Terapia comportamentală în stomatologia pediatrică. Tehnici nefarmacologice de management comportamental
Child behavior management technology in pediatric dentistry. Review of non-pharmacological techniques
Abstract
The dental treatment can easily lead to strong reactions of fear and acute anxiety in adults and children alike. It is one of the most common reasons for avoiding the dental office and for neglecting orodental problems. Dental anxiety has been shown to increase the incidence of dental pathology (decayed and/or extracted teeth), increase the frequency and intensity of episodes of dental pain, and reduce the overall quality of oral health. Dental disorders can not only have significant physical consequences for the child, such as disturbed sleep, reduced food intake, digestive disorders, delayed growth and development, but can also affect their mental concentration, which leads to decreased school performance; social interactions can also be adversely affected. Pain, previous unpleasant experiences with dentists or less trained dentists can be serious reasons why the child is afraid, developing phobias that can follow him for a lifetime. To gain their trust and help them escape the fear of the dental office, children always need to be treated by a calm, warm, patient doctor who can understand their fears and explain, step by step, what is going on. Behavior management is widely accepted as a key factor in providing oral and dental care to children. It is imperative that any behavioral approach of the pediatric patient be based on empathy and concern for the physical and mental well-being of each child. A wide variety of behavioral management techniques (pharmacological and non-pharmacological) are available to pediatric dentists. It is important to choose the right one for the benefit of each child patient, depending on the individual’s physical and mental characteristics in each case.Keywords
behavior managementpediatric dentistrychild behaviordental anxietyRezumat
Vizitarea medicului stomatolog poate provoca cu uşurinţă reacţii puternice de teamă şi anxietate acută la adulţi şi copii, deopotrivă. Acesta este unul dintre motivele cele mai frecvente pentru evitarea cabinetului stomatologic şi neglijarea problemelor orodentare. Anxietatea dentară s-a dovedit a duce la creşterea incidenţei patologiei dentare (dinţi cariaţi şi/sau extraşi), la creşterea frecvenţei şi intensităţii episoadelor de durere dentară şi la o reducere globală a calităţii sănătăţii orale. Afecţiunile dentare pot avea nu numai consecinţe fizice notabile pentru copil, cum ar fi somnul agitat, reducerea aportului de alimente, tulburări digestive, creşterea şi dezvoltarea întârziată, dar pot afecta şi concentrarea acestuia, ceea ce conduce la scăderea performanţei şcolare; interacţiunile sociale pot fi, de asemenea, afectate negativ. Durerea, experienţele neplăcute anterioare în cabinete de stomatologie sau medici stomatologi mai puţin instruiţi pot reprezenta motive serioase pentru care copilului îi este teamă, dezvoltând fobii care îl pot urmări o viaţă întreagă. Pentru a le câştiga încrederea şi pentru a-i ajuta să scape de frica de cabinetul stomatologic, copiii au întotdeauna nevoie să fie trataţi de un medic calm, cald, răbdător, care să le înţeleagă temerile şi care să le explice pas cu pas ce se petrece. Managementul comportamentului este larg acceptat a fi un factor-cheie în acordarea îngrijirii orodentare la copii. Într-adevăr, dacă ghidarea comportamentală a copilului în cabinetul stomatologic eşuează, atunci este dificil, dacă nu chiar imposibil, de realizat îngrijirea dentară de care este nevoie. Este imperativ ca orice abordare comportamentală a pacientului pediatric să aibă ca bază empatia şi preocuparea pentru bunăstarea fizică şi psihică a fiecărui copil. Medicii stomatologi pediatri au la dispoziţie o mare varietate de tehnici de management comportamental (farmacologice şi nefarmacologice), fiind importantă alegerea celei adecvate pentru beneficiul fiecărui copil pacient, în funcţie de particularităţile fizice şi psihice individuale, şi care, important, trebuie să ia în considerare şi exigenţele de natură culturală, socială sau educaţională, precum şi cerinţele legale în vigoare pentru fiecare caz în parte.Cuvinte Cheie
ghidare comportamentalăstomatologie pediatricăanxietate dentarăIntroduction
The child is a special patient, and the dental visit is an event in which the child cannot be engaged without a specific approach to his age, personality and dental experience. Modern dentistry pursues a multidisciplinary approach to small patients(1,2). Our goal and intervention are to positively stimulate the perception at the entrance to the office, regardless of the emotional load that the patient comes with.
Dental anxiety. Dentophobia
Dental practice is related to pain and, although pain is the symptom that brings the patient to the dentist’s office, it is also the one that keeps him apart from it. The dental treatment can easily lead to strong reactions of fear and acute anxiety in adults and children alike. It is one of the most common reasons for avoiding the dental office and neglecting orodental problems. The patient is primarily afraid of pain, the pain being an experience that each person experiences more or less frequently, with greater or lesser intensity. Pain, previous unpleasant experiences in dentists or less trained dentists can be serious reasons why the child is afraid, developing phobias that can follow him for a lifetime.
Odontophobia can appear from the childhood, following traumatic experiences, strengthening from year to year and producing a vicious circle. Dental anxiety has been shown to increase the incidence of dental pathology (decayed and/or extracted teeth), increase the frequency and intensity of episodes of dental pain, and reduce the overall quality of oral health.
According to Chadwick and Hosey(3), anxiety is familiar in children and the symptoms of anxiety depend on the age of the child. Toddlers reveal anxiety by crying, while grown-up children express anxiety in other ways. Common anxieties among kids include fearing the mysterious and being worried regarding a lack of management, both of which can happen with dental assessment and treatment. The capability of a child to deal with dental procedures depends on his/her phase of development.
Although the visit to the dentist still arouses great emotions in many patients, in recent years there has been more and more progress in this regard, with dental clinics trying a new approach to working with patients, especially with children. Distinctive emphasis is placed on psychodontics, which explores the patients’ psychobehavioral resources in order to define a set of strategies designed to increase their tolerance for dental treatment, and on child psychology, from which dentistry can take psychotherapeutic concepts and techniques for the correction of fear-dominated behavior, uncooperative, in children.
Encouraging a supportive attitude toward the dental visit will help your child or adolescent overcome his fears and prevent further adult anxiety.
What is behavior management?
Absolutely unintentionally, towards the end of the 19th century, Mc Elroy(4) formulated a definition of this concept. She wrote: “although the operative dentistry may be perfect, the appointment is a failure if the child departs in tears”. It was the first time in the literature that the assessment of failure or success in treating children was made on criteria other than those strictly technical.
Behavior management or behavioral guidance of the child, as this concept is also called, generally refers to the means used in the dental treatment of the child in order to obtain his acceptance and compliance. Given the frequent use of these terms, it is surprising that a clear definition of the concept was not formulated until 1975, when Wright(5) formulated the first clear definition of the concept of behavioral management, thus: “the means by which the dental health team effectively and efficiently performs treatment for a child patient and at the same time instills a positive dental attitude”.
Wright suggested that the purpose of the behavior management is getting a “positive dental attitude”, and subsequently clearly defined the concept(6). The goal is not to model behavior strictly in the interest of successfully completing a therapeutic act, but also to create an attitude, a long-term concern on the part of the patient for the continuous prevention and improvement of oral status in the future. In fulfilling this goal, the dentist’s relationship with the child and the accompanying adult must be based on trust and cooperation (the so-called “treatment alliance”(7)); in this way, compliance with preventive measures is ensured and the treatment will be carried out in optimal conditions.
Since the introduction of this definition, the American Academy of Pediatric Dentistry (AAPD) guidelines have stated: “The goals of behavior guidance are to establish communication, alleviate fear and anxiety, deliver quality dental care, build a trusting relationship between dentist and child, and promote the child’s positive attitude toward oral/dental health and oral health care.”(8,9)
According to the AAPD(9), the main goals of behavior management are to:
-
Establish communication and cooperation with the child and parent.
-
Reducing fear and relieving dental anxiety.
-
Ensuring quality dental treatments in safe conditions.
-
Build, between the dentist, child and parent, a relationship based on trust.
-
Promote the child’s positive long-term attitude toward oral healthcare.
Classifying children’s behavior
Children go to their dentist geared up with a found out set of behaviors which have efficiently helped them to address different hard or tension-inducing situations, and they will certainly use those coping techniques within the dental setting. Some of their techniques could be beneficial, while others will make it more difficult to supply nice dental care. The purpose is to construct and hold relationships with the child and figure out which is the right method to allow the best dentistry to be delivered. It is likewise important to assist every baby to expand the capabilities and behaviors vital to willingly search for suitable life of dental care, now no longer hindered through undue tension or fear(10).
Numerous structures were advanced for classifying children’s conduct within the dental environment. Interestingly, maximum class structures which are utilized in medical exercise these days had been spawned from studies investigations(11).
When a clinician treats a toddler patient, the primary problem of subject is the kid’s behavior. There is a huge variation among class structures. One of the first were defined by Wilson(12), who indexed four trainings of behavior: every day or bold, bashful or timid, hysterical, and rebellious. This device recognized behaviors at some stage in dental strategies that specifically constrained the achievement of remedy. Nowadays, class structures are frequently primarily based totally on standards utilized in mental questionnaires. Child behaviors at some stage in daily, non-dental conditions can be categorized into classes that summarize the persona of the child(13). When we refer to the child's personality, we have in mind his general character traits, unrelated to a medical act.
One of the most broadly used system belongs to Frankl et al., in 1962(14). It is known as the Frankl Behavioral Rating Scale. The scale divides the conduct into four categories, starting from absolutely advantageous/positive to absolutely negative.
Categories of behavior (the Frankl Behavior Rating Scale)
Rating 1. Absolutely negative: refusal of treatment, crying forcefully, fearfulness, or some other overt proof of excessive negativism.
Rating 2. Negative: reluctance to just accept treatment, uncooperative behavior, a few proof of a poor mindset, however now no longer pronounced (i.e., sullen, withdrawn).
Rating 3. Positive: acceptance of treatment, at instances cautious, willingness to conform with the dentist, at instances with reservation, however following the dentist’s directions cooperatively.
Rating 4. Absolutely advantageous/positive: good rapport with the dentist, interested by the dental procedures, guffawing and playing the situation.
The Frankl classification method, as seen above, is often considered the gold standard in clinical rating scales, mainly due to its wide usage and acceptance in pediatric dentistry.
Children have a limited ability to communicate and have real difficulty expressing themselves fears and/or anxiety. Their behavior is essentially the image of their inability to control their anxiety, which they feel they cannot cope with; therefore, they try to avoid an imminent situation that triggers fears. The subsequent change in behavior should be perceived as a form of manifestation of anxiety or the discomfort of a child facing an imminent event, which he has no other way to deal with. Behavior management aims to create strategies and means of communication and adaptation for children specific to their age(3).
More or less consciously, most clinicians place children in one of the following three categories(5):
1. cooperative
2. lacking in cooperative ability, or
3. potentially cooperative.
Knowing the clinical aspects of these distinctive child behaviors is important to behavior management and treatment planning.
Children who, in the past, have gone through a negative experience, even a singular, isolated one, in the dental office, are included in the category of the “uncooperative”; the child is intentionally difficult or uncontrollable, which, in practice, is extremely rare(3).
Cooperative behavior
Once in dentist’s office, most children cooperate(15). Cooperative children are relaxed, have a minimum degree of anxiety; sometimes, they can be enthusiastic. This category of children offered a “affordable level” of cooperation, which lets in the dentist to treat efficaciously and efficiently. They seldom require pharmacologic adjuncts to assist accomplish their treatments(11).
Lacking cooperative ability
Unlike the cooperating child, some children lack the ability to cooperate. This group may include very young children (under 3 years old) with whom they cannot communicate, not having the ability to understand. The agreement cannot be expected from them.
They can raise major behavioral issues if their treatment needs are urgent. In most cases, their treatment involves the combination of pharmacological adjuvants. McDonald’s(16) referred to these children as being in the pre-cooperation phase, in the sense that time solves, for the most part, the behavioral problems, as they grow up, they become cooperating patients.
Children with specific debilitating or disabling conditions are another category of pediatric patients who lack the ability to cooperate. In this group of children, additional data on their intellectual development can provide the dentist with information that helps predict the level of cooperation. During therapeutic maneuvers, no major behavioral changes were expected in a positive sense(11).
Potentially cooperative behavior
The potentially cooperating child was listed, until recently, as one with behavioral problems, regardless of whether he was healthy or disabled. The potentially cooperating child has the ability to behave appropriately; it is an important distinction from one who does not have this ability. Once characterized as a potential cooperator, the reasoning indicates that there is a possibility of changing the behavior of such a child who has cognitive abilities, appropriate to age, to be guided behaviorally to deal with dentistry and can become cooperative. The term “potentially cooperative”, as described above, is preferred to the ambiguous term “noncooperative”(3).
The principle that children are miniature adults is completely wrong! Therefore, understanding the child’s development is essential for the effective application of behavior management techniques, which must be adapted and applied differentiated, for each child, according to his abilities of cooperation and understanding.
Factors underlying children’s cooperation
Why do children vary so much in their responses to dentistry?
Behavioral modeling and guidance are the keys to therapeutic success. While some children are balanced and tolerant of stressful situations and are unlikely to engage in uncooperative behavior, others are more vulnerable and may need more attention, patience and time to feel comfortable for cooperating with the doctor during their dental treatment. The challenge is to identify these vulnerable children and, subsequently, the factors that could influence their behavior in the dental office. It goes without saying that an anxious child, faced with an event that he anticipates as an unpleasant experience, is more likely to have such an experience, while a child with a low level of fear or anxiety is expected to perceive the visit to the dental office as a pleasant experience(11).
Behavioral reactions in situations can be conditioned by internal factors that have their origin in chronic fear and anxiety. Anxiety, as a mental state, is a personality trait, but there are several factors in the presence of which there has been an increase in the likelihood of behavioral disorders during dental appointments or other stressful situations.
On the other hand, child behavior is influenced by parenting styles, general health, pathology, culture, social expectations and temperament(17). Sometimes, the behavioral reactions may be due to factors related to the child’s perception of the dental office or previous unpleasant medical experiences. These are called external factors. If the initial interrogation, at the time of the first meeting with the patient, is conducted logically and the questions are appropriate, the child’s history may reveal important external factors, some of them listed below.
Medical history
Children who had unpleasant experiences in association with medical treatment may be more concerned during the dental procedures(18-20). Similarly, worry sustained from previous dental visits has additionally been associated with a bad behavior at next visits(19-21). The dentist needs to encompass, during the compilation of the child’s medical history, questions on previous hospital/scientific contact/remedies and the kid’s reactions to them.
Parental anxiety
A correspondence between maternal tension and problems in infants’ affected person control at every age has been proven(18-20,22-24), and this is in particular critical for children younger than 4 years old(18,19). When an adult is not able to incorporate his personal dental anxieties, he can also additionally boom the kid’s personal tension; in such instances, it can be helpful to find an alternate adult who’s much less apprehensive(22). Parents also are capable of appropriately predict the possible behavior in their children(23,25). The infant who gets an extremely good deal of interest from a worried parent while he/she cries is possibly to be strengthened by concern and, accordingly, be much more likely to cry at the following visit. Likewise, if the kid is being treated in the presence of a very anxious parent, then the social learning theory of modelling/vicarious conditioning can explain why he can also become anxious(26).
Awareness of a dental trouble
Children who realize they have got a dental trouble are much more likely to show off negative behavior at the primary dental appointment(18,19). Dental fear has been shown to be the major predictor of dental behavior management problems (DBMP), and temperamental reactivity (i.e., frustration, anger, shyness) has also been shown to play a large role in DBMP with child and adolescent patients(27).
Parental influences on child dental behavior
A balanced and warm familiar environment is vital to an infant’s nurturing and development. An infant’s experience of self-worth develops from being cared for, loved and valued. Along with assembly primary bodily desires, households offer youngsters with emotional help, socialization, coping techniques and other life capabilities.
Families impact children’s dental status in everyday lifestyles through ingesting behaviors and oral hygiene practices. Parents determine the moment when their children ought to see a dentist, pick out the workplace or health facility and dentist, set up the visit, and regularly accompany their kids to the appointments. Before getting into the dental workplace, the parents have invested withinside highly satisfactorily in their infant’s dental experience.
The familiar environment serves as the kid’s connection to the entire world and has a vital function in making ready an infant for lifestyles out of doors of the domestic. Socialization, the manner with the aid of using which a man or woman learns and accepts the set-up methods of a specific social institution or society, can be considered as the “nurture of nature”, wherein the own circle of relatives transmits cultural values, expectancies and behavioral requirements to the child. Socialization can also decide an infant’s reaction in dental office. It can impact conduct requirements, mindset closer to grownup authority, how pain justifies complaint, and the way to explicit distress(28).
Education, through the influence of parental influences, plays a major role in how a child manages stress and reactions during dental treatment(29). There seems to be a consensus in the literature that stress tolerance and children’s coping skills are best when there is a structured family environment, parents are receptive and confident, set boundaries and offers adequate rewards, but also appropriate punishments, in order to stimulate or discourage a certain way of reaction of the child(30-32).
Parenting patterns have modified in recent decades. Dentists are confronted with demanding situations from the growing wide variety of children who in a number of instances are ill informed regarding the capabilities and willpower vital to cope with novel stories within the dental workplace. Commonly, parental expectancies for the kid’s behavior (e.g., no tears) are impracticable, though the expectancies for the dentist who steer their conduct are enormous. Some parents can also, additionally, even try to dictate remedy, although their understanding of the technique is lacking. Effective conversation with extra difficult parents represents a danger for the dentist to chose carefully over conduct and remedy alternatives and collectively decide on what’s in the infant’s best interests.
Each practitioner has the responsibility to set up the conversation and help techniques that quality optimize the remedy setting, figuring out his/her personal capabilities, the functionality of the child, and the specific needs of the concrete procedure(33-37).
Each dentist who treats children will have to decide for himself whether the presence of an adult during treatment will have a beneficial impact or not. In recent years, it has been noted that parents have a greater desire to be actively involved in all aspects of their children’s lives(38) , with an increased reluctance to allow another responsible adult to guide their own child’s behavior. Provided that the presence or absence of parents is significantly influenced by the management capacity of the dentist, it can be used as a behavior management strategy(39-41).
Research indicates that children’s behavior is unaffected with the aid of using parental presence or absence(7,39). The exception is younger kids (much less than 4 years old) who behave better in their mom’s presence(7). Thus, for younger children, parental presence is critical, while for older children, parental presence seems now no longer to have this sort of clean impact on infant behavior, however can be critical to the adult accompanying the child. What is crucial is that dental practitioners provide an explanation for their exercise regulations on parental presence to the parents(3).
The dental crew. The pediatric dentistry triangle
The whole crew has an active challenge to play. First, get in contact with the receptionist, who can relieve parental worries with an assured technique; the chairside assistant can deliver a useful function in helping the dentist in dealing with behavior issues; the dental hygienist can give schooling through the right conversation with the child and parent, and be capable of assisting the relatives for preventing future dental disease(10). An infant’s future approach closer to dentistry can be decided with the aid of using a chain of taking place stories in nice dental surroundings. The entire dental crew contributors are endorsed to extend their capabilities and attention in behavior guidance strategies with the aid of using evaluation dental literature, tracking video pre-sensations or attending systematic education courses(33,42).
The ones provided to date have as a place to begin and medical basis the idea of the pediatric dentistry triangle, mentioned for the first time in 1975 by Wright(5). It isn’t viable to view many single points of this triangle in isolation. The infant is on the apex of the triangle and is the focal point of interest of both the family and the dental crew. The strains of conversation emanating from the dentist’s angle emphasize a major distinction among children’s dentistry and adult’s dentistry. These strains display that treating kids as a minimum 1:2 courting (i.e., dentist: infant and adult). Adult dentistry has a tendency to be a 1:1 situation (i.e., dentist: the affected person). It is extraordinarily critical for all dental employees to speak in both directions. The arrows suggest that the conversation is reciprocal. They additionally symbolize that the dental remedy of the child affected is a dynamic connection among the corners of the triangle – the kid, the family, and the dentist.
Societal rules influence all corners of the triangle individually, in addition to the interactions among all three components. The close connection among adult and infant has been modified with the aid of using society. The expert relationships among dentist and infant and dentist and parent have additionally evolved, dictated with the aid of using societal changes. In 1975, it turned into broadly widely widespread that a mother’s mindset extensively affected her offspring’s conduct within the dental workplace.
Roles in households are converting and now the whole familial environment surroundings ought to be considered. A father bringing an infant for treatment isn’t unusual. Not infrequently, each father and mother are working, and the child offers on the dental workplace with a caregiver. Hence, the brand new triangular example acknowledges the alternate that has took place within the last forty years(11).
Once there is information of the underlying elements that could impact an infant’s attitude, a remedy plan may be developed. Some infants may need extra time in making ready them for what’s to come, mainly those with chronic fears and anxieties. Patients with competitive behaviors can also additionally need actions certainly defined and an exceptionally established technique for the duration of their dental visits. Understanding the kid’s desires in remedy making plans ought to decorate the opportunity of a success outcome(11).
Behavioral management techniques
Since each baby is one of a kind, pediatric dentists have an extensive variety of approaches to assist a baby for dental treatment. A pediatric dentist recommends conduct steering techniques for the child primarily based totally upon their history, unique healthcare wishes, dental wishes, the types of remedy required, the results of no remedy, their emotional and highbrow improvement, the mother’s and father’s options, and the dentist’s options and abilities.
The AAPD Clinical Guideline on Behavior Management defines the techniques currently used in the management of children in contemporary pediatric dentistry. It outlines the objectives, indications and contraindications for each of the techniques approved by the AAPD, as documented in the dental literature and reflected in the professional standards. The guideline has divided the techniques into two categories: basic behavior guidance and advanced behavior guidance.
The simple behavior steering consists of conversation and communicative guidance, tell-show-do, voice control, nonverbal communication, positive reinforcement, distraction, parental presence/absence, nitrous oxide/oxygen inhalation. Less cooperative children can be managed by more advanced behavior guidance techniques, which include protective stabilization (active and passive restraint), sedation and general anesthesia(9).
Only non-pharmacological behavioral management techniques are the subject of this presentation; their popularity and degree of acceptance vary within wide limits but, overall, they are the ones that should be the rule, the pharmacological techniques being reserved only for particular cases.
Behavior management techniques are not all equally accepted by parents(43). Several studies of parental acceptance of behavior guidance techniques used in pediatric dentistry show different views of parental attitudes. Parental attitudes are constantly changing as society, so it is important to regularly reassess their beliefs and update our understanding of their attitudes toward behavior management techniques. As a result, the selection of the behavior management techniques to be used is no longer made largely by the dentist but, rather, with the active involvement and consent of the parents(44,45).
Therefore, effective communication is crucial and affords the possibility to carefully work together and pick the best remedy technique to make the child’s visit as safe and comfortable as possible. Communication is the most important method of behavioral treatment that aims to change the child’s attitude towards dental treatment. It is a form of psychological treatment that is carried out through the educational process and offers real advantages compared to pharmacological or coercive methods.
Recommendations for the choice of behavior management techniques
Because working with children involves additional precautions compared to working with an adult, pediatric dentists need to master a variety of techniques and approaches at their disposal to deal effectively with the many situations and reactions they may experience. For each child’s behavior there will be a response method of the doctor meant to help the child to adapt to the dental experience in a positive way; at the same time, the physician must possess the ability to model his or her own behavior in order to respond to the individual needs of the child patient. Some of the behavior modeling methods aim to improve the communication process, others are meant to limit inappropriate behavior or reduce anxiety. Therefore, the dentist must pay attention to the level of understanding(46) of each child, stage or development(47) and to any possible special conditions (disability or sensory deprivation), when deciding which communication technique to adopt.
In 2-years-old children, whose ability to understand the language of others (receptive language) is far more developed than the ability to be understood by others (expressive language), explanations of the dental act should be short, using words simple or euphemisms. Affirmative rather than interrogative sentences are used (e.g., “Let’s ride the elevator chair!” is better than saying “Would you like to ride the elevator chair?”; “No” rather than “Yes” if he is afraid). In 3-year-olds, expressive language is more varied, some children may have a simple discussion, and others are limited to short sentences. Their receptive language develops further, so that at this age more detailed explanations of the dental procedure can be given. In 4-year-olds, the receptive language is well developed, and the expressive language is quite developed and, therefore, the child should not be treated as if he is not present or does not understand but will have to be trained in discussion using age-appropriate words. At a young age (3-4 years old), children have short-term attention, they get bored quickly and, therefore, it is recommended that behavioral, prophylactic and curative treatment sessions be as short as possible. Five years of age and older children understand the language of others and are understood through the language by others and may, therefore, become more and more involved in adult conversation; the ability to socialize and understand the importance of the rules is increasing, a skill that is very useful in dental treatment; however, it is necessary to keep the treatment sessions as short as possible.
It is recognized that, although there is a fairly wide variety of management techniques, they are rarely used in isolation; for example, say-show-do, a basic desensitization technique, is almost always immediately followed by a form of praise (reinforcement). At the same time, regardless of the technique used, its effectiveness will vary within extremely wide limits depending on the concrete way of its application, as well as, not to be neglected, the empathic reaction ability proven by the dentist(10).
Parental consent should be obtained for all behavior management techniques; it’s also essential to make certain that the accompanying adult is aware of what techniques you are likely to undertake and that he is prepared. If they understand that you can increase your voice under certain circumstances (voice manage) and why, they may react correctly must it occur(3). Techniques that are used to discourage inappropriate behavior, however, should be discussed with the parents first. Helping the adult to recognize what’s going to show up improves the remedy alliance(22).
A. Noninvasive strategies
1. Tell-Show-Do
The introduction of novel devices and/or methods can regularly scare children with tension as they’ll now no longer be alert on the meant reason of those devices or methods. Tell-Show-Do is an essential precept utilized in pediatric dentistry wherein the kid is bringing in progressively to the tool and/or process, and which includes:
Tell: words to provide an explanation for methods in language appropriate to the extent of accepting for every kid.
Show: exhibition of the process in a watchfully described, non-threatening placing.
Do: Complete the process without a deviating from the explanation and demonstration.
For instance, whilst introducing the slow speed handpiece in advance to initiate a prophylaxis, initially discuss about the sound that will be made while the device is turned on, then demonstrate it applying on the child’s finger, and follow with using the handpiece in your patient’s mouth(42).
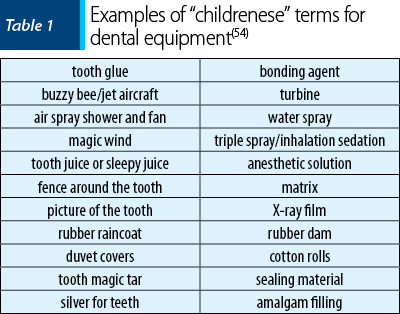
It is essential that the language used is suitable to the kid’s age: many dentists use a non-public model of this “childrenese” (Table 1) and the entire dental crew should adopt the equal technique. Specifically emotive or bad phrases are avoided; it has been shown to be a powerful manner of decreasing anticipatory tension in new infant patients(48). The approach is beneficial for all children who can communicate. It is extensively used in pediatric dentistry and easily accepted by parents(3). More recently, it has been proven to reduce anticipatory tension in new child patients, however, it turned into much less beneficial in youngsters with previous dental experiences(48). There aren’t any contraindications.
2. Systematic desensitization (SD)
The technique involves the gradual introduction of therapeutic stimuli or procedures (from the simplest and most painless to the most complex and with a greater degree of discomfort) that could induce fear, while working to replace anxiety with a more relaxed behavior. However, the technique is time consuming. It starts with procedures such as sealing, fluoridation, small fillings, atraumatic restoration technique (ART) and continues with the rest of the treatment methods. The child’s present anxieties are handled by means of exposing her or him to a chain of dental experiences, provided in an order of growing tension evocation, progressing most effective whilst the kid can be given the preceding one in a comfortable state(50).
3. Nonverbal communication
This type of conversation takes place constantly and might give a boost to or contradict verbal signals. Such conversation consists of having a baby in pleasant surroundings and a happy, smiling crew(6). Reassurance has been proven to be useless as a way of controlling distress. In contrast, reinforcement – enquiring how the kid is feeling or mild pats and squeezes – has been observed to decrease distress(31). These verbal directions and symptoms are used to provide wonderful encouragement and beautify different management techniques and can be beneficial for all children. A friendly environment, a smiling medical team, the satisfied facial expression of the doctor, the friendly handshakes or the encouraging pats on the shoulder reduce the tension much better than the verbal calm.
4. Voice management
Young kids regularly reply to the tone of voice as opposed to the real phrases(6). This approach is a managed amendment of voice volume, tempo and tones, to steer immediately the child’s attitude. It is special for the uncooperative or distracted children to benefit interest and observance, keep away from bad course, and set up authority. For instance, an abrupt alternate from gentle to loud to benefit interest of a baby who isn’t complying. It isn’t used with kids who, because of their age, disability or emotional immaturity, are incapable to recognize or cooperate. Once the desired conduct is accomplished, it’s far waged and positively reinforced(42).
5. Modeling
It involves changing the behavior of the fearful child through the personal example of another child who is cooperative (children are very receptive to their peers of the same age and gender). Throughout the treatment, the dentist should provide positive feedback, encourage, and especially praise the attitude of the child who will stay calm. This technique is more helpful in those aged between 3 and 5 years old(21).
6. Behavior shaping and positive reinforcement
Many dental methods require pretty complicated behaviors and moves from our patients which want to be defined and learned. For kids, this calls for small clean steps. This method is named behavior shaping. It includes a described collection of steps in the direction of the best conduct. This is maximum effortlessly accomplished meaning of selective reinforcement. Reinforcement is the strengthening of a sample of behavior, growing the opportunity of that behavior being displayed once more in the future. Anything that the kid finds pleasurable can act as a positive reinforcer, stickers or badges are regularly used. However, the maximum effective reinforcers are social stimuli, consisting of facial expression, pleasant voice modulation, verbal reward, approval via way of means of hugging(51). A child-centered, empathic reaction giving unique reward – for instance, “I just like the manner you maintain your mouth open” – has been proven to be more powerful than a popular remark like “Good girl”(51). As with Tell-Show-Do, the usage of age’s unique language is essential(6). Selective reinforcement of suitable responses and ignoring irrelevant responses lead the kid at their personal tempo in the direction of the best. Unrewarded responses have a tendency to be extinguished whilst suitable conduct is straight away reinforced(31). The approach is beneficial for all children who can communicate. There aren’t contraindications.
7. Distraction
Distraction intends to change the child’s interest far from the remedy dealing. This might be done using the shape of cartoons, books, music or stories. An extra nicely trendy technique is for dentists to talk to children as they work in order that children take note of them, as opposed to focusing at the remedy process. Short-time period distractions, consisting of pulling the cheek or lip and chatting to the child whilst making use of local anesthesia, are also beneficial(3).
8. Enhancing control
At this point, the child receives a scale of manage over their dentists’ conduct through the usage of forestall signals. Such marks had been proven to decrease suffering throughout usual dental procedure in addition to using injection. The forestall signal, normally elevating an arm, should be rehearsed, and the dentist must act in reaction unexpectedly whilst it’s far used. The approach is beneficial for all children who can communicate. There aren’t contraindications(52).
B. Invasive (aversive) strategies
9. Protective stabilization (restraint)
Restraint within the dental placing is the act of bodily restricting the frame moves of the child to facilitate the dental treatment and to lower feasible accidents to the kid and/or dentist(10). Varieties of defensive stabilization may be engaged, starting from a member/caregiver protecting the kid’s arms to make use of a stabilization tool (i.e., papoose board or pedowrap). Informed acquiesce should be acquired for the usage of defensive stabilization, and if a member of the family has a trouble at any time to the usage of defensive stabilization, the approach is stopped up straight away. We do now no longer make use of any stabilization plans as they might limit the respiration(53). This technique should be used when absolutely necessary, not as a punishment; the least restrictive alternative should be chosen(10).
10. Negative reinforcement
The effective impact of positive reinforcement has been mentioned already. Negative reinforcement has additionally been utilized in dental procedures. It is the strengthening of a sample of conduct by the elimination of a stimulus which the patient perceives as ugly (a bad reinforcer) as quickly as the desired attitude is exhibited. The stimulus is carried out to all moves besides the desired one, hence reinforcing it by elimination of a bad stimulus. It must now no longer be used as punishment, which means, in fact, applying negative stimulus in response to inappropriate attitude.
A well-known example in dental practice is Hand Over Mouth (HOM), which includes restraining the child within the dental seat, setting a hand over the mouth (to permit the kid to hear). The nose should no longer be covered. The dentist then talks quietly to the kid, explaining that the hand could be eliminated as quickly as crying stops. As quickly as this occurs, the hand is eliminated and the kid flattered. If the protests begin once more, the hand is replaced. The method pursues to increase the kid’s interest and allow conversation, give a boost to desirable behavior and set up that cancellation is in vain(54). WHO recommends this approach for 4-9-year-old patients whilst conversation is misplaced or throughout mood tantrums. Parental agreement is essential and the method must in no way be used on patients too young to comprehend or with intellectual or emotional impairment(54).
Nonetheless, while utilized in North America(55), the method stays disputed(56,57). There had been no research of the effectiveness of Hand Over Mouth technique. Its legality (concerning restraint and human rights) has additionally been questioned(57,58).
Conclusions
Behavior control is extensively agreed to be a key element providing dental care to children. It is important that any technique for the behavioral control for the pediatric patient should be rooted in compassion and a concern for the well-being of every child.
A wide range of behavioral control strategies are presented to pediatric dentists which should be used as appropriate for the benefit of every child and which, significantly, should bear in mind all cultural, legal and philosophical requirements in the country of practice of the pediatric dentist.
For the future, given the dynamics of society, the changing concepts, mentalities and the spectrum of pediatric pathology, but also the evolution and intellectual emancipation of pediatric patients, it is clear the need for a collaboration between dental and behavioral scientists in order to develop, adapt and implement additional behavioral management techniques in pediatric dentistry.
Bibliografie
-
Peretz B, Zadik D. Parents’ attitudes toward behavior management techniques during dental treatment. Pediatr Dent. 1999;21:201–204.
-
Scott S, Garcia-Godoy F. Attitudes of Hispanic parents toward behavior management techniques. J Dent Child. 1998;65:128–131.
-
Chadwick B. Non-pharmacological Behavior Management: Clinical Guidelines. The British Society of Pediatric Dentistry; 2002. Available from: http://www.Tiny.Cc/9kid0.
-
McElroy, CM. Dentistry for children. California Dental Association Transactions. 1985, 85.
-
Wright GZ. Behaviour management in dentistry for children. W.B. Saunders Company, 1975.
-
Wright GZ, Starkey PE, Gardner DE. Child management in dentistry, Oxford: Wright, 1987.
-
Frankl SH, Shiere FR, Fogels HR. Should the parent remain within the dental operatory? J Dent Child. 1962;29:150–163
-
AAPD (American Academy of Pediatric Dentistry) Clinical Affairs Committee, Guideline on Behavior. Guidance for the Paediatric Dental Patient. Pediatr Dent Reference Manual. 2008;29:115-124.
-
American Academy of Pediatric Dentistry. Guideline on Behavior Guidance for the Pediatric Dental Patient. Pediatr Dent. 2011;36:161-73.
-
Roberts JF, Curzon ME, Koch G, Martens LC. Review: behaviour management techniques in paediatric dentistry. Eur Arch Paediatr Dent. 2010;11(4):166-174.
-
Wright GZ. Behavior Management in Dentistry for Children, Second Edition. John Wiley & Sons, Inc. Published, 2014.
-
Wilson CW. Child Management. Journal of the American Dental Association. 1933;20:890–892.
-
Klaassen MA, et al. Stressful situations for toddlers: indications for dental anxiety? ASDC Journal of Dentistry for Children. 2002;69:297–305.
-
Frankl SN, Shiere FR, Fogels HR. Should the parent remain with the child in the dental? ASDC Journal of Dentistry for Children. 1962;29:150–155.
-
ten Berge M, Veerkamp JS, Hoogstraten J, et al. Childhood dental fear in the Netherlands: prevalence and normative data. Community Dentistry and Oral Epidemiology. 2002;30:101–107.
-
McDonald RE. Dentistry for the Child and Adolescent. C. V. Mosby Co, St. Louis, 1969.
-
Carey WB. Let’s give temperament its due. Contemporary Pediatr. 1998;15:91-113.
-
Wright GZ, Alpern GD. Variables influencing children’s co-operative behaviour at first dental visit. J Dent Child. 1971;23:124-128.
-
Wright GZ, Alpern GD, Leake JL. A cross-validation of the variables affecting children’s co-operative behaviour. J Canad Dent Assoc. 1973;39:268-273.
-
Bailey PM, Talbot M, Taylor PP. A comparison of maternal anxiety and anxiety levels manifested in the child patient. J Dent Child. 1973;40:277-284.
-
McTigue DJ. Behaviour management of children. In: Spedding, R.H. Symposium on pedodontics. Dent Clin North Am. 1984;28:81-93.
-
Freeman R. The case for mother in the surgery. Brit Dent J. 1999;186:610-613.
-
Johnson R, Baldwin DC Jr. Maternal anxiety and child behaviour. J Dent Child. 1969;36:87-92.
-
Corkey B, Freeman R. Predictors of dental anxiety in 6-year-old children – a report of a pilot study. ASCD J Dent. 1994;61:267-271.
-
Johnson R, Baldwin DC Jr. Relationship of maternal anxiety to the behaviour of young children undergoing dental extraction. J Dent Res. 1968;47:801-805.
-
Bandura A. Principles of Behavior Modification. New York: Holt, Rinehart & Winston, 1969.
-
Gustafsson A, Broberg A, Bodin L, Berggren U, Arnrup K. Dental behaviour management problems: the role of child personal characteristics. Int J Paediatric Dent. 2010;20:242-253.
-
Maccoby EE, Martin JA. Socialization in the context of the family: Parent-child interaction. In: Mussen P, Hetheringon EM. (Eds). Handbook of Child Psychology, Volume IV: Socialization, personality, and social development. 1–101. New York: Wiley, 4th Ed, 1983.
-
Bailey PM, Talbot A, Taylor PP. A comparison of maternal anxiety levels manifested in the child dental patient. J Dent Child. 1973; 40:277-284.
-
Venham LL, Murray P, Gaulin-Kremer E. Child-rearing variables affecting the pre-school child’s response to dental stress. J Dent Res. 1979b;58:2042-5.
-
Weinstein P, Getz T, Ratener P, Domoto P. The effect of dentist’s behaviors on fear-related behaviors in children. J Amer Dent Assoc. 1982a;104:32-38.
-
Melamed BG, Ross SL, Courts F, et al. Dentist’s behavior management as it affects compliance and fear in paediatric patients. J Amer Dent Assoc. 1983;106:324-330.
-
Guideline on Behavior Guidance for the Pediatric Dental Patient, Council of Clinical Affairs. Reference Manual. 2011;35:13-14.
-
Klingberg G, Berggren U. Dental problem behaviors in children of parents with severe dental fear. Swed Dent J. 1992;16:27-32.
-
Baier K, Milgrom P, Russell S, Mancl L, Yoshida T. Children’s fear and behavior in private pediatric dentistry practices. Pediatr Dent. 2004;26:316-21.
-
Long N. The changing nature of parenting in America. Pediatr Dent. 2004;26:121-4.
-
Hockenberry MJ, Wilson D. Wong’s Essentials of Pediatric Nursing. 8th ed. St. Louis, Mo: Mosby, Inc.; 2009. p. 162.
-
Pinkham J. An analysis of the phenomenon of increased parental participation during the child’s dental experience. J Dent Child. 1991;58:458-463.
-
Fenlon WL, Dabbs AR, Curzon ME. Parental presence during treatment of the child patient: a study with British parents. Br Dent J. 1993 Jan 9;174(1):23-8.
-
Feigal RJ. Guiding and managing the child dental patient: a fresh look at old pedagogy. J Dent Educ. 2001; 65(12):1369-77.
-
Kotsanos N, Coolidge T, Velonis D, Arapostathis KN. A form of parental presence/absence (PPA) technique for the child patient with dental behaviour problems. Eur Archs Paediatr Dent. 2009;10:90-92.
-
Singh H, Rehman R, Kadtane S, Dalai DR, Jain CD. Techniques for the Behavior Management in Pediatric Dentistry. Int J Sci Stud. 2014;2(7):269-272.
-
Murphy MG, Fields HW, Machen JB. Parental acceptance of pediatric dentistry behavior management techniques. Pediatr Dent. 1984;6:193-8.
-
Hagan PP, Hagan JP, Fields HW, Machen JB. The legal status of informed consent for behavior management techniques in pediatric dentistry. Pediatr Dent. 1984;6:204-8.
-
Havelka C, McTigue D, Wilson S, Odom J. The influence of social status and prior explanation on parental attitudes toward behavior management techniques. Pediatr Dent. 1992;14:376-81.
-
Kreinces GH. Ginott psychology applied to pedodontics. J Dent Child. 1975;45:119-122.
-
Christen AG. Piagetian psychology: some principles as helpful in treating the child dental patient. J Dent Child. 1977;44:448-452.
-
Carson P, Freeman R. Tell-show-do: reducing anticipatory anxiety in emergency paediatric dental patients. Int J Health Prom & Educ. 1998;36:87-90.
-
Fayle S, Crawford PJM. Making dental treatment acceptable to children. Dental Profile. 1997 September;18-22.
-
Wolpe J. Psychotherapy by Reciprocal Inhibition. Palo Altos; Stamford University Press, 1958, 71-75.
-
Weinstein P, Nathan JE. The challenge of fearful and phobic children. Dent Clin North Am. 1988;32(4):667-692.
-
Wardle J. Management of Dentalpain. Paper Presented at the British Psychological Society Annual Conference, York; 1982.
-
Luscre DM, Center DB. Procedures for reducing dental fear in children with autism. J Autism Dev Disord. 1996;26:547-56.
-
American Academy of Paediatric Dentistry. Guidelines for behaviour management. Pediatr Dent. 1998;20(Special Issue):27-32.
-
Barton DH, Hatcher C, Porter R, et al. Dental attitudes and memories: a study of the effects of hand over mouth/restraint. Ped Dent. 1993;15:13-19.
-
Andlaw RJ, Rock WP. A Manual of Paedodontics, 2nd edition, Edinburgh, Churchill Livingston, 1982.
-
Roberts JF. How important are techniques? The empathic approach to working with children. J Dent Child. 1995;62:38-43.
-
Wright FAC, McMurray NE, Giebartowski J. Strategies used by dentists in Victoria, Australia to manage children with anxiety or behaviour problems. J Dent Child. 1991;58:223-228.





