Vaginal leiomyoma: a case report and narrative review
Leiomiomul vaginal: prezentare de caz şi review narativ
Abstract
Leiomyoma is one of the most common tumors of mesenchymal origin, being detected in 70% of women of reproductive age. Vaginal leiomyoma (VL) refers to quite rare tumors. To date, about 300 cases of VL have been published in the English language specialized literature. We present the case of a 25-year-old patient, complaining of vaginal discomfort and periodic pains of varying intensity. Ultrasonography examination revealed a 21.9x17.6 mm hypoechoic mass on the anterior vaginal wall, normal-sized uterus, and normal bilateral adnexa. MRI examination determined a 25x18x22 mm isointense solid tumor in the fornix (the left side of the cranial part of the vagina), clearly dissociated from the surrounding tissues. Surgical enucleation was performed. Histopathology testing of the specimen revealed that it was a leiomyoma of the vagina. A clinical examination at a follow-up consultation, after 14 months, showed that her vagina was normal. We also present a brief review of the English language literature on the features of diagnosis and treatment methods for vaginal leiomyoma.Keywords
vaginal myomamyomectomyleiomyomaRezumat
Leiomiomul este una dintre cele mai frecvente tumori de origine mezenchimală, fiind detectat la 70% dintre femeile de vârstă reproductivă. Leiomiomul vaginal (LV) se referă la tumori destul de rare. Până în prezent, aproximativ 300 de cazuri de LV au fost publicate în literatura de specialitate în limba engleză. Prezentăm cazul unei paciente de 25 de ani, cu acuze de disconfort vaginal şi dureri periodice de intensitate diferită. Examenul ecografic a evidenţiat o masă hipoecogenă de 21,9x17,6 mm pe peretele vaginal anterior, uter de dimensiuni normale şi anexe bilaterale normale. Examenul IRM a pus în evidenţă o tumoră solidă, izointensă, de 25x18x22 mm în fornix (partea stângă a părţii craniene a vaginului), clar disociată de ţesuturile adiacente. S-a efectuat enuclearea chirurgicală. Testele histopatologice ale specimenului au evidenţiat un leiomiom al vaginului. Un examen clinic la distanţă, după 14 luni, a arătat că vaginul pacientei era normal. De asemenea, prezentăm o scurtă trecere în revistă a literaturii în limba engleză privitoare la caracteristicile metodelor de diagnostic şi tratament pentru leiomiomul vaginal.Cuvinte Cheie
miom vaginalmiomectomieleiomiomIntroduction
Leiomyoma is one of the most common tumors of mesenchymal origin, being detected in 70% of women of reproductive age(1). More frequently, this type of tumor is located in the uterine body, and vaginal leiomyoma refers to quite rare tumors(2,3). To date, about 300 cases of vaginal leiomyomas have been published in the English language specialized literature(4,5).
Vaginal leiomyoma (VL) refers to slow-growing tumors, being characterized by the presence of a small, painless mass over several years(3,6). In case of symptomatic VL, the clinical manifestations are quite various and depend mostly on the location and size of the tumor(7-11). The correct preoperative diagnosis of vaginal leiomyoma in some cases presents some difficulties, and the definitive diagnosis is established at the pathomorphological examination of the removed tumor(6,7,10,11). Due to the low incidence of VL, the diagnostic and therapeutic algorithm of this tumor has not been developed until now(6). Given the rarity of this pathology, we present our own clinical observation of vaginal leiomyoma.
Case report
A 25-year-old patient, gravida 0, para 0, complaining of vaginal discomfort and periodic pains of varying intensity, was hospitalized for scheduled surgical treatment with tumoral mass in the vaginal wall. The tumor was detected on an outpatient basis during the transvaginal ultrasonography examination which revealed a 21.9x17.6 mm hypoechoic mass on the anterior vaginal wall, with well-defined margins, similar to vaginal fibroma. Uterus and adnexa were unremarkable.
When assessing the general condition of the patient, no concomitant diseases were identified (ASA class 1) and no abnormalities were found in the laboratory parameters. Gynecological status: menarche from 13 years old, 4-5 days, regular, moderate. Sex life since the age of 19 years old. A gynecological examination revealed a mass in the vagina from the anterior wall, of 2x2 cm, being hard to the touch (palpatory), with a smooth surface.
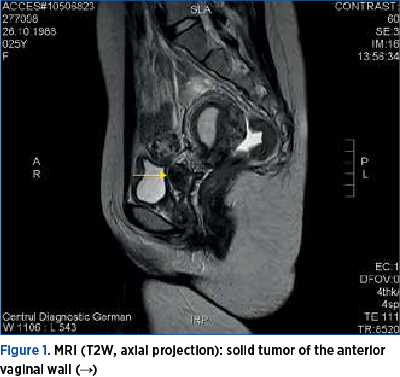
On magnetic resonance imaging (MRI) (Figure 1), vaginal leiomyomas appear as well-demarcated solid masses of low signal intensity in T1- and T2-weighted images, with homogenous contrast enhancement. The MRI examination revealed a 25x18x22 mm isointense solid tumor in the fornix (the left side of the cranial part of the vagina), clearly dissociated from the surrounding tissues. The preoperative diagnosis was vaginal fibroma.
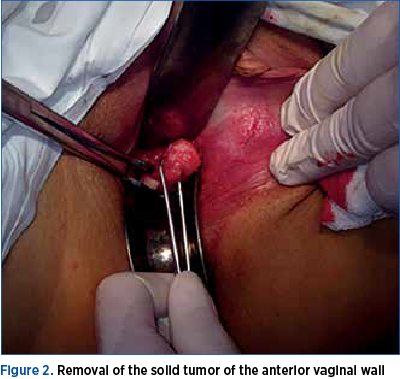
Surgical enucleation was performed with the patient under intravenous general anesthesia. The tumor was fixed with forceps and completely enucleated and exteriorized using a lateral colpotomy (Figure 2). The incision was sutured with Vicryl (2/0), the operation time being 20 minutes, and the blood loss was evaluated as being minimal.
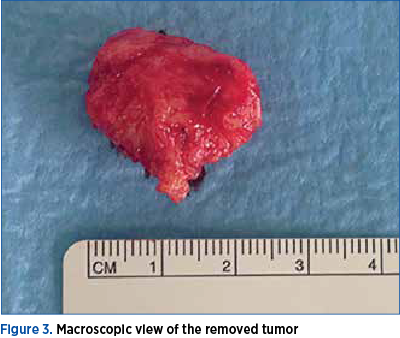
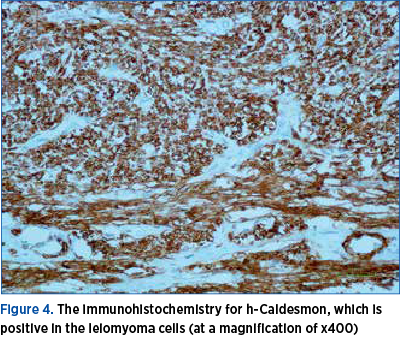
The removed tissue was a sharply circumscribed, round, firm, 2x3 cm solid tumor, whitish in section (Figure 3). The tumor tissue consisted of well-differentiated smooth muscle cells. Immunohistochemically, the tumor cells were stained intensely with alpha-SMA and h-Caldesmon (Figure 4). The diagnosis of leiomyoma was subsequently established.
The patient had an uneventful postoperative recovery. Her hospital stay was two days. A clinical examination at a follow-up consultation, after 14 months, revealed the complete healing and no vaginal abnormalities. The patient is asymptomatic, and at the time of the transvaginal ultrasonographic examination we didn’t identify any tumor recurrence.
Discussion
Vaginal leiomyoma was first described by Denys de Leyden, in 1733(7). Vaginal leiomyoma refers to a rather rare pathology, therefore Braga et al. (2020), based on a systematic review of the literature (using the PRISMA principle) with the use of Medline, Embase and PubMed databases, found 85 documented cases of VL during the last 20 years(12).
The exact histogenesis of vaginal leiomyoma is not fully established; however, according to the specialized literature, there is a hypothesis that these tumors originate from smooth muscle fibers or from the remaining tissue of embryonic vessels(5,12). Vaginal leiomyoma occurs more frequently in the fourth and fifth decades of life(6,9,10,12), but unique cases of vaginal leiomyomas in adolescent girls(8) and in postmenopausal patients(13) are also described. Moreover, taking into account that vaginal leiomyomas are estrogen-dependent tumors, their regression was observed in menopause or at the administration of gonadotropin-releasing hormones(12,14).
These tumors arise most commonly from the anterior vaginal wall, causing various clinical presentations(3,7-9,12,14). According to Braga et al. (2020), vaginal leiomyomas are located in the anterior wall of the vagina in 69.5% of cases, and less often in the posterior wall (17%) and lateral walls (13.5%) of the vagina(12). In some cases, vaginal leiomyoma is combined with uterine leiomyomas(7).
It is unanimously accepted that vaginal leiomyoma refers to tumors with a slow growth, but cases of progressive growth over a short period of time up to 7 cm in diameter are described in the literature as well(10). Most often, vaginal leiomyomas are small in size (from 1.5 to 5 cm) and, as a rule, they are covered by the smooth and intact mucosa of the vagina(3,7,9). At the same time, there are unique publications on vaginal leiomyomas with dimensions larger than 10 cm(4,6,8,13,15). In some cases, vaginal leiomyomas are associated with the appearance of trophic disorders on the vaginal mucosa, defects with purulent discharges and contact bleeding(4,5,10,11).
Due to the small size of the tumor, vaginal leiomyomas remain asymptomatic for a long period of time(6,12). The clinical manifestations of VL are quite various and largely depend on the location of the tumor and its size, and may be manifested by pain, dyspareunia, hemorrhages, urine retention, dysuria and prolapsed vaginal mass(4-17). Due to the wide range of symptoms, vaginal leiomyoma is rarely diagnosed preoperatively and is erroneously interpreted as pedunculated uterine leiomyoma (myomatous node at birth), cervical fibroids, cervical polyp, vaginal cysts, Bartholin gland volume formations, cystocele, hematocolpos or malignant tumors(2,7,8,10,12,15).
Usually, the imaging examinations in the VL are aimed at elucidating the nature of the tumor, its location and the differential diagnosis with malignant tumors in this area(10). When using transvaginal ultrasonography, this type of tumor appears as a well-defined, solid mass, with a echogenicity similar to the one of the uterus(3-5,14,16). In the presence of tumor necrosis and hyaline degeneration, vaginal leiomyomas are defined as heterogeneous mass(8).
On MRI, vaginal leiomyomas are presented as a solid tumor with a smooth contour with hypointense signal in T1W and with homogeneous, hyperintense signal in T2W(3,4,7,11,14,16). It should be noted that the radiological characteristics of VL depend on the histopathological changes (hemorrhages, necrosis) in the tumor tissues and can mimic malignant tumors (leiomyosarcoma, rhabdomyosarcoma)(8,10). In unique cases, the preoperative biopsy of the tumor was used for the successful diagnosis of vaginal leiomyoma(4,14).
The surgical treatment is the only method of treating vaginal leiomyoma, and the surgical approach depends on the location and dimensions of the VL(5,8,11,14). In most cases (more than 90%), the transvaginal approach is used for VL removal(3-11,13,14,16). In rare cases, when the size of the tumor is huge and it is located in the upper third of the vagina, it is recommended to use laparotomy or the combined approach (transabdominal plus transvaginal)(9,12,15). Zhang et al. (2020) published the use of laparoscopic techniques for the removal of a 5-cm vaginal leiomyoma located in the upper third of the vagina. The authors claim that during laparoscopic operations a better visualization of the dissection area is created, which prevents injury of the bladder, ureters, rectum etc.(17)
Liu et al. (2021) used GnRH analogues for six months preoperatively to reduce VL sizes occupying the entire vaginal cavity and with subsequent transvaginal tumor removal. The authors found that the vaginal leiomyoma at the time of surgery was two times smaller than the initial size, which made it possible to simplify and secure the surgery(14).
The goal of surgery in VL is enucleation (excision) of the tumor(3-17). In the case of vaginal leiomyoma removal from the anterior wall of the vagina, the ratio between the tumor and the urethra and the urinary bladder must be taken into consideration, and preventive urinary catheterization is recommended(5,7,9,10). For vaginal leiomyomas located on the side walls of the vagina, the growth in the pararectal space is characteristic, which dictates a clear definition of their localization in relation to the wall and the sphincter apparatus of the rectum(11,13). In the case of a combination of vaginal leiomyoma with uterine leiomyoma, one-time surgical intervention was performed – hysterectomy with appendages and vaginal myomectomy(7).
Macroscopically, in the vast majority of cases, vaginal leiomyomas are presented as solid, elastic formations and sometimes with the presence of the capsule(2,4,5,12,16). The morphological examination of VL revealed three histopathological variants: fusiform, epithelial and myxoid(3,4,6,10). In some cases, areas of necrosis, hyaline and cystic degeneration were determined(8-10). The histopathological examination provides a differential diagnosis of VL with atypical leiomyoma and leiomyosarcoma(6,9).
The immunohistochemical studies of vaginal leiomyomas usually show diffuse cytoplasmic expression of smooth muscle actin (SMA)(2,3,10), and positive expression of estrogen receptors (ER) and progesterone receptors (PR)(14). A negative reaction to DOG1, CD 117 and CD34 is characteristic for VL(15). The recurrence of vaginal leiomyoma after surgical treatment is an extremely rare phenomenon, but still, the surveillance after this category of patients is mandatory(2,3,6,8-10,12).
In conclusion, vaginal leiomyoma should be considered in the differential diagnosis of benign and malignant vaginal tumors. MRI allows the correct preoperative diagnosis of vaginal leiomyoma, determining the exact location, size and relationship with neighboring structures, as well as the presence/absence of uterine leiomyoma. The information obtained by MRI allows to adequately plan the access and volume of the surgical intervention. The removal of small vaginal leiomyomas through the transvaginal approach is the method of choice in the treatment of this pathology.
Ethics. Written informed consent was obtained from the patient for the publication of the present study.
Funding. The author has no funding to report.
Competing interests. The author has declared that no competing interests exist.
Acknowledgements. The author has no support to report.
Conflict of interest: none declared
Financial support: none declared
This work is permanently accessible online free of charge and published under the CC-BY.
Bibliografie
-
Stewart EA, Cookson CL, Gandolfo RA, Schulze-Rath R. Epidemiology of uterine fibroids: a systematic review. BJOG. 2017;124(10):1501-1512.
-
Heller DS. Benign tumors and tumor-like lesions of the vulva. Clin Obstet Gynecol. 2015;58(3):526-35.
-
Witherspoon C, Garcia B, Behbehani S, Nahas S, Stuparich MA. Vulvar leiomyoma presenting as a painless vulvar mass. J Minim Invasive Gynecol. 2022;29(2):187-189.
-
Egbe TO, Kobenge FM, Metogo JAM, Manka’a Wankie E, Tolefac PN, Belley-Priso E. Vaginal leiomyoma: medical imaging and diagnosis in a resource low tertiary hospital: case report. BMC Womens Health. 2020;20(1):12.
-
Patil RR, Vijay NR, Joshi S. An unusual presentation of vaginal leiomyoma. J Midlife Health. 2019;10(4):204-205.
-
Sun C, Zou J, Wang Q, Wang Q, Han L, Batchu N, Ulain Q, Du J, Lv S, Song Q, Li Q. Review of the pathophysiology, diagnosis, and therapy of vulvar leiomyoma, a rare gynecological tumor. J Int Med Res. 2018;46(2):663-674.
-
Akkamahadevi CH, Neekita P, Pooja S, Bhavana N, Prashanth R, Shivakumar KS. Benign primary vaginal leiomyoma – a diagnostic challenge: Rare case report. Eur J Obstet Gynecol Reprod Biol. 2020;247:261-262.
-
Upadhyay M, Chauhan M, Gautam S, Yadav TC. Rare case of vaginal leiomyoma in an adolescent girl: a diagnostic dilemma. Int J Reprod Contracept Obstet Gynecol. 2018;7(3):1269–72.
-
Koranne PS, Raut D, Wahane A, Uike P. A rare case of anterior vaginal wall leiomyoma. J Obstet Gynaecol India. 2015;65(2):129-31.
-
Sim CH, Lee JH, Kwak JS, Song SH. Necrotizing ruptured vaginal leiomyoma mimicking a malignant neoplasm. Obstet Gynecol Sci. 2014;57(6):560-3.
-
Wethmara EI, Moutona AD, Dreyera G. Vaginal leiomyoma presenting as a lateral vaginal wall mass. South Afr J GynaecolOncol. 2017;9(1):16–18.
-
Braga A, Soave I, Caccia G, Regusci L, Ruggeri G, Pitaku I, Bassi V, Papadia A, Serati M. What is this vaginal bulge? An atypical case of vaginal paraurethral leiomyoma. A case report and literature systematic review. J Gynecol Obstet Hum Reprod. 2020:101822.
-
Goyal LD, Kaur H, Kaur K, Kaur S. An unusual case of vaginal myoma presenting with postmenopausal bleeding. J Family Reprod Health. 2013;7(2):103-4.
-
Liu Y, Wang X, He Y. GnRH analogue followed by surgery in treatment of vaginal leiomyoma - a case report. Medicine (Baltimore). 2021;100(8):e24911.
-
Asnani M, Srivastava K, Gupta HP, Kunwar S, Srivastava AN. A rare case of giant vaginal fibromyoma. Intractable Rare Dis Res. 2016;5(1):44-6.
-
Lőrincz J, Jakab A, Török P. Vaginal fibroma: An unusual vaginal tumor. J Gynecol Surg. 2017;33(3):114-116.
-
Zhang NN, Li D, Chen SL, Zuo N, Sun TS, Yang Q. An effective method using laparoscopy in treatment of upper vaginal leiomyoma. Fertil Steril. 2020;114(1):185-186.




