.
- Al-Aridi R, El Sibai K, Fu P, et al. Clinical and biochemical characteristic features of metastatic cancer to the sella turcica: an analytical review. Pituitary 2014; 17:575-87.
- Heaney AP, Sumerel B, Rajalingam R, et al. HLA Markers DQ8 and DR53 Are Associated With Lymphocytic Hypophysitis and May Aid in Differential Diagnosis. J Clin Endocrinol Metab 2015; 100:4092-7.
- Cooper O, Geller J, Melmed S. Ovarian hyperstimulation syndrome caused by an FSH-secreting pituitary adenoma. Nat Clin Pract Endocrinol Metab 2008; 4:234-8.
- Thakkar A, Kannan S, Hamrahian A, et al. Testicular “Hyperstimulation” Syndrome: A Case of Functional Gonadotropinoma. Case Reports in Endocrinology 2014; Volume 2014, Article ID 194716.
- Shah N, Cavanagh Y, Shaaban H, et al. An unusual initial presentation of hepatocellular carcinoma as a sellar mass. J Nat Sci Biol Med 2015; 6:471-4.
- Abele TA, Yetkin ZF, Raisanen JM, et al. Non-pituitary origin sellar tumours mimicking pituitary macroadenomas. Clin Radiol 2012; 67:821-7.
- Gopan T, Toms SA, Prayson RA, et al. Symptomatic pituitary metastases from renal cell carcinoma. Pituitary 2007; 10:251-9.
- Warmuth-Metz M, Gnekow A, Müller H, Solymosi L. Differential diagnosis of suprasellar tumors in children. Klin Padiatr 2004; 216:323-30.
- Deopujari CE, Kumar A, Karmarkar VS, et al. Pediatric suprasellar lesions. J Pediatr Neurosci 2011; 6 (Suppl1):46-55.
- Rao VJ, James RA, Mitra D. Imaging characteristics of common suprasellar lesions with emphasis on MRI findings. Clinical Radiology 2008; 63:939-47.
- 3Horvath E, Kovacs K, Scheithauer B. Pituitary hyperplasia. Pituitary 1999; 1:169-79.
- Penn I. Tumors of the Immunocompromised Patient. Ann Rev Med 1988; 39:63-73.


