A flare-up case during endodontic retreatment of an upper premolar
Un caz de acutizare în cazul retratamentului endodontic al unui premolar superior
Abstract
A flare-up is an acute exacerbation after the initiation or following the root canal treatment. In some cases, the patient may develop a flare-up due to the penetration or development of the microorganisms into the endodontic space. The main symptom felt by the patient is the pain caused by the clinical manifestation of complex pathologic changes occurred at a cellular level. This article discusses the predisposing conditions represented by insufficient instrumentation and by pushing the remnants out to the root canals, factors that lead to an exacerbation during the root canal retreatment.Keywords
endodontic treatmentflare-uproot canal infectionRezumat
O acutizare reprezintă o exacerbare a simptomatologiei după iniţierea sau în urma tratamentului de canal. În unele cazuri, pacientul poate dezvolta o acutizare din cauza pătrunderii sau dezvoltării microorganismelor în interiorul spaţiului endodontic. Principalul simptom resimţit de pacient este durerea cauzată de manifestarea clinică a unor modificări patologice complexe apărute la nivel celular. Articolul discută condiţiile predispozante reprezentate de instrumentarea insuficientă şi de împingerea resturilor din interiorul canalelor radiculare în teritoriul periapical, factori care conduc la o exacerbare în timpul retratării canalului radicular.Cuvinte Cheie
tratament endodonticacutizareinfecţie endodonticăIntroduction
A flare-up represents an acute exacerbation of an asymptomatic pulp or periapical lesion, after the beginning or during the root canal treatment. The average percentage of incidence of flare-ups was found to be 8.4% and, while one patient may be asymptomatic during or after the treatment, another may have a flare-up(1). The most common causes are the mechanical, chemical or microbial injury to the pulp or periradicular tissues. The etiology of a flare-up is multifactorial and depends on interactions between host’s immunological response, microbial infection and tissues damage. Retreatment cases have a significant higher incidence of flare-ups than conventional cases(2). During retreatment, one may have a tendency to push remnants of gutta-percha, debris of dentine or chemical solvents into the periapical tissues. But the major causative factor has been described as microbial, the microbes being pushed apically during the retreatment process(3,4). Pain is the main symptom, ranging from moderate to severe inter-appointment pain, with or without swelling.
Retreatment cases are frequently associated with a secondary root canal infection by therapy-resistant microbes that could be very difficult to eradicate when compared to primary infection(5,6). For treatment, the clinician must determine if the cause is iatrogenic or microbiologically based. Selecting the appropriate treatment, the pain can be reduced and the correct root canal treatment can be achieved with favorable outcomes for tooth or periapical lesion.
Clinical case
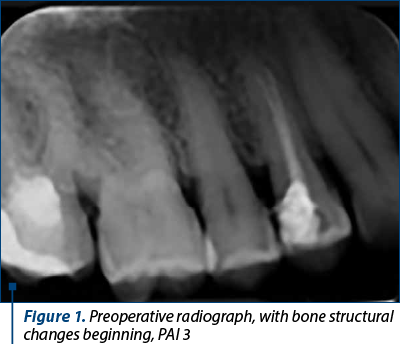
A healthy 38-year-old female presented to the dental office with coronal fracture of first upper premolar. An objective exam revealed a tooth without vitality, no pain during mastication and no fistula. At radiographic examination, there were noted an incomplete root canal filling and some loss of hard periapical tissue, classified as PAI 3 score (Figure 1).
PAI is a visual radiographic index defined by Ørstavik et al. in 1986, consisting of five scores representing a scale from healthy periapical bone to destructive apical periodontitis. Scores 1 and 2 represent healthy periapical bone, and scores 3, 4 and 5 represent apical periodontitis, as follows(7):
-
Score 1 – normal periapical tissues.
-
Score 2 – little bone structural changes, but not apical periodontitis yet.
-
Score 3 – bone structural changes beginning, with some reduced loss, characteristic of apical periodontitis.
-
Score 4 – well-defined radiolucency.
-
Score 5 – radiolucency with high expansions in periapical and adjacent tissues.
We decided to retreat the premolar using rotary instrumentation. After placing the rubber dam, ProTaper Universal Retreatment files were used in crown-down manner at 500 rpm, according to the manufacturer’s recommendations. D1 ProTaper file was used for filling the material removal from the coronal part of root canal, while D2 and D3 files were used for material removal in the medium and apical part, respectively. A brushing movement combined with apical pressure was applied to these files. Only D3 file was applied on the entire working length of root canals.
Retreatment was made without solvents in order not to create a sticky layer on the walls, due to the combination of gutta-percha heated by friction movement and solvent(8). Copious irrigations with 3% sodium hypochlorite after each file was applied. The files have been cleaned before reinsertion in the root canal. When D3 file reached the working length and no filling materials or debris were seen on its surface, the retreatment was considered fulfilled.
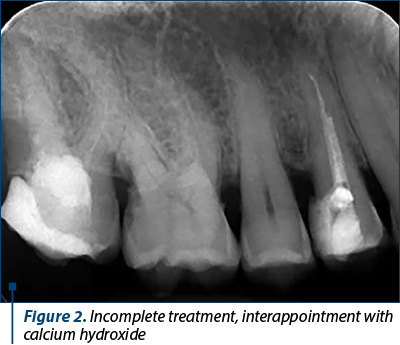
The root canals were finally irrigated using 2% chlorhexidine and dried using paper points. Although we intended a single-visit retreatment, the patient was very anxious, with persistent cough, and we decided to apply an interappointment with calcium hydroxide and Ketac Molar (3M ESPE, Germany) – Figure 2.
After five days, the patient came again to the dental office with mild pain symptoms in the same region and axial percussion sensitivity in tooth 14. No swelling or fistula were noted at the clinical exam. The integrity of coronal restoration was good, with no signs of leakage. The appointment was reserved for emergency procedures: local anesthesia, application of rubber dam, endodontic drainage, copious irrigation with 3% sodium hypochlorite and 2% chlorhexidine, minimal rotary instrumentation using ProTaper Next system (Dentsply Sirona) till X1 instrument (20.04), Ca(OH)2 dressing and temporary sealed coronal filling with Ketak Molar (3M ESPE, Germany). As the drainage was successful, we only gave to the patient general anti-inflammatory and painkiller medication for three days only (ibuprofen 200 mg and paracetamol 500 mg, twice to four times a day).
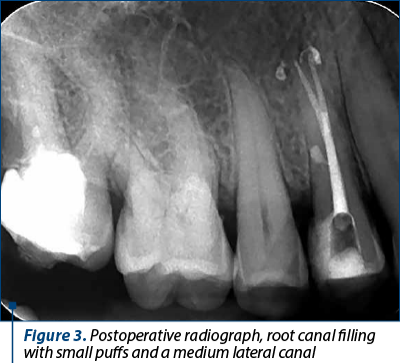
After one week, the pain was gone. In this appointment, the root canal disinfection and chemomechanical preparation have been completed, till X2 instrument (25.06) and apical patency was performed. After copious irrigation with 3% sodium hypochlorite and EDTA 17%, the tooth was filled by continuous wave of condensation using Fi-P (Woodpecker). In the down-pack stage, a master F2 gutta-percha cones were used and the rest of the canals were filled with Fi-G gun in the back-fill stage and AH Plus sealer (Dentsply DeTrey, Germany). The postoperative X-ray revealed a complete root canal filling, with small puffs around the terminus points of the canals and a medium lateral canal (Figure 3).
The patient was referred to prosthetic specialist for final restoration, but was called at six months for checking the results of the retreatment.
Discussion
Retreatment cases are often difficult to treat and one study found an extremely high incidence of flare-ups (13.6%) in cases with chronic apical periodontitis(9). During retreatment, cases with a lot of remnants of gutta-percha or other debris are pushed into the apical tissues and this is probably one of the causes for acute exacerbation of periapical pathosis in our clinical case. Another cause may be the push of microorganisms from the root canal in the periapical area during the retreatment process.
In non-vital teeth associated with a periapical lesion, microorganisms may be at or near the apical foramen and in lateral canals. Correct working length in these cases is essential(10). Over-instrumentation may force infected remnants into the periapical tissues, leading to inflammatory response and pain. On the one hand, apical patency is a controversial procedure(11) but, on the other hand, its lack can lead to clogging the apical constriction and foramen with dirt and mug, and jeopardize the outcome of root canal treatment.
Incomplete instrumentation with ProTaper Retreatment system only in the first appointment might disrupt the balance within the microbial flora and allow previously inhibited species to overgrow(12). In order to avoid increased postoperative pain after root canal filling, the patient had to be postponed until the tooth would be more comfortable, thus increasing the number of appointments. Warm vertical condensation is considered to be a very successful technique because, during these procedures, the residual microorganisms may remain entombed into the well compacted gutta-percha. Also, AH Plus sealer, with an increased flowing rate when temperature rises during continuous wave procedures, seems to be able to fill and seal the dentinal tubules and accessory canals(13).
High levels of stress and anxiety can increase the duration of treatment and healing. Perhaps, the patient should have been more informed about treatment procedures and about sensations experienced during retreatment, in order to have a positive impact in reducing his anxiety.
The combination of ibuprofen/acetaminophen (paracetamol) has been advocated for managing pulpal and periapical pain(14). Especially acetaminophen should be considered for those with sensitivity to NSAIDs, aspirin, or with other disorders like as ulcers, colitis, asthma or hypertension(15). Antibiotics, although frequently wrongly recommended in endodontic patients, were not recommended in this case, with localized endodontic infection and healthy status.
The treatment was directed at the cause of the flare-up. We considered that the main cause was microbiologically based, during the retreatment procedures. Once the tooth has fully instrumented and irrigated in order to eliminate the microbial cause of the problem, working length was confirmed, patency to the apical foramen obtained and root canal filling accomplished, and the outcome of this retreatment has good chances to improve.
Conclusions
The treatment of a flare-up depends upon understanding its biological cause. The causes could be iatrogenic or microbiologically based, as in necrotic cases. The treatment should be directed at the cause of the problem. Pain relief depends on analgesic strategy, and the tooth must be instrumented, irrigated and correctly obturated.
Acknowledgements. For this article, all the authors have equal contributions.
Conflicts of interests: The authors declare no conflict of interests.
Bibliografie
-
Torabinerad M, Kettering JD, McGraw JC, et al. Factors associated with endodontic interappointment emergencies of teeth with necrotic pulps. J Endod. 1988;14:261-266.
-
Walton R, Fouad A. Endodontic interappointment flare-ups: a prospective study of incidence and related factors. J Endod. 1992;18:172-177.
-
Tsesis I, Faivishevsky V, Fuss Z, Zuckerman O. Flare-ups after endodontic treatment: a meta-analysis of literature. J Endod. 2008;14:1177-1181.
-
Baumgartner JC, Rosenberg PA. Treatment of endodontic abscesses/cellulitis, cysts and flare-ups. In: Ingle’s Endodontics 7, PMPH-USA Ltd Raleigh, North Carolina 2019; p. 972-979.
-
Siquera JF, Jr. Aetiology of root canal treatment failure: why well treated teeth can fail. Int Endod J. 2001;34:1-10.
-
Sundqvist G, Figdor D. Life as an endodontic pathogen. Endod Topics. 2003;6:3-28.
-
Ørstavik D, Kerekes S, Eriksen HM. The periapical index: a scoring system for radiographic assessment of apical periodontitis. Endod Dental Traumatol J. 1986;2(1):20-34.
-
Kfir A, Tsesis I, Yakirevich E, Matalon S, Abramovitz I. The efficacy of five techniques for removing root filling material: microscopic versus radiographic evaluation. Int Endod J. 2012;45:35–41.
-
Trope M. Flare-up rate of single-visit endodontics. Int Endod J. 1991;24:24-27.
-
Siquera JF. Reaction of periradicular tissues to root canal treatment. Endod Topics. 2005;10:261-265.
-
Ng YL, Mann V, Gulabivala K. A prospective study of the factors affecting outcomes of nonsurgical root canal treatment: part 1: periapical health. Int Endod J. 2011;44:583–609.
-
Sundqvist G. Ecology of the root canal flora. J Endod. 1992;18:427-430.
-
Venturi M, Pratti C, Capelli G, Falconi M, Breschi I. A preliminary analysis of the morphology of lateral canals after root canal filling using a tooth-clearing technique. Int Endod J. 2003;36: 54-63.
-
Hargreaves KM, Goodis HE, Seltzer S. Pharmacologic control of dental pain. In: Hargreaves KM, Goodis HE, eds. Seltzer and Bender’s Dental Pulp. Chicago: Quintessence Publications, 2002:205-221.
-
Holstein A, Hargreaves KM, Niederman R. Evaluation of NSAID’s for treating post-endodontic pain. Endod Topics. 2002;3:3-13.




