Impactul dializei asupra parametrilor clinici şi paraclinici în insuficienţa renală acută asociată cu sarcina sau cu perioada post-partum
The impact of dialysis on clinical and paraclinical parameters in acute renal failure associated with pregnancy or postpartum period
Abstract
Acute renal injury remains a diagnostic and management challenge, given the low incidence of reported cases. Due to the lack of clear criteria for defining it in pregnancy, the therapeutic strategy and its early onset become important factors in reducing maternal and fetal mortality and morbidity. The aim of this article is to review and correlate data obtained from the literature with those obtained in the Obstetrics and Gynecology Department of the Bucharest University Emergency Hospital over a period of 20 months, discussing the evolution of clinical and paraclinical parameters and the need for dialysis as component part of the therapeutic strategy.Keywords
acute renal injurydialysispregnancyRezumat
Insuficienţa renală acută rămâne o provocare ca diagnostic şi management, având în vedere incidenţa redusă a cazurilor raportate. Luând în considerare lipsa criteriilor clare de definire a acestei patologii în sarcină, strategia terapeutică şi debutul precoce al acesteia devin factori importanţi în reducerea mortalităţii şi morbidităţii materno-fetale. Scopul acestui articol este de a trece în revistă şi a corela datele obţinute din literatura de specialitate cu cele obţinute în cadrul Departamentului de obstetrică-ginecologie al Spitalului Universitar de Urgenţă Bucureşti pe o perioadă de 20 de luni, punând accentul pe evoluţia parametrilor clinici şi paraclinici şi pe necesitatea dializei ca parte componentă a strategiei terapeutice.Cuvinte Cheie
insuficienţă renală acutădializăsarcinăIntroduction
Due to the lack of constant definition criteria, the incidence of acute renal injury is not accurately defined, ranging from 1 in 50 patients to 1 in 20,000 patients in various studies(1,2). Regardless the existing tendency towards an increased incidence (4.5 per 10,000 deliveries), it is estimated that the obstetric causes leading to acute kidney injury are involved in less than one case in 20,000 pregnancies(3-5).
Being defined as a severe and acute reduction in kidney function and manifested by nitrogen retention and oliguria/anuria, the term acute renal failure has been replaced in recent years by acute renal injury, a term that includes both types of injury, structural and functional(6).
A bimodal distribution of the cases with pregnancy-related acute renal injury was reported: an early peak as an outcome of septic abortion, and a second peak, in the second and third trimesters of pregnancy, as a consequence of hypertensive pathology or obstetric complications, such as hemorrhage occurring in placenta praevia, placenta with abnormal adhesion or uterine atony(2).
Thus, the gestational age is correlated with background pathology, but independent of age and comorbidities(7,8).
Having a various underlying etiology, acute renal injury in pregnancy is described as a heterogenous disease, which may sum up renal, prerenal or postrenal causes similar to those in the general population and which can develop at any peripartum time(7,8). Resuming the causal factors, the most common causes that are involved in acute renal failure include preeclampsia, HELLP syndrome, placental abruption, hemorrhage, puerperal sepsis or intrauterine fetal death(1). Acute fatty liver of pregnancy, thrombotic microangiopathies, such as thrombotic thrombocytopenic purpura or atypical hemolytic-uremic syndrome, are rarely associated with renal dysfunction in pregnancy(9).
Acute renal injury during pregnancy is associated with an increased risk of caesarean delivery, placental abruption, uterine atony or disseminated intravascular coagulation. Also, regarding the fetal mortality and morbidity, stillbirths, low gestational age at birth and low birth weight are often found in this pathology(8).
Diagnosis of acute kidney injury in pregnancy
Since there is no consensus on the definition of acute renal injury in pregnancy, the diagnosis is based on the increase in serum creatinine. The following criteria are used in pregnant women: a creatinine level ≥1 mg/dL or a sudden increase of 0.5 mg/dL from baseline in less than 48 hours, oliguria or anuria, or the need to institute dialysis(9,10). Taking into consideration preeclampsia, the most frequent cause which leads to renal dysfunction (about one percent of pregnant women), the American College of Obstetricians and Gynecologists has defined the acute kidney injury as a serum creatinine level >1.1 mg/dL or a double baseline level in the absence of kidney disease(7,8).
Dialysis in acute renal injury
As in the general population, the indications for dialysis in pregnancy are represented by volume overload, metabolic acidosis, uremic encephalopathy, uremic neuropathy, uremic pericarditis or hyperkalemia(9). An increased uremic value is associated with a high risk for prematurity and polyhydramnios. On the other hand, the uteroplacental perfusion may be diminished by the hemodynamic fluctuation induced by hemodialysis, therefore when prescribed in a pregnant woman, the dialysis dose should be increased, with a duration of more than 20 hours per week(11,12).
Also, when the GFR falls below 20 ml/min/1.73 m2, dialysis is recommended, taking care that certain biological parameters are within limits (sodium 135 mEq/L and bicarbonate 25 mEq/L)(13). The need for long-term dialysis may suggest, in association with persistent renal dysfunction, the existence of chronic renal disease or a preexistent hypertension(9,14).
Materials and method
We performed a systematic electronic research using National Center for Biotechnology Information, including PubMed, gathering data that were compared with those obtained from the statistics performed in a research project conducted in the Obstetrics and Gynecology Department of the Bucharest University Emergency Hospital. All the publications used are mentioned in the references section.
We retrospectively evaluated the cases admitted in our department between the 1st of January 2020 and the 31st of October 2021 with a diagnosis of pregnancy-related acute renal injury, taking into account demographic characteristic, biological parameters, risk factors or causal factors and the therapeutic strategy. Patients with a known history of renal disease or autoimmune diseases with renal dysfunction, such as lupus erythematous systemic, were excluded. Also, the cases of acute renal failure associated with septic abortion or extrauterine pregnancy were excluded from the study, along with the patients from whom the informed consent wasn’t obtained. The statistical analysis was performed using Microsoft Excel and all the imaging presented in the article belongs to our department’s collection.
Results
The incidence reported in our study, 4.5 per 1000 pregnant women (18 cases diagnosed with acute renal failure in a lot of 4000 patients), was similar with the one presented in the specialty literature.
The age range was 17-38 years old (mean: 30 ± 4.4). Most patients were primiparous, with no previous abortion (44.44%), and no pregnant woman had a significant personal pathological history. The mean gestational age was 30 weeks (ranging from 22 to 38 weeks).
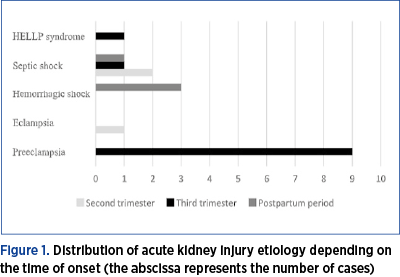
The second trimester, third trimester and postpartum period comprised three cases (16.67%), 11 cases (61.11%) and four cases (22.22%), respectively. Regarding the etiology, most cases of acute renal injury were determined by preeclampsia (50%), followed by septic shock in 22.22% of cases, and hemorrhage shock in 16.67% of cases. The distribution of the etiology depending on the time of occurrence is represented in Figure 1. We must mention that 88.88% of the pregnancies were investigated and the rate of caesarean section was 94.44%, the surgery being performed in all cases within 24 hours of admission.
In terms of neonatal outcome, the mean birth weight was 1610 g, with an Apgar index of 6, with a favorable evolution, except for one case with acute respiratory distress which resulted in fetal death at 48 hours postpartum. We recorded two fetal intrauterine deaths, one associated with maternal septic shock and one associated with placental abruption resulting in uncontrolled hemorrhage.
The number of hospitalization days was between three and 60 days, with an average of 19.6 days. All the patients with more than seven days of hospitalization were admitted to the intensive care unit for vital function monitoring and hemodynamic and electrolytic rebalancing. Regarding the need for acute dialysis, most of the patients (six out of eight patients) who resorted to this therapeutic strategy had an average of 36 days of hospitalization and only one patient required transfer to the nephrology department for long-term dialysis. Among dialysis patients, four cases were not associated with a decreased nitrogen retention value.
Regarding the clinical parameters, most patients had a favorable evolution after the introduction of specific treatment (administration of erythrocyte mass and plasma in case of hemorrhagic shock, antihypertensive treatment in cases with preeclampsia). Also, the febrile syndrome associated with the cases with septic shock was completely remitted within 48 hours after the initiation of antibiotic treatment and the oliguria was remitted after diuretic medication, associated with hydroelectrolytic rebalancing. In six cases (30%), the evolution was burdened by infectious complications (positive urine cultures, especially with Klebsiella pneumoniae). Two cases of hemorrhagic shock and one case of septic shock resulted in maternal death, despite the establishment of hemodynamic rebalancing treatment and specific therapy, including dialysis.
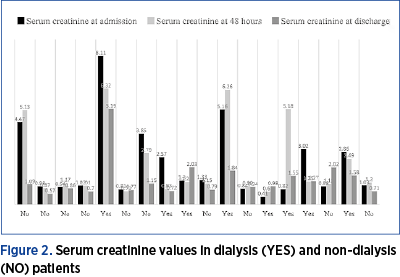
Regarding the paraclinical results, the mean value of serum creatinine at admission was 2.25 mg/dL and the mean value of serum urea was 63.54%. Regarding the evolution, we found that the decrease in creatinine values was below 0.5% at 48 hours and approximately 60.8% at discharge. On the other hand, the serum urea at discharge was with 10.17% lower than at admission. No clear correlation was established between the difference in creatinine values at admission and the one at discharge in relation to the number of days of hospitalization. However, we can establish that a dramatic decrease in values was directly proportional to the number of days of hospitalization, regardless of the therapy used. The difference is substantial between the decreased creatinine values compared to established therapy, without or with dialysis (mean value 0.72 mg/dL versus 2.31 mg/dL). The distribution of serum creatinine values in both dialyzed and non-dialyzed groups is presented in Figure 2.
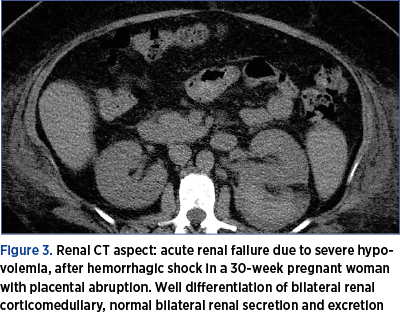
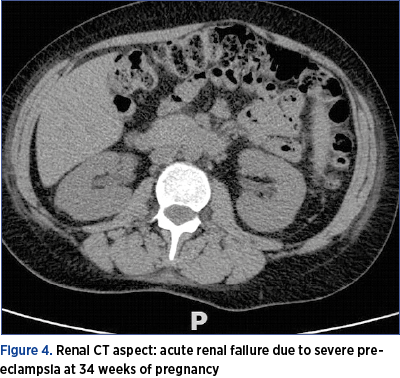
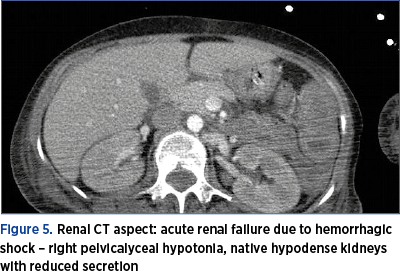
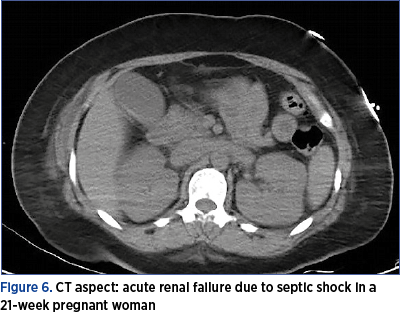
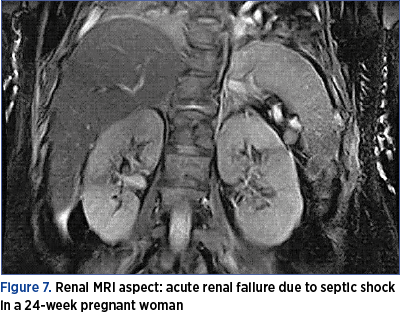
During the hospitalization, in addition to biological follow-up, we performed imaging evaluation, using MRI and CT, to conclude that acute renal failure cannot be primarily assessed by this method, although in most cases it associates tubular necrosis (Figures 3-7).
Discussion
As we mentioned before, the incidence of pregnancy-related acute renal injury was similar to that reported in other studies which describe a range between 3% and 7%(15). Regarding the etiology, most cases involve septic and hemorrhagic shock and in more than 50% of the cases preeclampsia is considered to be the main trigger(16). In our study, in more than half of the cases, the complications of hypertension were involved in triggering the acute renal injury.
The most common age group was 30-35 years old, with a decade older than the group described by Godara et al. in 2017(17).
As for fetal outcomes, the lower mean gestational age at delivery and lower birth weight were mainly caused by the premature birth, given the obstetric complications, and by fetal growth restriction, which brings to the fore the need to draw the attention on the angiogenesis mechanism that can lead to acute renal injury and to uteroplacental unit dysfunction(18).
Maternal mortality was 16.67%, similar with the mortality rate described in a study performed by Goplani et al. in 2008 on a lot of 70 cases of acute renal failure associated with pregnancy complications (18.57%)(19).
Regarding the therapeutic strategy, we concluded that, in our study, dialysis, although it was associated with a high decrease in serum creatinine value, did not improve the length of hospitalization and the mortality rate. None of the cases included in our study presented signs of uremia and all the patients with metabolic acidosis unresponsive to the initial treatment instituted in intensive care unit were included in the dialysis group.
Recommendations for dialysis in pregnancy include: maintaining serum urea below 60 mg/dL (in our study, all the cases with favorable outcome had a value within limits), increasing the frequency of dialysis, and avoiding hypotension, which may affect the fetus(20).
Conclusions
Pregnancy-related acute renal injury treatment includes general measures as the identification of the underlying source, hydroelectrolytical and hemodynamic rebalancing, prompt delivery of the fetus if necessary and, in some cases, the initiation of dialysis. Even though it is rarely necessary, dialysis represents a therapeutic strategy that can improve both maternal and fetal outcomes.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Prakash J, Niwas SS, Parekh A, Pandey LK, Sharatchandra L, Arora P, Mahapatra AK. Acute kidney injury in late pregnancy in developing countries. Renal Failure. 2010 Apr 1;32(3):309-13.
- Acharya A. Management of acute kidney injury in pregnancy for the obstetrician. Obstetrics and Gynecology Clinics. 2016;43(4):747-765.
- Mehrabadi A, Dahhou M, Joseph KS, Kramer MS. Investigation of a rise in obstetric acute renal failure in the United States, 1999-2011. Obstet Gynecol. 2016;127:899–906.
- Resnik R. Creasy and Resnik’s Maternal-Fetal Medicine: Principles and Practice. Philadelphia, MO: Elsevier, 2018.
- Szczepanski J, Griffin A, Novotny S, Wallace K. Acute kidney injury in pregnancies complicated with preeclampsia or HELLP syndrome. Frontiers in Medicine. 2020 Feb 7;7:22.
- Makris K, Spanou L. Acute kidney injury: definition, pathophysiology and clinical phenotypes. The Clinical Biochemist Reviews. 2016;37(2):85-98.
- ACOG Practice Bulletin No. 202: gestational hypertension and preeclampsia. Obstet Gynecol. 2019;133:e1–25.
- Liu D, He W, Li Y, Xiong M, Wang L, Huang J, et al. Epidemiology of acute kidney injury in hospitalized pregnant women in China. BMC Nephrol. 2019 Feb 26;20(1):67.
- Prakash J, Ganiger VC. Acute kidney injury in pregnancy-specific disorders. Indian Journal of Nephrology. 2017;27(4):258.
- Prakash J, Pant P, Prakash S, Sivasankar M, Vohra R, Doley PK, et al. Changing picture of acute kidney injury in pregnancy: Study of 259 cases over a period of 33 years. Indian J Nephrol. 2016;26:262–7.
- Liu Y, Ma X, Zheng J, Liu X, Yan T. Pregnancy outcomes in patients with acute kidney injury during pregnancy: a systematic review and meta-analysis. BMC Pregnancy Childbirth. 2017;17(1):235.
- Krane NK, Hamrahian M. Pregnancy: kidney diseases and hypertension. Am J Kidney Dis. 2007;49(2):336–45.
- Lindheimer M, Conrad K, Umans J. The normal and disease kidney in pregnancy. In: Schrier R, editor. Diseases of the Kidney and Urinary Tract. 8th ed. Vol. 3. Philadelphia, PA: Lippincott Williams and Wilkinson; 2007; 1933
- Drakeley AJ, Le Roux PA, Anthony J, Penny J. Acute renal failure complicating severe preeclampsia requiring admission to an obstetric intensive care unit. Am J Obstet Gynecol. 2002;186(2):253–6.
- Mahesh E, Puri S, Varma V, Madhyastha PR, Bande S, Gurudev KC. Pregnancy-related acute kidney injury: An analysis of 165 cases. Indian Journal of Nephrology. 2017;27(2):113.
- Pahwa N, Bharani R, Kumar R. Post-partum acute kidney injury. Saudi J Kidney Dis Transpl. 2014;25(6):1244–7.
- Godara SM, Kute VB, Trivedi HL, Vanikar AV, Shah PR, Gumber MR, Gumber VM. Clinical profile and outcome of acute kidney injury related to pregnancy in developing countries: a single-center study from India. Saudi Journal of Kidney Diseases and Transplantation. 2014;25(4):906-11.
- van der Graaf AM, Toering TJ, Faas MM, Titia Lely A. From preeclampsia to renal disease: a role of angiogenic factors and the renin–angiotensin aldosterone system?. Nephrology Dialysis Transplantation. 2012;27(suppl_3):51-57.
- Goplani KR, Shah PR, Gera DN, Gumber M, Dabhi M, Feroz A, Trivedi HL. Pregnancy-related acute renal failure: A single-center experience. Indian Journal of Nephrology. 2008;18(1):17.
- Gammill HS, Jeyabalan A. Acute Kidney Injury in Pregnancy. In: Critical Care Nephrology. 2019; 222-234.





