Intratumoral heterogeneity in breast cancer – a real challenge for diagnosis and treatment
Heterogenitatea intratumorală în cancerul de sân – o adevărată provocare de diagnostic şi tratament
Abstract
We present the case of a patient with breast neoplasm which presented a particular evolution with pronounced molecular intratumoral heterogeneity proven at multiple biopsies. If in the first instance, at the primary tumor it was discovered a negative molecular HER2 luminal B pattern, in the end stage, after treatment with neoadjuvant chemotherapy, the residual tumor from the mastectomy tissue presented a luminal B profile with HER2 amplification. Under targeted anti-HER2 treatment, there was cutaneous and pleural progression, lesions that were subjected to biopsy and which revealed the presence of secondary masses with triple negative molecular pattern.Keywords
breast cancerintratumoral heterogeneityHER2 amplificationtriple negative breast cancerRezumat
Prezentăm cazul unei paciente cu neoplasm mamar la care, în evoluţia bolii, prin biopsii multiple, s-a remarcat o pronunţată heterogenitate intratumorală din punctul de vedere al constelaţiei moleculare. Pornind de la o tumoră primară cu pattern molecular de tip luminal B HER2 negativ, s-a ajuns la un profil luminal B cu amplificare HER2 în tumora reziduală din piesa de mastectomie, după chimioterapia neoadjuvantă. Sub tratament ţintit anti-HER2, s-a înregistrat progresie la nivel cutanat şi pleural, leziuni ce au putut fi abordate biopsic, caz în care s-a remarcat prezenţa de determinări secundare cu pattern molecular triplu negativ.Cuvinte Cheie
cancer de sânheterogenitate intratumoralăamplificare HER2cancer de sân triplu negativIntroduction
In recent years, the intratumoral heterogeneity of breast cancer has been very debated, and this phenomenon has become a real challenge in terms of diagnosis, treatment and management of patients. State-of-the-art technology and molecular biology research have allowed the breast neoplasm to be approached as an entity composed of multiple cell subtypes.
This case illustrates the temporal and spatial heterogeneity of breast malignancy, the versatility and cellular adaptability, and emphasizes the importance of repeated biopsies throughout the course of the disease. Nowadays, the intratumoral heterogeneity of breast cancer is considered one of its many mechanisms of resistance(1).
Case report
We present a case of breast cancer in a 64-year-old female patient, admitted to the “Prof. Dr. Alexandru Trestioreanu” Institute of Oncology, Bucharest, for a suspicious tumor on the left breast. The patient was without family or personal history of cancer and without other associated pathologies. Our patient was postmenopausal and had given birth to two children whom she had breastfed for approximately six months. On physical examination, there was an approximatively 2-cm mass in her left breast, with no nipple retraction or discharge, no changes in the overlying skin, and palpable axillary lymph nodes. The initial mammography and breast ultrasound showed the presence of a tumor in the inferior left quadrant, measuring 1.7x1.3 mm, which associated axillary lymphadenopathy with a BIRADS score of 5.
An ultrasound-guided core biopsy was performed, after which the histopathological and immunohistochemical examinations indicated the presence of invasive breast cancer, moderately differentiated, with positive hormone receptors (Allred score 3), without amplification of the HER2 component (score 0), and with a Ki-67 proliferation index of 35%.
Pre-therapeutic CT scan imaging confirmed the presence of the left mammary node associated with left axillary lymphadenopathy, with no evidence of distant metastasis. Madden modified radical mastectomy with axillary lymphadenectomy was performed following six series of neoadjuvant chemotherapy with epirubicin 90 mg/m2/cyclophosphamide 600 mg/m2. The pathology showed an incomplete response ypT1b ypN2a, with the presence of residual tumor in which the amplification of the HER2 protein was objectified. For the first time, a molecular conversion of a negative HER2 luminal B subtype to a positive HER2 luminal B appeared. Adjuvant anti-HER2 therapy in combination with taxane-based chemotherapy was given for 12 months, followed by hormone therapy letrozole. After nine months of anti-HER2 therapy, CT imaging evaluation showed hepatic metastasis and adenopathy in the anterior mediastinum and in the hepatic hilum (Figure 1).
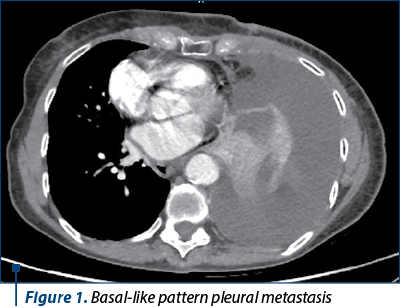
Pertuzumab systemic therapy was initiated in combination with trastuzumab and docetaxel for five months, at which time the patient presented with an altered general condition, dyspnea at rest and fatigue. Imagistically, numerical and dimensional progression of the disease was noted, including at the postoperative scar. In addition, a large left pleural effusion that caused the left lung to collapse was described and mass effect on the mediastinal structures was encountered.
Pleural drainage followed by chemical pleurisy with talc made by the thoracic surgeon was required and the patient had a good evolution. Pleural and postoperative scar biopsies were also taken and the pathological results showed the presence of secondary masses originating from the breast carcinoma with a triple-negative immunohistochemical constellation (Figure 2).
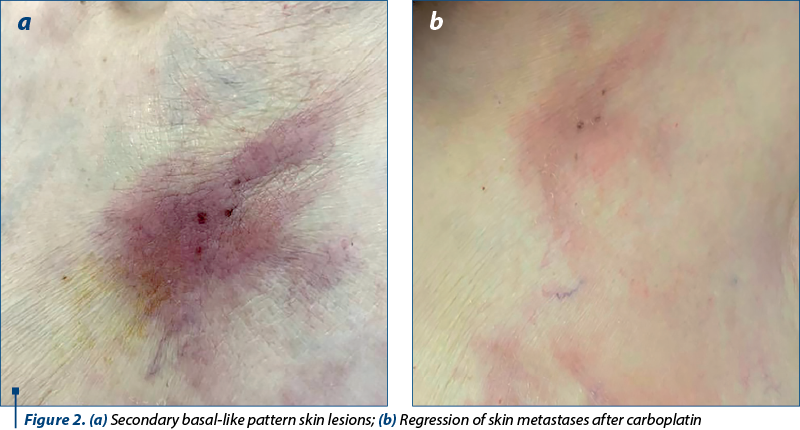
A new molecular pattern emerged, marking at the same time the existence of a dual metastatic disease, one with positive HER2 secondary lesions, and one with skin and pleural basal-like type lesions.
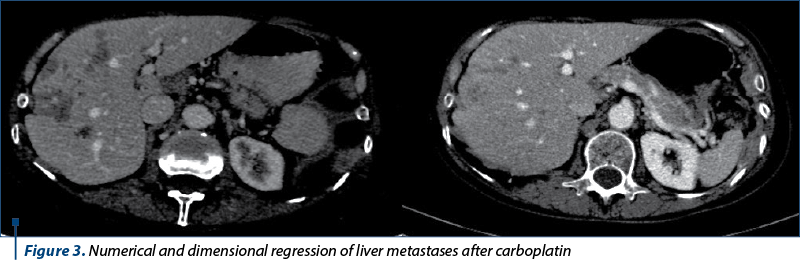
A complex therapeutic approach was initiated, which required the administration of an oncological treatment targeting both the basal-like cellular component and the HER2 amplification. The addition of carboplatin to the pertuzumab-based treatment in combination with trastuzumab and docetaxel appeared to have been a successful option. A positive evolution of the patient, with almost complete remission of clinical signs, including significant regression of secondary skin lesions, numerical and dimensional regression of pleural, hepatic and lymph node metastases, was noted (Figures 2 and 3).
Discussion
Currently, breast malignancies are seen as complex entities and heterogeneous in terms of phenotype and genetics. Heterogeneity is also described both in the primary tumor and in the case of metastases. Also, modern therapeutic approaches are increasingly based on gene expression profiling.
To explain the intratumor heterogeneity in breast cancer, two theories have been developed: malignant stem cells and clonal evolution. These two theories are complementary, both supporting the idea of a primordial malignant cell of the primary tumor with multiple molecular alterations and with unlimited proliferative potential. Both theories also emphasize the importance of the microenvironment and its influence on the tumor evolution.
The theory of clonal evolution appeared first in 1976, stating that a single cell leads to the formation of a tumor through the continuous accumulation of mutations, thus allowing genetic instability which leads to various subpopulations with increasingly aggressive phenotypes. In turn, each cell subpopulation will mutate independently, thus contributing to the intratumoral heterogeneity(2,3).
The cell line is frequently compared to a tree, where the trunk is the original cell and the branches are different subclones arranged separately from a spatial point of view and store various mutations during their evolution. In this theory, breast cancer intratumoral heterogeneity can be observed in HER2-positive tumors, where in distinct regions of the tumor we can observe cells with different patterns of HER2 amplification(4,5).
Unlike the clonal evolution model, which emphasizes that all cells in a tumor have the same potential for tumor progression, malignant stem cell theory states that a tumor is based on a small cell population capable of renewal. Subsequently, malignant stem cells undergo a process of non-stem differentiation, this way obtaining numerous subpopulations with new sets of markers. This aberrant way of differentiating malignant stem cells appears to be responsible for intratumoral heterogeneity(5,6).
Conclusions
The intratumoral heterogeneity of malignant breast tumors makes this pathology a real challenge for the oncologist, both in terms of diagnosis and especially in terms of therapeutic approach. This feature of breast cancer supports the need for a personalized therapeutic approach, which takes into account both the cellular phenotype and the tumor microenvironment.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
Turner NC, Reis-Filho JS. Genetic heterogeneity and cancer drug resistance. Lancet Oncol. 2012;13:e178-85.
-
Greaves M, Maley CC. Clonal evolution in cancer. Nature. 2012;481:306-13.
-
Burrell RA, McGranahan N, Bartek J, Swanton C. The causes and consequences of genetic heterogeneity in cancer evolution. Nature. 2013;501:338-45.
-
Ferlay J, Soerjomataram I, Dikshit R, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer. 2015;136:E359-8
-
Plaks V, Kong N, Werb Z. The cancer stem cell niche: how essential is the niche in regulating stemness of tumor cells? Cell Stem Cell. 2015;16:225-38.
-
Esparza-López J, Escobar-Arriaga E, Soto-Germes S, Ibarra-Sánchez MJ. Breast Cancer Intra-Tumor Heterogeneity: One Tumor, Different Entities. Rev Invest Clin. 2017 Mar-Apr;69(2):66-76.



