Dificultăţi de examinare ecografică la gravidele supraponderale. Studiu retrospectiv şi analiza literaturii
Ultrasound examination difficulties in overweight pregnant patients. Review of literature and retrospective study
Abstract
Introduction. In the last decades, the medical system has encountered more frequently obese or overweight patients. Obesity is associated with higher risks for one’s life and with technical difficulties when it comes to management and treatment. It is estimated that 15-20% of the population is affected by this condition, and the percentage for the pregnant women has doubled in the last decade. As ultrasound examination is an important part of prenatal care, we studied how the Body Mass Index (BMI) affected the ultrasound examination in a specialized medical clinic. Materials and method. This is a longitudinal retrospective study on the second- and third-trimester ultrasound scans performed in the last five years on patients with BMI over 25 kg/m2. The repartition was done regarding the recommended categories: overweight (25-30 kg/m2), first-degree obesity (30-35 kg/m2), second-degree obesity (35-40 kg/m2) and third-degree obesity (>35 kg/m2). The statistical analysis regarded the number of ultrasound examinations performed for each patient and the technical difficulties experienced due to overweight or obese patients. Factors such as timing for each scanning and recommendations for better ultrasound examination were mentioned. Results. There were 1101 ultrasound scans selected, that were performed for second- and third-trimester morphological ultrasounds in 942 patients. These patients were distributed as overweight (69%), with first-degree obesity (22%), second-degree obesity (6%) and third-degree obesity (3%). In general, the number of repeated scans in the study was higher than in normal patients, although no statistical correlation to BMI could be established. In 58% of cases, the specialist marked the technical difficulties in the fetal ultrasound assessment, mainly related to the abdominal maternal adiposity. Most frequently, the recommendation was for the scan to be repeated after 2-4 weeks, as opposed to the usual 6-8 weeks interval in regular patients. No correlation to the BMI was found for fetal anomalies, Doppler parameters or estimation of fetal growth. Conclusions. Obesity has become an important risk factor during pregnancy and implies difficulties in performing antenatal fetal ultrasound. The new specialists for antenatal fetal morphology ultrasound evaluation should be trained to deal with the pitfalls and tricks related to the accuracy of fetal ultrasound examination in obese or overweight patients. The limitations of this imagistic investigation should be explained to each patient.Keywords
obesitypregnancyantenatal carefetal ultrasoundRezumat
Introducere. În ultimele decenii, sistemul medical se confruntă tot mai des cu paciente obeze sau supraponderale. Obezitatea este asociată cu un risc vital crescut şi cu dificultăţi tehnice legate de management şi tratament. Se estimează că 15-20% din populaţie este afectată de această patologie şi că procentajul gravidelor obeze s-a dublat în ultimul deceniu. Deoarece ecografia obstetricală este parte esenţială a urmăririi prenatale, am analizat cum indicele de masă corporală (BMI) a influenţat examinarea ecografică într-un centru de specialitate. Materiale şi metodă. Acesta este un studiu longitudinal retrospectiv, realizat pe ecografii obstetricale de al doilea şi al treilea trimestru, efectuate în ultimii cinci ani la paciente cu BMI de peste 25 kg/m2. Pacientele au fost împărţite după clasificarea recomandată: supraponderale (25-30 kg/m2), obezitate de gradul I (30-35 kg/m2), obezitate de gradul II (35-40 kg/m2) şi obezitate de gradul III (peste 40 kg/m2). Analiza statistică a urmărit numărul de ecografii efectuate şi dificultăţile tehnice descrise în funcţie de suprapondere sau obezitate. Factori precum momentul ecografiei sau recomandări pentru o mai bună vizualizare au fost menţionaţi. Rezultate. Au fost selectate 1101 ecografii morfologice de trimestre doi şi trei, efectuate la 942 de paciente. Pacientele au fost clasificate pe baza greutăţii dinaintea sarcinii ca supraponderale (69%), obezitate de gradul I (22%), obezitate de gradul II (6%) sau obezitate de gradul III în 3% din cazuri. În general, numărul de ecografii per pacientă a fost mai mare decât la pacientele normoponderale, dar nu a existat o corelaţie statistică cu BMI. În 58% din cazuri, ecografistul a remarcat dificultăţi tehnice de evaluare a morfologiei fetale, legate mai ales de peretele abdominal matern. Cel mai des, recomandarea a fost să se repete ecografia la 2-4 săptămâni, spre deosebire de intervalul de 6-8 săptămâni la sarcinile normale. Nu s-au găsit corelaţii cu anomaliile fetale, indicii Doppler sau cu creşterea fetală. Concluzii. Obezitatea este un factor de risc important în sarcină, implicând dificultăţi de evaluare ecografică fetală antenatală. Noii specialişti în ecografia morfologică fetală ar trebui să fie pregătiţi pentru a cunoaşte capcanele şi artificiile tehnice legate de acurateţea ecografiei fetale la gravidele supraponderale sau obeze. Limitele acurateţei acestei explorări imagistice ar trebui explicate şi înţelese de fiecare pacientă.Cuvinte Cheie
obezitatesarcinăurmărire prenatalăecografie fetalăIntroduction
Worldwide obesity has become a major public health issue, characterized as an epidemic situation. It is affecting people of all ages, gender and social or economic status. Patients are diagnosed with obesity by calculating their Body Mass Index (BMI), and values higher than 30 kg/m2 have been identified in approximately 15-20% of the global population. As already mentioned, this pathological state is affecting people throughout their entire life cycle, including females in their reproductive period; the particularity of this group consists in the complications which obesity adds during pregnancy(1). Studies performed globally identified a percentage of 26% of non-pregnant female individuals suffering from obesity in the United States of America, with ages between 20 to 39 years old(2). United Arab Emirates offers a specific statistic which shows that 40% of married females were diagnosed with obesity(3). Lower incidences were found in Australia where, according to statistics performed between 2004 and 2005, only 15% of their female population with ages between 25 and 34 years old were suffering from obesity(4).
For women who already suffer from obesity and its complications, pregnancy implies gaining additional weight, therefore leading to an increasing range of complications for this category of patients. Studies performed in the North East of England found increasing rates of obesity among pregnant patients, from 9.9 % in 1990 to 16% in 2004(5).
World Health Organization (WHO) established four different categories of weight in accordance with maternal BMI: underweight, with a BMI lower than 18.5 kg/m2, normal weight, with a BMI between 18.5 kg/m2 and 24.9 kg/m2, overweight, with a BMI between 25 kg/m2 and 29.9 kg/m2, and obese, with a BMI higher or equal to 30 kg/m2(6).
The effects of overweight and obesity in pregnant patients are not to be neglected, affecting both mother and the fetus. Among the most frequent, we encounter preeclampsia, gestational diabetes, preterm delivery, thromboembolic disease, stillbirth and macrosomia(7-9). When associated with increased maternal age, complications due to obesity are even higher and are often identified during elective or emergency caesarean delivery(10). Newborns resulted from pregnancies associated with obesity are at higher risk of requiring medical intervention after delivery, as well as admission to neonatal intensive care unit(11). During child age and throughout their life, these children are at an increased risk for obesity themselves and often associate cardiovascular disease and diabetes(12).
The excess of adipose tissue can induce metabolic disorders, damage of the vascular and inflammatory pathways in multiple organs. These obesity effects are exacerbated by the physiological modifications that occur during pregnancy, leading to adverse outcomes(13). Patients with obesity and desiring for a pregnancy should be correctly informed of the benefits of weight loss before conception. Strategies to manage weight intake during pregnancy have been implemented, but had minor effects in reducing maternal and neonatal complications(14). Pre-conception counseling for this category of women should include information about the benefits of a healthy diet, physical exercise and behavioral modifications(15,16). A weight loss of 5-10% in non-pregnant female patients showed an improvement in the metabolic disorders associated with obesity, such as renal function and better glycemic levels(17).
Certain clinical assessments of fetal status and size in obese or overweight patients represent a challenge for obstetricians. One of the essential imagistic investigations during pregnancy consists in the ultrasound examination of the fetus. It is an accurate method for evaluating the estimated fetal weight (EFW) and it has been used for decades(18). Contrary to the reliability of this investigational method, a prospective study reported error ranges of 20% after comparing the EFW determined by ultrasound investigation and the actual births weights(19). However, studies evaluating the influence of obesity in pregnant patients on accurate estimation of the fetal weight are limited. When taking into consideration the association between increased maternal BMI and fetal macrosomia, high rates of delivery by caesarean operation and abnormalities of labor, we understand the importance of an appropriate sonographic fetal weight assessment(20).
The most important fetal ultrasound examination is the second-trimester scan, as it is performed in order to identify fetal morphologic characteristics(21). Eurofetus multicenter study was conducted in 1999 in order to establish the accuracy of second-trimester routine ultrasonography fetal examinations. They managed to detect 56% of 4615 malformations and to identify 55% of major anomalies before 24 weeks of gestation. Obviously, the accuracy of second-trimester ultrasonography is correlated to various factors, such as the sonographer’s experience, the adequate training and the method of performing the examination. Factors related to the patient are highly important as well, such as maternal body habitus, uterine fibroids, abdominal wall scarring and other internal pelvic masses, fetal position, duration of the examination and the quality of the machine on which the scan is performed(22). Female pregnant patients who are overweight or obese have a higher chance of misdiagnosis for multiple minor markers and a lower probability of detecting common anomalies(23,24). A basic fetal anatomic assessment is normally performed in approximately 10 minutes, each 5 minutes added to the evaluation being related to an improvement in the examination(25).
The aim of this study was to estimate the difficulties encountered during fetal examination in the second and third trimesters of pregnancy due to overweight or obesity, unfavorable fetal position, placental position, quantity of amniotic fluid and other particular situations.
Materials and method
We conducted a retrospective study on overweight or obese pregnant patients admitted to Avicena Profertis Medical Clinic of Iaşi, Romania, a specialized center for prenatal diagnosis. A total of 942 patients, with ages between 18 and 47 years old, were enrolled in our study and underwent second- or third-trimester fetal scan in a period of five years. A total of 1101 fetal ultrasound examinations were performed. No multiple pregnancies were assessed, only pregnancies with a singleton viable fetus between 16 weeks and 36 weeks and 6 days being considered. We referred the pathologic fetuses towards a specialized obstetrical professional center for appropriate medical management. The gestational age was according to the last menstrual period and adjusted by the crown-rump length obtained during the first-trimester scan. Patients with normal body weight were not included in this study. The Institutional Review Board approved the study protocol and, as a standard requirement, all patients provided signed informed consent for a fetal examination. Fetal scans were performed by two expert sonographers, specialized in obstetric sonography and following the guidelines of the International Society of Ultrasound in Obstetrics and Gynecology(26). In all cases, a VOLUSON e8 (General Electric TM) system with transabdominal (2-6 MHz RAB2-6-D) and endovaginal (4-9 MHz- RCI5-9-D) probes was used. Each fetal scan lasted approximately around 30-40 minutes with no time constraints and, in cases with unfavorable factors, a minimum of three attempts were performed, asking the women to change position or walk for a few minutes. If the examination was incomplete, patients were rescheduled within two weeks for another scan performed by the same sonographer. The reason for the incomplete examination was documented in each sonographic report.
Results
Out of 942 patients admitted to the Avicena Profertis Obstetrics and Gynecology Medical Center for second- and third-trimester scans, who met the inclusion criteria, 385 represented difficult ultrasonography examinations (40.87%). Difficulties were encountered as it follows: 5% due to amniotic fluid quantity, 12.2% due to placental position, 42% due to excess fat tissue, and 40.52% due to fetal position. Excess fat tissue and fetal position represented the vast majority of difficult assessments. The characteristics are reported in Figure 1.
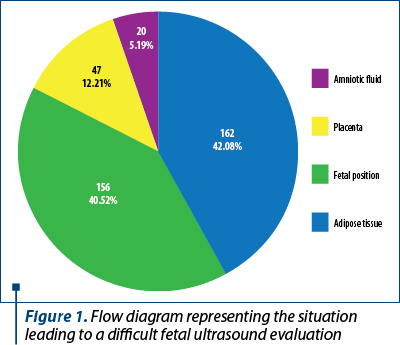
All patients included in our study for fetal ultrasound assessment according to the including criteria were overweight or obese. As shown in Figure 2, we identified that 657 patients (70.27%) were overweight, 201 patients (21.50%) had first-degree obesity, 50 patients (5.35%) had second-degree obesity and 27 patients (2.89%) had third-degree obesity.
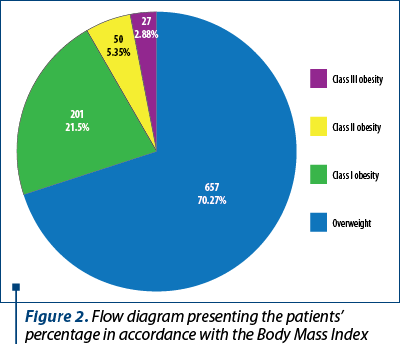
We took into consideration the associated pathologies of our patients that might be caused by overweight or obesity. We identified 132 (14.3%) with added pathologies: 4 patients (3.03%) with gestational diabetes, 26 patients (19.70%) with high blood pressure, 74 patients (56.06%) with thrombophilia, 24 (18.18%) with thyroid pathologies, and 4 (3.03%) with associated infections. The most frequently encountered associated pathology was thrombophilia. The distribution of added pathologies can be seen in Figure 3.
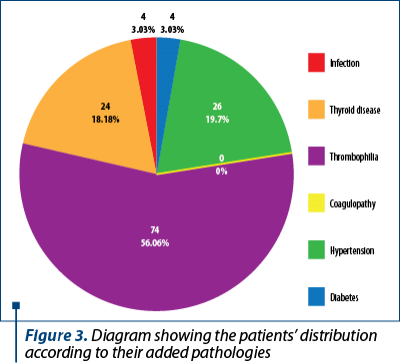
Discussion
According to our study, it is common to encounter difficulties while performing fetal ultrasounds during second and third trimesters in an obese population. Fetal ultrasounds were performed by expert sonographers in a specialized center for prenatal diagnosis following the rules implemented by ISUOG for specialized ultrasounds. In order to provide accurate counseling to pregnant patients, a precise EFW is needed, especially for determining the delivery management. Overestimation or underestimation of EFW before delivery can lead to unnecessary interventions and therefore to perinatal compromise. The inaccuracy associated with the technique while performing fetal ultrasounds in obese pregnant patients represents a major clinical concern(27,28). The first study regarding difficulties encountered while performing fetal ultrasounds in obese patients was released in 1990 by Wolf et al. They managed to analyze data from 1622 examinations performed at a mean gestational age of 28.5 weeks and determined that a maternal BMI higher than the 90th percentile imposed a greater risk of suboptimal fetal visualization(29). Most initial studies focused on identifying problems when fetal scans were done in the first and second trimesters, but lately the challenge consists in obtaining the correct EFW during the third trimester of pregnancy due to the importance it has in the management of delivery. In the present study, patients with a higher BMI imposed significantly higher efforts to obtain an accurate EFW. A considerable number of patients needed multiple fetal ultrasound evaluations, prolonged times of examination and changing position of the patients in order to capture the correct echography parameters. In opposition with the multiple studies that sustain the results of our study, Field et al. and Farrell et al. claim that sonographic EFW results were not affected by maternal obesity. Field et al. analyzed the effect of maternal obesity on the EFW on 998 singleton pregnancies with gestational ages varying from 26 to 43 weeks, whereas Farrell et al. analyzed data from 96 obese patients, randomly selected, who were submitted for induction. The disparities of the results may be due to differences in gestational age, as we now know that EFW is highly influenced by gestational age. Differences on their study might be due to varying study protocols(19,30).
The strength of this study was due to the relatively large data set of pregnant patients with BMI above normal in a population where obesity is increasing on a rapid scale and the fact that all ultrasounds were performed by registered sonographers. As a weakness of our study, we point out the lack of analysis for inaccurate measurement for each sonographic parameter. As cited in the literature and sustained by the Faster study, it was shown that, for second-trimester sonographic markers, maternal obesity led to difficulties in identifying short length humeral and femoral fetal bone and pyelectasis. On the other hand, it was demonstrated that it has not affected the right measurement of the nuchal fold, intracardiac hyperechoic focus or hyperechoic bowels(24).
In 2015, Tsai et al. published a review with the purpose to provide evidence-based perspective on the difficulties experienced while performing fetal ultrasound in obese women. The results showed suboptimal cardiac visualization in 29% of patients with first-degree obesity, in 39% patients with second-degree obesity and in 49% of patients with third-degree obesity. Challenges were seen also when scanning the cranial and vertebrae structures, and difficulties were identified in 37% of patients with first-degree obesity, in 53% of patients with second-degree obesity and in 49% of patients with third-degree obesity. Facial structures were seen with difficulties in 39% of pregnant patients with BMI above normal and the abdominal wall was seen in 3% of patients included in this category. Indeed, our study focused on ultrasounds performed during second and third trimester, but first-trimester ultrasounds should be taken into consideration as well. The same study conducted by Tsai et al. in 2015 showed that, during first-trimester scan, the chances of obtaining an accurate measurement of the nuchal translucency decrease with the increasing of the maternal BMI. It decreases with 3.2% for first- and second-degree obesity and with 7.8% for third-degree obesity. Timing until the correct measurement is obtained is prolonged with 14.1 minutes for second-degree obesity and with 12.3 minutes for third-degree obesity. The necessity of using transvaginal ultrasound is increased with 42% in obese patients, compared to 23% in normal weight pregnant patients(31).
A more recent study performed in 2020 by Simmons et al. on pregnant patients with BMI above normal showed a rate of 90% of incomplete fetal scan in pregnant patients with BMI higher than 50 compared to incomplete fetal scan in 42% of patients with BMI lower than 30(32).
Recent recommendations have been published in order to help sonographers to overcome the challenges of performing ultrasound scans in obese pregnant patients. Benacerraf recommends improving the signal-to-noise ratio by using compound imaging, speckle-reduction filters, pre- and post-processing and the use of tissue harmonics. He also recommends to use umbilicus as acoustic window, sitting up and image above panniculus, sims position and image from flank or groin, transvaginal scan with manipulation of the fetus externally and a full maternal bladder(33). Tsai et al. recommend the implementation of particular technical settings for obese pregnant patients, such as modifying the focus and image contrast, as well as prolonged examination timing with extra 10-15 minutes(32). Weatherborn et al. recommend for the ultrasound examination to be performed between 21 and 22 weeks of gestation(34).
Therefore, we can conclude that the rate of completed anatomic surveys is noticeable reduced in pregnant patients suffering from obesity. As this comorbidity continues to increase in the general population, more research will be needed to correctly asses the challenges of performing fetal scans in this particular category of patients and more recommendations should be brought up, discussed and implemented in rigorous protocols in order to help specialized sonographers to overcome this situation. Overweight female patients during the reproductive period of life and intending to procreate should be informed on the benefits of having a normal weight before achieving a pregnancy.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
Siega-Riz AM, Laraia B. The implications of maternal overweight and obesity on the course of pregnancy and birth outcomes. Matern Child Health J. 2006;10(5 Suppl):S1536.
-
Odgen CL, Carroll MD, Curtin LR, McDowell MA, Tabak CH, Flegal KM. Prevalence of overweight and obesity in the United States, 1999-2004. JAMA. 2006;295(13):1549–55.
-
Castro LC, Avina RL. Maternal obesity and pregnancy outcomes. Curr Opin Obstet Gynecol. 2002;14(6):601–6.
-
Khaskan AS, Kenny LC. The effects of maternal body mass index on pregnancy outcome. Eur J Epidemiol. 2009;24(11):697–705.
-
Heslehurst N, Ells LJ, Simpson H, Batterham A, Wilkinson J, Summerbell CD. Trends in maternal obesity incidence rates, demographic predictors, and health inequalities in 36, 821 women over a 15-year period. Br J Obstet Gynaecol. 2007;114(2):187–94.
-
Statistics Canada. Adult obesity in Canada: measured height and weight. Ottawa (ON): Statistics Canada; 2005. Available at: http://www.statecan.gc.ca/pub/82-620-m/2005001/article/adults adultes/8060-eng.htm. Accesed January 6, 2010.
-
Sebire NJ, Jolly M, Harris JP, et al. Maternal obesity and pregnancy outcome: a study of 287213 pregnancies in London. Int J Obes Relat Metab Disord. 2001;25(8):1175–82.
-
Chu SY, Callaghan WM, Kim SY, et al. Maternal obesity and risk of gestational diabetes mellitus. Diabetes Care. 2007;30(8):2070–6.
-
Cnattingius S, Villamor E, Johansson S, et al. Maternal obesity and risk of preterm delivery. JAMA. 2013;309(22):2362–70.
-
Poobalan AS, Aucott LS, Gurung T, et al. Obesity as an independent risk factor for elective and emergency caesarean delivery in nulliparous women – systematic review and meta-analysis of cohort studies. Obes Rev. 2009;10(1):28–35.
-
Usha Kiran TS, Hemmadi S, Bethel J, et al. Outcome of pregnancy in a woman with an increased body mass indes. BJOG. 2005;112(6):768-72.
-
Leddy MA, Power MI, Schulkin J. The impact of maternal obesity on maternal and fetal health. Rev Obstet Gynecol. 2008 Fall;1(4):170-8.
-
Ramsay JE, Ferrell WR, Crawford L, et al. Maternal obesity is associated with dysregulation of metabolic, vascular, and inflammatory pathways. J Clin Endocrinol Metab. 2002;87(9):4231-7.
-
Moos Mk, Dunlop AL, Jack BW, et al. Healthier women, healthier reproductive outcomes: recommendations for the routine care of all women of reproductive age. Am J Obstet Gynecol. 2008;199(6 Suppl 2):S280-9.
-
Hanson M, Barker M, Dodd JM, et al. Interventions to prevent maternal obesity before conception, during pregnancy and post partum. Lancet Diabetes Endocrinol. 2017;5(1):65-76.
-
Villamor E, Cnattingius S. Interpregnancy weight change and risk of adverse pregnancy outcomes: a population-based study. Lancet. 2006;368(9542):1164-70.
-
Cohen JB, Cohen DL. Cardiovascular and renal effects of weight reduction in obesity and the metabolic syndrome. Curr Hypertens Rep. 2015;17(5):34.
-
American College of Obstetricians and Gynecologists. Fetal growth restriction. Practice Bulletin no. 134. Washington DC, ACOG;2013.
-
Farrell T, Holmes R, Stone P. The effect of body mass index on three methods of fetal weight estimation. BJOG. 2002;109(6):651-7.
-
Kritzer S, Magner K, Warshak CR. Increasing maternal body mass index and the accuracy of sonographic estimation of fetal weight near delivery. J Ultrasound Med. 2014;33(12):2173–9.
-
Goldberg JD. Routine screening for fetal anomalies: expectations. Obstet Gynecol Clin North Am. 2004;31(1):35–50.
-
ISUOG Education Committee recommendations for basic training in obstetric and gynecological ultrasound. Ultrasound Obstet Gynecol. 2014;43(1):113–6.
-
Weichert J, Hartge DR. Obstetrical sonography in obese women: a review. J Clin Ultrasound. 2011;39(4):209–16.
-
Aagaard-Tillery KM, Flint Porter T, Malone FD, et al. Influence of maternal BMI on genetic sonography in the FaSTER trial. Prenat Diagn. 2010;30(1):14–22.
-
Catanzarite V, Delaney K, Wolfe S, et al. Targeted mid-trimester ultrasound examination: how does fetal anatomic visualization depend upon the duration of the scan? Ultrasound Obstet Gynecol. 2005;26(5):521–6.
-
Salomon LJ, Alfirevic Z, Berghella V, et al. Practice guidelines for performance of the routine mid-trimester fetal ultrasound scan. ISUOG Clinical Standards Committee. Ultrasound Obstet Gynecol. 2011;37(1):116–26.
-
Kurmanavicius J, Burkhardt T, Wisser J, et al. Ultrasonographic fetal weight estimation: Accuracy of formulas and accuracy of examiners by birth weight from 500 to 5000 g. J Perinat Med. 2004;32(2):155–61.
-
Dudley NJ. A systematic review of the ultrasound estimation of fetal weight. Ultrasound Obstet Gynecol. 2005;25(1):80–9.
-
Wolfe HM, Sokol RJ, Martier SM, et al. Maternal obesity: A potential source of error in sonographic prenatal diagnosis. Obstet Gynecol. 1990;76(3 Pt1):339–42.
-
Field NT, Piper JM, Langer O. The effect of maternal obesity on the accuracy of fetal weight estimation. Obstet Gynecol. 1995;86(1):102–7.
-
Tsai PJ, Loichinger M, Zalud I. Obesity and the challenges of ultrasound fetal abnormality diagnosis. Best Pract Res Clin Obstet Gynaecol. 2015;29(3):320-7.
-
Simmons P, et al. Accuracy and completion rate of the fetal anatomic survey in the super obese parturient. J Ultrasound Med. 2020;40(10):2047-51.
-
Benacerraf B. The use of obstetrical ultrasound in the obese gravida. Semin Perinatol. 2013;37(5):345-7.
-
Weatherborn M, McGuinness B, Ogamba MI, Leung K, Leftwich HK. Optimal timing of the second trimester fetal ultrasound in the obese gravida. J Matern Fetal Neonatal Med. 2020;1-5. doi:10.1080/14767058.2020.1797667.





