Introduction. Anorectal manometry is an objective method used to assess the anorectal function and rectal sensitivity. The purpose of this study was to evaluate the main indications for anorectal manometry in patients admitted to our hospital and to describe the manometric changes noticed in each patients category. Materials and method. From October 2011 to March 2018, a total of 135 patients were examined using conventional anorectal manometry. The measurements of the resting anal pressure and the determination of the recto-anal inhibitory reflex (RAIR) were performed in all children. Maximum squeeze pressure, first rectal sensation, sensations of urge to defecate and critical volume were only determined in children with whom we were able to collaborate. The examined patients were aged between 11 days and 17 years old (14 under 1 year old, 45 with ages between 1 and 4 years old, and 76 aged over 4 years old). Results. We evaluated 116 patients diagnosed with functional constipation, six patients with irritable bowel syndrome (IBS), two patients with Hirschsprung’s disease, six patients with non-retentive fecal incontinence, and five patients were evaluated after surgery for anorectal malformations. The retrospective evaluation of the manometry tracings revealed the absence of the rectoanal inhibitory reflex in four patients. In two of them, Hirschsprung’s disease was confirmed. Out of patients with functional constipation, 52% had a threshold for the sensation of critical volume over 250 cm3. Conclusions. The main indications for the evaluation of pediatric patients using anorectal manometry were the exclusion or confirmation of Hirschsprung’s disease, evaluation of the rectal sensitivity and pressures of the anal sphincter in patients with constipation and/or fecal incontinence, and the anorectal function after surgery in patients with anorectal malformations.
Evaluarea funcţională a tractului digestiv inferior la copii – manometria anorectală
Functional evaluation of the inferior digestive tract in children – anorectal manometry
First published: 18 noiembrie 2019
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Pedi.55.3.2019.2642
Abstract
Rezumat
Introducere. Manometria anorectală este o metodă obiectivă utilizată pentru examinarea funcţiei anorectale şi a sensibilităţii rectale. Scopul acestui studiu a fost evaluarea principalelor indicaţii de efectuare a manometriei anorectale la pacienţii din spitalul nostru şi descrierea modificărilor manometrice decelate la fiecare categorie de pacienţi. Materiale şi metodă. Din octombrie 2011 până în martie 2018 s-au examinat prin manometrie anorectală convenţională 135 de pacienţi. Măsurarea presiunii bazale a sfincterului anal şi determinarea prezenţei sau absenţei reflexului rectoanal inhibitor (RRAI) au fost efectuate la toţi pacienţii examinaţi. La pacienţii cu care s-a putut colabora, s-au determinat şi presiunea anală maximă de contracţie, sensibilitatea rectală la distensie, senzaţia de urgenţă incipientă de defecaţie şi volumul critic. Pacienţii examinaţi au avut vârste cuprinse între 11 zile şi 17 ani (14 cu vârsta sub 1 an, 45 cu vârste între 1 şi 4 ani şi 76 cu vârsta de peste 4 ani). Rezultate. Au fost examinaţi 116 pacienţi având constipaţie funcţională, şase pacienţi cu sindromul intestinului iritabil (SII), doi pacienţi cu boală Hirschsprung, şase pacienţi cu incontinenţă fecală nonretentivă, iar cinci pacienţi au fost evaluaţi postoperatoriu, după intervenţii chirurgicale pentru malformaţii anorectale sau ale colonului. Evaluarea retrospectivă a traseelor de manometrie anorectală a relevat absenţa RRAI în cazul a patru pacienţi, la doi dintre aceştia fiind confirmată boala Hirschsprung. Dintre pacienţii având constipaţie funcţională cu vârsta de peste 4 ani, 52% aveau un prag al volumului critic de peste 250 cm3 aer. Concluzii. Principalele indicaţii de evaluare prin manometrie anorectală a pacienţilor examinaţi au fost: excluderea sau confirmarea bolii Hirschsprung, evaluarea sensibilităţii rectale şi a presiunilor sfincterului anal la pacienţii având constipaţie refractară la tratament şi evaluarea funcţiei anale la pacienţii cu incontinenţă fecală.
Introduction
In the past years, more and more information regarding the colonic and anorectal motility have emerged. Numerous techniques that evaluate the intestinal transit time, colonic and anorectal motility and of the anorectal sensitivity have been developed(1).
The defecation and fecal continence mechanisms are complex processes to which the muscular structures of the anal canal and abdomen contribute with coordinated relaxations and contractions. The passage of the faces in the rectum leads to the involuntary relaxation of the anal sphincter – recto-anal inhibitory reflex (RAIR) – and triggers the sensation of urgency to defecate. The simultaneous contraction of the external anal sphincter and the puborectalis muscles increase the anorectal pressure, prevent the elimination of the faces and reduce the sensation of urgency to defecate. When defecation can take place, the puborectalis muscles and the external anal sphincter relaxe, allowing the evacuation of the faces(2).
Anorectal manometry is an investigation used in children with defecation disorders, since the newborn period, for the evaluation of the rectal and anal motor and sensorial function(3). The main indication is for the assessment of RAIR, in patients with suspicion of Hirschsprung’s disease. It is also indicated for the evaluation of the anal sphincter function in children with fecal incontinence, after surgery in patients with Hirschsprung’s disease or anorectal malformations if they have obstructive symptoms or fecal incontinence, and in children in which biofeedback training is taken into consideration(4).
Constipation is a frequently encountered problem in pediatric gastrointestinal pathology. The worldwide prevalence varies between 0.7% and 29.6%(5). In 95% of the situations, it doesn’t have an organic cause, but fulfills the criteria of a functional disorder. The physiopathology background is the result of a withholding behavior, avoiding defecation, and less frequently of the slow intestinal transit. The onset of the constipation can be triggered in infants by the introduction of complementary food, toddlers by the toilet training and in older children by the avoidance of the defecation in the school toilet. Almost one-third of the children with constipation continue to present symptoms during adolescence, in spite of a correctly conducted and administered treatment(6).
The prevalence of irritable bowel syndrome (IBS) in children, in different countries, varies between 1.2% and 5.4%(7-11). In the Rome IV classification, the difference between functional constipation and IBS manifested with constipation was clarified. Seventy-five percent of the children diagnosed with chronic constipation have abdominal pain, so this criterion, mandatory for the diagnosis of IBS, was creating confusion. It was established that patients should initially be diagnosed with functional constipation and treated as such, and if the abdominal pain persisted in spite of the favorable evolution of constipation, these patients should be diagnosed as having IBS(7).
Anorectal malformations include a large number of congenital anomalies in which the anal sphincter doesn’t normally open at the perineum. Most of the anorectal abnormalities can be anatomically successfully corrected, but functionally some of these patients do not have a good outcome and present fecal incontinence and/or constipation after the surgery(12).
Objective
This study aimed to describe the manometric characteristics of patients with defecation disorders evaluated in our department.
Materials and method
Between October 2011 and March 2018, anorectal manometry was used to evaluate 135 patients aged 11 days and 17 years old. The indications for performing this investigation were constipation and/or fecal incontinence. Patients diagnosed as having a functional gastrointestinal disorder based on Rome III or Rome IV criteria after organic causes of constipation or fecal incontinence have been excluded.
The clinical data were collected from the patients’ files or by giving the parents questionnaires developed based on the Rome III or Rome IV criteria.
One day before and on the day of the investigation, enemas were performed in our patients. Some patients needed sedation with midazolam. For performing the anorectal manometry, we used a water perfused catheter with four channels. The channels open with radially placed holes, which allow the transmission of the pressure through the water. The measured parameters are shown on the computer’s screen in real-time. At the distal end, the anorectal manometry catheter has a balloon which is introduced in the rectum. The pressures are measured from 5 cm of the anal verge (the basal pressure, and in patients with which we could collaborate, the maximum squeeze pressure), then the catheter was progressively withdrawn 1 cm at a time. The anal sphincter was identified this way (the high-pressure zone). The holes of the catheter were then placed at the level of the anal sphincter, and the air was introduced in the balloon (first 10 cm3 air, then 20, 30, 40, and 50 cm3 air) for determining the presence of the RAIR. We determined the rectal sensitivity parameters (rectal distension, initial urge to defecate, critical volume) in older patients.
Results
We evaluated in the aforementioned period 14 patients aged under 1 year old (10.4%), 45 patients aged between 1 and 4 years old (33.3%), and 76 patients older than 4 years of age (56.3%). Twenty patients needed sedation with midazolam.
RAIR was absent in four patients. Two of them – aged 2 years and 11 months, and 5 years and 8 months, respectively – were confirmed as having Hirschsprung’s disease. One of the patients, evaluated at 11 days of life, was first interpreted as having an immaturity of the enteral nervous system, but later Hirschsprung’s disease was confirmed. The fourth patient had an operated anorectal malformation.
In two patients, RAIR was present at high volumes of air introduced in the balloon (40 and 50 cm3 air), but the histopathology exam confirmed the Hirschsprung’s disease.
Of the total number of patients, most of them (116/135; 86%) were diagnosed with chronic constipation. We analyzed the anorectal manometry data of 89 of these patients, and the clinical data of 74 them, the others being patients sent to us from other departments of our hospital. Four patients were aged under 1 year old, 32 were aged between 1 and 4 years old, and 53 were aged over 4 years old. The clinical data of the patients with functional constipation are summarized in Table 1.
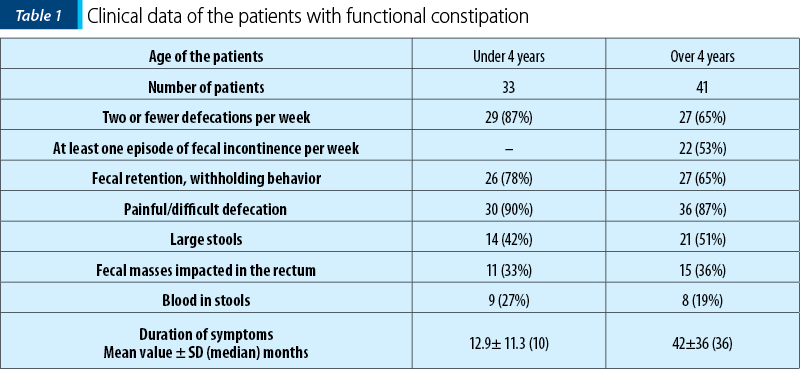
The mean value ±SD of the anal sphincter pressure was 46.5±18 mmHg in children aged less than 1 year old, 46±11 mmHg in children aged between 1 and 4 years old, and 50.6±6.5 mmHg in those older than 4 years. The maximum squeeze pressure of the anal sphincter was only measured in children older than 4 years, and the mean value ±SD was 160±47 mmHg. RAIR was present in all the patients diagnosed with functional constipation.
The sensitivity to rectal distension was measured in 30/53 patients over 4 years of age; mean value ±SD=47.3±35 cm3 air. Eight of the 30 patients (26%) had values over 40 cm3 air.
The sensation of urgency to defecate was determined in 44/53 children over 4 years old, with mean value ± SD = 158.6±85.7 cm3 air; 35/44 (79%) had values over 80 cm3 air. The measurements of the critical volume were performed in 46/53 patients over 4 years old; 27/46 (58%) had values over 250 cm3 air, and mean value ± SD was 286.5±102.4 cm3 air.
In this period, six patients with IBS were evaluated, aged between 6 and 14 years old (mean ± SD=10±3 years). The values of the basal pressure of the anal sphincter and the maximum squeeze pressure were normal. The mean value ±SD of the rectal sensitivity was 30±14 cm3 air. The mean value ±SD of the volumes of air necessary to induce the sensations of urgency to defecate was 83±26 cm3 air, and of the critical volume of 140±56 cm3 air. Only one patient had high values of the rectal sensitivity, and at only one of its parameters, the critical volume (240 cm3 air).
We included in the study six patients with non-retentive fecal incontinence, aged between 5 and 13 years old (mean value ±SD=9±3 years). The values of the basal pressure of the anal sphincter, the maximum squeeze pressure, and the rectal sensitivity features were normal.
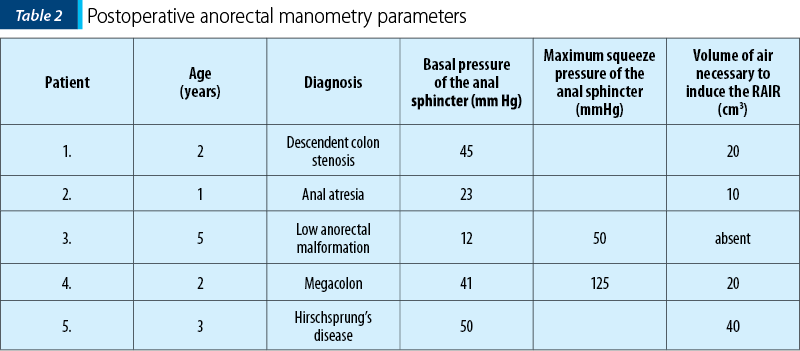
We performed the postoperative evaluation of five patients. The diagnosis for which the surgical procedure was indicated, the age at which anorectal manometry was performed and the evaluated anorectal manometry features are shown in Table 2. The 1-year-old patient in which the surgical intervention was performed for anal atresia and the 5-year-old child in which surgery was indicated for low anorectal malformation had low values of the basal pressure of the anal sphincter.
Discussion
This study aimed to characterize the changes of the anorectal manometric features of some of the defecation disorders diagnosed in our hospital.
The primary mechanism of constipation in children is the retention of the faces in the rectum. Through the colonic mucosa, the water is absorbed from the faces, their consistency increases, and the elimination becomes difficult and painful. A vicious circle is created, and the pain experienced during defecation triggers a withholding behavior, which leads to dilatation of the rectum, fecal incontinence because of the overflow, alteration of the rectal sensitivity and finally the sensation of urge to defecate.
Most patients diagnosed with chronic constipation do not need investigations. For those who have signs and symptoms suggestive of an organic disease or are resistant to conventional therapy, the investigations are aimed to confirm the organic pathology which is suspected or to elucidate the pathophysiologic mechanism leading to constipation(1). Most of the patients with functional constipation evaluated in our department had a long duration of the symptoms (with a mean value of over three years and a mean value of one year in patients younger than 4 years old), resistant or only partially responsive to treatment. Also, more than half of the patients from our department in which we analyzed the clinical data and were aged more than 4 years old had fecal incontinence.
The main change that is brought by the Rome IV classification as opposed to Rome III in the diagnosis of chronic constipation is the shortening of the period in which symptoms must be present in order to make the diagnosis, from two months to one month(7). This change is significant, mainly because it allows starting the treatment earlier, for avoiding the dilatation of the rectum and alteration of the rectal sensitivity. In some situations, it might take even six months to improve rectal sensitivity even after a short period in which the rectum is distended; at that time, the fecal incontinence can reappear(13). Almost 80% of the patients aged over 4 years old included in our study had an altered sensation of urgency to defecate, and more than half tolerated very high volumes of air inflated in the intrarectal balloon, which mimic the faces.
We analyzed the manometric data of six patients diagnosed at the moment of the evaluation with IBS. It is possible that some of the patients we diagnosed as having functional constipation to fit later the criteria of IBS, considering the fact that the new Rome IV criteria mention that patients with functional constipation, correctly treated and with resolution of the symptoms of constipation, but with persistence of the abdominal pain, should be diagnosed as having IBS, manifested predominantly with constipation. IBS is associated with rectal and colonic hypersensitivity(7). Comparing the values of the parameters of the rectal sensitivity in patients with functional constipation with those in IBS patients, there is a significant difference, especially in the volumes of air necessary to induce the sensations of urgency to defecate and critical volume, much higher in patients with functional constipation.
Non-retentive fecal incontinence is characterized by an involuntary loss of faces, in the absence of fecal retention, and is not due to other diseases (such as a neurologic or organic gastrointestinal disease). The changes must be present at least one month (a change from Rome III where they had to be present for at least two months)(7). The parameters of anorectal and colonic manometry and the intestinal transit are normal in these patients.
The postoperative evaluation of the two patients with anorectal malformations (one aged 1 year old, and the other 5 years old) had very low values of the anal basal pressure (also of the maximum squeeze pressure in the 5-year-old patient). These parameters could explain the fecal incontinence. Although from a structural point of view the surgical procedure solves the malformation, the functional deficit can be present in some patients and affects the quality of life.
Conventional anorectal manometry uses water perfused catheters, and the channel holes are radially placed. The radial asymmetry of the anal canal can lead to measuring of different pressure values of the circumference of the anal sphincter/canal. Sedation with benzodiazepines, chloral hydrate or ketamine does not influence the measurements(14). Sedation with propofol reduces the pressure of the anal sphincter(15).
We must mention some limits in our study. It is a retrospective study. We did not evaluate the dynamic of defecation by the expulsion of the balloon from the rectum, a maneuver which could diagnose the dyssynergia of the pelvis. We still use conventional anorectal manometry for the evaluation of defecation disorders, because high-resolution manometry is still not accessible in our hospital. High-resolution manometry would bring more accurate data because the catheters have a much higher number of sensors, which allows a better evaluation of the pressures of different muscular structures of the anal canal.
Conclusions
The main indications for the evaluation with anorectal manometry of our patients were: the exclusion of Hirschsprung’s disease, the evaluation of rectal sensitivity and of the pressures of the anal sphincter in children with constipation refractory to conventional treatment, and the evaluation of the anal function in patients with fecal incontinence. More than half of the patients aged over 4 years old and diagnosed with functional constipation had high values of the sensation of urgency to defecate and critical volume.
Conflict of interests: The authors declare no conflict of interests.
The manuscript has been approved by all authors. The manuscript has not been submitted to another journal at the same time or accepted or published elsewhere.
Bibliografie
- Tambucci R, Quitadamo P, Thapar N, et al. Diagnostic tests in pediatric constipation. JPGN. 2018; 66 (4): e89-e98.
- Le-Carlson M, Berquist W. Anorectal manometry. In: Faure C, Di Lorenzo C, Thapar N (editors). Pediatric neurogastroenterology – gastrointestinal motility and functional disorders in children. Humana Press. 2013; 119-128.
- Rodriguez L, Sood M, Di Lorenzo C, et al. An ANMS-NASPGHAN consensus document on anorectal and colonic manometry in children. Neurogastroenterol Motil. 2016; 29 (1): 1-8.
- Di Lorenzo C, Hillemeier C, Hyman P, et al. Manometry studies in children: minimum standards for procedures. Neurogastroenterol Motil. 2002; 14: 411-20.
- Mugie SM, Di Lorenzo C, Benninga MA. Constipation in childhood. Nat Rev Gastroenterol Hepatol. 2011; 8 (9): 502-11.
- Bongers ME, van Wijk MP, Reisma JB, et al. Long-term prognosis for childhood constipation: clinical outcomes in adulthood. Pediatrics. 2010; 126: e156-62.
- Hyams JS, Di Lorenzo C, Saps M, et al. Childhood functional gastrointestinal disorders: child/adolescent. Gastroenterology. 2016; 150: 1456-68.
- Saps M, Nichols-Vinueza DX, Rosen JM, et al. Prevalence of functional gastrointestinal disorders in Colombian School children. J Pediatr. 2014; 164: 542-545.
- Van Tilburg MAL, Walker L, Palsson O, et al. Prevalence of child/adolescent functional gastrointestinal disorders in a national U.S. community sample. Gastroenterology. 2014; 144 (Suppl 1): S143-S144.
- Devanarayana NM, Mettananda S, Liyanarachchi C, et al. Abdominal pain-predominant functional gastrointestinal diseases in children and adolescents: prevalence, symptomatology, and association with emotional stress. J Pediatr Gastroenterol Nutr. 2011; 53: 659-65.
- Saps M, Adams P, Bonilla S, et al. Parental report of abdominal pain and abdominal pain-related functional gastrointestinal disorders from a community survey. J Pediatr Gastroenterol Nutr. 2012; 55: 707-10.
- Wang Z, Hu L, Jin X, et al. Evaluation of postoperative anal functions using endoanal ultrasonography and anorectal manometry in children with congenital anorectal malformations. J Pediatr Surg. 2016; 51 (3): 416-20.
- Trajanovska M, King SK, Gibb S, Goldfield S. Children who soil: A review of the assessment and management of faecal incontinence. J Paediatr Child Health. 2018; 54 (10): 1136-41.
- Pfefferkorn MD, Croffie JM, Corkins MR, Gupta SK, Fitzegrald JF. Impact of sedation and anesthesia on the rectoanal inhibitory reflex in children. J Pediatr Gastroenterol Nutr. 2004; 38: 324-27.
- Tran K, Kuo B, Zibaitis A, Bhattacharya S, Cote C, Belkind-Gerson J. Effect of propofol on anal sphincter pressure during anorectal manometry. J Pediatr Gastroenterol Nutr. 2014; 58: 495-97.
Articole din ediţiile anterioare
Incontinenţa fecală asociată constipaţiei – cum o putem evita?
Introducere. Incontinenţa fecală asociată constipaţiei (incontinenţă fecală funcţională retentivă – IFFR) reprezintă o problemă majoră, afectân...
Îmbunătăţirea motricităţii fine la copiii cu nevoi speciale utilizând terapia ocupaţională
Terapia ocupaţională încearcă să dezvolte calitatea vieţii oricărei persoane a cărei capacitate funcţională este limitată, acest obiectiv fiind...
Carcinomul corticosuprarenal – evoluţia fatală a unui tip rar de cancer la copil
Carcinomul corticosuprarenal la copii este o tumoră rară, dezvoltată din celulele corticale suprarenale. Un pas foarte important în procesul de d...
Urticaria autoimună
Afecţiunile alergice pot fi considerate boli sistemice, având în vedere polimorfismul simptomelor şi afectarea mai multor organe şi sisteme concomi...