Excizia unui papilom scuamos de vestibul nazal cu electrochirurgie de înaltă frecvenţă
Excision of squamous papilloma of the nasal vestibule with high-frequency electrosurgery
Abstract
Benign nasal tumors represent an uncommon pathology with various histopathological types. Squamous papilloma of the nasal vestibule, also called verruca vulgaris, is a benign epithelial tumor, sessile or pedunculated, small in size, unique or comprising multiple lesions, which can present with intermittent epistaxis or nasal obstruction. We chose to explore a case of squamous papilloma of nasal vestibule excision using high-frequency electrosurgery. A 38-year-old woman presented with one-month history of intermittent right nasal bleeding. The anterior rhinoscopy and the endoscopic examination revealed an 1x0.5 cm sized, unique, sessile and irregular shaped mass in the right nasal vestibule. An excisional biopsy was performed under local anesthesia, using high-frequency electrosurgery. The follow-up period consisted of two years, without any recurrence.Keywords
benign tumornasal vestibulepapillomaepistaxishigh-frequency electrosurgeryRezumat
Tumorile nazale benigne reprezintă o patologie neobişnuită, cu diferite tipuri histologice. Papilomul scuamos al vestibului nazal, denumit şi verruca vulgaris, este o tumoră epitelială benignă, sesilă sau pedunculată, de dimensiuni reduse, unică sau care cuprinde leziuni multiple, care se poate prezenta cu epistaxis intermitent sau obstrucţie nazală. Am ales să explorăm un caz de excizie de papilom scuamos de vestibul nazal folosind electrochirurgie de înaltă frecvenţă. O femeie de 38 de ani s-a prezentat cu o simptomatologie de sângerare nazală dreaptă intermitentă de o lună. Rinoscopia anterioară şi examinarea endoscopică au evidenţiat o masă unică, sesilă, de 1x0,5 cm şi de formă neregulată în vestibulul nazal drept. S-a efectuat o biopsie excizională sub anestezie locală, folosind electrochirurgie de înaltă frecvenţă. Perioada de urmărire a constat în doi ani, fără nicio recidivă.Cuvinte Cheie
tumoră benignăvestibul nazalpapilomepistaxiselectrochirurgie de înaltă frecvenţăIntroduction
Benign nasal tumors represent an uncommon pathology with various histopathological types. Papillomas of the nasal cavities include three forms: exophytic, inverted and oncocytic papilloma. The risk of recurrence and the potential for malignancy make the papilloma a dangerous benign nasal tumor.
Squamous papilloma of nasal vestibule, also called verruca vulgaris, is different from inverted papilloma. Papilloma in the nasal vestibule is a benign epithelial tumor, sessile or pedunculated, small in size, unique or comprising multiple lesions, which can present with intermittent epistaxis or nasal obstruction. On the other side, inverted papilloma arises from the lateral nasal wall, from the Schneiderian membrane(1).
Cytogenetically, squamous papilloma of the nasal vestibule may be positive for low-risk HPV (type 6 and 11), which rarely develop into cancer(2,3).
High-frequency or radio-frequency electrosurgery comprises of four different settings: electrosection, electrofulguration, electrodesiccation and electrocoagulation. These involve high-frequency alternating current, which is converted to heat by resistance as it passes through the tissue(4).
The applications for electrosurgery are multiple within the ENT field: hemostasis, rhinophyma excision and some of benign tumors, as well as turbinate reduction.
Case presentation
A 38-year-old woman presented with one-month history of intermittent right nasal bleeding. There was no history of injury or infection and no significant past history of bleeding disorder.
The anterior rhinoscopy and the endoscopic examination revealed an 1x0.5 cm sized, unique, sessile and irregular shaped mass in the right nasal vestibule (Figure 1).
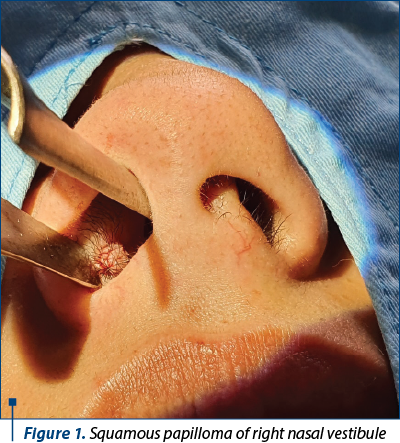
The clinical and endoscopic appearance raised the suspicion of papilloma of the nasal vestibule, without the need for imaging exploration of the nasal cavity.
The surgical treatment comprises both the excision and the electrocauterization of the tumoral base to prevent recurrence.
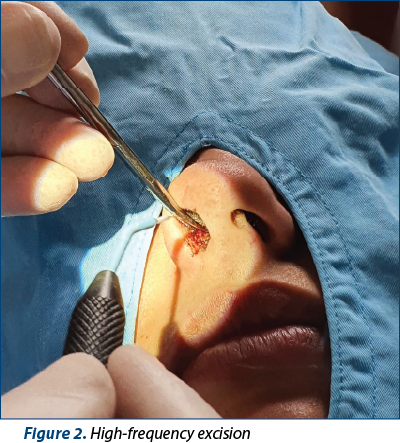
An excisional biopsy was performed under local anesthesia. The tumor was removed by an elliptical incision, with the safety edges going up to normal tissue, using high-frequency electrosurgery.
The preserved specimen for histopathological examination showed exophytic proliferations, well differentiated stratified squamous epithelium, with delicate fibrovascular core, establishing the diagnosis of squamous papilloma.

The follow-up period consisted of two years, without any recurrence.
Discussion
In this case, we used the electrodesiccation mode of high-frequency electrosurgery, where the electrode is in contact with the skin, resulting in superficial dehydration due to ohmic heating. Electrodesiccation uses markedly damped, low-amperage, high-voltage current with a single terminal to produce local tissue destruction(4).
Fortunately, the lesion did not reappear, but in many cases this happens. “Recurrence” represents residual tumor in most cases.
In such cases, the surgical excision can be performed once more, or the surgeon can try another technique, such as cryotherapy or laser CO2 vaporization(5).
In the current case, the patient presented a unique lesion, but if there had been multiple lesions, the surgical excision would also have been more difficult.
For benign tumors with malignant potential risk, complete surgical excision is mandatory.
In this case, the patient did not want to pursue a molecular analysis of the biopsy.
At the moment, there are three vaccines that protect against HPV: Ceravix®, Gardasil® and Gardasil 9® – all protecting against high-risk types of HPV (16,18). For low-risk type HPV, both Gardasil® and Gardasil 9® are effective. Vaccines are available for girls and boys from 9 up to 26 years old(6-8).
Conclusions
Even though the surgical treatment is curative, the risk of recurrence is high. The “recurrence” is, in fact, the tumor residue in most of the cases, and can be avoided if the surgeon chooses the appropriate technique for the injury he is facing. The use of high-frequency electrosurgery adds accuracy in addition to being minimally invasive. n
Conflicts of interests: The authors declare no conflict of interests.
Bibliografie
-
Vorasubin N, Vira D, Suh JD, Bhuta S, Wang MB. Schneiderian papillomas: Comparative review of exophytic, oncocytic, and inverted types. Am J Rhinol Allergy. 2013;27:287–292.
-
Bishop J. OSPs and ESPs and ISPs, Oh My! An Update on Sinonasal (Schneiderian) Papillomas. Head and Neck Pathol. 2017;11(3):269-77.
-
Weindorf S, Brown N, McHugh J, Udager A. Sinonasal Papillomas and Carcinomas: A Contemporary Update with Review of an Emerging Molecular Classification. Archives of Pathology & Laboratory Medicine. 2019;143(11):1304-16.
-
Soon SL, Washington Jr CV. Electrosurgery, Electrocoagulation, Electrofulguration, Electrodessication, Electrosection, Electrocautery. Robinson JK, Hanke CW, Siegel DM, Fratila A, eds. Surgery of the Skin; Procedural Dermatology. 2nd ed, St. Louis, Mo: Mosby Elsevier; 2010. 9/137-152.
-
Sterling JC, Handfield-Jones S, Hudson PM. Guidelines for the management of cutaneous warts. Br J Dermatol. 2001;144:4–11.
-
Cheng L, Wang Y, Du J. Human Papillomavirus Vaccines: An Updated Review. Vaccines (Basel). 2020;8(3):391. Published 2020 Jul 16. doi:10.3390/vaccines8030391.
-
Einstein MH, Takacs P, Chatterjee A, Sperling RS, Chakhtoura N, Blatter MM, Lalezari J, David MP, Lin L, Struyf F, et al. Comparison of long-term immunogenicity and safety of human papillomavirus (HPV)-16/18 AS04-adjuvanted vaccine and HPV-6/11/16/18 vaccine in healthy women aged 18-45 years: End-of-study analysis of a Phase III randomized trial. Hum Vaccines Immunother. 2014;10:3435–3445.
-
Chaturvedi AK, Graubard BI, Broutian T, Pickard RKL, Tong ZY, Xiao W, Kahle L, Gillison ML. Effect of Prophylactic Human Papillomavirus (HPV) Vaccination on Oral HPV Infections Among Young Adults in the United States. J Clin Oncol. 2018 Jan 20;36(3):262-267.




