Este dexametazona o idee bună atunci când vorbim despre naşterea prin operaţie cezariană?
Is dexamethasone a good idea when we talk about caesarean delivery?
Abstract
Respiratory distress syndrome is one of the most frequently researched and always of immediate interest topics, representing one of the main causes of morbidity and mortality in the neonatal population. Therefore, the antenatal administration of corticosteroids in preterm births (between the 24th week and the 34th week of gestational age) is one of the most important antenatal therapies available, with a positive influence on the long-term neonatal prognosis. The effects on both the interstitium and other organs reduce the risk of respiratory distress syndrome, necrotizing enterocolitis and intracranial hemorrhage. Scientific data about corticosteroid use in women at risk for preterm birth under 34 weeks of gestation and the benefits on the newborn adaptation to the extrauterine life, especially when it comes to caesarean delivery, are abundant. Of course, the benefit of corticoprophylaxis versus the possible long-term results on neurodevelopment, especially in school age, in this category of newborns should be considered. Among early-terms and full-term newborns, delivered by caesarean section, the pathophysiology of respiratory distress is closely related to the absorption of alveolar fluid and to the concentration of catecholamines in the fetal blood, and if there is no labor, these latter ones are affected. In this article, we present the observations obtained in a study conducted on 81 newborns from pregnancies with ages between 36 0/7 and 37 0/7 weeks, who received dexamethasone less than seven days before birth, conducted within the Obstetrics-Gynecology and Neonatology Clinic of the “Elias” University Emergency Hospital, Bucharest. We compared the results with data published in the field research, having as purpose to elucidate the controversies of antenatal corticosteroid therapy for various populations and, possibly, to establish individualized therapies.Keywords
antenatal corticosteroidsrespiratory distresselective caesarean sectionfollow-upneurological developmentNa+ epithelial channelsRezumat
Sindromul de detresă respiratorie reprezintă unul dintre subiectele frecvent cercetate şi mereu de actualitate, reprezentând una din principalele cauze de morbiditate şi mortalitate la populaţia neonatală. Prin urmare, administrarea corticosteroizilor înainte de naşterea prematură (între 24 şi 34 de săptămâni vârstă gestaţională) este una din cele mai importante terapii antenatale disponibile, cu o influenţă pozitivă asupra prognosticului neonatal pe termen lung. Efectele, atât asupra interstiţiului pulmonar, cât şi asupra altor organe, scad riscul de apariţie a sindromului de detresă respiratorie, a enterocolitei ulceronecrotice şi a hemoragiei intracraniene. Tot mai mult, se publică date ştiinţifice cu privire la corticoprofilaxia la gravidele cu vârsta gestaţională de peste 34 de săptămâni şi la efectele asupra adaptării nou-născutului la viaţă extrauterină, mai ales atunci când vorbim despre naşterea prin operaţie cezariană. Sigur că trebuie cântărit beneficiul corticoprofilaxiei versus posibilele rezultate pe termen lung asupra neurodezvoltării, mai ales la vârsta şcolară, la această categorie de nou-născuţi. În rândul nou-născuţilor prematuri şi la termen, extraşi prin operaţie cezariană, fiziopatologia detresei respiratorii este strâns legată de absorbţia lichidului alveolar şi de concentraţia de catecolamine din sângele fetal, acestea fiind afectate în lipsa travaliului. În acest articol, prezentăm observaţiile obţinute în cadrul unui studiu realizat la 81 de nou-născuţi proveniţi din sarcini cu vârsta gestaţională între 36 0/7 şi 37 0/7 săptămâni, care au primit dexametazonă cu mai puţin de şapte zile înainte de naştere, studiul fiind desfăşurat în cadrul Clinicii de obstetrică-ginecologie şi neonatologie a Spitalului Universitar de Urgenţă „Elias” Bucureşti. Rezultatele au fost comparate cu rezultatele publicate în literatura de specialitate, din dorinţa de a elucida controversele privind terapia antenatală corticosteroidiană pentru diversele populaţii şi, eventual, pentru stabilirea unor terapii individualizate.Cuvinte Cheie
corticosteroizi antenatalidetresă respiratorieoperaţie cezariană electivăfollow-updezvoltare neurologicăcanale epiteliale de Na+Introduction
For almost three decades, the administration of corticosteroids before preterm birth has been one of the most important antenatal therapies available, with a positive influence on the prognosis and neonatal mortality. A single course of corticosteroids is recommended for pregnant women between 24 0/7 weeks and 33 6/7 weeks of gestation who are at risk of preterm birth within seven days. Also, the administration of corticosteroids after 34 weeks of gestation can be considered on pregnant women who are at risk of premature birth within seven days. Long-term follow-up after uterine exposure to corticosteroids is recommended, as there are studies in the field research that support the hypothesis which says that there may be changes in neurological development in this category of newborns, most often reporting delayed school-age acquisitions(1,2).
When discussing the administration of corticosteroids to women with more than 34 weeks of pregnancy, in order to prevent the occurrence of lung complications, we must consider the unforeseen events, such as neonatal hypoglycemia and unknown disorders related to long-term neurological development and metabolic risks(3,4).
Compared to the newborns from physiological birth, the newborns from caesarean section have a higher risk of developing immediately after birth neonatal respiratory distress, neonatal transient tachypnea and the need of admission in the neonatal intensive care unit and, at the same time, with longer high costs for patient care. This risk is even higher in the case of scheduled caesarean operations in the absence of labor. Studies have shown the usefulness of administering antenatal corticosteroids to pregnant women with more than 34 weeks of gestational age, with beneficial effects, especially pulmonary, and not only, such as reducing the risk of necrotizing enterocolitis and intracranial hemorrhage amongst newborns(5-7).
The pathophysiology of respiratory distress syndrome in full-term newborns is different from that of preterms. Thus, the onset of symptoms is caused by the deficiency of fluid resorption at the alveolar level. Among the well-known effects of antenatal administered glucocorticoids, the maturation of the pulmonary interstitium, it should be considered the potential resorption of alveolar fluid in the interstitial space that can occur immediately after birth. Research data describe several cellular components involved in the process of alveolar resorption, including the Na+ channels in the lung epithelium, the Na+/K+-pump-ATPase and AQP5 (aquaporin 5)(8,9).
Elevated concentrations of glucocorticoids and catecholamines in the umbilical cord have been linked to an increase in the expression of Na+ channels in the lung epithelium by mRNA-like mechanisms, which facilitates the drainage of alveolar fluid. During physiological birth, the serum level of catecholamines and corticosteroids is increased due to birth stress. In newborns delivered by caesarean section, there are hormonal changes that have been linked to favorable neonatal pulmonary adaptation, which are prone to respiratory complications shortly after birth(8,9).
The administration of corticosteroids at gestational ages between 34 0/7 weeks and 36 0/7 weeks is increasingly encouraged, due to the risk of developing respiratory distress syndrome or transient neonatal tachypnea in this age group. Taking into account the observations made, the beneficial effect can be considered by administering antenatal corticosteroids in the case of pregnancies with a gestational age higher than 36 weeks, especially when the increased possibility of caesarean delivery is expected in the absence of labor, having as purpose to obtain a similar effect to the physiological hormonal changes induced by vaginal birth(10-12).
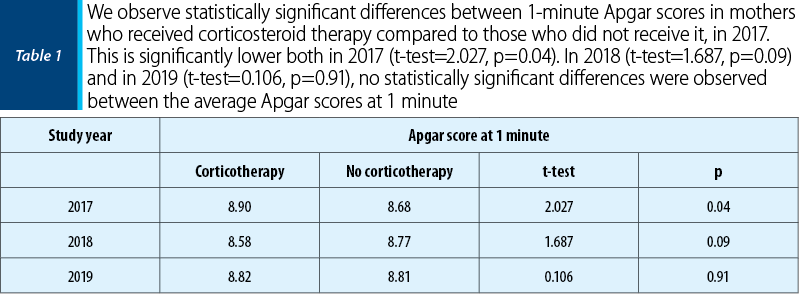
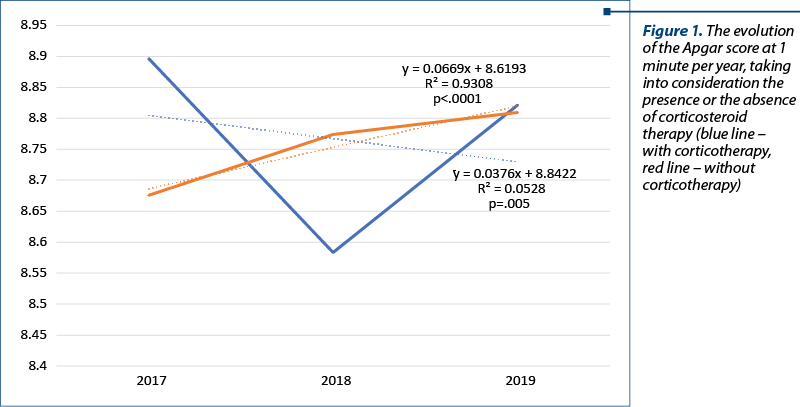
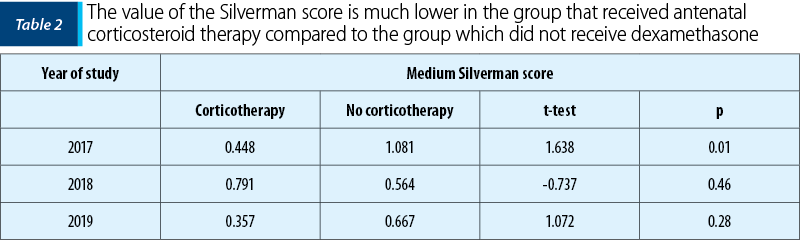
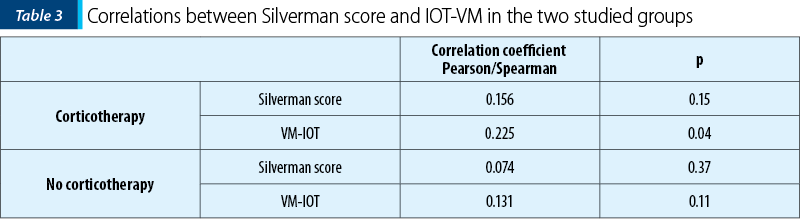
In our study, we analyzed 81 newborns obtained from pregnancies between the ages of 36 0/7 and 37 0/7 weeks, who received 8 mg of dexamethasone at 12 hours, for two days, within less than seven days before birth. This study was conducted in the Clinic of Obstetrics-Gynecology and Neonatology of the “Elias” University Emergency Hospital, Bucharest. The main observation was that there was a significantly higher value of the Apgar score in the group that received dexamethasone, compared to the group that did not receive corticosteroid prophylaxis (Table 1, Figure 1). There was also a significant reduction in the need for mechanical monitoring, surfactant use and a shortening of the number of days spent in neonatal intensive care units (Table 2 and Table 3).
However, there are concerns about the administration of both betamethasone and dexamethasone, due to potential adverse effects on neurological development, which most often correlate with delays in school acquisition. However, most data come from animal studies or from pregnancies in which more than two treatments have been administered. A follow-up of a study performed at gestational age (over 37 0/7 weeks of gestation) showed subjective differences in the assessment of children’s learning abilities, but the same study showed that there was no objective difference in neurocognitive development. In our study, no adverse effects on neurological development were found in newborns in the group receiving dexamethasone who had psychomotor and cognitive development corresponding to their age(12,13).
Further opinions/discussion
The present study aims to provide information in addition to those already existing in the literature, and the results obtained timidly support the effectiveness of corticosteroid therapy in pregnant women in the term or near term; however, more evidence is needed to standardize this treatment. The information obtained in our study is similar to the information already presented in other articles discussing this topic.
We need to consider the beneficial effects of antenatal glucocorticoids with unanticipated effects such as neonatal hypoglycemia and the risks factors related to the long-term follow-up of neurological development and metabolic risks.
Of great interest is the elucidation of the pathophysiological mechanism, which involves many cellular components with an important role in the transport of water and transmembrane electrolytes, such as the Na+ channel in the lungs, the Na+/K+-pump-ATPase and aquaporins. There are scientific data which conclude that the presence of high serum concentrations of catecholamines and glucocorticoids in the newborn, during birth, increases the membrane expression of Na+ and AQP5 channels and stimulates the activity of the Na+/K+-pump-ATPase.
Conclusions
The administration of corticosteroids before the premature birth (between the 24th week and the 34th week of gestational age) is the gold standard in available antenatal therapies, with a proven beneficial influence on the short-term and long-term neonatal prognosis. The effects on both the pulmonary interstitium and other organs reduce the risk of respiratory distress syndrome, ulcerative necrotic enterocolitis and intracranial hemorrhage.
When taking into consideration the administration of antenatal glucocorticoids at gestational ages between 34 0/7 weeks and 36 0/7 weeks, we must take into account the risk of developing respiratory distress syndrome or neonatal transient tachypnea in this age group. Based on the observations made, the use of antenatal corticosteroids in near-term pregnant women is considered beneficial, with the purpose of obtaining an effect similar to the physiological hormonal changes induced by vaginal birth.
The administration of corticosteroids at gestational ages between 34 0/7 weeks and 36 0/7 weeks is increasingly encouraged due to the risk of developing respiratory distress syndrome or transient neonatal tachypnea in this age group. There was a significant reduction in the need for mechanical ventilation, surfactant use and a shortening of the number of days spent in neonatal intensive care units. A decrease in the frequency of pneumothorax in this age group was also observed. There are concerns about the administration of both betamethasone and dexamethasone due to potential adverse effects on neurological development, but these latter risks are not completely confirmed by the studies performed until the present days.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Lee MJ, Guinn D. Antenatal corticosteroid therapy for reduction of neonatal respiratory morbidity and mortality from preterm delivery. UpToDate, Nov 2021.
- McGoldrick E, Stewart F, Parker R, Dalziel SR. Antenatal corticosteroides for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst Rev. 2020;12(12):CD004454.
- Saccone G, Berghella V. Antenatal corticosteroides for maturity of term or near term fetuses: systematic review and meta-analysis of randomized controlled trials. BMJ. 2016;355:i5044.
- Berghella V, Lockwood CJ, Barss VA. Cesarean birth: preoperative planning and patient preparation. UpToDate. Oct 29, 2021.
- Jobe AH, Goldenberg RL. Antenatal corticosteroids: an assessment of anticipated benefits and potential risks. Am J Obstet Gynecol. 2018;219(1):62-74.
- Kamath-Rayne BD, Rozance PJ, Goldenberg RL, Jobe AH. Antenatal corticosteroids beyond 34 weeks gestation: What do we do now? Am J Obstet Gynecol. 2016;215(4):423-30.
- Magann EF, Haram K, Ounpraseuth S, Mortensen JH, Spencer HJ, Morrison JC. Use of antenatal corticosteroids in special circumstances: a comprehensive review. Acta Obstet Gynecol Scand. 2017;96(4):395–409.
- Smith DE, Otulakowski G, Yeger H, Post M, Cutz E, O’Brodovich HM. Epithelial Na+ channel (ENaC) expression in the developing normal and abnormal human perinatal lung. Am J Respir Crit Care Med. 2000;161(4 Pt 1):1322-31.
- Suvari L, Janer C, Helve O, Kaskinen A, Turpeinen U, Pitkanen-Argillander O, Andresson S. Postnatal gene expression of airway epithelial sodium transporters associeted with birth stress in humans. Pediatr Pulmonol. 2019;54(6):797-803.
- Norman J, Shennan A, Jacobsson B, Stock SJ. FIGO good practice recommendations on the use of prenatal corticosteroides to improve outcomes and minimize harm in babies born preterm. Int J Gynecol Obstet. 2021;155(1):26-30.
- Schmand B, Neuvel J, Smolders-de Hass H, Hoeks J, Treffers PE, Koppe JG. Psychological development of children who were treated antenatally with corticosteroides to prevent respiratory distrees syndrome. Pediatrics. 1990;86(1):58-64.
- Shanks AL, Grasch JL, Quinney SK, Haas DM. Controversies in antenatal corticosteroides. Semin Fetal Neonatal Med. 2019;24(3):182-8.
- Liggins Institute. Antenatal Corticosteroid Clinical Practice Guidelines Panel. Antenatal corticosteroids given to women prior to birth to improve fetal, infant, child and adult health: Clinical Practice Guidelines. The University of Auckland, Auckland. New Zealand. 2015. https://www.ligginstrials.org/ANC_CPG/downloads/Antenatal_Corticosteroid_Clinical_Practice_Guidelines.pdf




