Tratamentul paliativ şi suportiv în cancerul bronhopulmonar avansat
Palliative and supportive care in advanced lung cancer
Abstract
This paper seeks to present concisely the essentialaspects of palliative and supportive therapy in advanced lung cancer. It distinguishes between addressing patient palliative therapy essentials of the human being:
physical, informational, emotional, spiritual and social versus supportive therapy dealing with side effects of treatment with antitumor active medication. It then addresses treatment of main respiratory symptoms (dyspnea and cough) and psychological problems of advanced lung cancer patients. It revealed the idea of palliative care as early in the evolution of patients, element that has been shown in clinical trials as a positive influence on survival.
Keywords
palliative therapyadvanced lung cancersupportive therapyRezumat
Lucrarea caută să prezinte concis aspecte esenţiale în terapia paliativă şi suportivă a cancerului bronhopulmonar avansat. Se face distincţia între terapia paliativă care abordează pacientul din punctele de vedere esenţiale ale fiinţei umane: fizic, informaţional, emoţional, spiritual şi social, faţă de terapia suportivă care tratează efectele secundare ale tratamentului activ antitumoral. Se abordează ulterior tratamentul principalelor simptome respiratorii (dispneea şi tusea) precum şi problemele psihologice ale pacienţilor cu cancer bronhopulmonar avansat. S-a relevat ideea unei îngrijiri paliative aplicate cât mai devreme în evoluţia pacienţilor, element care a fost demonstrat în studii clinice ca influenţând în mod pozitiv supravieţuirea.Cuvinte Cheie
terapie paliativăcancer bronhopulmonar avansatterapie suportivăPalliative care
Dr. Baulfor Mount coined the term “palliative care” around 1975 to describe his hospice program in Canada, and it has since gained acceptance worldwide.
“The provision of the necessary services for those living with or affected by cancer to meet their informational, emotional, spiritual, social or physical need during their diagnostic treatment or follow-up phases encompassing issues of health promotion and prevention, survivorship, palliation and bereavement... In other words, supportive care is anything one does for the patient that is not aimed directly at curing his disease but rather is focused at helping the patient and family get through the illness in the best possible condition” (Toronto-Bayview Regional Cancer Centre, 1992).
Supportive care
Definition of supportive care: “a term that describes the management of side effects that are caused by chemotherapy and radiation”.
These side effects may be both physical and psychological in nature. Supportive care includes, but is not limited to, the treatment of emesis, nausea, depression, alopecia, oral complications, fatigue, and myelosuppression. These side effects adversely affect the patient’s quality of life and may interfere with ultimate treatment success if the symptoms require significant chemotherapy dose reduction”(O’Neill, What is Supportive Care and why is it important?, J Pediatr Oncol Nurs 2000).
WHO definition of palliative care
Palliative care is an approach that improves the quality of life of patients and their families facing the problem associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual.
Palliative care:
- provides relief from pain and other distressing symptoms;
- affirms life and regards dying as a normal process;
- intends neither to hasten or postpone death;
- integrates the psychological and spiritual aspects of patient care;
- offers a support system to help patients live as actively as possible until death;
- offers a support system to help the family cope during the patients illness and in their own bereavement;
- uses a team approach to address the needs of patients and their families, including bereavement counselling, if indicated;
- will enhance quality of life, and may also positively influence the course of illness;
- is applicable early in the course of illness, in conjunction with other therapies that are intended to prolong life, such as chemotherapy or radiation therapy, and includes those investigations needed to better understand and manage distressing clinical complications.
ESMO-PSCWG
“Supportive care” is defined as care that aims to optimize the comfort, function and social support of the patients and their family at all stages of the illness. This dimension of care emphasizes the oncologist’s role in optimizing quality of life for all patients, including those with potentially curative illness.
“Palliative care” is defined as care that aims to optimize the comfort, function and social support of the patients and their family when cure is not possible. This dimension of care emphasizes the special needs of patients whose illness is either unlikely to be cured or that is incurable. These needs include physical and psychological symptom control, education and optimization of community supports.
“End of life care” is defined as palliative care when death is imminent. Patients who are imminently dying and their families have very special and often intense needs, which commonly require individualized and intensive clinical care (N.I. Cherny, R. Catane, P. Kosmidis and Members of the ESMO Taskforce on Supportive and Palliative Care).
Introduction in palliative care
of lung cancer
Approximately 1.6 million people worldwide are diagnosed with lung cancer annually, of which about 85% of cases are non-small cell lung cancer (NSCLC). With nearly 1.4 million deaths annually, lung cancer is the leading cause of deaths attributable to malignancies.
Locally advanced NSCLC patients have a median survival of 10-17 months.
Patients with metastatic disease have a median survival of only 6-9 months.
Patients with advanced disease often have significant symptoms and reduced quality of life Palliative care, therefore, plays a prominent role in the care and management of patients with advanced NSCLC.
Multiple studies have shown that poor quality of life correlates with shorter survival times among patients with metastatic NSCLC. Despite these findings, palliative care is often administered late in the disease course, a time when intervention is less able to improve patient outcomes or quality of life (Palliative care for patients with locally advanced and metastatic non-small cell lung cancer; http://www.amepc.org/apm/article/view/2650/3722; Charles B. Simone II, Joshua A. Jones).
Early palliative care, symptoms,
and overall survival
Palliative care focuses on symptomatic management and aids patients and their caregivers with psychosocial support and decision making. Interdisciplinary palliative care teams use open communication to focus on patient symptoms and patient and family coping and quality of life in a broad context. Palliative care teams frequently include a combination of physicians, nurses, social workers, nutritionists, physical therapists, occupational therapists, and chaplains (Palliative care for patients with locally advanced and metastatic non-small cell lung cancer; http://www.amepc.org/apm/article/view/2650/3722; Charles B. Simone II, Joshua A. Jones).

Palliative care can be administered concurrently with standard NSCLC treatment modalities used to attempt to prolong life, but the role of palliative care in this capacity has often been limited by physician perceptions that palliative care is an alternative to life-prolonging anti-cancer interventions. As a result, palliative interventions are often initiated when standard NSCLC treatment modalities are no longer deemed beneficial or tolerable. Combining palliative care with standard NSCLC-directed therapies can improve quality of life and patient symptoms and may also lead to improvements in overall survival (Palliative care for patients with locally advanced and metastatic non-small cell lung cancer; http://www.amepc.org/apm/article/view/2650/3722; Charles B. Simone II, Joshua A. Jones).
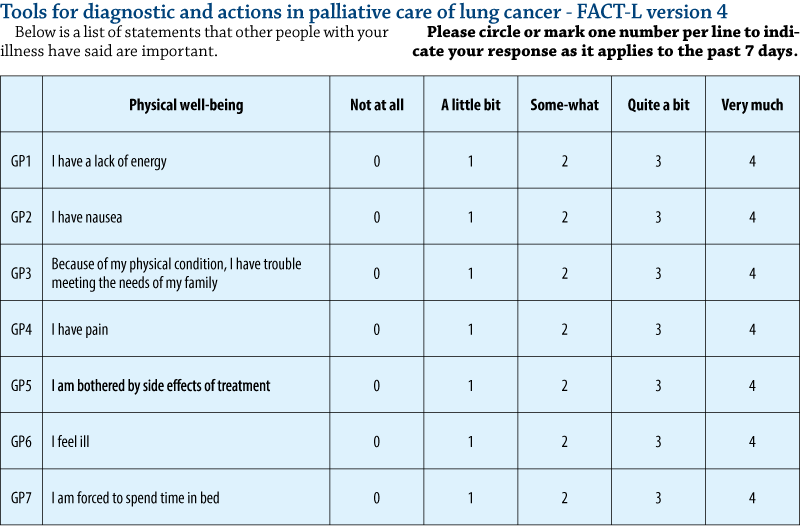
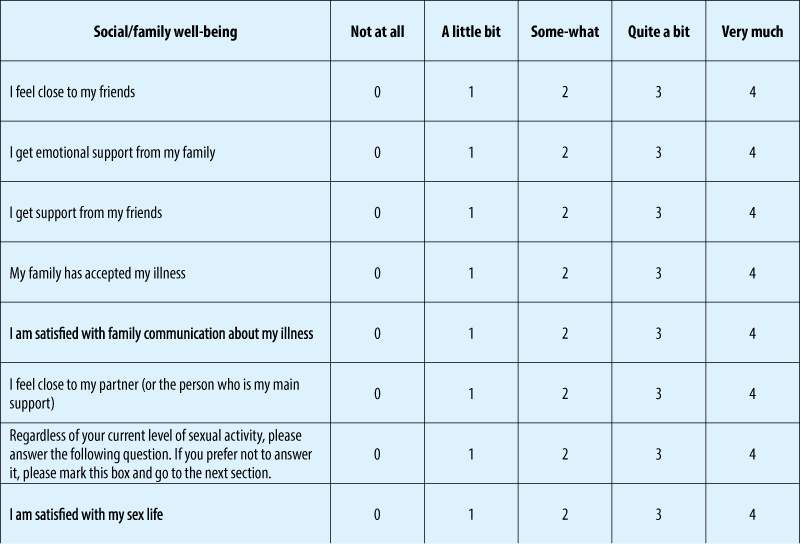
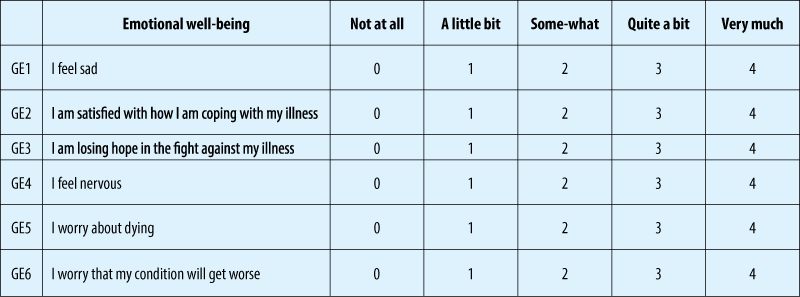
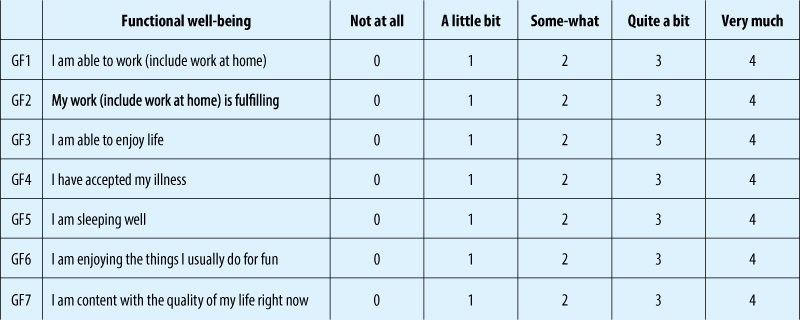
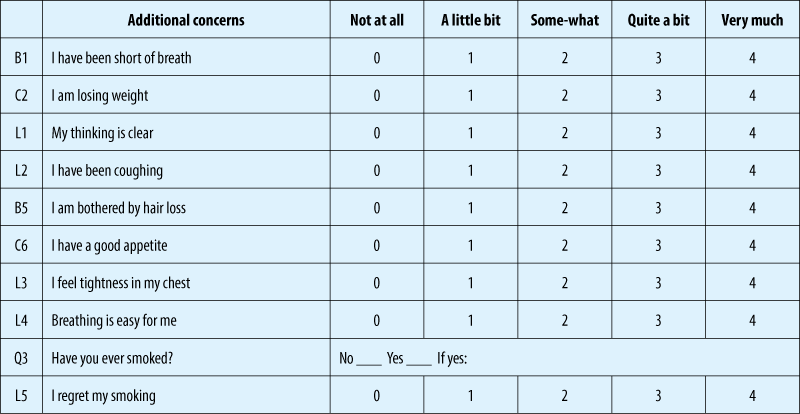
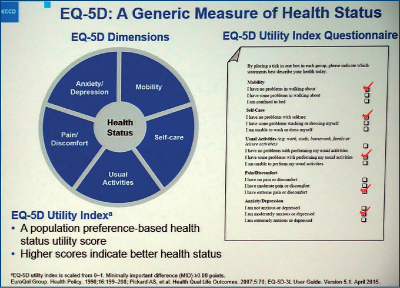
Authors “randomly assigned patients with newly diagnosed metastatic non-small-cell lung cancer to receive either early palliative care integrated with standard oncologic care or standard oncologic care alone. Quality of life and mood were assessed at baseline and at 12 weeks with the use of the Functional Assessment of Cancer Therapy-Lung (FACT-L) scale and the Hospital Anxiety and Depression Scale, respectively. The primary outcome was the change in the quality of life at 12 weeks. Data on end-of-life care were collected from electronic medical records” (Early Palliative Care for Patients with Metastatic Non-Small-Cell Lung Cancer, Jennifer S. Temel, M.D., Joseph A. Greer, Ph.D., Alona Muzikansky, M.A., Emily R. Gallagher, R.N., Sonal Admane, M.B., B.S., M.P.H., Vicki A. Jackson, M.D., M.P.H., Constance M. Dahlin, A.P.N., Craig D. Blinderman, M.D., Juliet Jacobsen, M.D., William F. Pirl, M.D., M.P.H., J. Andrew Billings, M.D., and Thomas J. Lynch, M.D.).
Of the 151 patients who underwent randomization, 27 died by 12 weeks and 107 (86% of the remaining patients) completed assessments. Patients assigned to early palliative care had a better quality of life than did patients assigned to standard care (mean score on the FACT-L scale [in which scores range from 0 to 136, with higher scores indicating better quality of life], 98.0 vs. 91.5; P=0.03). In addition, fewer patients in the palliative care group than in the standard care group had depressive symptoms (16% vs. 38%, P=0.01). Despite the fact that fewer patients in the early palliative care group than in the standard care group received aggressive end-of-life care (33% vs. 54%, P=0.05), median survival was longer among patients receiving early palliative care (11.6 months vs. 8.9 months, P=0.02).
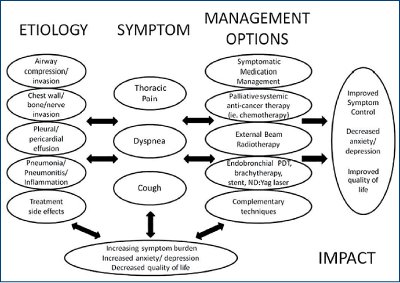
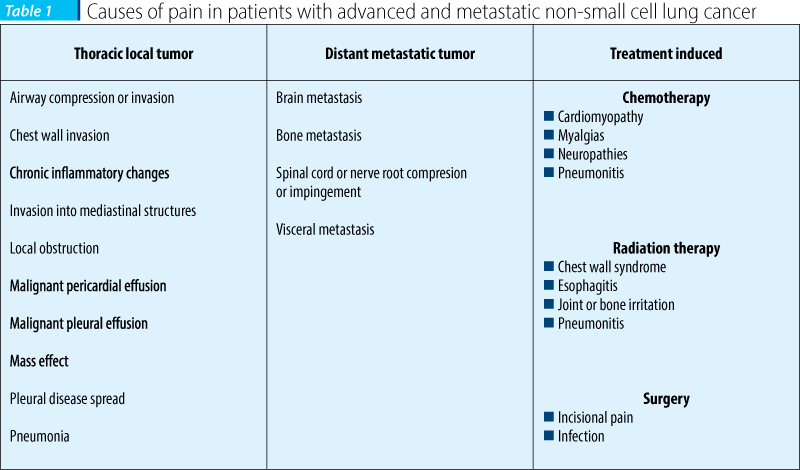
Dyspnea
Patients experience dyspnea as an uncomfortable sensation or awareness of restricted breathing. About 46-90% of patients with NSCLC experience dyspnea.
Dyspnea occurs both from the tumor and therapies used to treat the underlying malignancy.
Palliative management of dyspnea can improve quality of life among NSCLC patients.
Dyspnea can be relieved via palliative procedures or cancer-directed therapies.
Patients with symptomatic tumor invasion or obstruction of the central airway can be considered for endoscopic palliation interventions, including laser therapy, stent placement, and endobronchial brachytherapy.
Symptomatic pleural effusions can be managed with palliative thoracentesis, catheter or chest tube drainage, chemical pleurodesis, or pleurectomy.
Medical interventions, such as bronchodilators, opioids, diuretics, supplemental oxygen, training in breathing techniques, pulmonary rehabilitation, and chest wall vibration, can also improve patient-reported dyspnea (Palliative care for patients with locally advanced and metastatic non-small cell lung cancer, http://www.amepc.org/apm/article/view/2650/3722, Charles B. Simone II, Joshua A. Jones).
Pharmacological management
The evidence base for the pharmacological management of chronic refractory breathlessness is continuing to improve. In this context, chronic is defined as “daily for more than three of the last six months”, and refractory refers to cases where all underlying causes contributing to breathlessness have been assessed as to whether they can be reversed and, if so, whether they should be reversed.
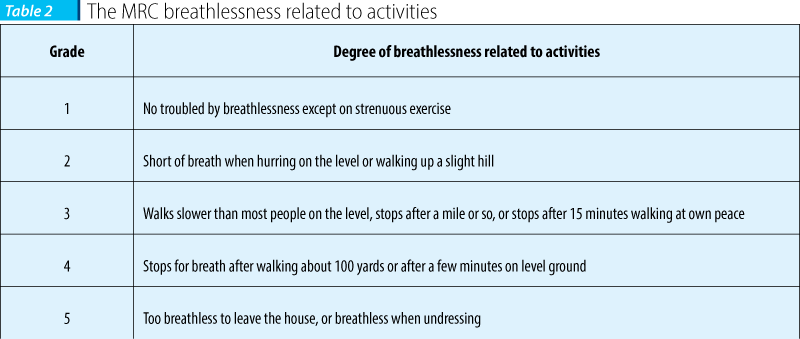
Breathlessness in this case is defined as modified Medical Research Council (mMRC) scale 3 or 4 - breathless at rest or on minimal exertion such as the basic activities of daily living (dressing, bathing or preparing food). It is likely, however, that people with mMRC scale 2 will also benefit from breathlessness interventions. The aim of a therapeutic intervention for this population is to reduce symptomatic breathlessness, as breathlessness will rarely be controlled at all times once chronic irreversible underlying causes of the symptom are established (Supportive and palliative care for lung cancer patients, Patsy Yates, Penelope Schofield, Isabella Zhao, and David Currow, J Thorac Dis. 2013 Oct; 5(Suppl 5): S623–S628; Abernethy AP, Currow DC, Frith P, et al. Randomised, double blind, placebo controlled crossover trial of sustained release morphine for the management of refractory dyspnoea. BMJ 2003;327:523).

Systemic opioids, where morphine has been the most frequently studied medication, are likely to offer the most benefit in the treatment of dyspnea.
Was demonstrated that between 10-30 mg of oral morphine per 24 hours delivered a sustained benefit for two thirds of patients who were started on the medication. The majority of this sample derived benefit from just 10 mg per 24 hours.
A systematic review did not demonstrate benefit from nebulised opioids, despite the wide-spread presence of opioids receptors in the bronchial tree. This potentially was a type II error and may relate to the way in which opioids were nebulised .
However, more recent work suggests that opioids delivered at the alveolar level are likely to help reduce chronic refractory breathlessness.
Other drugs for the treatment of dyspnea
A systematic review suggested that there may be benefits from nebulised furosemide unrelated to a diuretic effect.
The first large study of this has recently been reported and suggests that there may be sustained symptomatic benefit by using nebulised frusemide at a dose of 40 mg/4 mls compared to 4 mls of normal saline. This therapy appeared to be well tolerated.
Of note, the widespread use of benzodiazepines is not supported with current evidence. Although one randomised trial suggested symptomatic benefit was generated more quickly with benzodiazepines in the setting of acute breathlessness where a diagnostic workup was required, the trade-off was increased somnolence.
Non-pharmacological management of dyspnea in lung cancer
Non-invasive ventilation was well tolerated in people with advanced disease, many of whom derived symptomatic benefit at rates greater than those people treated only with oxygen. It is a therapy which will require careful ongoing evaluation in order to understand the net effect that such interventions will deliver to patients with chronic refractory breathlessness in the last days or weeks of life.
Interventions to improve breathing efficiency and interventions targeting the affective component of breathlessness by seeking to reduce anxiety and distress. Interventions to improve breathing efficiency include a range of breathing retraining techniques, with systematic reviews concluding there is good evidence to support the effectiveness of these techniques, including pursed lip breathing, diaphragmatic breathing, “blow-as-you-go”, positioning and pacing techniques.
With regard to the program of exercise to improve dyspnea it seems that further research is required to establish the effect of exercise, especially in the advanced stage of disease, as well as to determine the optimum type and dose of exercise training.
With regard to interventions aiming to reduce distress associated with breathlessness, interventions including relaxation techniques, coping skills training, and general support for patients and their carers have been reported to achieve positive outcomes
Treatment of cough in lung cancer
Cough is a normal but complex physiological mechanism that protects the airways and lungs by removing mucus and foreign matter from the larynx, trachea, and bronchi, and is under both voluntary and involuntary control.
Pathological cough is common in malignant and non-malignant disease. Cough can be classified in various ways, and several causes might coexist in one patient.
- Nonpharmacologic treatment
Nonpharmacologic therapy is directed at the symptom rather than the underlying etiology, and it aims to control rather than eliminate cough: proper positioning reduces coughing secondary to reflux or aspiration.
Saline via nebulizer reduces dryness and irritation of airways.
Chest physiotherapy helps expectorate mucus.
These nonpharmacologic treatments can be used in addition to medications.
- Pharmacologic treatment
Oral drugs: Drugs that suppress cough by modifying the excitability of the afferent receptors in the airways are defined as peripheral antitussive agents.
Central antitussive agents suppress cough by controlling the excitability of neural elements in the brainstem that produce cough.
There is no evidence (i.e., no double-blind trial with an adequate number of patients to have a sufficient statistical power) that cough suppressant therapy can prevent coughing.
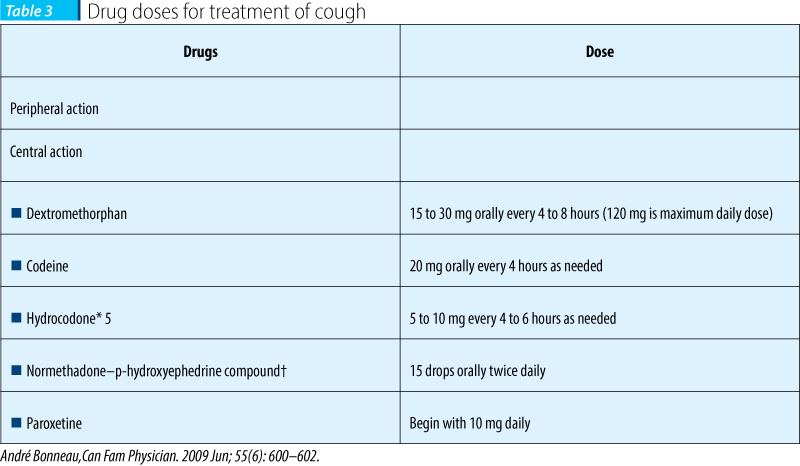
Opioids suppress cough, but there is no scientific evidence allowing comparison of one opioid with another. For those patients already using substantial doses of opioids, one might increase the dose by 20% every 24-hour period, until control of coughing is obtained or side effects become unacceptable. The addition of dextromethorphan to the opioid might have a synergistic effect
Nebulizers: There is very little scientific evidence to support the use of nebulizers in the symptomatic management of patients with breathlessness or cough related to primary or secondary malignancy, or in chronic cardiac, pulmonary, neuromuscular, and neurodegenerative disorders. Doses and schedules have been partly derived from experience in patients with chronic obstructive pulmonary disease (COPD) and from practitioners’ experience.
Nebulizers can be valuable for other symptoms as well. When using nebulizers, patients should be sitting in an upright position of at least 45°.
Interventions to manage psychological distress and unmet needs in lung cancer patients
Despite high levels of distress and perceived unmet need experienced by this group, evidence to inform effective psycho-educational and supportive care interventions for lung cancer patients is scarce.
Available studies of psychosocial and psycho-educational interventions have notable limitations in their design including selection, attrition and reporting bias, small samples, insufficient intervention dose and/or a lack of a suitable control group.
Notwithstanding these limitations, it is highly plausible that psychosocial interventions can reduce distress associated with lung cancer. Such approaches are therefore an important part of a comprehensive management plan for this population, although further research is needed to define the precise nature and scope of these interventions and application in differing patient contexts.
Service delivery models to optimise
outcomes for patients with lung cancer
In recent years, a body of evidence has emerged regarding various health service level interventions that have been designed to achieve optimal outcomes for this group. For example, two studies have investigated post-treatment nurse follow-up versus standard physician follow-up. One three-arm study involved a sample size of 166 people with progressive lung cancer who were randomised to receive a specialised oncology home care program delivered by nurses, a standard home care program delivered by a multidisciplinary team or an office care program delivered by physicians (control group). Participants who received one of the two home-based nurse groups had lower symptom distress, but self-perceived health was also poorer in comparison to the physician follow-up.
Conclusions
Evidence reviews highlight that case management approaches and nurse-led follow-up programs are effective in reducing breathlessness and may be useful in reducing symptom and psychological distress.
Such models also have the potential to positively influence the way health services are used.
Some evidence also exists to support early referral of patients with metastatic lung cancer to palliative care, alongside standard oncology care.
