Din aceeași categorie
Introduction
Omphalocele, also called exomphalos, is a congenital malformation due to a defect in the closure of the anterior abdominal wall. The characteristic ultrasound appearance includes a midline defect with herniation of abdominal contents into the base of the umbilical cord. The incidence of omphalocele is 1 to 2 per 10,000 live births(1-3). However, the true incidence and morbidity and mortality may be higher when elective abortions or fetal demise are taken into account(3). In more than 50% of the cases, the malformation is linked to various pathologies, and it can be a warning sign for genetic disorders(4,5).
The use of prenatal ultrasound to diagnose omphalocele was first reported in 1978(4). Gastroschisis is the main differential diagnosis of omphalocele. In gastroschisis, the intestinal protrusion is usually to the right of the midline, and there is no involvement of the umbilical cord. Also, gastroschisis is characterized by free-floating bowel loops(4-6).
Omphalocele is frequently associated with congenital anomalies and syndromes such as Beckwith-Wiedemann syndrome and trisomies 13, 18 and 21(6). Also, the long-term prognosis for infants with gastroschisis is considerably better than that for infants with omphalocele, in whom a 50% to 60% survival rate and frequently chronic medical problems are noticed(5,6).
The prognosis depends on the size of the defect and the associated birth defects. As such, large omphalocele with associated abnormalities have a higher mortality rate. Also, neonates with liver protrusion through the defect appear to have a poorer prognosis(7-9).
Case report
We report the case of a 30-year-old primigravida presented for a routine nuchal ultrasound examination. Ultrasonography revealed a single live intrauterine fetus of 12 weeks. This was her second ongoing pregnancy following in vitro fertilization (IVF) conception. She had a vaginal delivery at term with a healthy baby (3441 g). Her chance for aneuploidies in this pregnancy was deemed to be high for trisomy 18 (T21: 1/2000; T13 1:550; T18: 1/50), with a nuchal translucency measurement of 2.9 mm.
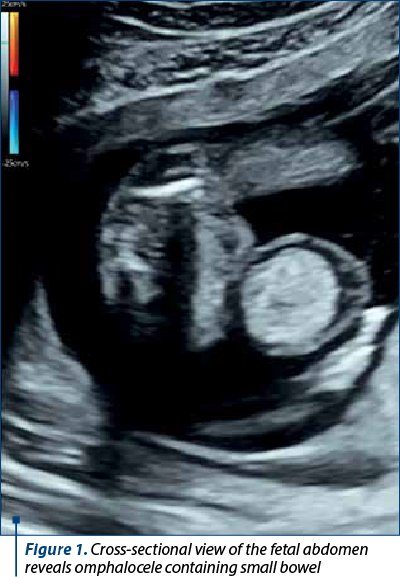
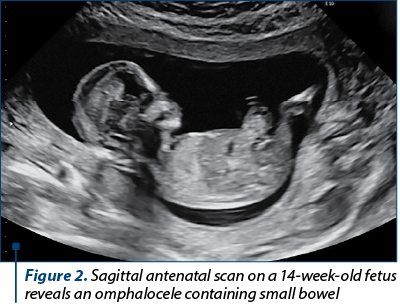
There was a defect in the abdominal wall at the umbilical cord insertion through which there was herniation of the small bowel, measuring 12.6 mm. These findings were consistent with a diagnosis of exomphalos. There were no other major defects, and the other ultrasound markers of chromosomal abnormalities appeared normal. The gravida underwent chorionic villus sampling at 12 weeks of gestation. Genetic chorionic villus sampling analysis revealed the existence of trisomy 18 mosaicism. After discussion, the couple decided to end the pregnancy. Pregnancy termination was performed at 14 weeks.
Discussion
Between January 2, 1982 and December 31, 1999, Hwang et al. examined 127 cases of omphalocele and 121 cases of gastroschisis. Ninety-three of the 127 probands with omphalocele had karyotype determinations, and 20% were abnormal; for gastroschisis, 37 had cytogenetic studies, and none had chromosomal anomalies. Seventy-six percent of the probands with omphalocele had associated abnormalities; twenty-three percent of the probands with gastroschisis, none of which were syndromic, had associated anomalies. The prematurity rate for omphalocele was 42%, and the mortality rate was 22%(10).
Chromosomal aberrations are involved in 38% to 67% of the omphaloceles, mainly aneuploidies. The most frequent chromosomal aberrations associated with omphalocele are trisomy 18 which ranks the first place (22% to 89% of fetuses having omphalocele) and trisomy 13(11).
The possible association of Down syndrome (DS) with omphalocele is controversial. The majority of epidemiological studies showed no association of Down syndrome with omphalocele. In surgical series, the occasional infant with both defects (gastroschisis and omphalocele) was more likely to undergo surgery than infants with omphalocele and trisomy 13 or 18, or other severe birth defects(12).
Between January 1985 and January 2004, Brantberg et al. followed ninety fetuses with omphalocele from the time of prenatal diagnosis. Abnormal karyotype was found in 40/58 (69%) of the central and in 4/32 (12.5%) of the epigastric omphaloceles. Trisomy 18 was the most frequent abnormality associated with omphalocele(9,11,13,14).
The associated congenital anomalies, the ruptured sac and the size of omphalocele determine the prognosis of the newborn. Improvements in prenatal genetic screening and diagnostic techniques will decrease the gestational ages in terminations of pregnancies(9-11).
Conclusions
The prenatal diagnosis of omphalocele remains significant. The majority of fetuses with omphalocele have other congenital abnormalities and, in many cases, an abnormal karyotype. Early detection of chromosomal anomalies remains essential, as this has a direct correlation to the prenatal and postnatal prognosis.

