Valoarea predictivă a indicilor Doppler ai arterei uterine la 11-14 săptămâni pentru complicaţiile hipertensive ale sarcinii
The predictive value of 11-14 week uterine artery Doppler indices for hypertensive pregnancy complications
Abstract
Introduction. Hypertensive complications of pregnancy can often lead to serious, even life-threatening situations for the mother and fetus. First-trimester uterine artery Doppler can be a predictive tool for such complications. Materials and method. At the Department of Obstetrics and Gynecology of the Arad County Emergency Clinical Hospital, we examined 305 pregnant patients, from 11 weeks to 13 weeks+6 days gestational age, by ultrasound, both as inpatients and outpatients, and we have assessed the evolution of their pregnancy. Results. There were 21 patients with hypertensive pregnancy complications (6.89%) and 284 patients with normal outcome (93.11%). Three patients had pregnancy-induced hypertension (0.98%), and 18 had preeclampsia (PE; 5.9%), with 12 cases of mild PE (3.95%) and six cases of severe PE (1.97%). The sensitivity for uterine artery PI above the 95th percentile, for uterine artery RI above the 95th percentile, and for uterine artery PI/RI above the 95th percentile was 0%, 0-33.33% and 0%, respectively. The specificity was 94.72-95.03%, 94.98-95.42% and 94.98-95.03%, respectively. The positive predictive value was 0%, 0-13.33% and 0%, respectively. The negative predictive value was 92.76-98.97%, 93.45-99.31% and 92.76-98.97%, respectively. Odds ratios were 0.453-3.966, 1.147-10.286 and 0.453-3.966, respectively. Conclusions. Uterine artery Doppler indices above the 95th percentile during the 11-14 week gestational age offers low to medium detection rates, the best index being the resistivity index.Keywords
pregnancygestational ageuterine artery notchingpreeclampsiascreeningRezumat
Introducere. Complicaţiile hipertensive ale sarcinii pot duce adesea la situaţii grave, chiar cu potenţial letal pentru mamă şi făt. Ecografia Doppler a arterelor uterine în primul trimestru poate fi un instrument predictiv pentru aceste complicaţii. Materiale şi metodă. În Secţia de obstetrică-ginecologie a Spitalului Clinic Judeţean de Urgenţă Arad am examinat 305 paciente gravide, cu vârsta gestaţională de la 11 săptămăni la 13 săptămâni şi 6 zile, atât internate, cât şi ambulatoriu, şi am urmărit evoluţia sarcinii. Rezultate. Un număr de 21 de paciente au avut complicaţii hipertensive (6,89%), iar 284 de paciente au avut o evoluţie normală (93,11%). Trei paciente au avut hipertensiune gestaţională (0,98%) şi 18 au avut preeclampsie (5,9%), cu 12 cazuri de preeclampsie uşoară (3,95%) şi şase cazuri de preeclampsie severă (1,97%). Sensibilitatea pentru IP peste percentila 95, IR peste percentila 95 şi IP/IR peste percentila 95 a fost 0%, 0-33,33% şi, respectiv, 0%. Specificitatea a fost 94,72-95,03%, 94,98-95,42% şi 94,98-95,03%. Valoarea predictivă pozitivă a fost 0%, 0-13,33% şi 0%, iar cea predictivă negativă, 92,76-98,97%, 93,45-99,31% şi 92,76-98,97%. Odds ratio au fost 0,453-3,966, 1,147-10,286 şi 0,453-3,966. Concluzii. Indicii Doppler ai arterelor uterine peste percentila 95 între săptămânile 11 şi 14 de vârstă gestaţională oferă rate de detecţie joase spre medii, cel mai bun fiind indexul de rezistivitate.Cuvinte Cheie
sarcinăvârstă gestaţionalănotch-ul arterei uterinepreeclampsiescreeningIntroduction
Preeclampsia (PE) is one of the leading causes of maternal and fetal mortality and morbidity around the world. The first trimester is the preferred gestational interval for PE screening(1).
The study of Doppler ultrasound flow of maternal uterine arteries in pregnancy provides a useful tool for evaluating the physiology of the maternal-fetal unit(2). The relationship between abnormal uterine artery Doppler flow and several complications of pregnancy is well established(3).
An increased risk of maternal and fetal complications has been reported in women showing an increased resistance to the blood flow in the uterine arteries during pregnancy(4). Pregnancies which result in normal term deliveries show increased diastolic blood flow velocity and loss of the early diastolic notch by 22 weeks of gestation(5).
Doppler velocimetry of the uterine arteries during the first trimester of gestation and its relationship with preeclampsia prediction have been intensely studied(6).
First- and second-trimester uterine artery Doppler blood flow assessments have been shown to have a high predictive value for clinical outcome, with a rather wide range of specificity and sensitivity values for pregnancy complications(7).
Reference ranges for uterine artery Doppler ultrasound indices are recommended to be used during pregnancy screening(8). The pulsatility index (PI) was significantly higher in both trimesters when using transvaginal ultrasound(9-12).
For a correct uterine artery Doppler indices measurement, the gestational age of the patient must be between 11 weeks + 0 days and 13 weeks + 6 days. In case of transabdominal route for ultrasound, a midsagittal section of the uterus and cervical canal should be obtained, the internal cervical os is identified and the transducer should be tilted from side to side in each paracervical region by color flow mapping, in order to identify the uterine arteries(13,14). The sampling gate of the pulsed wave Doppler must be set at 2 mm to cover the whole vessel and the angle of insonation must be less than 30°; blood flow velocity waveforms from the ascending branch of the uterine artery at the closest possible point to the internal os; the PI is to be measured after obtaining at least three similar consecutive waveforms and the mean PI of the arteries is calculated(13,14).
Materials and method
Uterine artery Doppler flow indices were assessed, in a prospective study, on 305 pregnant patients with singleton pregnancies who eventually gave birth vaginally or by caesarean section within the 11 weeks + 0 days and 13 weeks + 6 days gestational ages in our clinic during the 2014-2018 period (as both inpatients and outpatients) by using a Sonoscape SSI-6000 (China) and a General Electric Logiq e (USA) ultrasound devices.
The Doppler flow was analyzed with a 2-mm window and an insonation angle of less than 30 degrees, according to existing guidelines.
The ultrasound results and demographics were recorded and statistically assessed using Microsoft Excel and MedCalc.
Sensitivity, specificity, positive and negative predictive values and odds ratios of bilateral, unilateral and total uterine artery notching for hypertensive pregnancy complications were calculated.
Results
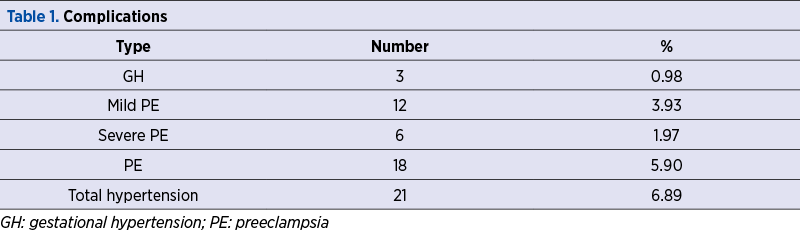
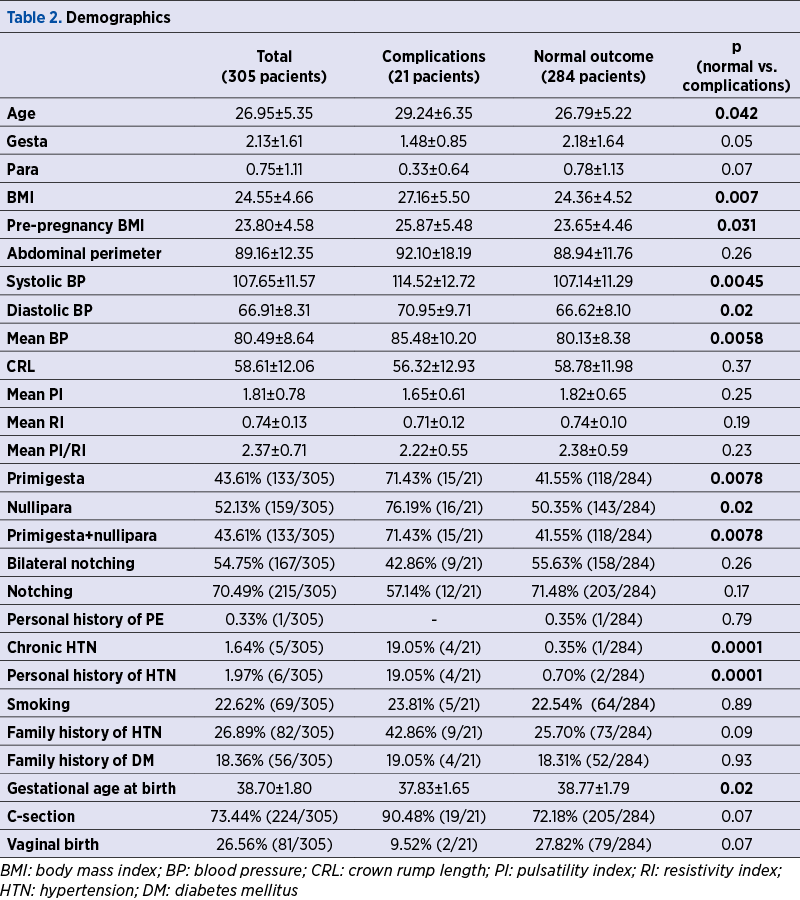
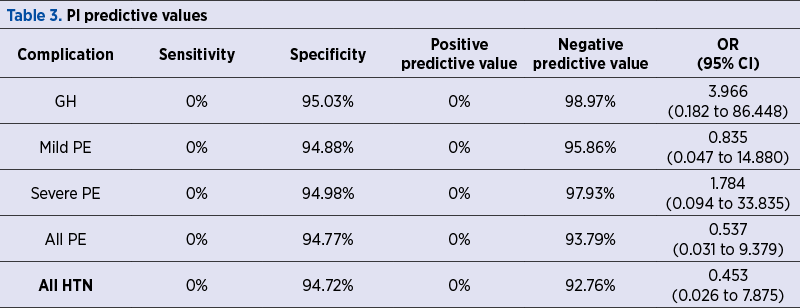
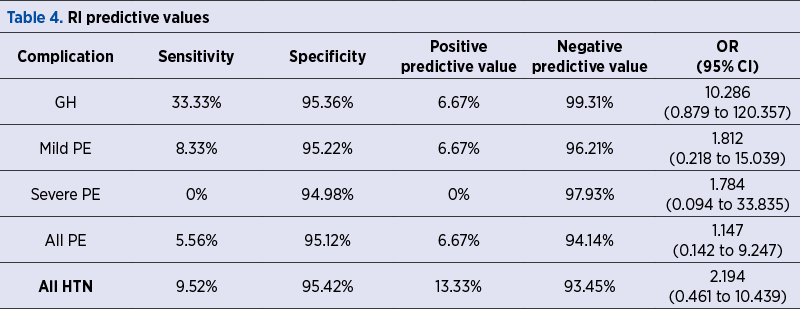
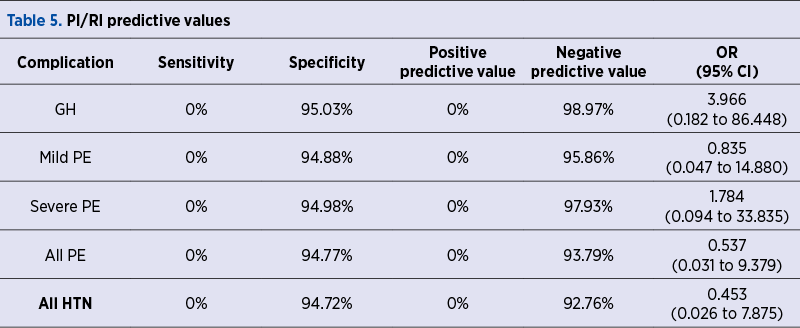
A number of 21 patients in our study group had hypertensive pregnancy complications, which are detailed in Table 1. The demographics of the study group and the statistical significance of the differences between the patients with normal outcome and with hypertensive complications are presented in Table 2. Tables 3, 4 and 5 reveal the sensitivity, specificity, the positive and negative predictive values and odds ratios of PI, RI and PI/RI above the 95th percentile for hypertensive pregnancy complications (RI: resistivity index; GH: gestational hypertension; HTN: hypertension; OR: odds ratio).
Discussion and conclusions
The highest detection rates and positive predictive values were offered by using any type of notching (bilateral and unilateral). The RI revealed the highest specificity, positive and negative predictive value, and odds ratios.
The overall detection rates ranged from 0% to 33.33%, the RI having the highest values.
Positive predictive values were low (0-13.33%), the usefulness of the screening residing in the very high negative predictive values, in addition to the sensitivity.
The main weakness of our study was the relatively low number of patients.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
1. Alves JA, Silva BY, de Sousa PC, Maia SB, Costa Fida S. Reference range of uterine artery Doppler parameters between the 11th and 14th pregnancy weeks in a population sample from Northeast Brazil. Rev Bras Ginecol Obstet. 2013 Aug; 35(8):357-362.
2. Scission A, Hayes E. Uterine artery Doppler Flow studies in obstetric practice. Am J Obstet Gynecol. 2009; 201:121–126.
3. Barati M, Shahbazian N, Ahmadi L, Masihi S. Diagnostic evaluation of uterine artery Doppler sonography for the prediction of adverse pregnancy outcomes. J Res Med Sci. 2014 Jun; 19(6): 515–519.
4. Ghi T, Youssef A, Piva M, et al. The prognostic role of uterine artery Doppler studies in patients with late-onset preeclampsia. Am J Obstet Gynecol. 2009; 201:36 (e1-5).
5. Toal M, Keating S, Machin G, et al. Determinants of adverse perinatal outcome in high-risk women with abnormal uterine artery Doppler images. Am J Obstet Gynecol. 2008; 198:330.e1–330- e7.
6. Plasencia W, Maiz N, Poon L, et al. Uterine artery Doppler at 11 + 0 to 13 + 6 weeks and 21 + 0 to 24 + 6 weeks in the prediction of preeclampsia. Ultrasound Obstet Gynecol. 2008; 32:138-146.
7. Akbaş M, Şen C, Calay Z. Correlation between first and second trimester uterine artery Doppler velocimetry and placental bed histopathology. Int Sch Res Notices. 2014; 890534.
8. Ferreira AE, Mauad Filho F, Abreu PS, Mauad FM, Araujo Junior E, Martins WP. The reproducibility of first and second trimester uterine artery pulsatility index by transvaginal and transabdominal ultrasound. Ultrasound Obstet Gynecol. 2015; 46: 546-52. [CrossRef] J Turk Ger Gynecol Assoc. 2016; 17: 16-20.
9. Peixoto AB, Da Cunha Caldas TM, Tonni G, et al. Reference range for uterine artery Doppler pulsatility index using transvaginal ultrasound at 20-24w6d of gestation in a low-risk Brazilian population. J Turk Ger Gynecol Assoc. 2016 Jan 12; 17(1):16-20.
10. Scandiuzzi RM, de Campos Prado CA, Araujo Júnior E, et al. Maternal uterine artery Doppler in the first and second trimesters as screening method for hypertensive disorders and adverse perinatal outcomes in low-risk pregnancies. Obstet Gynecol Sci. 2016; 59(5):347-356.
11. Ghulmiyyah L, Sibai B. Maternal mortality from preeclampsia/eclampsia. Semin Perinatol. 2012; 36:56-9.
12. Velauthar L, Plana MN, Kalidindi M, Zamora J, Thilaganathan B, Illanes SE, et al. First-trimester uterine artery Doppler and adverse pregnancy outcome: a meta-analysis involving 55,974 women. Ultrasound Obstet Gynecol. 2014; 43:500-7.
13. Poon LC, Syngelaki A, Akolekar R, Lai J, Nicolaides KH. Combined screening for preeclampsia and small for gestational age at 11-13weeks. Fetal Diagn Ther. 2013; 33(1):16-27.
14. Khalil A, Nicolaides KH. How to record uterine artery Doppler in the first trimester. Ultrasound Obstet Gynecol. 2013; 42: 478–479.



