Comportamentul neurotoxic al medicaţiei antidepresive şi consecinţele clinice: sindromul serotonergic şi sindromul de discontinuitate
Neurotoxic behavior of antidepressant medication and its clinical consequences: serotonergic syndrome and discontinuity syndrome
Abstract
Nowadays, antipsychotic and antidepressant medications are recommended and prescribed for a large variety of psychoorganic syndromes and for other neuropsychiatric clinical conditions. However, not much has been discussed about their neurotoxicity and their consequences on specific brain structures. Certain effects of their neurotoxic impact can mask other neuropsychiatric disorders, and they can be a real challenge and a diagnostic pitfall.Keywords
toxic behaviorantidepressantsantipsychoticssyndromeneuropsychiatryRezumat
În zilele noastre, medicaţia antipsihotică şi antidepresivă este recomandată şi prescrisă pentru un spectru larg de sindroame psihoorganice şi în alte afecţiuni neuropsihiatrice. În ciuda acestui fapt, nu s-a discutat foarte mult despre neurotoxicitatea lor şi despre consecinţele asupra anumitor structuri ale creierului. Unele efecte determinate de impactul neurotoxic pot masca alte afecţiuni neuropsihiatrice şi pot constitui adevărate provocări sau capcane de diagnostic.Cuvinte Cheie
comportament toxicantidepresiveantipsihoticesindromneuropsihiatrieThe behavioral toxicity of antidepressants
Antidepressants are a category of drugs clinically indicated in relieving symptoms of depression, social anxiety disorder, seasonal affective disorder, mild chronic depression, or dysthymia. They are designed to influence, change and modulate the neurochemistry of the brain, in mood and emotional pathology.
Selective serotonin reuptake inhibitors (SSRIs) are some of the most frequently prescribed antidepressants available, used to treat the major depression, mood disorders, sometimes the attention deficit hyperactivity disorder (ADHD), the obsessive-compulsive disorder (OCD), menopause symptomatology, fibromyalgia and neuropathic pain. Those inhibitors are largely used in the treatment of different stages of depression and have less neurotoxic effects. Most antidepressants may have undesirable effects caused by maladaptive neurogenesis, deficient synaptic functionality, poor regulation of glycogenesis, and on neurotransmitter postsynaptic transduction pathways, with a final impact on the neural network in the central nervous system. When deciding and choosing antidepressant medication and its initiation, we must consider two aspects, namely the critical flicker fusion threshold (CFF) and the choice reaction time (CRT). These two pharmacodynamic characteristics are a kind of indicator of the clinical efficacy of both antidepressants and psychotropics(1).
Due primarily to their direct action on the central nervous system, antidepressants may somehow disrupt cognitive function, thus increasing anhedonia, with impaired sexual function by decreasing sexual libido. Sometimes there is a decrease in the ability to think, synthesize and process, and we can even talk about a cognitive toxicity. Also, antidepressant drugs and psychotropic drugs cause changes in the behavior of patients(2). The metabolism of antidepressants is a very important aspect, as well.
If the medication is taken orally, it will respect the classical pathway: small and large intestine, liver, bloodstream. Once it has entered the bloodstream, the active compound molecule will interact with various cellular effectors (proteins, receptors, fatty acids), an interaction which will affect the distribution. From the hepatocellular point of view, through a demethylation cycle, the half-life of antidepressants is longer than normal, justifying their slow inactivation and elimination(3).
The neurochemistry of antidepressants’ metabolism in certain areas of the brain is an extremely complex process that will influence both the success or the failure of treatment, and the worsening or improvement of the symptoms. The involvement of cellular and molecular mechanisms at the level of neural metabolic signaling cascades in case of antidepressants often involves brain structures such as: frontal, temporal, occipital, parietal cortex, cerebellum, thalamus with neurochemical effectors such as G proteins, adenylyl cyclase, protein kinases, protein cyclase, kinase activation receptors, and phosphoinositide. Besides these, the metabolism of antidepressants at the neuronal level involves structures such as: cortex, limbic cortex, amygdala, hippocampus, with molecular components such as ATP, glucose and inositol, sensitive to the action of pharmacological agents such as fluoxetine, imipramine, moclobemide, paroxetine, sertraline and tranylcypromine. Decreased cognitive function and neuromotor disorders have been observed in depressed elderly with chronic antidepressant medication. For example, tricyclic antidepressants cause a certain impairment of cognitive and motor function, and that is not only due to sedation. Antidepressants that do not affect these functions are those with a relatively unsaturated profile and those that inhibit serotonin reuptake(4). Comparative studies have been conducted on the psychopharmacological profiles of several selective serotonin reuptake inhibitors, and their neurotoxicity contrasted with both the placebo effect and the tricyclic antidepressants dothiepin and amitriptyline(5). New-generation antidepressants, such as escitalopram and mirtazapine, are preferred by most clinical guidelines(6,7,8), but very few clinical trials have been performed to demonstrate their effects on cognition and neuromotor function. Also, from the experience of some psychiatric clinics, it has been observed that escitalopram and mirtazapine improve the psychomotor function of patients with endogenous depression, while amitriptyline deteriorates it, therefore in clinical practice escitalopram and mirtazapine are preferred to amitriptyline.
The neurotoxic effects with neuropsychiatric consequences in the case of antidepressants have led to the description of two distinct clinical entities. The first one is serotonergic syndrome, which occurs if only one type of serotonin reuptake inhibitor is chosen, may/may not be installed until the optimal dose is established, and may occur from overdose and/or administration of two serotonergic drugs simultaneously.
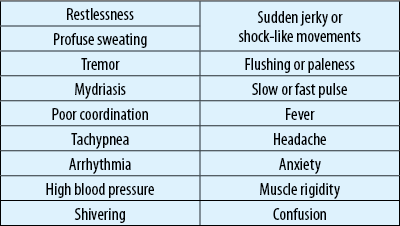
The symptoms of serotonin syndrome can be mild to severe, revealing anything from a slight serotonin excess to a life-threatening syndrome. The most common symptoms include(9):
The discontinuation syndrome (antidepressant discontinuation syndrome) – or antidepressant withdrawal syndrome – is a psychiatric condition that can appear following the uncontrolled stoppage, reduction or interruption of antidepressant medication. The symptoms are equivocal and fluctuating, including flu-like symptoms, gastrointestinal symptoms (nausea), sensory disturbances, affective symptoms, mood balance problems and sleep disturbance(10). Discontinuation symptoms can be confused with the recurrence of the underlying psychiatric illness and might also be misdiagnosed. This syndrome needs to be distinguished from relapse. Due to a lack of specific clinical protocols, the management and prevention of this syndrome need to be personalized for each patient, according to severity and clinical condition.The serotonergic syndrome, if well individualized and controlled, does not cause any problems. Once the neuronal serotonin levels have returned to normal, there is no risk of worsening. If the dose is played with, if the patient is not strictly supervised when administering the medication, then serious unwanted problems – such as hyperpyrexia, arrhythmias unconsciousness and even death – may occur.
Onset and duration: generally, on the first week, but evidence studies suggest a mean time of onset of two days after stopping. A spontaneous resolution between two days and three weeks after onset was reported.
Prevention and management of antidepressant discontinuation syndrome(11,12)
Tapering may not be necessary for patients taking an antidepressant for less than four weeks or for those who are substituted with fluoxetine.
-
Tapering at a slow rate.
-
Antidepressants with short half-life need to be reduced progressively; however, progressive tapering may not preclude the syndrome onset in all patients.
-
Providing patients assurance.
Conclusions
The clinical and pharmacological profile of the antidepressants therapy neurotoxicity and its clinical consequences need to be emphasized, taking into account that depression is a common mental disorder, a recurrent pathology with a self-induced vulnerability and that, globally, more than 264 million people of all ages suffer from depression. The neurotoxic syndromes were briefly explained, suggesting, among other things, that the choice, initiation, continuation, interruption and stopping of the antidepressant therapy contribute fundamentally both to the quality and effectiveness of treatment, and to the patient’s quality of life. Neurotoxicity hypothesis of depressive disorder, apart from allowing a different strategy of communicating with our patients and to facilitate their compliance, plays an important role in treatment adhesion. n
Bibliografie
- Hindmarch I, Alford C, Barwell F, Kerr JS. Measuring the side effects of psychotropics: the behavioral toxicity of antidepressants. J Psychopharmacol. 1992; (2)198-203.
- Hindmarch I. Cognitive toxicity of pharmacotherapeutic agents used in social anxiety disorder. The International Journal of Clinical Practice. 2009 Jul; Vol. 63, Issue 7, 1085-1094.
- Undurraga J, Baldessarini RJ. Direct comparison of tricyclic and serotonin-reuptake inhibitor antidepressants in randomized head-to-head trials in acute major depression: Systematic review and meta-analysis. J Psychopharmacol. 2019; (9):1184-1189.
- Lane RM, O’Hanlon JF. Cognitive and psychomotor effects of antidepressants with emphasis on selective serotonin reuptake inhibitors and the depressed elderly patient. German Journal of Psychiatry. 1999; 1, 1–42.
- Hill LL, Lauzon VL, Winbrock EL, Li G, Chihuri S, Lee KC. Depression, antidepressants and driving safety. Injury Epidemiology. 2017 Dec; 4(1):10.
- Davidson JR. Major depressive disorder treatment guidelines in America and Europe. J Clin Psychiatry. 2010; 71 Suppl E1:e0.
- Lam RW, Kennedy SH, Grigoriadis S, McIntyre RS, Milev R, Ramasubbu R, et al. Canadian network for mood and anxiety treatments (CANMAT) clinical guidelines for the management of major depressive disorder in adults. III. Pharmacotherapy. J Affect Disord. 2009; 117 Suppl 1: S26.
- Anderson IM, Ferrier IN, Baldwin RC, Cowen PJ, Howard L, Lewis G, et al. Evidence-based guidelines for treating depressive disorders with antidepressants: A revision of the 2000 British Association for Psychopharmacology Guidelines. J Psychopharmacology. 2008; 22:343-96.
- Foong AL, Grindrod KA, Patel T, Kellar J. Demystifying serotonin syndrome (or serotonin toxicity). Can Fam Physician. 2018; 64(10):720-727.
- Berber MJ. FINISH: remembering the discontinuation syndrome. Flu-like symptoms, insomnia, nausea, imbalance, sensory disturbances, and hyperarousal (anxiety/agitation). J Clin Psychiatry. 1998; 59:255.
- Fava GA, Gatti A, Belaise C, et al. Withdrawal symptoms after selective serotonin reuptake inhibitor discontinuation: a systematic review. Psychother Psychosom. 2015; 84:72–81.
- Ogle NR, Akkerman S. Guidance for the discontinuation or switching of antidepressant therapies in adults. J Pharm Pract. 2013; 26:389–96.





