Abordarea modernă a tratamentului paradontitei apicale cronice - review al literaturii
The modern approach to the treatment of chronic apical periodontitis - review of literature
Abstract
This paper reviews the literature on the current concept of the treatment of chronic apical periodontitis. This is an important issue because without adequate endodontic treatment, the infection of the root canal and periradicular tissue may result in loss of supporting apical periodontium and increases the possibility of tooth extraction.Keywords
chronic apical periodontitisconservative endodontic treatmentmodern strategyRezumat
Articolul de faţă trece în revistă literatura de specialitate în privinţa concepţiei actuale despre tratamentul parodontitei apicale cronice. Abordarea endodontică conservatoare reprezintă un aspect important, deoarece fără tratament adecvat infecţia canalului radicular şi a ţesuturilor periapicale poate conduce la distrucţia parodonţiului apical şi la pierderea dintelui prin necesitatea extracţiei dentare.Cuvinte Cheie
parodontită apicală cronicătratament endodontic conservatorstrategie modernăAbbreviations:
- sodium hypochlorite - NaOCl;
- disodium ethylene diamine tetra-acetic acid - EDTA;
- Nickel-titanium - Ni-Ti.
Introduction
Chronic apical periodontitis is an infectious disease caused by bacteria colonizing the necrotic endodontic system(1,2). In order to achieve an optimal outcome of the endodontic treatment, the antibacterial medication is still mandatory, although being considered as having a subordinate role after the root canal cleansing and shaping(3). Its targets are maintaining of the disinfection conditions between the treatment appointments, as well as triggering the re-mineralization process in the apical territory(4). The purpose of this review is to evaluate the literature on modern strategy of the treatment of chronic apical periodontitis.
Modern approach to endodontic treatment in chronic apical periodontitis is based on the following principles of intervention.
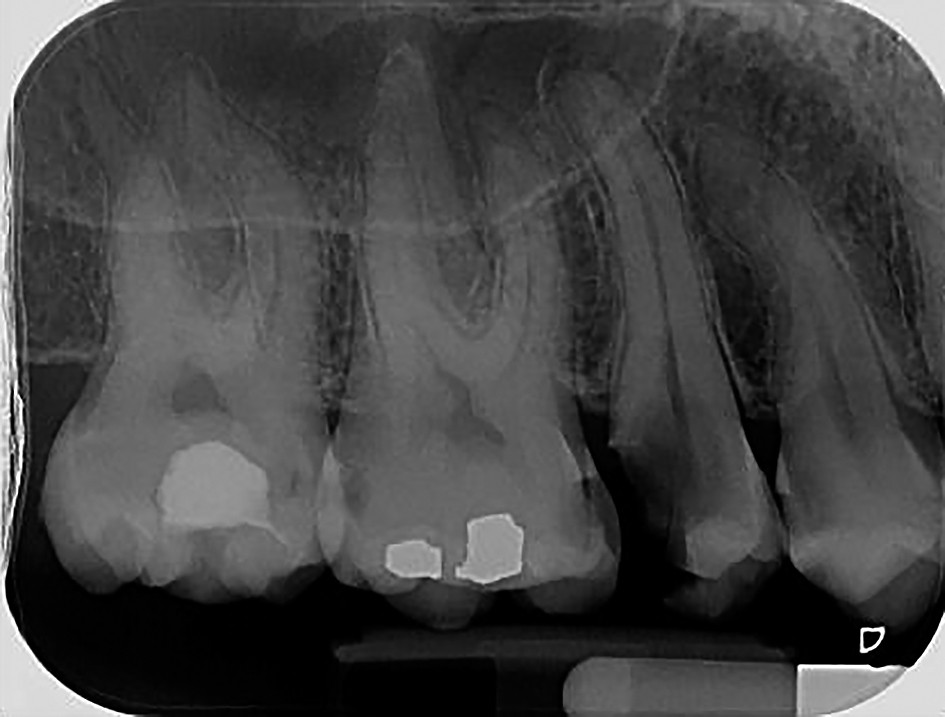
1. Biomechanical treatment of root canals is essential and can not be replaced by any of the subsequent stages of work. Mechanical treatment is performed strictly according to well-known principles of endodontics. Enlarging the root canal is three-dimensional, regardless of the method of preparation, in proportion to their original size and undeflected from the original path. Thus, the final shape of the root canal is concentric to the original form and has an obelisk shape. Currently, biomechanical treatment is done by hand or mechanical way, ultrasonic preparation being no longer approved. It is reserved for activating irrigant solution for 2-3 minutes.
Romanian school of dentistry has a significant contribution in the modern era and believes that the concept of apical enlargement is still insufficiently documented; there are still needed to be determined and individualized both the apical constriction diameter and master apical file(5). In any case, it is essential to avoid repeated passage of the endodontic files through the apical constriction with consequent trauma of periapical tissues(6).
The best instruments for endodontic root canal length measurement and determination of apical constriction diameter are nickel-titanium files due to security, resilience and their flexibility. Nickel-titanium instruments are indicated to be used mainly in the middle third of the root canal where is the highest curvature(7). This area has the advantage of being prepared with these flexible files. Direct reduction of microbial load by using Ni-Ti instruments is the same as those obtained with conventional stainless steel (Kerr files)(8,9). Therefore, have been developed mechanical treatment techniques alternating mechanical instrumentation (Gates-Glidden drills) for the initial portion of the root canals, the middle third with the Ni-Ti hand files and the apical third using the classical Kerr files.
The techniques for biomechanical preparation in endodontic treatment in chronic apical periodontitis are well known: step-back technique, step-down technique and compensated forces technique.
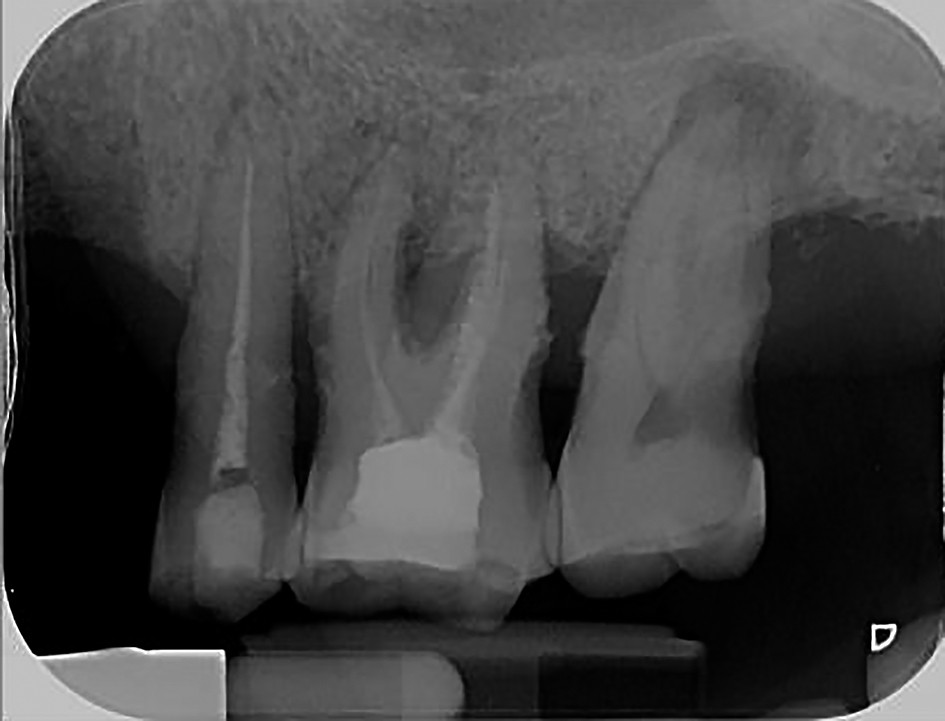
2. It is mandatory to associate endodontic lavages to biomechanical endodontic treatment. The irrigation solution of choice, as stated, is sodium hypochlorite (NaOCl) at a concentration of 1-2.5%, but the most effective way to use it is in combination with a chelator: disodium ethylene diamine tetra-acetic acid (EDTA) 15%(10,11). These two irrigations have complementary effect: the first is effective on necrotic tissue, microorganisms and other organic components within the endodontic system, and the second removes the remaining debris on the root dentin (smear layer) and from the initial portion of the dentinal tubules (smear pluggers). The result is the opening of these ducts. The debris so far is presented as a suspension in the root canal. It is removed by a final lavage with sodium hypochlorite. By removing the smear layer facilitates the diffusion of drug substances through dentinal tubules and ultimately provides a better final seal. Thus, the combined use of NOCl and EDTA is an absolute necessity to any modern biomechanical treatment.
Another positive effect of chelator (EDTA) is that it has a certain antimicrobial activity particularly on Gram+ bacteria, such as, for example, on Streptococcus species(12,13). Lavage solution of sodium hypochlorite generates an effervescent effect, due to which it can penetrate and perform in every irregularity of the root canals and also enter in initial portion of the dentinal tubules.
Nowadays, great emphasis is put on endodontic irrigation technique: use sterile, disposable, blunt needle, 25-30 gauge. Angulation of the needle gets to about 30 degrees so that it can easily penetrate inside the root canal without touching its walls. Important factors in the removal of debris from the endodontic space are the volume and the frequency of the endodontic irrigation: irrigation solution volume is 1-2 ml per washed channel, and this maneuver is preceded by the use of a Ker apical file. This causes release of previously compacted debris in the apical third into the irrigation fluid which helps the removal of the debris. The best results are obtained thus by the synergistic action (additive effect) of sodium hypochlorite solution 2.5%, 2 ml, followed by 2 ml 15% EDTA solution, and the final irrigation sodium hypochlorite (ultrasonic activated for 2-3 minutes).
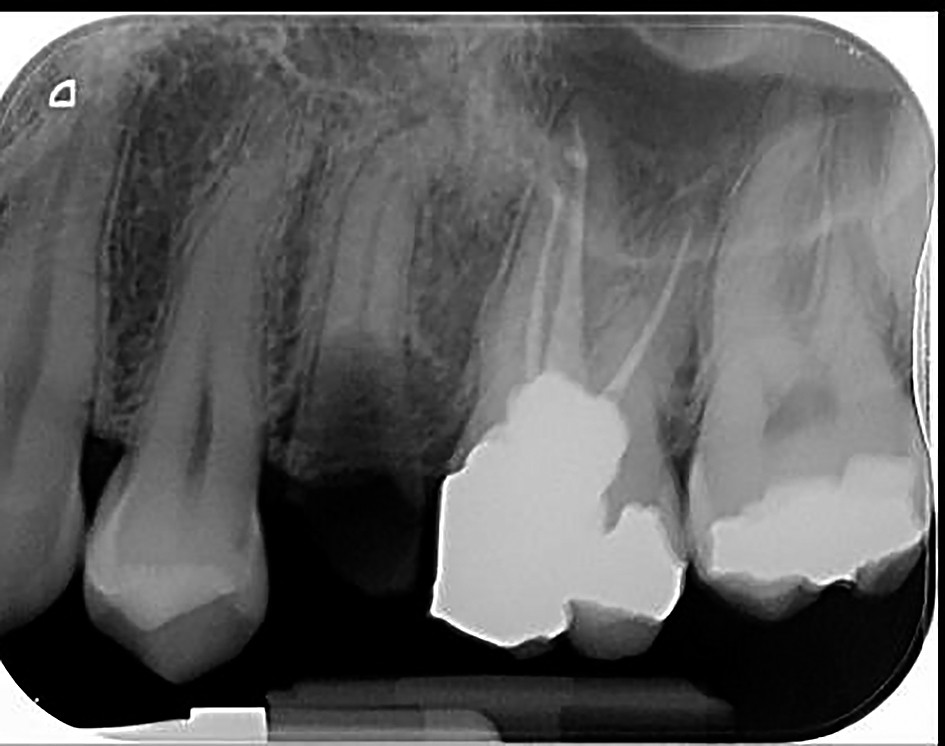
3. Antibacterial endodontic medication in chronic apical periodontitis is established immediately after completion of biomechanical treatment; its targets are to support and the improvement of the disinfection conditions obtained by proper endodontic root canal cleaning and shaping. Endodontic medication is recommended as part of routine endodontic therapy, but is no substitute for effective mechanical preparation, which is the key for a successful endodontic treatment(14,15).
In case of endodontic therapy which extended several sessions, as in chronic apical periodontitis, intracanal medication has the following objectives:
- aid in elimination of endodontic microorganisms which colonize endodontic space(16);
- increases patient’s comfort by reducing inflammation and pain(17);
- removes exudate and controls apical inflammatory bone resorption(18);
- triggers and stimulates periapical bone healing mechanisms (remineralisation process in the periapical territory).
Endodontic microflora, which is the etiological factor of chronic apical periodontitis, is generally sensitive to antimicrobial agents commonly used, even if the treatment susceptibility of different species varies.
Different combinations of antibiotics were tested, in addition to classical compounds with antiseptic and antibiotic group, for example: ciprofloxacin in association with metronidazole and minocycline; spiramycin and metronidazole(19).
The use of topical antibiotics is becoming narrower, being limited to subacute cases which do not permit the application in the first session of a classic antiseptic(20). Currently, the substance of choice for conservative endodontic treatment in chronic apical periodontitis is calcium hydroxide(21). This is the only product that has a long action and can act to induce remineralization and periapical bone healing.
The rules for the use of calcium hydroxide in chronic apical periodontitis are the following:
- short-term routine endodontic medication: calcium hydroxide is placed for 7-10 days into the root canal;
- various types of endodontic medication: calcium hydroxide can be associated with iodo-iodine solution or 2% chlorhexidine gluconate 0.2-0.5%. Chlorhexidine is a broad spectrum antibacterial agent whose effect is mainly due to its molecules, which can be absorbed into dentin and prevent colonization of microorganisms on the surface of the dentin for a given period of time(22). The combination of chlorhexidine and calcium hydroxide is effective on the species of fungi (for example, Candida albicans), otherwise resistant to single calcium hydroxide;
- endodontic medication for specific flora: calcium hydroxide in association with erythromycin (aa); erythromycin is effective on Streptococcus fecalis which is resistant to calcium hydroxide(23); calcium hydroxide in association with amphotericin (it is active on Candida albicans); calcium hydroxide in association with neomycin and metronidazole(24).
The insertion of calcium hydroxide into endodontic space is made in the classic way (Lentullo file, by injection with a syringe with ampoule or by compaction) to complete filling of the root canal, but without exceeding the apical arrest created by biomechanical preparation. The calcium hydroxide paste is first replaced at an interval of about 10 to 14 days, then at every 2-3 months, in order to introduce fresh active substance, until radiographic confirmation of periapical healing or at least its initiation. Radiological images must show increased bone density in the area of radiolucent lesion of chronic apical periodontitis and decrease in its diameter(25).
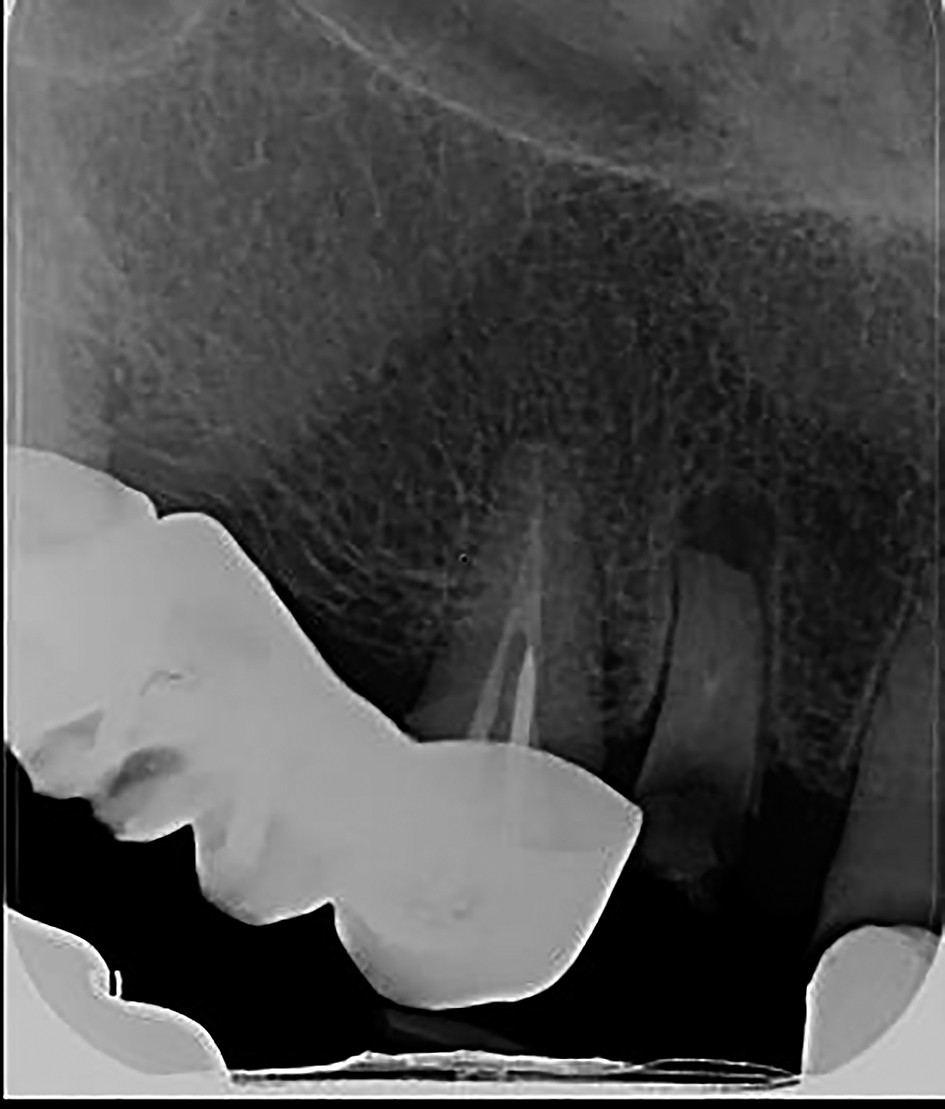
4. Final sealing of the endodontic space contributes to a very large extent to the long-term success or failure of the conservative endodontic treatment.
Currently, none of the well-known classes of endodontic sealants do not fully meet the actual requirements of an ideal root canal filling material. Traditionally, the main effect of root canals sealants was to fill the entire intracanal space, but today the emphasis is on materials that can meet a large number of properties in the same time:
- biocompatibility (low tissue toxicity);
- low solubility in tissue fluid (maintaining the structural integrity of fillings);
- moderate antimicrobial effect;
- biostimulation effect of healing by stimulating the formation of calcified tissue repair in the periapical area.
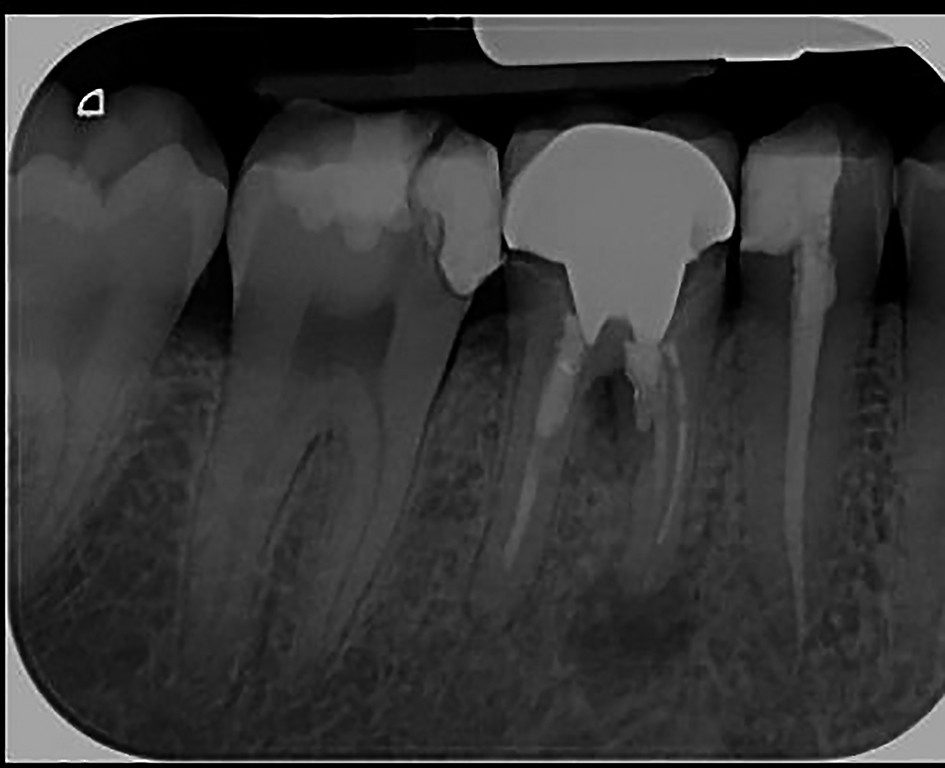
5. Monitoring period of chronic apical periodontitis and parameters which are quantifying the healing process: the modern concept for a tooth with chronic apical periodontitis and conservative endodontic treatment is to be monitored over a period up to 5 years, not for 1-2 years, as it used to be several decades ago(26).
Criteria for assessing the outcome of conservative endodontic treatment are clinical (absence of any symptomatology) in conjunction with radiological (which expresses in an objective way the evolution of the periapical bone lesion) and have been described previously(27).
On the other hand, the results of root canal treatment in chronic apical periodontitis cannot be fully appreciated immediately after its completion. When the endodontic therapy is completed, one can assess the effectiveness partially, the results being considered a success or a failure mostly based on clinical signs.
During the monitoring period, absolutely mandatory for chronic apical periodontitis, radiological criteria are those which primarily lead to a final conclusion on the success of conservative treatment (unless, of course, any clinical symptoms occur). Conservative endodontic treatment is considered a success only if the clinical and radiological criteria for assessing treatment outcome meet(28).
Conclusions
Based on this literature review, it is concluded that the vast majority of chronic apical periodontitis benefit from conservative treatment today. Compared to classical principles of endodontic treatment in chronic apical periodontitis, the changes are not essential. They rather refer to the importance of one or another stage of treatment. Conservative endodontic treatment success in chronic apical periodontitis is actually the result of performing accurately and with responsibility of each mandatory stages of work: rigorous biomechanical treatment, appropriate antibacterial therapy and proper sealing of the endodontic space.
Bibliografie
1. Kovác J, Kovác D. Histopathology and etiopathogenesis of chronic apical periodontitis - periapical granuloma. Epidemiol Mikrobiol Imunol. 2011 Jun; 60(2):77-86.
2. Hommez G, De Moor R. Endodontics and apical periodontitis. Rev Belge Med Dent (1984). 2005; 60(1):9-30.
3. Manzur A, González AM, Pozos A, Silva-Herzog D, Friedman S. Bacterial quantification in teeth with apical periodontitis related to instrumentation and different intracanal medications: a randomized clinical trial. J Endod. 2007 Feb; 33(2):114-8.
4. Trusewicz M, Buczkowska-Radlińska J, Giedrys-Kalemba S. The effectiveness of some methods in eliminating bacteria from the root canal of a tooth with chronic apical periodontitis. Ann Acad Med Stetin. 2005; 51(2):43-8.
5. Gafar M., Iliescu A.: Endodonţie clinică şi practică, ediţia a II-a, Editura Medicală, Bucureşti, 2003: 94-104, 113-130.
6. Tamarut T, Kovacevic M, Glavicic S. Influence of the length of instrumentation and canal obturation on the success of endodontic therapy. A 10-year clinical follow-up. Am J Dent. 2006 Aug; 19(4):211-6.
7. De Rossi A, Silva LA, Leonardo MR, Rocha LB, Rossi MA. Effect of rotary or manual instrumentation, with or without a calcium hydroxide/1% chlorhexidine intracanal dressing, on the healing of experimentally induced chronic periapical lesions. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005 May; 99(5):628-36.
8. Shuping G.B., Orstavik D., Sigurdsson A., Trope M.: Reduction of intracanal bacteria using nickel-titanium rotary instrumentation and various medications. J Endod 2000, 26(12): 751-755.
9. Jiang YT, Xia WW, Liang JP, Ma SF, Yan PF. Quantitative evaluation of residual endodontic microorganisms after mechanical root canal preparation different chemical preparations by real-time PCR. Shanghai Kou Qiang Yi Xue. 2009 Feb; 18(1):10-4.
10. Clegg MS, Vertucci FJ, Walker C, Belanger M, Britto LR. The effect of exposure to irrigant solutions on apical dentin biofilms in vitro. J Endod. 2006 May; 32(5):434-7.
11. Siqueira JF Jr, Magalhães KM, Rôças IN. Bacterial reduction in infected root canals treated with 2.5% NaOCl as an irrigant and calcium hydroxide/camphorated paramonochlorophenol paste as an intracanal dressing. J Endod. 2007 Jun; 33(6):667-72.
12. Fujii R, Saito Y, Tokura Y, Nakagawa KI, Okuda K, Ishihara K. Characterization of bacterial flora in persistent apical periodontitis lesions. Oral Microbiol Immunol. 2009 Dec; 24(6):502-5.
13. Rôças IN, Siqueira JF Jr. Root canal microbiota of teeth with chronic apical periodontitis. J Clin Microbiol. 2008 Nov; 46(11):3599-606.
14. Rôças IN, Siqueira JF Jr, Debelian GJ. Analysis of symptomatic and asymptomatic primary root canal infections in adult Norwegian patients. J Endod. 2011 Sep; 37(9):1206-12.
15. Rôças IN, Siqueira JF Jr. Distribution of Porphyromonas gingivalis fimA genotypes in primary endodontic infections. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010 Mar; 109(3):474-8.
16. Siqueira JF Jr, Rôças IN, Alves FR, Silva MG. Bacteria in the apical root canal of teeth with primary apical periodontitis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009 May; 107(5):721-6.
17. Segura-Egea JJ, Cisneros-Cabello R, Llamas-Carreras JM, Velasco-Ortega E. Pain associated with root canal treatment. Int Endod J. 2009 Jul; 42(7):614-20.
18. Buonavoglia A, Latronico F, Pirani C, Greco MF, Corrente M, Prati C. Symptomatic and asymptomatic apical periodontitis associated with red complex bacteria: clinical and microbiological evaluation. Odontology. 2013 Jan; 101(1):84-8.
19. Sakamoto M, Siqueira JF Jr, Rôças IN, Benno Y. Diversity of spirochetes in endodontic infections. J Clin Microbiol. 2009 May; 47(5):1352-7
20. Jungermann GB, Burns K, Nandakumar R, Tolba M, Venezia RA, Fouad AF. Antibiotic resistance in primary and persistent endodontic infections. J Endod. 2011 Oct; 37(10):1337-44.
21. Liang YH, Zhang G, Wang JD. Clinical effects of calcium hydroxide-based sealer on chronic apical periodontitis. Zhonghua Kou Qiang Yi Xue Za Zhi. 2007 Nov; 42(11):658-62.
22. Bebek B, Bago I, Skaljac G, Plecko V, Miletić I, Anić I. Antimicrobial effect of 0.2% chlorhexidine in infected root canals. Coll Antropol. 2009 Dec; 33(4):1159-63.
23. Ozbek SM, Ozbek A, Erdorgan AS. Analysis of Enterococcus faecalis in samples from Turkish patients with primary endodontic infections and failed endodontic treatment by real-time PCR SYBR green method. J Appl Oral Sci. 2009 Sep-Oct; 17(5):370-4.
24. Lin S, Sela G, Sprecher H. Periopathogenic bacteria in persistent periapical lesions: an in vivo prospective study. J Periodontol. 2007 May; 78(5):905-8.
25. Carrillo C, Penarrocha M, Ortega B, Martí E, Bagán JV, Vera F. Correlation of radiographic size and the presence of radiopaque lamina with histological findings in 70 periapical lesions. J Oral Maxillofac Surg. 2008 Aug; 66(8):1600-5.
26. Yu VS, Messer HH, Shen L, Yee R, Hsu CY. Lesion progression in post-treatment persistent endodontic lesions. J Endod. 2012 Oct; 38(10):1316-21.
27. Ricucci D, Lin LM, Spångberg LS. Wound healing of apical tissues after root canal therapy: a long-term clinical, radiographic, and histopathologic observation study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009 Oct; 108(4):609-21.
28. Heffernan M., Martin W., Norton D.: Prognosis of endodontically treated teeth? Quint Int 2003, 34(7): 558-560.

