The treatment of breast cancer comprises a broad variaty of antineoplastic drugs, from the classic chemotherapeutic agents such anthracyclines, cyclophosphamide, taxans, 5-fluorouracil, methotrexate, to the targeted therapies like anti-HER2/neu antibody (trastuzumab), tyrosine-kinase inhibitor (lapatinib) and endocrine drugs. These can affect the cardiovascular system, more or less, alone or in combination with other oncologic drugs or radiotherapy. Among them, the anthracyclines are recongnised to have the highest cardiotoxic potential due to their capacity of causing irreversible cardiac injuries. The aim of this review is to briefly present some of the latest published articles that studied the issue of clinical and paraclinical approach of cardiotoxicity during the treatment of breast cancer. A detailed knowledge of the cardiovascular risks and the relevant evaluation methods which can be performed during breast cancer treatment is important in order to prevent or attenuate acute or delayed cardiotoxicity, by adjusting the chemotherapeutic agents’ dose and/or by initiating the appropriate cardioprotective treatment.
Evaluarea cardiotoxicităţii din timpul tratamentului cancerului de sân - actualizare
Update on cardiotoxicity evaluation during the treatment of breast cancer
First published: 20 decembrie 2017
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/OnHe.41.4.2017.1348
Abstract
Rezumat
Tratamentul cancerului de sân cuprinde o varietate de agenţi chimioterapici, de la clasicele citostatice, precum antraciclinele, ciclofosfamida, taxanii, 5-fluorouracilul sau metotrexatul, până la terapiile ţintite, cum sunt anticorpii monoclonali anti-HER2/neu (trastuzumabul), inhibitorii de tirozin-kinază (lapatinib) şi terapia endocrină. Aceştia pot afecta mai mult sau mai puţin sistemul cardiovascular, singuri sau în combinaţie cu alţi agenţi antineoplazici sau cu radioterapia. Dintre aceştia, antraciclinele sunt recunoscute ca având potenţialul cardiotoxic cel mai ridicat, din cauza capacităţii lor de a produce leziuni cardiace ireversibile. Scopul acestui review este să prezinte succint ultimele publicaţii pe tema abordării clinice şi paraclinice a cardiotoxicităţii în perioada tratamentului cancerului mamar. O cunoaştere detaliată a riscului cardiotoxic şi a investigaţiilor relevante ce pot fi efectuate pe parcursul tratamentului cancerului de sân este importantă pentru a putea preveni sau atenua cardiotoxicitatea acută sau tardivă, prin ajustarea dozelor agenţilor citostatici şi/sau iniţierea unei medicaţii cardioprotective eficiente.
Introduction
The treatment of breast cancer is a rapidly evolving field, from the radical mastectomy and classic cytostatic substances to more conserving interventions and targeted adjuvant therapies, leading to the increase of survival rate(1). Thus, according to the National Cancer Institute’s SEER from America, the 5-year relative survival rate is almost 100% in stage 0/I, 93% in stage II, 72% in stage III and 22% in stage IV(2).
Apart from the common side effects such as nausea and vomiting, fatigue, cytopenia, mucositis, diarrhea/constipation(1), a real issue of anticancer therapy is the cardiovascular toxicity(3). Most of the agents from polichemotherapic regimens or the biological agents used in the treatment of mammar cancer are medication with an intermediate and high cardiotoxic related risk, by themselves or when used concomitantly(4). Chemotherapy-related cardiotoxicity (CTRCT) can occur acutely (during or shortly after treatment), early (within first year after treatment) or late (more than one year, median of 7 years after treatment), in some cases even leading to death(3,5,6).
In a prospective cohort study conducted on 5.868 women from Southeast Asia treated for non-metastasized breast cancer, Gernaat et al. showed that a proportion of 6.8% of deaths that occured within 10 years of follow-up were due to cardiovascular diseases, especially acute myocardial infarction. The rate was highest in the first year after diagnosis and increased with older aged(7). Colzani et al. obtained similar results in a study conducted on 12.850 Caucasian women with breast cancer(8).
Pathophysiology of chemotherapy-induced cardiotoxicity
There are two types of cardiotoxicity according to their potential of reversibility:
1. Type 1 cardiotoxicity refers to an injury of the cardiomyocytes. It is considered to be caused by anthracyclines, which generate oxidative free radicals that lead to cellular death and fibrous tissue formation instead. The risk factors are older age (>65 years old), dose (cumulative dose of 300 mg/m2 for doxorubicin, >900 mg/m2 for epirubicin and liposomal anthracyclines)(9) and schedule of infusions, polichemothery regimes including taxans or alkylating agents and molecular therapies, concomitant thorax irradiation and pre-existing cardiovascular conditions. This type of myocardial dysfunction can be recoverd to some degree, if is detected at the beginning of the onset and adequately treated. Otherwise, it becomes irreversible, leading to heart failure(10).
2. Type 2 cardiotoxicity is traditionally associated to trastuzumab. The risk factors are older age, obesity, diabetes, underlying cardiovascular conditions, recently or concomitant treatment with anthracyclines or radiotherapy(6,11). Trastuzumab-induced cardiotoxicity (TIC) ranges from 2% to 7%, but the incidence rises significantly up to 27% when used in combination with other chemotherapic agents like paclitaxel, cyclophosphamide and especially anthracyclines. It develops during the treatment and is normally reversible under appropriate therapy or at drug removal(5,6).
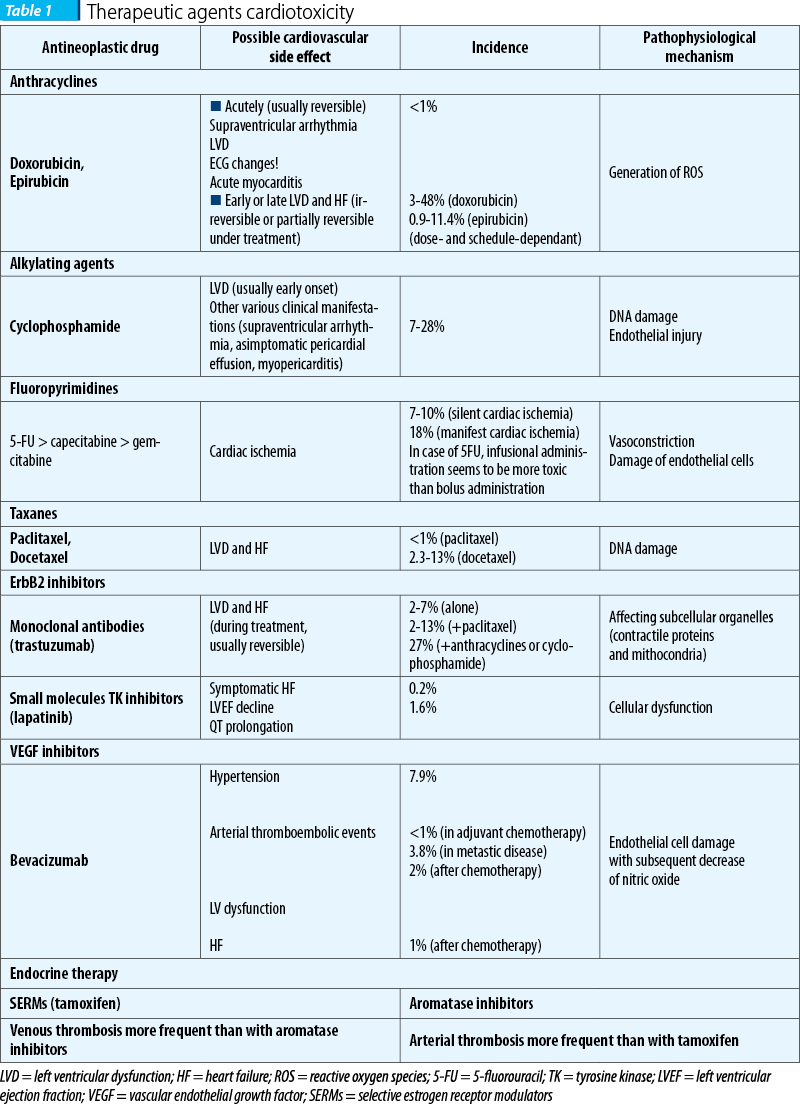
Table 1 provides an overview of the possible cardiovascular damage induced by a range of antineoplastic agents, used in the treatment of breast cancer, and their pathophysiological mechanisms(5,12-16).
Among the classic polichemotherapy regimens used to treat breast cancer, anthracyclines-containing ones are recognised as the most cardiotoxic(17). Anthracyclines have also different cardiotoxicity profiles. It was shown in many meta-analyses that pegylated liposomal anthracycline is as effective as nonliposomal convensional doxorubicin, with the advantages of higher cumulative dose and less toxicity(18-20).
Radiotherapy
Radiotherapy is an integrated step in many breast cancer stages’ treatment, before or after chemotherapy. Although radiation techniques have been improved in the latest years, the heart still receives between 1 and 5 Gy during radiotherapy regimens for breast cancer, a dose which is sufficient to cause pathophysiological changes(21). Radiotherapy exerts cardiotoxic effects by itself and/or by increasing the cardiotoxic potential of certain cytostatic drugs, like anthracyclines.
There are more clinical cardiovascular entities, consequences of radiation exposure at this level. One of the most frequent consequences is pericardial involvement, which can present as an acute impairment, typically with pericardial effusion or between 6 months and 15 years after radiotherapy completion, as a delayed manifestation, including pericarditis, chronic pericardial effusion or pericardial constriction(5,6).
Valvular heart disease is a common sequela after thorax irradiation, with a preponderant involvement of left-sided valves, caused through fibrous thickenig and calcification. Typically, radiation-induced valvular disease does not affect commissures and tips of the mitral valve(22).
Ischemic heart disease can also develop as a result of irradiation of the heart, due to the impairment of cardiac nervous system, manifesting as a silent ischemia or chest pain(6,21).
Assessment and monitoring of cardiac function
1. Risk stratification
Thus far, there is no validated risk score for the risk profile stratification of chemotherapy-induced cardiotoxicity in oncologic patients. A prediction score for the 3-year risk heart failure and cardiomyopathy after adjuvant trastuzumab therapy was proposed by Ezaz et al., that consists of 7 factors: age, adjuvant chemotherapy, coronaropathy, supraventricular arrythmia (fibrillation/flutter), diabetes mellitus, hypertension and renal failure. From echocardiographic parameters, peak velocity of myocardial systolic wave (Sm) (OR=0.4, p=0.002) and Tei index (OR=3.24, p=0.02) were found as independent predictors for patients at high-risk for anthracyclines-induced cardiomiopathy(23). Still, a clinical judgment is needed, considering two main factors: the cardiotoxic potential of the drug and patient-related risk factors(4,6,24).
2. Electrocardiography (ECG) is recommended at the beginning and during treatment for the detection of acute or subacute changes such as arrhythmias, conduction disturbances, repolarization changes, but which are transitory and unrelated to late cardiomyopathy(5).
3. Cardiac imaging (echocardiography, nuclear imaging, cardiac magnetic resonance)
3.1. Transthoracic echocardiography
A great number of studies have been conducted to determine the most appropriate echocardiographic parameters that can predict the onset of myocardial dysfunction from an earlier stage as possible.
According to the last guideline for cardiotoxicity of the European Society of Cardiology (ESC), the two recommended echocardiographic parameters for cardiac monitoring during cardiotoxic cancer treatment are left ventricular ejection fraction (LVEF) and global systolic longitudinal myocardial strain (GLS).
As yet, the most commonly used parameter to evaluate cardiac function during antineoplastic drug administration is LVEF calculated by modified biplane Simpson’s technique, by 2D-echocardiography. For a more precise acquision other imaging tools can be used, but they are not largely available or need specialised operators: 3D-echocardiography, contrast echocardiography, which is indicated in patients with suboptimal echocardiographic view, MUGA (nuclear cardiac imaging) or cardiac MRI. According to the latest European Society of Cardiology Guideline for cardiotoxicity, dependent on LVEF, cardiotoxicity is considered when this decreases >10% with a value below LLN (lower limit of normal) (<50%), confirmed by a repeated cardiac ultrasound at 2 or 3 weeks(6,13). The assessment of LVEF has, though, two major limitations: it practically starts to decrease when myocardial dysfunction is often irreversible, and it cannot detect the heart failure cases with normal LVEF(13,14).
GLS is an echocardiographic parameter measured by speckle tracking echocardiography, which assesses longitudinal deformation of myocardium. It is confirmed to be a very sensitive indicator for CTRCD, as it can detect LVD from a subclinical phase, when it decreases >15% from baseline. However, in asymptomatic patients, the antineoplastic treatment should not be stopped or reduced in dose based if only a GLS decrease is present. Its major limitation is that in daily clinical practice it is not a forthcoming parameter because of technical requirements and inter-vendor variability, being recommended the use of the same equipment for follow-up(5,6,25).
Thus, many echocardiographic markers, from simpler to more complex, were studied in an attempt to find more accessible, appropriate predictive parameters for CTRCD.
Regarding the diastolic function, ASE (American Society of Echocardiography) suggests a comprehensive assessment, given the fact that diastolic dysfunction commonly settles before the sistolic dysfunction in cardiovascular diseases, though there is still not conclusive evidence to support its evaluation role in the prediction of later CTRCD. Diastolic dysfunction is frequently found in cancer patients, but the antineoplastic treatment should not be stopped based on this(5).
Tissue-Doppler Imaging (TDI), a modality that uses Doppler echocardiography for the measurement of myocardial motion(26), was also shown to correlate with subclinical cardiac damage among patients treated for breast cancer(27,28).
E/e` ratio, which assesses left ventricular diastolic function and filling pressures, was shown in some studies to have no significance in predicting early changes, up to 3-6 months of adjuvant therapy with trastuzumab in combination or not with polichemotheray(29,30). Another study, conducted by Alici H et al., found E/e` ratio to be significantly increased (p=0.04) by the reduction in the value of e` (p=0.001), at the end of 6 months treatment with anthracyclines for breast cancer(27).
16-segment resting wall motion score index (WMSI), combined with LVEF, is proved to be a sensitive marker of anthracyclines-CTRCD(28,31).
Another promising parameter is Tei index (myocardial performance index), which sensitively evaluates the global cardiac function and is associated with impaired cardiac function caused by anthracyclines(5) and might be also an indicator of occult 5-FU cardiotoxicity(32).
3.2. Nuclear imaging
123I-MIBG (metaiodobenzylguanidine) scintigraphy. During anthracycline-containing antineoplastic treatments, several studies conducted on rats and on small number of humans showed promising results of this approach in detecting anthracycline-induced cardiomyopathy(33). Regarding trastuzumab-induced cardiotoxicity, Stokkel et al. showed that 123I-MIBG might indicate the reversibility of cardiac impairment(34). However, further investigation is needed in this area to conclude its benefit in monitoring cardiac function during breast cancer treatment, especially because of its cost and radiation exposure.
MUGA (multigated acquisition) scan is a more sensitive and precise tool for the measurement of LVEF, but must be wisely indicated because of the cumulative radiation exposure(6,35).
CMR (cardiac magnetic resonance) is a tool that helps in the accurate detection of chemotherapy-related cardiotoxicity, as it characterizes both the myocardial tissue and vasculature, but it is less used, because of its limited availability and contraindications like ferromagnetic devices (breast tissue exapanders) used for breast reconstruction after mastectomy(6,36).
4. Blood biomarkers
A range of serum markers have been evaluated regarding the prediction of the occurence of cardiac impairment: natriuretic peptides (ANP - atrial natriuretic peptide; BNP - brain natriuretic peptide and its inactive form NT-proBNP), cardiac enzymes (LDH, CK, CK-MB, troponin isoforms I and T, high sensitive troponins I and T) and other biomarkers like (hs)CRP, L-carnitine, nitric oxide, myeloperoxidase, IgE etc. Among these, NT-proBNP and troponins are reported to be the most valuable in assessing CTRCT(37), when used in serial measurements coupled with LVEF assessment(5). Inflammatory markers such as C-reactive protein and pro-inflammatory cytokines cannot be used for cardiotoxicity prediction, as their fluctuations are related to both anti- and proinflammatory responses and are not myocardial-specific. A novel biomarker for doxorubicin and trastuzumab-associated cardiac dysfunction might be IgE, as it is shown in a recent study where higher levels of IgE detected at baseline were associated with lower risk of CTRCT(38).
Screening protocols
There are not standard screening protocols for the cardiovascular assessment during antineoplastic treatment. The optimal methods and the frequency must be chosen considering more factors: the cardiovascular risk profile of the patient, the cardiotoxic potential of oncologic agents and delivery protocol and duration. The recommendations of current guidelines are summarised below.
When anthracycline-containing chemotherapy regimens are used, a proper echocardiographic surveillance should be carried at the beginning of treatment, accompanied by the evaluation of at least one cardiac biomarker. If there is already a myocardiac dysfunction, the chemotherapic regimens options should be discussed or a cardioprotective treatment initiated. If the baseline cardiac assessment is normal, the frequency of follow echocardiographic surveillances might be considered upon the troponin level, which should be measured at each cycle of chemotherapy, knowing that cardiac biomarkers are sensitive tools in identifying early cardiac toxicity. The maintenance of a negative troponin during the treatment requires echocardiographic evaluation at completion of the treatment and then after one year. If troponin level increases, a cardioprotective treatment must be initiated and a closer echographic monitoring should be assessed every 3 months after treatment completion for one year and long term follow-up (echocardiography every 6 months for 5 years). In case of not determining the troponin level during chemotherapy, a close echocardiographic monitoring should be assessed in follow-up. The lenght of follow-up should be decided also depending on the baseline clinical risk, the cumulative dose and the clinical response during chemotherapy.
At Her2/neu positive breast cancer patients, who require additional therapy with trastuzumab, cardiac monitoring should be performed every 3 months during the treatment, at the end of the treatment and then at 6 months, considering also the clinical indications. A significant LVEF decrease implies treatment interruption and echographic reassessment after 3 weeks. When available, GLS combined with troponins measurement are preferred, as it is proven that they can better detect a subsequent LVEF decrease. The measurement of troponin level might help in differentiating a reversible from an irreversible myocardial impairment(6,13,25).
Conclusion
Breast cancer is one of the most frequent types of cancer, with a high probability of long-term survival. The oncologic agents used for its treatment can cause several adverse effects that decrease the quality of life of these patients, cardiovascular morbidities being among the most important ones.
Anthracyclines, widely used in breast cancer due to their effectiveness, are among the most cardiotoxic cytostatic agents. An enhanced carefulness is needed in the subset of Her2/neu-positive patients receiving anthracyclines and trastuzumab, knowing the synergy of these two drugs in cardiotoxicity. The prescription of a comprehensive cardiovascular assessment is therefore necessary in the care of breast cancer patients, pre-, peri- and post-therapy.
Cardiac imaging is the most used tool in the current practice for the identification of cardiotoxicity, the association with biomarkers increasing its utility. This interdisciplinary approach, from a cardio-oncologist perspective, allows the detection of cardiotoxicity from early stages and the initiation of a strategy to avoid developing cardiac sequelae.
Bibliografie
2. https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html
3. Shaini KL, Sharma TD, Konyak W et al., Chemotherapy-Induced Cardiotoxicity, Ind. Med. Gaz., vol. CXLIX, no. 2, pp. 68–74, 2015.
4. Larsen CM and Mulvagh SL. Cardio-oncology: what you need to know now for clinical practice and echocardiography, Echo Res. Pract., vol. 4, no. 1, pp. R33–R41, Mar. 2017.
5. Rosa GM, Gigli L, Tagliasacchi MI et al. Update on cardiotoxicity of anti-cancer treatments, European Journal of Clinical Investigation, vol. 46, no. 3. pp. 264–84, 2016.
6. Zamorano JL, Lancellotti P, Muñoz DR et al. 2016 ESC Position Paper on cancer treatments and cardiovascular toxicity developed under the auspices of the ESC Committee for Practice Guidelines, Eur. Heart J., vol. 37, no. 36, pp. 2768–801, Sep. 2016.
7. Gernaat SAM, Ho PJ, Rijnberg N et al. Risk of death from cardiovascular disease following breast cancer in Southeast Asia: a prospective cohort study, Sci. Rep., vol. 7, no. 1, p. 1365, Dec. 2017.
8. Colzani E, Liljegren A, Johansson A et al. Prognosis of Patients With Breast Cancer: Causes of Death and Effects of Time Since Diagnosis, Age, and Tumor Characteristics, J. Clin. Oncol., vol. 29, no. 30, pp. 4014–4021, Oct. 2011.
9. Chung W-B, Yi J-E, Jin J-Y et al. Early Cardiac Function Monitoring for Detection of Subclinical Doxorubicin Cardiotoxicity in Young Adult Patients with Breast Cancer, J. Breast Cancer, vol. 16, no. 2, p. 178, Jun. 2013.
10. Moudgil R and Haddad H. Chemotherapy-related cardiac dysfunction, Curr. Opin. Cardiol., vol. 32, no. 2, p. 1, Dec. 2016.
11. Jawa Z, Perez R, Garlie L et al. Risk factors of trastuzumab-induced cardiotoxicity in breast cancer, Medicine (Baltimore), vol. 95, no. 44, p. e5195, Nov. 2016.
12. Albini A, Pennesi G, Donatelli F et al. Cardiotoxicity of anticancer drugs: The need for cardio-oncology and cardio-oncological prevention, Journal of the National Cancer Institute. 2010.
13. Curigliano G, Cardinale D, Suter T et al. Cardiovascular toxicity induced by chemotherapy, targeted agents and radiotherapy: ESMO Clinical Practice Guidelines, Ann. Oncol., vol. 23, no. suppl 7, p. vii155-vii166, Oct. 2012.
14. Cardinale D, Colombo A, Lamantia G et al. Anthracycline-Induced Cardiomyopathy, J. Am. Coll. Cardiol., vol. 55, no. 3, pp. 213–220, Jan. 2010.
15. de Forni M, Malet-Martino M, Jaillais P et al. Cardiotoxicity of high-dose continuous infusion fluorouracil: a prospective clinical study, J. Clin. Oncol., vol. 10, no. 11, pp. 1795–801, Nov. 1992.
16. Zambelli A, Della Porta M, Eleuteri E et al. Predicting and preventing cardiotoxicity in the era of breast cancer targeted therapies. Novel molecular tools for clinical issues, The Breast, vol. 20, no. 2, pp. 176–183, Apr. 2011.
17. de Azambuja E, Ameye L, Diaz M et al. Cardiac assessment of early breast cancer patients 18 years after treatment with cyclophosphamide-, methotrexate-, fluorouracil- or epirubicin-based chemotherapy, Eur. J. Cancer, vol. 51, no. 17, pp. 2517–24, Nov. 2015.
18. Xing M, Yan F, Yu S et al. Efficacy and Cardiotoxicity of Liposomal Doxorubicin-Based Chemotherapy in Advanced Breast Cancer: A Meta-Analysis of Ten Randomized Controlled Trials, PLoS One, vol. 10, no. 7, p. e0133569, Jul. 2015.
19. Rom J, Bechstein S, Domschke C et al. Efficacy and toxicity profile of pegylated liposomal doxorubicin (Caelyx) in patients with advanced breast cancer, Anticancer. Drugs, vol. 25, no. 2, pp. 219–224, Feb. 2014.
20. Harris L, Batist G, Belt R et al. Liposome-encapsulated doxorubicin compared with conventional doxorubicin in a randomized multicenter trial as first-line therapy of metastatic breast carcinoma, Cancer, vol. 94, no. 1, pp. 25–36, Jan. 2002.
21. Darby SC, Ewertz M, McGale P et al. Risk of Ischemic Heart Disease in Women after Radiotherapy for Breast Cancer, N. Engl. J. Med., vol. 368, no. 11, pp. 987–998, Mar. 2013.
22. Hering D, Faber L, and Horstkotte D, Echocardiographic features of radiation-associated valvular disease, Am. J. Cardiol., vol. 92, no. 2, pp. 226–30, Jul. 2003.
23. Erdoğan D, Yücel H, Alanoğlu E et al. Can comprehensive echocardiographic evaluation provide an advantage to predict anthracycline-induced cardiomyopathy?, Turk Kardiyol. Dern. Ars., vol. 39, no. 8, pp. 646–53, Dec. 2011.
24. Ezaz G, Long JB, Gross CP et al. Risk Prediction Model for Heart Failure and Cardiomyopathy After Adjuvant Trastuzumab Therapy for Breast Cancer, J Am Hear. Assoc, no. 3:e000472, 2014.
25. Plana JC, Galderisi M, Barac A et al. Expert Consensus for Multimodality Imaging Evaluation of Adult Patients during and after Cancer Therapy: A Report from the American Society of Echocardiography and the European Association of Cardiovascular Imaging, J. Am. Soc. Echocardiogr., vol. 27, no. 9, pp. 911–939, Sep. 2014.
26. Rajapreyar P, Lorenzana A, Prabhu A et al. Tissue Doppler Imaging and Focal, Late-Onset Anthracycline-Induced Cardiovascular Disease in Long Term Survivors of Childhood Cancer: A Research Article, J. Clin. Diagn. Res., vol. 10, no. 8, p. SC01-4, Aug. 2016.
27. Alici H, Balakan O, Ercan S et al. Evaluation of early subclinical cardiotoxicity of chemotherapy in breast cancer, Anadolu Kardiyol. Dergisi/The Anatol. J. Cardiol., vol. 15, no. 1, pp. 56–60, Jan. 2015.
28. Tassan-Mangina S, Codorean D, Metivier M et al. Tissue Doppler imaging and conventional echocardiography after anthracycline treatment in adults: early and late alterations of left ventricular function during a prospective study, Eur. J. Echocardiogr., vol. 7, no. 2, pp. 141–146, Mar. 2006.
29. Lange SA, Ebner B, Wess A et al. Echocardiography signs of early cardiac impairment in patients with breast cancer and trastuzumab therapy, Clin. Res. Cardiol., vol. 101, no. 6, pp. 415–426, Jun. 2012.
30. Honda K, Takeshita K, Murotani K et al. Assessment of left ventricular diastolic function during trastuzumab treatment in patients with HER2-positive breast cancer, Breast Cancer, vol. 24, no. 2, pp. 312–318, Mar. 2017.
31. Bountioukos M, Doorduijn J, Roelandt J et al. Repetitive dobutamine stress echocardiography for the prediction of anthracycline cardiotoxicity, Eur. J. Echocardiogr., vol. 4, no. 4, pp. 300–305, Dec. 2003.
32. Turan T, Agac M, Aykan A et al. Usefulness of Heart-Type Fatty Acid-Binding Protein and Myocardial Performance Index for Early Detection of 5-Fluorouracil Cardiotoxicity, Angiology, vol. 68, no. 1, pp. 52–58, Jan. 2017.
33. Laursen AH, Thune JJ, Hutchings M et al. 123I-MIBG imaging for detection of anthracycline-induced cardiomyopathy, Clin. Physiol. Funct. Imaging, Feb. 2017.
34. Stokkel MPM, de Wit-van der Veen LJ, and Boekhout A. I-123-MIBG myocardial imaging in trastuzumab-based cardiotoxicity: the first experience, Nucl. Med. Commun., vol. 34, no. 1, pp. 19–24, Jan. 2013.
35. Abidov A, Hachamovitch R, and Berman DS. Modern nuclear cardiac imaging in diagnosis and clinical management of patients with left ventricular dysfunction, Minerva Cardioangiol., vol. 52, no. 6, pp. 505–19, Dec. 2004.
36. Hendel RC, Patel MR, Kramer CM et al. ACCF/ ACR/ SCCT/ SCMR/ ASNC/ NASCI/ SCAI/ SIR 2006 Appropriateness Criteria for Cardiac Computed Tomography and Cardiac Magnetic Resonance Imaging, J. Am. Coll. Cardiol., vol. 48, no. 7, pp. 1475–1497, Oct. 2006.
37. Cao L, Zhu W, Wagar EA et al. Biomarkers for monitoring chemotherapy-induced cardiotoxicity, Crit. Rev. Clin. Lab. Sci., vol. 54, no. 2, pp. 87–101, Feb. 2017.
38. Beer LA, Kossenkov AV, Qin L et al. Baseline Immunoglobulin E Levels as a Marker of Doxorubicin- and Trastuzumab-Associated Cardiac Dysfunction, Circ. Res., vol. 119, no. 10, pp. 1135–1144, Oct. 2016.
Articole din ediţiile anterioare
Faslodex in second line of hormonal treatment of advanced breast cancer - case report
Acest caz se referă la o pacientă cu cancer mamar avansat local şi cu metastaze osoase multiple. Pacienta a suferit o intervenţie chirurgicală pali...
A case report of fulminant hepatitis due to docetaxel in breast cancer
Prezentăm cazul unei femei de 57 de ani diagnosticată cu cancer mamar metastatic, fără comorbidităţi, care a avut hepatotoxicitate severă (gradul 4...
Opţiuni terapeutice în cancerul de sân metastatic HER2-pozitiv
Luând în considerare faptul că incidenţa şi mortalitatea prin cancer de sân sunt încă importante în lume, acest tip de neoplasm constituind o probl...
Can we achieve successfully local control by IMRT radiotherapy in the treatment of male breast cancer? A case report
Această prezentare descrie un caz rar de cancer mamar la un pacient de gen masculin, patologie care are o incidenţă mai mică de 1% din toate cazur...