Screeningul naţional pentru cancerul de col uterin. Experienţă preliminară pentru screeningul cancerului de sân
National screening for cervical cancer. Preliminary experience for breast cancer screening
Abstract
Introduction. In Romania, cervical cancer is a public health issue, 4000 women being diagnosed annually with this disease, of which 2000 will die. The incidence is three times higher than UE average. A total of 9629 women are diagnosed with breast cancer annually, and deaths reaches 3209. Approximately 90% of these patients are diagnosed in stages II, III or IV. The high rate of cancer cases diagnosed in advanced stages is caused by the lack of an organised screening, Romania being one of the few European countries which doesn’t have implemented yet a screening program for breast cancer. Another causes are represented by the low level of health education and the difficult access to some medical services and adequate treatments. Materials and method. World Health Organization and European Cancer Leagues recommend, among the preventing measures for cervical cancer scientifically proven to be effective, the screening for active early detection, along with HPV vaccination. The Ministry of Health, through the national program for the active early detection, reinitiated the screening campaign through improving the informing level regarding cervical cancer, and the access facilitation for a large number of women for performing free Babeş-Papanicolaou testing (Ministry of Health Order no. 377/2017). In 2018, the “Prof. Dr. Alexandru Trestioreanu” Institute of Oncology (IOB) and the Romanian Patriarchy signed a collaborative protocol for performing Babeş-Papanicolaou test in disadvantaged areas from Ilfov county, the Romanian Patriarchy taking care of logistics and publicity. Results. If in a two-year period at IOB there had been performed maximum 20 tests and none in 2017, after the collaboration with the Patriarchy 581 women have been tested between 2018 and 2019. Of these, 7.87% presented aggressive lesions which needed additional investigations (colposcopy ± biopsy, HPV phenotyping for revealing agressive strains), and approximately 25.3% needed treatments for infections/inflammations. A breast clinical exam was also performed in 120 women. Conclusions. The patients are not sufficiently informed regarding the necessity and utility of the screening. The collaboration between the family doctors and the local authorities was essential for the actions coordinated by IOB and the Romanian Patriarchy. The publicity realized within parishes made by the Patriarchy decisively contributed to the increase of the number of patients compliant to screening. Thus, late diagnostication leads to serious consequences, both on survival chances and quality of life, but also on social and financial resources assigned by the Romanian state for the management of each case and at the institutional level. In the future, it is necessary a larger mediatic coverage from the Ministry of Health along with local authorities and family doctors, the solution being represented by inviting letters for screening participation.Keywords
screeningcervical cancerbreast cancerRezumat
Introducere. Cancerul de col uterin reprezintă o problemă de sănătate publică în România, anual fiind diagnosticate 4000 de femei şi înregistrate 2000 de decese. Incidenţa este de trei ori mai mare decât media ratei din UE. 9629 de femei sunt diagnosticate cu cancer mamar în fiecare an, iar numărul deceselor se ridică la 3209. Aproximativ 90% dintre aceste paciente sunt diagnosticate în stadiile II, III sau IV. Rata mare a cazurilor de cancer diagnosticate în stadiu avansat este cauzată de lipsa screeningului organizat, România fiind una dintre puţinele ţări europene care nu are încă implementat un program de screening pentru cancerul de sân. Alte cauze sunt reprezentate de nivelul scăzut al educaţiei privind menţinerea stării de sănătate şi de accesul dificil la anumite servicii medicale şi tratamente adecvate. Materiale şi metodă. Organizaţia Mondială a Sănătăţii şi European Cancer Leagues recomandă screeningul pentru depistarea activă precoce şi vaccinarea HPV printre măsurile de prevenire a cancerului dovedite ştiinţific ca fiind eficiente. Ministerul Sănătăţii, prin programul naţional pentru depistarea activă precoce, a reînceput campania de screening, prin îmbunătăţirea nivelului de informare privind cancerul de col şi facilitarea accesului unui număr mare de femei la testarea gratuită Babeş-Papanicolau (Ordinul M.S. 377/2017). În anul 2018, Institutul Oncologic „Prof. Dr. Alexandru Trestioreanu” (IOB) a semnat un protocol de colaborare cu Patriarhia Română pentru realizarea de recoltări Babeş-Papanicolau în zonele defavorizate din judeţul Ilfov, Patriarhia ocupându-se de logistică şi mediatizare. Rezultate. Dacă timp de doi ani în IOB s-au realizat maximum 20 de recoltări, iar în 2017 nicio recoltare, după începerea colaborării cu Patriarhia Ortodoxă Română s-au testat 581 de femei, în perioada 2018-2019. La 7,74% dintre acestea s-au depistat leziuni agresive care au necesitat investigaţii suplimentare (colposcopie ± biopsie, fenotipare HPV pentru evidenţierea tulpinilor agresive), iar aproximativ 25,3% au necesitat tratamente pentru infecţii sau inflamaţii. La 120 de paciente s-a realizat şi un examen clinic al sânilor. Concluzii. Pacientele nu sunt încă suficient informate cu privire la necesitatea şi utilitatea screeningului. Colaborarea dintre medicul de familie şi autorităţile locale a fost esenţială pentru desfăşurarea acţiunii coordonate de IOB şi Patriarhie. Mediatizarea prin parohii realizată de Patriarhie a contribuit decisiv la creşterea numărului de paciente aderente la acţiune. Astfel, diagnosticarea tardivă ajunge să aibă consecinţe majore, atât asupra speranţei de supravieţuire şi a calităţii vieţii, cât şi asupra resurselor financiare şi sociale alocate de statul român pentru managementul fiecărui caz în parte şi la nivel de sistem. Pe viitor, este necesară o implicare mediatică mai mare a Ministerului Sănătăţii alături de autorităţile locale, soluţia fiind scrisorile de invitare la participarea la screening.Cuvinte Cheie
screeningcancer colcancer sânIntroduction
Cervical cancer is the most frequent neoplasia of the genital area in women and the second cause of mortality, after breast cancer. Annually, there are diagnosed approximately 500,000 new cases of cervical cancer worldwide. The screening program for cervical cancer is meant to discover premalignant lesions which can be removed before the onset of cancer or an early-staged cancer that is easier to treat(1-4).
In Romania, cervical cancer is a public health issue, being the second most frequent type of cancer in women between 15 and 44 years old. Annually, 4000 women are diagnosed with this disease, of which 2000 will die(3).
Cervical cancer represents 12% of the total number of neoplasms diagnosed each year in the European Union, our country ranking first regarding incidence, which is three-fold higher than the European average (34.9/100,000 women in Romania versus 11.3/100,000 women in EU)(3,5).
In our country, there are 6 million women between 25 and 64 years old, more than 700,000 living in Bucharest-Ilfov region. Between 2012 and 2017, more than 700,000 women (10.8%) benefited from the Ministry of Health screening program. The total number of tests performed in 2008 was 42,154, which means an annual coverage rate of eligible aged persons of 7.47%. The optimal coverage rate of eligible people for the program to be effective is 14% per year, for a 5-year period of the program. The number of Babeş-Papanicolaou test to be made in one year of this program should be approximately 780,000. In Bucharest-Ilfov, the rate was 5.9% (5.2% in Ilfov, and 6.1% in Bucharest)(6). The program is considered efficient when more than 60% of the women have been tested. In contrast, other countries have significantly higher participation rates: Norway – 78.9%, Denmark – 66.3%, UK – 78.5%, Finland – 100% (beginning the screening in 1960) etc.(7)
Materials and method
The cervix presents squamous cells on its surface (exocervical area) and glandular cells (endocervical area). The transition area between the two categories of cells (transformation area) is the most frequent site of preneoplastic lesions. The evolution towards cancer is slow, in 10-20 years. Therefore, it is important to make a Babeş-Papanicolaou test(1-3). The risk factors for the development of cervical neoplasia are: human papillomavirus (HPV), infection with Herpes hominis type 2 virus (HSV2), HIV/AIDS, smoking, the early onset of sexual activity, deficient hygiene, multiple pregnancies, oral contraception use, sexual promiscuity, and familial history of cervical cancer. HPV infection is transmitted through sexual intercourse and preceds with a few years the development of intraepithelial lesions which can evolve to cervical cancer. The disease can be prevented, being preceded by preneoplastic lesions classified as CIN 1-3 (cervical intraepithelial neoplasia 1-3) or moderated/severe dysplasia, with a slow evolution, over 10-20 years. HPV strains 16 and 18 have a high oncogenic risk (more than 70% of the cervical cancers). HPV 16, 18, 31, 33, 45, 52 and 58 are responsible for 90% of the cervical neoplasms. Statistically, 80% of the sexually active women will be infected with HPV at least once in their life, worldwide(8). The infection does not mean that the person will develop cervical cancer. Most lesions are asymptomatic and transient. Both men and women can carry the virus and transmit it further, but 90% of people will heal by themselves in two years. Preneoplastic lesions and cervical cancer in early stages can be found at the periodic Babeş-Papanicolaou exam (3-5 years). Thus, the disease incidence is reduced by 80%, and the severe evolution can be prevented. HPV can also cause other types of cancer, the virus being present in more than 70% of vulvar, vaginal, penile, oropharyngeal and anal cancers(9,10).
Treatments recommended for CIN 2-3: ablative therapies (cryosurgery, CO2 laser therapy, diathermic electrocoagulation, electrosurgical excision [LEEP], RFA); conization may be the only therapeutic method when the depth of invasion is <3 mm and there is no vascular/lymphatic invasion, and the margins are histologically negative; it is recommended especially in young women who want to preserve fertility; radical trachelectomy – cervix removal; simple total hysterectomy when the depth of invasion is <3 mm (conization with free margins) and there is no vascular and lympathic invasion – ovariectomy is optional and must be avoided in young women; radical hysterectomy with regional lymphadenectomy (Wertheim surgery, performed clasically, laparoscopically or robotically) in patients with 3-5 mm depth of tumoral invasion or uncertain (conization with free margins), with a 10% risk for regional ganglionary metastases; intracavitary brachytherapy alone when the depth of tumoral invasion is <3 mm and there is no lymph invasion; external radiotherapy ± brachytherapy.
Patients’ survival is good in early stages. The average 5-year survival rate in all cancer stages is 75%. In stage I, when precancerous lesions are discovered, there are 99-100% healing chances. In stage II, when cancer exceeded cervix but didn’t reach the pelvic floor, there are 60% healing chances. In stage III, when cancer reached the pelvic floor, there are 22% recovery chances, and in stage IV, when cancer invaded the bladder and rectum, there are 7% survival chances.
World Health Organization (WHO) and European Cancer Leagues recommend, among the preventing measures for cervical cancer scientifically proven to be effective, the screening for active early detection, along with HPV vaccination(2). The Ministry of Health, through the national program for the active early detection, reinitiated the screening campaign through improving the informing level regarding cervical cancer, and the access facilitation for a large number of women for performing free Babeş-Papanicolaou testing. Thus, women can benefit of free testing if they are aged between 25 and 64 years, regardless they are insured through the national security system; the patients must not have a confirmed diagnosis of cervical cancer and must be asymptomatic (Ministry of Health Order no. 377/2017).
For screening, there can be used the Babeş-Papanicolaou exam (Pap) that uses lamellar cytology or liquid-based cytology. For lesions’ diagnosis it is used the Bethesda classification system, ASC-US/ASC-H, which replaced the CIN2/CIN3 classification system, and beginning with the age of 30 years old, HPV ADN (16 and 18 subtypes) testing can be associated. It is possible to opt for the following association: a) if Pap exam reveals ASC-H/HSIL, colposcopy + biopsy + HPV will be done; b) HPV detection, and in case of positivity, Pap test must be done; in case of ASC-H/HSIL result, colposcopy + biopsy will be done. The check-up must be repeated at 6-12 months. If normal, the patient will be reviewed in three years. Thus, the efficiency of HPV testing is much more sensitive than Babeş-Papanicolaou cytology in determining CIN2 lesions at the screening programs, but it increases the number of colposcopies performed due to the high rate of HPV persistence(11).
Results
In 2018, the “Prof. Dr. Alexandru Trestioreanu” Institute of Oncology (IOB) and the Romanian Patriarchy signed a collaborative protocol for the organization of medical events with humanitarian purposes. The beneficiaries are women from Ilfov county, and the purpose is the early detection of cancer (cervix, breast, colonic-rectal etc.). The volunteers from the Chapel of People’s Salvation Cathedral help IOB logistically and mediatic. The action has the approval of Ilfov Sanitary Direction and is performed in authorized medical practices of family doctors from this local areas. We mention that in 2017 no woman had been tested at IOB, but from the beginning of collaboration with the Romanian Patriarchy, 340 women were tested in 2018, which means 37.9% from the total number of patients with Pap test in Ilfov county. According to Ministry of Health data, in 2018 there were tested 897 women in Ilfov county, and in 2012-2017 the coverage rate of investigations was 5.2%(6). The event was highly mediated at Trinitas TV, TVR and TVR International, but also in online media (amosnews.ro, basilica.ro, hotnews.ro, agerpres.ro, ziarele.com etc.), and was a real success at the level of local community, receiving requests from the rest of the country for extending the screening actions.
The tests have also continued this year, 241 women being investigated in the first six months. Simultaneously, it was initiated a clinical breast examination, 120 women being subsequently directed for imagistic examinations (echography, mammography). Thus, between January 2018 and September 2019, there had been investigated 581 women, and another 50 were informed regarding the importance of cancer prevention. Of these, 45 (7.74%) were diagnosed with lesions at the cervix level, and 147 presented infections and inflammations which needed specialised treatment. The women discovered with health problems were invited at IOB for complex laboratory and imagistic exams (videocolposcopy, ecography, mammography, CT, MRI), but also for performing the adequate surgical and gynecologic treatment. Unfortunately, only a small part – two patients with cervix lesions (4.4%) and ten patients with breast examination (8.3%) – presented at IOB, and other patients, although they were called and informed they had health issues, didn’t go to doctor. The data collected at IOB, as screening coordinator for Bucharest-Ilfov region, revealed that 2133 women were investigated in 2018, and 147 (6.89%) were diagnosed with cervix dysplasia. In the first semester of 2019, there were investigated 1049 women, 80 (7.62%) being found with cervical modifications.
The data presented by the Department of Statistical Evaluation of IOB revealed that in 2018 there were registered and treated at IOB 475 patients with cervical neoplasm histopathologically confirmed, 253 patients being diagnosed in the institute, most of them being older than 40 years of age. Four deaths have been registered. Ten patients were registered with benign tumor diagnosis. Also, data reveal that in 2018 there were admitted 1678 patients with the diagnosis of breast neoplasm (histopathologically confirmed). A total of 740 patients represented new cases, most of them older than 40 years, and 63 cases (8.51%) were in advanced stages (II and III). Three deaths have been recorded for the registered cases. Seventy-one patients were diagnosed with benign breast tumor, 45 being at the first presentation.
Discussion
The screening with Babeş-Papanicolaou primary testing combined with HPV testing performed within the national program for the early detection of cervical cancer could determine an increased rate of positive hystological detection of CIN 2-3 lesions, more than using the simple Pap cytology alone. The issue is represented by the women’s presentation at the doctor, especially of the young persons aged 30 and above. The statistical data offered by countries in which the screening was performed in a proportion larger than 60% reveal that, after the age of 35 years old, women become interested in screening programs (in average, 35 years old in Sweden, 39 years old in UK, 41 years old in Italy and The Netherlands, 50 years old in Finland), and the HPV testing is much more sensitive in detecting CIN 2-3 lesions (97%)(11).
A solution used by other countries is represented by the screening caravans that employ specially equipped vans and which, along with medical personnel specially trained, go to isolated locations and in disadvantaged populations in order to perform specific investigations.
Taking into account the difficulties faced in realising the screening for cervical cancer, we consider that is usefull to use the experience accumulated in 2018-2019 for the screening of breast cancer, also. Thereby, according to estimations, anually there are diagnosed 9629 women at the national level, and the number of deaths is 3209. Approximately 90% of these women are diagnosed in stages II, III or IV (GLOBOCAN 2018)(14). The high rate of cancer cases diagnosed in advanced stages is caused primarly by the lack of organised screening, Romania being one of the few European countries with no screening program for breast cancer implemented yet. Another causes are represented by the low level of health education and the difficult access to some medical services and adequate treatments. Thus, late diagnostication leads to serious consequences, both on survival chances and quality of life, but also on social and financial resources assigned by the Romanian state for the management of each case.
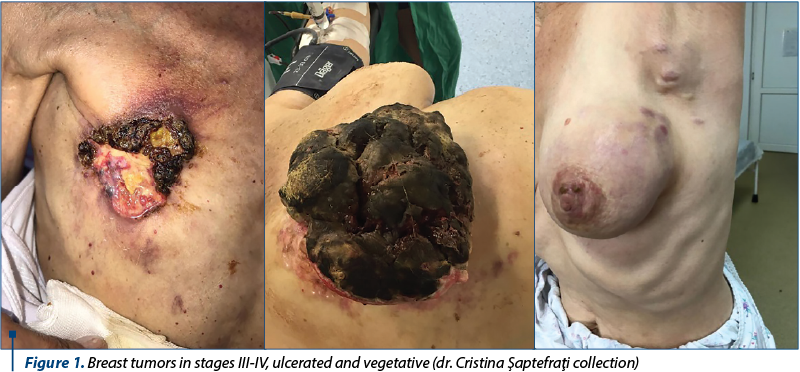
In order to avoid the apparition of new cases such as those presented in Figure 1, it is necessary to realize and apply a screening program for breast cancer. Thus, in many European countries, the screening is addressed to women between 50 and 69 years old, who are invited to perform a mammography every two years (ten mammograms in 20 years). The goal is represented by the early detection of breast cancer, the rapid initiation of treatment, and the improvement of healing chances. Unfortunately, some mammograms give false positive results and lead to the application of unnecessary treatments(15).
The solution chosen by Western countries is to send an invitation letter to people from the targeted group to come at medical centers accredited by the Ministry of Health or by the city hall of those countries. The letter contains a date and an hour for an appointment, and provides information on the screening program and the mammogram to be done. Women are given the choice whether to perform the test. Mammographies are only performed in accredited medical centers for the screening program. Women are warned that the investigation doesn’t prevent breast cancer. Before mammography, the patient must present to physician (family doctor, surgeon, gynecologist) included in the screening program in order to be clinically examined and then sent for testing. If the patient didn’t present at the first invitation, another invitation for mammography will be sent after two years(15).
Clinical and mammographic examinations can be performed in hospitals or in specially equipped vans. The results of the mammograms will pe available in a few days. Two specialised physicians will interpret the images and provide the results. In case of diagnostic discrepancies, a third specialised physician will be consulted. The result of the investigation will be sent to patients in a letter. Most women have normal results, without signs of cancer. It is important to inform the patients that not every mammogram modification is also a sign of cancer. In case of anomalies revealed by radiological images, additional tests will be necessary (ecography, MRI, tomodensitrometry) which can guide the cancer diagnosis.
The medical examiner will recommend for certitude the biopsy puncture at the breast level. After tumor confirmation at the microscopical exam, the multidisciplinary consult will be performed (surgeon-oncologist-radiotherapist) which will establish the following conduct according to disease stage and treatment guides.
The patients who will be subjected to surgical interventions must receive the information regarding the type of surgery: limited interventions, conservative intervention or masectomy, with or without intervention of oncoplastic reconstruction. Other treatments include chemotherapy, radiotherapy and hormonotherapy.
The statistical data reveal that, out of 1000 women, 970 have normal results. Of the 30 patients with abnormal results and subsequently subjected to additional tests, 24 don’t have breast cancer. Only six patients are diagnosed with cancer after supplementary tests. Five out of the six patients are diagnosed with invasive tumors which, not treated on time, can lead to distance metastases, and only one of the six patients is diagnosed with in situ ductal carcinoma. These women will present at the specialised doctor (surgeon, gynecologic oncologist) to receive explanations regarding the treatment to be followed. It was found that only two women in 1000 will be diagnosed with cancer in the two-year interval between mammograms(15).
Thus, the greatest advantages of mammography examination are the detection of cancer in early stages, the survival increase, and the lower risk of death. Between two and six women out of 1000 can be saved from dying using screening methods. The method’s drawback, as in other screening programs, is overdiagnosis and useless surgical interventions. Other exams that can be performed for breast cancer screening are echography and/or MRI, but don’t bring further information compared to mammography(15).
What is to be considered is that mammography does not prevent breast cancer, but can detect incipient stages. The test cannot detect all tumors, therefore these can also develop in the two-year interval between exams. Thus, along with the clinical examination within the screening, women will be instructed to perform breast self-examinations and to go to the doctor when they find breast modifications: nodules, skin modifications, nipple retractions, bleeding at any level etc.
The best method for publicity and for informing the population on national screening programs are the invitation-reinvitation letters sent by the Ministry of Health (Germany: Nationaler Krebsplan – Bundesministerium für Gesundheit, 2017) or by local authorities (Nordic countries). These proved to have the greatest positive impact within population, leading to a significant increase of participation at screening programs. This method also proved beneficial in older patients, in those with low educational level and in immigrants(11,12,16). All data regarding the screening results for cervical and breast cancers must be confidential and take into consideration the regulation for personal data protection.
Conclusions
-
Patients are not yet sufficiently informed regarding the necessity and utility of the screening (cervical cancer, breast cancer, colorectal cancer).
-
The collaboration between the family doctors and local authorities (priest, mayor) was essential for the actions coordinated by the “Prof. Dr. Alexandru Trestioreanu” Institute of Oncology and the Romanian Patriarchy.
-
The publicity provided by the Romanian Patriarchy decisively contributed to the increase of the number of patients compliant to screening.
-
In the future, it is necessary a larger mediatic coverage from the Ministry of Health, along with local authorities and family doctors.
-
The solution are the inviting and reinviting letters (once at one or two years) for screening participation.
-
It is necessary to create a national registry for preneoplastic lesions (cervix, breast, colon).
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- American Cancer Society. What is cervical cancer? Available at: http://www.cancer.org/cervicalcancer/detailedguide/cervical-cancer-what-is-cervical-cancer
- Comprehensive Cervical Cancer Control: A Guide to Essential Practice, 2nd edition. Geneva, World Health Organization, 2014. Available at: http://www.ncbi.nlm.nih.gov/books/NBK269619
- Bruni L, et al. ICO Information Centre on HPV and Cancer (HPV Information Centre). Human Papillomavirus.
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global Cancer Statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018 Nov; 68(6):394-424.
- European Cancer Observatory. Available at: http://eco.iarc.fr//EUCAN/CancerOne.aspx?
- Guvernul României, Ministerul Sănătăţii – Raport activitate 2018. Available at: http://www.ms.ro/wp-content/uploads/2019/05/Raport-de-activitate-MS-2018-2.pdf
- Vaccarela S, et al. 50 Years of Screening in Nordic Countries: Quantifying the Effects on Cervical Cancer Incidence. British Journal of Cancer. 2014; 111.5: 965-969. PMC. Web.
- Wagner M, et al. Global Availability of Data on HPV Genotype-Distribution in Cervical in Cervical, Vulvar and Vaginal Disease and Vaginal Disease and Genotype-Specific Prelevance and Incidence of HPV Infection in Females. Infection Agents and Cancer. 2015; 10 (2015): 13 PMC. WEB.
- Hamborsky J, Kroger A, Wolf S, Centers for Disease Control and Prevention, Epidemiology and Prevention of Vaccine-Preventable Diseases. Chapter 11, Human Papillomavirus eds. 13th ed. Washington D.C. Public Health Fondation, 2015.
- Castellsague X, et al. HPV vaccination against cervical cancer in women above 25 years of age: key considerations and current prespectives. Gynecol Oncol. 2009 Dec; 115(3 Suppl):S15-23.
- Veijalainen O, Kares S, Kujala P, Tirkkonen M, Vuento R, Kholová I, Luukkaala T, Osuala V, Mäenpää J. Human papillomavirus test with cytology triage in organized screening for cervical cancer. Acta Obstet Gynecol Scand. 2016 Nov; 95(11):1220-1227.
- Ferroni E, Camilloni L, Jimenez B, Furnari G, Borgia P, Guasticchi G, Giorgi Rossi P. Methods to increase participation Working Group. How to increase uptake in oncologic screening: a systematic review of studies comparing population-based screening programs and spontaneous access. Prew Med. 2012: 55, 587-96.
- Radde K, Gottschalk A, Bussas U, Schülein S, Schriefer D, Seifert U, Neumann A, Kaiser M, Blettner M, Klug SJ. Invitation to cervical cancer screening does increase participation in Germany: Results from the MARZY study. Int J Cancer. 2016 Sep 1; 139(5):1018-30.
- The Global Cancer Observatory - May, 2019. Available at: https://gco.iarc.fr/today/data/factsheets/populations/642-romania-fact-sheets.pdf
- The breast cancer screening program in Germany. Created: January 27, 2016; Last Update: February 15, 2018. Available at: https://www.ncbi.nlm.nih.gov/books/NBK361021/
- Bundesministerium fur Gesundheit: National Krebsplan – Handlungsfelder, Ziele und Umsetzungsempfehlungen, 2012. Available at: www.bundesgesundheitsministeriunm.de/themen/praevention/nationaler-krebsplan/der-nationale-krebsplan-stell-sich-vor.htlm





