Background. Leiomyomas are a known cause of infertility and recurrent pregnancy loss, with a global incidence of 25-30% and 2.7-10.7% during pregnancy. They can have an unpredictable evolution and determine numerous complications during pregnancy, such as preterm delivery and severe postpartum hemorrhage.
Case presentation. This case report presents a successful pregnancy obtained after the removal of 21 leiomyomas by abdominal myometrectomy. A 28-year-old patient, gravida 2, abortus 1, with uterine fibroids, was subjected to multiple abdominal myometrectomy. Four months after surgery, the patient reported amenorrhea for 7 weeks, and intrauterine evolutive pregnancy was confirmed. She had an uncomplicated pregnancy and delivered by caesarean section a healthy female fetus, weighing 2900 g.
Conclusion. The management of leiomyomas before obtaining a pregnancy should be highly recommended. To the best of our knowledge, this is the first case reporting a successful pregnancy after the removal of 21 fibroid nodules by abdominal myometrectomy.
Sarcină obţinută după îndepărtarea a 21 de leiomioame prin miometrectomie abdominală
Successful pregnancy after 21-nodule removal by abdominal myometrectomy
First published: 16 iunie 2017
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Peri.1.2.2017.836
Abstract
Rezumat
Introducere. Leiomioamele sunt o cauză cunoscută de infertilitate şi avort spontan recurent, având o incidenţă globală de 25-30%, respectiv 2,7-10,7% în sarcină. Leiomioamele pot avea evoluţie imprevizibilă şi pot determina numeroase complicaţii în sarcină, precum naştere prematură şi hemoragie post-partum severă.
Prezentare de caz. Prezentăm cazul unei sarcini obţinute după îndepărtarea a 21 de leiomioame prin miometrectomie abdominală. O pacientă în vârstă de 28 de ani, II gesta, I para, cu leiomioame uterine, a beneficiat de miometrectomie abdominală multiplă. La 4 luni după intervenţia chirurgicală, pacienta a raportat amenoree de 7 săptămâni, confirmându-se prezenţa unei sarcini intrauterine în evoluţie, care nu a prezentat complicaţii. Pacienta a născut prin operaţie cezariană un făt sănătos, de sex feminin, cu greutate de 2600 g.
Concluzie. Pacientele ar trebui consiliate în vederea tratamentului leiomioamelor înainte de concepţie. În limita cunoştinţelor noastre, acesta este primul caz raportând o sarcină cu evoluţie favorabilă după îndepărtarea a 21 de fibroame prin miometrectomie abdominală.
Introduction
Uterine leiomyomas, also called uterine myomas or fibroids, are benign proliferations of smooth muscle cells of the myometrium. Being the most common benign genital solid tumors, leiomyomas are diagnosed in 25%-30% of females during their lives(1). Myomas have a major impact on women’s health, as they can cause significant morbidity, including heavy or prolonged menstrual bleeding, pelvic pressure of pain and, more rarely, reproductive dysfunction(2). Fibroids may cause infertility and recurrent pregnancy loss, being estimated as responsible for approximately 7% of recurrent spontaneous abortions(3,4).Numerous studies have assessed the effectiveness of either abdominal, laparoscopic or transvaginal myomectomy in the improvement of fertility and pregnancy outcomes. It has been suggested that the results are correlated with the patient’s age, myoma size, number and location, as well as the interval between myomectomy and pregnancy(5,6).
We report the case of a patient with multiple leiomyomas, who had a prior normal pregnancy and a first trimester abortion, who sponaneously conceived 3 months after abdominal myometrectomy with the removal of 21 fibroids.
Case report
The patient was a 28-year-old woman, gravida 2, para 1, who was admitted to our institution on the 8th of May 2015 for lower abdominal pain and abnormal uterine bleeding.The patient had previously a normal, uncomplicated pregnancy with term vaginal delivery. She had also experienced a spontaneous abortion at 8 gestational weeks three months before. The anamnesis indicated family history of leiomyomatosis, including her mother and sister. Nicotine use was noted: 4-5 cigarettes per day.
Clinical examination revealed uterine bleeding, enlarged uterus with irregular contour, suprapubic sensitivity to palpation.
Ultrasound examination revealed a globally enlarged uterus, presenting numerous well delimited hypoechoic nodules, including: one nodule located at the uterine fundus, measuring 5 cm, one intraligamentar nodule measuring 3.9 cm, and one intramural nodule located on the posterior uterine wall, measuring 3 cm. The sonographic aspect was highly suggestive for multiple leiomyomatosis.
The treatment options were presented to the patient, depending on her future will to conceive. Since she was not sure about ending her reproductive life, the patient opted for multiple myometrectomy, if the intraoperative findings made this option possible.
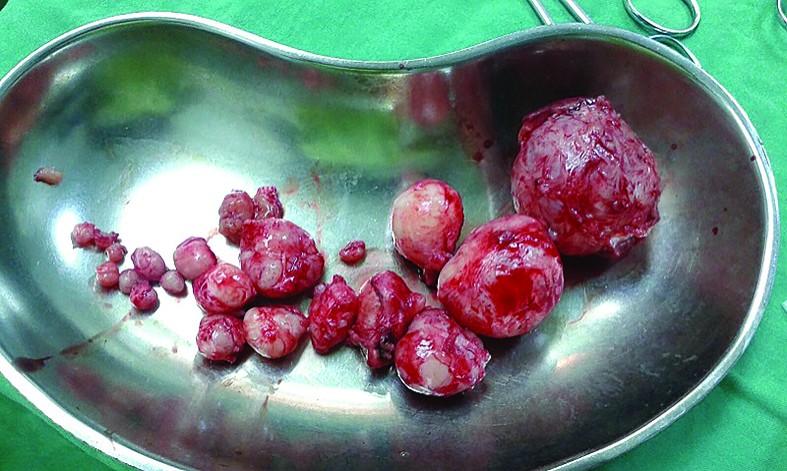
Intraoperative, multiple fibroids were observed, having subserosal and intramural location, along with small fibroids having an intramural and a submucosal component. Multiple myometrectomy was performed, with the removal of 21 fibroids, with diameters ranging from 0.5 to 6 cm (Figure 1). The uterus was repaired in layers, using vicryl sutures, and hemostasis was achieved. The postoperative evolution was normal, without complications. The pathology confirmed multiple fibroids, along with normal endometrial tissue in the secretory phase.
On 17th September 2015 (4 months after the surgical procedure) the patient presented to our institution for secondary amenorrhea.
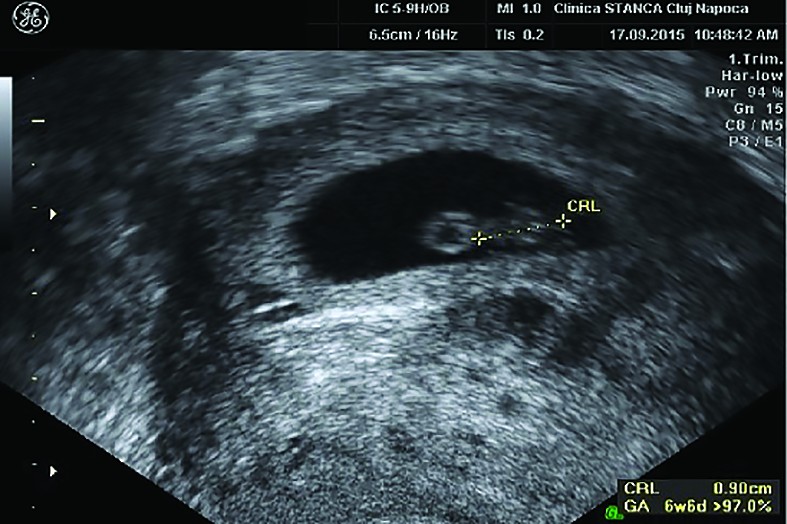
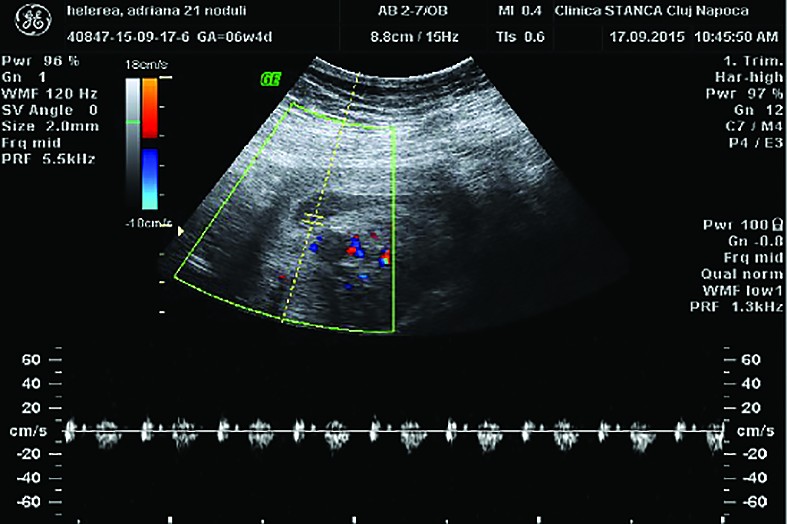
Ultrasound examination revealed intrauterine pregnancy, embryo with crown rump length corresponding to 6 weeks + 6 days (Figure 2), with detectable cardiac activity (Figure 3). The patient decided to continue the pregnancy.
At 36 gestational weeks, she was admitted in emergency to an institution in another region of the country for uterine contractions. Caesarean section was decided by the clinic personnel. The patient delivered by caesarean section a living female fetus, weighing 2900 g, Apgar index =9.
Discussion
Leiomyomas have a reported incidence of 2.7-10.7% during pregnancy(7,8). The stimulatory effects of pregnancy on leiomyomas are unpredictable and can be impressive(9). The complications associated with this condition are numerous and include: preterm delivery, abruptio placentae, malposition, breech presentation and severe postpartum hemorrhage(7,9,10).Since leiomyomas significantly increase the risk of adverse pregnancy outcomes and can sometimes represent a cause of infertility(11), ideally, they should be managed before conception(12,13). Treatment options include open surgery, laparoscopic or hysteroscopic removal of leiomyomas, embolization of the uterine artery and hormonal treatment.
Open and laparoscopic myomectomy are most commonly used, depending on the size, number and location of the masses. Although patients who undergo laparoscopy recover faster and have less blood loss, laparoscopy does not conserve future fertility better than abdominal myomectomy(3). Uterine artery embolization appears to increase the risk of miscarriage and postpartum hemorrhage, therefore this procedure is not appropriate for patients who want to conceive(9,14,15). Hormonal treatments with selective progesterone receptor modulators, such as ulipristal acetate, have also been used in order to reduce the size of leiomyomas and to facilitate the sugical procedure; some studies describe the hormonal therapy to have optimal effects when administered after myomectomy(16).
In our case, being given the wide spread of the myomas, abdominal myomectomy was considered the most suitable option.
When considering delivery after a prior myomectomy, most obstetricians would assess the risk for uterine rupture. It was demonstrated that there were no significant differences in the perinatal outcomes between the females who had laparoscopic or abdominal myomectomy(17). However, since the risk of uterine rupture might be underestimated by some studies and being given the potential impact of such a condition, even fatal consequences for both mother and fetus, obstetricians should perform a very careful follow-up for pregnant patients after a prior myomectomy(18). In our case, the patient was admitted in emergency to a small regional center, with regular uterine contractions occuring every 10 minutes. Given the limited experience of the center, vaginal delivery was considered inappropriate after multiple myometrectomy and caesarean section was performed at 36 gestational weeks. The patient delivered a healthy female fetus, weighing 2900 g.
In the presence of uterine fibroids in a patient of reproductive age, the management of leiomyomas before obtaining a pregnancy should be highly recommended. To the best of our knowledge, this is the first case reporting a successful pregnancy after the removal of 21 fibroid nodules by abdominal myometrectomy.
Bibliografie
2. Weibel H, Jarcevic R, Gagnon R, Tulandi T. Perspectives of Obstetricians on Labour and Delivery After Abdominal or Laparoscopic Myomectomy. Journal of Obstetrics and Gynaecology Canada. 2014; 36(2):128-132.
3. Sangha R, Strickler R, Dahlman M, Havstad S, Wegienka G. Myomectomy to Conserve Fertility: Seven-Year Follow-Up. Journal of Obstetrics and Gynaecology Canada. 2015; 37(1):46-51.
4. Zhang Y, Hua K. Patients’ Age, Myoma Size, Myoma Location, and Interval Between Myomectomy and Pregnancy May Influence the Pregnancy Rate and Live Birth Rate After Myomectomy. Journal of Laparoendoscopic & Advanced Surgical Techniques. 2014; 24(2):95-99.
5. Rovio P, Heinonen P. Pregnancy outcomes after transvaginal myomectomy by colpotomy. European Journal of Obstetrics & Gynecology and Reproductive Biology. 2012; 161(2):130-133.
6. Gavai M, Berkes E, Lazar L, Fekete T, Takacs Z, Urbancsek J et al. Factors affecting reproductive outcome following abdominal myomectomy. Journal of Assisted Reproduction and Genetics. 2007; 24(11):525-531.
7. Qidwai G, Caughey A, Jacoby A. Obstetric Outcomes in Women with Sonographically Identified Uterine Leiomyomata. Obstetrics & Gynecology. 2006, 107(2, Part 1):376-382.
8. Laughlin S, Baird D, Savitz D, Herring A, Hartmann K. Prevalence of Uterine Leiomyomas in the First Trimester of Pregnancy. Obstetrics & Gynecology. 2009; 113(3):630-635.
9. Cunningham F Gary, et al. Williams Obstetrics. 24th edition. New York: McGraw-Hill Education, 2014; 1219-1239.
10. Sheiner E, Bashiri A, Levy A, Hershkovits R, Katz M, Mazor M. Obstetric Characteristics and Perinatal Outcome of Pregnancies with Uterine Leiomyomas. Obstetrical & Gynecological Survey. 2004; 59(9):647-648.
11. Zepiridis L, Grimbizis G, Tarlatzis B. Infertility and uterine fibroids. Best Practice & Research Clinical Obstetrics & Gynaecology. 2016; 34:66-73.
12. Li T, Mortimer R, Cooke I. Myomectomy: a retrospective study to examine reproductive performance before and after surgery. Human Reproduction. 1999; 14(7):1735-1740.
13. Fauconnier A, Dubuisson J, Ancel P, Chapron C. Prognostic factors of reproductive outcome after myomectomy in infertile patients. Human Reproduction. 2000; 15(8):1751-1757.
14. Homer H, Saridogan E. Uterine artery embolization for fibroids is associated with an increased risk of miscarriage. FertilSteril. 2010 Jun; 94(1):324-30.
15. Stokes LS, Wallace MJ, Godwin RB, Kundu S, Cardella JF. Society of Interventional Radiology Standards of Practice Committee. Quality improvement guidelines for uterine artery embolization for symptomatic leiomyomas. J VascIntervRadiol. 2010 Aug; 21(8):1153-63.
16. Monleón J, Martínez-Varea A, Galliano D, Pellicer A. Successful Pregnancy after Treatment with Ulipristal Acetate for Uterine Fibroids. Case Reports in Obstetrics and Gynecology. 2014; 2014:1-3.
17. Fukuda M, Tanaka T, Kamada M, Hayashi A, Yamashita Y, Terai Y et al. Comparison of the perinatal outcomes after laparoscopic myomectomy versus abdominal myomectomy. GynecolObstet Invest. 2013; 76(4):203-8.
18. Kim HS, Oh SY, Choi SJ, Park HS, Cho GJ, Chung JH et al. Uterine rupture in pregnancies following myomectomy: a multicenter case series. ObstetGynecolSci 2016; 59(6):454-462.