Diabetul gestaţional – o provocare obstetricală, neonatală şi postnatală
Gestational diabetes – an obstetric, neonatal and postnatal challenge
Abstract
In recent decades, the demographics of pregnant women have changed, with an increase of women giving birth at an older age and which, associated with the increase of obesity, has led to a rise in the prevalence of gestational diabetes mellitus (GDM). This has become a global concern and, from a public health perspective, it has huge implications for the mother and the baby. This longitudinal and transversal retrospective study was conducted at the Department of Obstetrics and Gynecology of the “Regina Maria” Hospital – Private Health Network, Bucharest, and included 200 pregnant women who gave birth between 1 July 2021 and 30 June 2022. The patients selected were grouped into two major categories: the study group (100 pregnant women with gestational diabetes), and the control group (100 pregnant women without gestational diabetes). The total number of births in this period was 3807 (out of which 404 patients had gestational diabetes, representing 10.61%). The women were selected based on the following criteria: the glucose tolerance test with 75 g of modified glucose, with clinical exploration (age, Body Mass Index [BMI], hereditary antecedents, associated pathology, type of pregnancy), paraclinical and ultrasound. We included in our study patients of different ages and with different BMI. Women who gave birth to twins or more, with pre-pregnancy diabetes or with unavailable or incomplete case data were excluded from the study. The data used were collected from the patients’ observation documents, birth and operation records, and from the Medis medical information system. Microsoft Excel was used to analyze the data. The aim of the study is to show that having a normal BMI lowers the risks of gestational diabetes, and that patients with obesity have a higher risk of gestational diabetes. We want to demonstrate that there are direct correlations between clinical and paraclinical changes and maternal and fetal complications for pregnant women with gestational diabetes, and that having a good glycemic control is of great importance for the amelioration of pregnancy complications and perinatal conditions.Keywords
gestational diabetesobesitypregnancyBody Mass IndexRezumat
În ultimele decenii, demografia femeilor însărcinate s-a schimbat, observând o creştere a ratei femeilor care nasc la o vârstă mai înaintată şi care, asociată cu creşterea incidenţei obezităţii, a condus la creşterea prevalenţei diabetului gestaţional, devenind o preocupare la nivel global şi, din perspectiva sănătăţii publice, având implicaţii importante pentru mamă şi copil. Acest studiu retrospectiv longitudinal şi transversal a fost realizat la Secţia de obstetrică şi ginecologie a Spitalului „Regina Maria” – Reţea Privată de Sănătate, Bucureşti, şi include 200 de gravide care au născut în perioada 1 iulie 2021 – 30 iunie 2022. Pacientele selectate au fost grupate în două categorii: lotul de studiu (100 de gravide cu diabet gestaţional) şi grupul de control (100 de gravide fără diabet gestaţional). Numărul total de naşteri în această perioadă a fost de 3807 (dintre care 404 paciente au dezvoltat diabet gestaţional, reprezentând 10,61%). Femeile au fost selectate pe baza următoarelor criterii: testul de toleranţă la glucoză cu 75 g de glucoză modificată, cu explorare clinică (vârstă, indice de masă corporală [IMC], antecedente ereditare, patologie asociată, tip de sarcină), paraclinică şi ecografică. Pacientele cu sarcini gemelare sau multiple, cu diabet înainte de sarcină sau cu date de caz indisponibile şi incomplete au fost excluse din studiu. Datele utilizate au fost culese din documentele de observare ale pacientelor, fişele de naştere şi operaţie şi din sistemul de informaţii medicale Medis. Am inclus în studiul nostru paciente de diferite vârste şi cu diferiţi indici de masă corporală. Analiza datelor s-a realizat cu programul Microsoft Excel. Scopul studiului este de a arăta că, având un indice de masă corporal normal, riscul de diabet gestaţional scade, iar pacientele cu obezitate au un risc mai mare de diabet gestaţional. Dorim să demonstrăm că există corelaţii directe între modificările clinice şi paraclinice şi complicaţiile materne şi fetale pentru gravidele cu diabet gestaţional, precum şi faptul că a avea un bun control glicemic este de mare importanţă pentru ameliorarea complicaţiilor sarcinii şi a afecţiunilor perinatale.Cuvinte Cheie
diabet gestaţionalobezitatesarcinăindice de masă corporalăIntroduction
In recent decades, the demographics of pregnant women have changed, with an increase of women giving birth at an older age and which, associated with the increase of obesity, has led to a rise in the prevalence of gestational diabetes mellitus (GDM)(1).
The incidence of gestational diabetes is on the rise due to the sedentary lifestyle, the increase in the prevalence of obesity in women of childbearing age, the increase in the incidence of diabetes in the general population, as well as due to the advanced maternal age. In the 9th Edition of the Diabetes Atlas(2), published in 2019, the estimated global prevalence of GDM is 12.8%.
In 2008, the Hyperglycemia and Adverse Pregnancy Outcome (HAPO) Study recruited a large multinational cohort and brought clarifications on the risks of adverse outcomes associated with hyperglycemia. The findings of the study showed that maternal hyperglycemia independently increased the risk of preterm delivery, caesarean section delivery, infants born large for gestational age, admission to a neonatal intensive care unit, neonatal hypoglycemia and of hyperbilirubinemia(3).
This has become a global concern and from a public health perspective, because it has huge implications for the mother and her baby – it increases the risk of perinatal complications and, at the same time, predicts late, chronic metabolic complications, and sometimes its effects are felt during several generations(4). Among the specific risks of diabetes during pregnancy, we list: spontaneous abortion, preeclampsia, fetal death, macrosomia, fetal anomalies, neonatal hypoglycemia, intrauterine growth retardation, respiratory distress syndrome, complications of natural birth with shoulder dystocia, clavicle fractures, and perineal lacerations(5-7).
The aim of the study is to show that having a normal Body Mass Index (BMI) lowers the risks of gestational diabetes, and that patients with obesity have a higher risk of gestational diabetes. We want to demonstrate that there are direct correlations between clinical and paraclinical changes and maternal and fetal complications for pregnant women with gestational diabetes, and having a good glycemic control is of great importance for the amelioration of pregnancy complications and perinatal conditions.
Materials and method
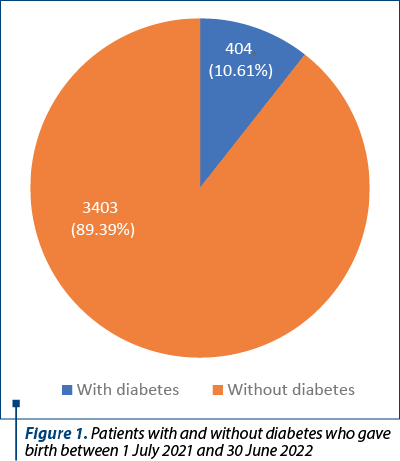
This longitudinal and transversal retrospective study was conducted at the Department of Obstetrics and Gynecology of the “Regina Maria” Hospital – Private Health Network, Bucharest, and included 200 pregnant women who gave birth between 1 July 2021 and 30 June 2022. As shown in Figure 1, the total number of births in this period was 3807 (out of which 404 patients had gestational diabetes, representing 10.61%). This rate is comparable to the average rate of women with diabetes that give birth worldwide(8).
Our sample (200 pregnant women) was divided into two major categories: the study group (100 pregnant women with gestational diabetes), and the control group (100 pregnant women without gestational diabetes).
The pregnant women were selected based on the following criteria: the glucose tolerance test with 75 g of modified glucose, with clinical exploration (age, BMI, hereditary antecedents, associated pathology, type of pregnancy, blood pressure monitoring, pulse, state of health), paraclinical (blood analysis, blood sugar and glucose tolerance test, biophysical score, cardiotocography) and ultrasound (fetal morphologies, growth curve monitoring, with serial measurements of the biparietal diameter, cranial and abdominal circumference, femur length, e.g., Doppler on uterine arteries, umbilical arteries and middle cerebral artery with the measurement of resistance and pulsatility indices) of the group of pregnant women.
The data used were collected from the patients’ observation documents, birth and operation records and from the Medis medical information system. We included in our study patients of different ages and with different BMI. Women who gave birth to twins or more, with pre-pregnancy diabetes and with unavailable or incomplete case data were excluded from the study. Microsoft Excel was used to analyze the data. All pregnant women performed oral glucose tolerance test (OGTT) with 75 g of glucose in weeks 24-28 of gestation. The test consisted in performing OGTT in the morning after overnight fast of ≥8 hours, with 75 g OGTT with plasma glucose (PG) measurement fasting, 1-hour and 2-hour. Patients who had at least one modified value from the ones below have been considered in the GDM group: fasting serum glucose of 92 mg/dl (5.1 mmol/l), 1-hour serum glucose of 180 mg/dl (10 mmol/l), 2-hour serum glucose of 153 mg/dl (8.5 mmol/l)(9).
There are different opinions regarding the testing procedures: ADA guidelines recommend selective screening of high-risk women for GDM, whereas ACOG guidelines and NICE guidelines recommend universal screening (for all women). All women had biochemical tests and ultrasound examination in the first, second and third trimesters of pregnancy.
Patients diagnosed with gestational diabetes initially received routine care, and those who could not achieve glycemic control with diet alone were advised to take insulin by diabetologists.
The glycemic control has a great importance in treating patients with GDM and in preventing pregnancy-related complications. However, research on the correlation between glycemic control and pregnancy outcomes, maternal health and newborn health is limited(10).
Results
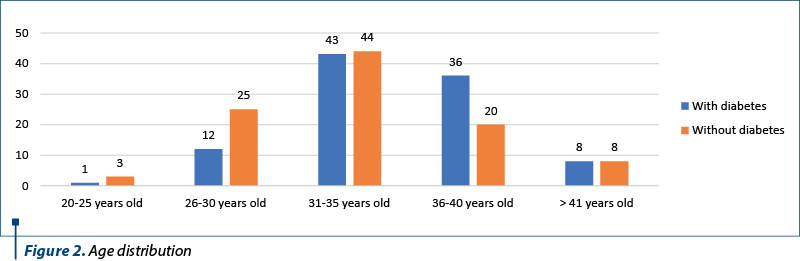
We included in our analysis patients within different age categories, and we noticed that most women gave birth between 31 and 40 years old (71.5%). If we consider only patients from the study group (patients with diabetes), 79% of the women are included in this age category. The number of births drastically decreased after the age of 41, for both groups.
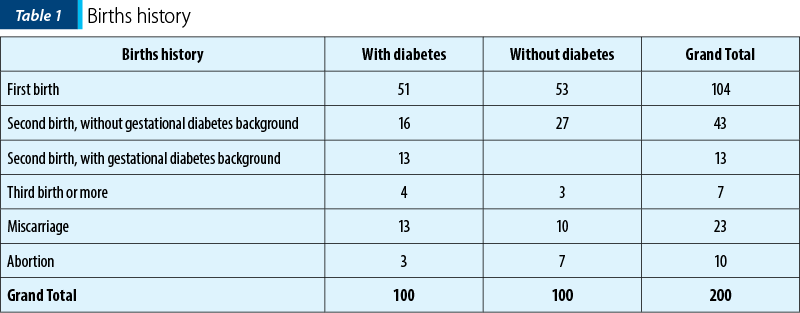
For 52% of the women, this was the first time when they gave birth, while 28% were at the second birth, and 3.5% at the third birth or more. Also, 16.5% of the women had a previous miscarriage or abortion.
In the study group particularly, 51% of diabetic patients gave birth for the first time, 29% for the second time (and almost half of them, 13 out of 29 patients, had diabetes in their first pregnancy) and 4% had three or more births; 16% of them had a previous miscarriage or abortion.
Of the total number of 200 patients, 138 (69%) had under normal or normal BMI at the beginning of the pregnancy (initial BMI), and in 62 patients (31%) their prenatal BMI exceeded the normal range – 41 patients were overweight (20.5%) and 21 patients were obese (10.5%).
Comparing the initial and the final BMI (during the pregnancy) for the two groups together (the study group and the control group), we noticed that:
-
During the pregnancy, only 42 patients kept the initial underweight and normal BMI (representing 21%); from this group, the number of patients without diabetes was 28 versus 14 patients with diabetes; this means that having a normal BMI at the beginning and during the pregnancy lowered by 200% the risks of GDM.
-
Patients who were overweight and had obesity as initial BMI had a higher rate of gestational diabetes (53 patients with diabetes versus nine patients without diabetes).
-
Patients with obesity (at different stages) as final BMI (no matter the initial BMI) have a 77.20% risk to develop gestational diabetes (44 patients out of 57).
If we consider only the study group (patients with diabetes), 53 patients had the initial BMI in the overweight and obesity category. The number of patients with initial under normal and normal BMI was 47, but during the pregnancy, only 14 patients kept their BMI in the normal range, while the others moved to overweight (27 patients) and obesity (seven patients) categories.
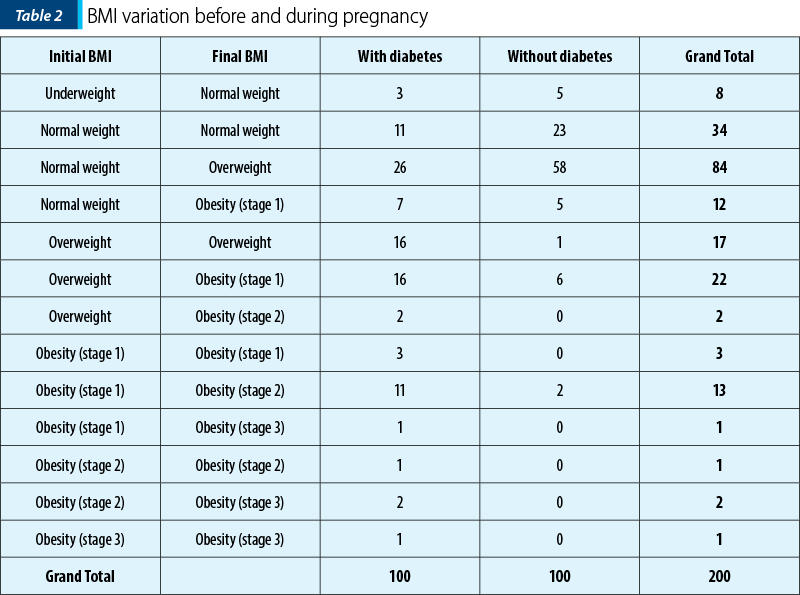
In the control group, we had nine patients with BMI in the overweight and obesity category. Ninety-one patients had initial underweight and normal BMI and, during the pregnancy, 27 patients remained in the normal BMI category, 58 patients moved to overweight BMI, and five patients moved to obesity stage 1 category.
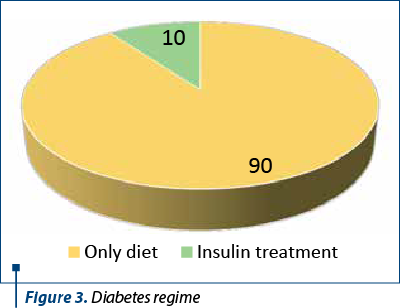
Considering all the above facts, we can draw the conclusion that there is a strong correlation between the variation of BMI (before and during the pregnancy) and the incidence of gestational diabetes. Our results indicate that the higher the initial BMI, the greater the risk of gestational diabetes. This is also highlighted in other research studies on this subject(11). Ninety percent of the patients with diabetes controlled their blood sugar levels with diet and took no medications, whereas 10% of the patients controlled it with insulin treatment.
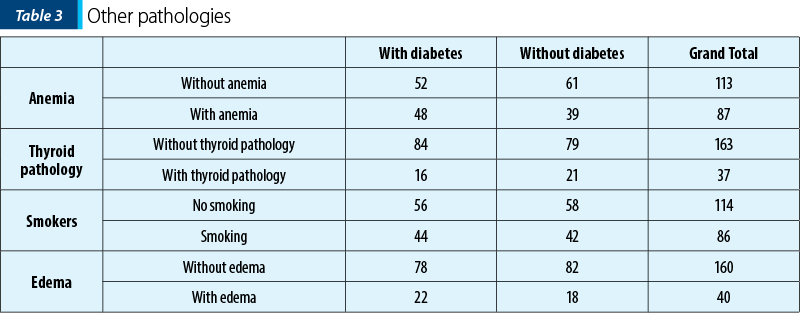
We also considered the associated pathologies of our patients. Mild anemia is considered normal during pregnancy and, in our study, it was noticed a higher percentage for patients with diabetes (48%) compared to those without diabetes (39%). The same situation was for edema: 22% of the diabetes patients had edema, compared to 18% of patients without diabetes who had edema.
Regarding smoking habit, the percentages were comparable between the two categories: 56% smokers for patients with diabetes versus 58% smokers for non-diabetes patients.
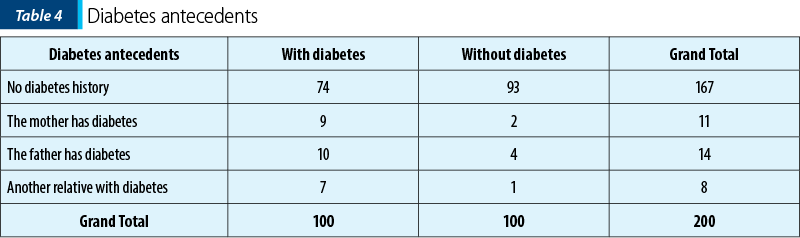
Moreover, we noticed that the presence of the diabetes familial risk factor in the first-degree relatives (mother/father) represents an important contribution to assessing the gestational diabetes risk: 76% (19 patients out of 25) of the patients who had their mother or father with diabetes developed gestational diabetes. If we extend this analysis to all relatives with diabetes (of any degree), the percentage increases to 79% (26 patients out of 33).
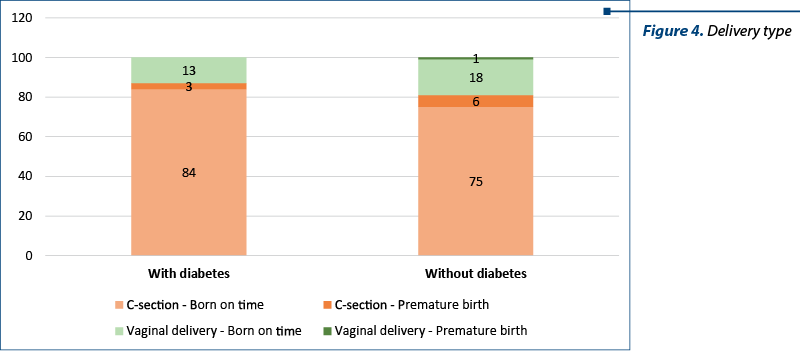
Increasing rates of worldwide caesarean section (C-section) operations can be also observed in our analysis. Many women prefer this method over the vaginal birth (due to personal and medical reasons), and this is reflected in our study: 87% of the women with diabetes had C-section; 97% of the babies were delivered on time, and 3% were born premature. For the patients without diabetes, the numbers were slightly different: 81% of the women had C-section; 93% of the babies were delivered on time, while 7% were born premature.
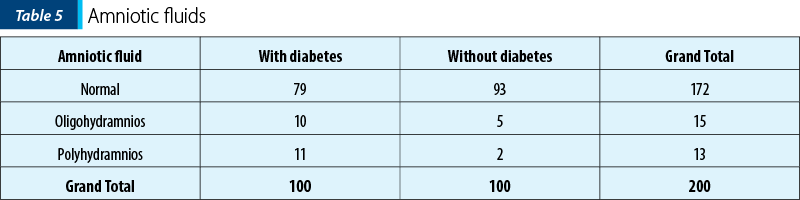
The ultrasound examination provided us details about the amniotic fluid: 86% (79 patients with diabetes and 93 patients without diabetes) had normal amniotic fluid, 7% (11 patients with diabetes and two patients without diabetes) of the cases had polyhydramnios and 8% (10 patients with diabetes and five patients without diabetes) had oligohydramnios.
Discussion
Preconception counseling for women should include information about the benefits of a healthy diet, exercise and behavioral changes. A 5-10% weight loss before getting pregnant has shown improvement in metabolic disorders associated with obesity(12).
A better understanding of the mechanisms that can lead to the onset of gestational diabetes should allow a better monitoring of risk factors, the administration of treatment during pregnancy, as well as more rational approaches to the prevention of diabetes during and after pregnancy. If it’s done during the routine clinical care in the early stages of the pregnancy, it represents a great opportunity to prevent the dysregulation of glucose metabolism (stages in which early intervention can substantially reduce the risk of post-pregnancy diabetes)(13).
We acknowledge that our study has some limitations. Among these, we mention: the sample size (200 pregnant women out of 3807), the limited timeline considered (one year), and the fact that we considered only patients from one medical center. Larger scale prospective studies are recommended to confirm these findings.
Conclusions
This study demonstrates that there are correlations between clinical and paraclinical changes and maternal and fetal complications for pregnant women with gestational diabetes. Good glycemic control is of great importance for the amelioration of pregnancy complications and perinatal conditions. The findings of this study contribute to a more comprehensive understanding of the effects of GDM and highlight the importance of preconception counseling for women with BMI>25. Pre-pregnancy care for diabetic women should be performed by a multidisciplinary care team (obstetrician, endocrinologist, nutritionist) and should include evaluations for vascular complications, cardiovascular status, assessment of glycemic control and, last but not least, promoting a healthy lifestyle that might involve behavioral changes (exercise regularly, be physically active, healthy diet, get enough sleep, quit smoking etc.).
Postpartum retesting is a very important aspect that can prevent complications of diabetes, metabolic or cardiovascular diseases. For patients with gestational diabetes, the oral glucose tolerance test must be repeated 6-12 weeks postpartum and every two years after birth in order to identify women with persistent diabetes(14,15).
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
McIntyre HD, Catalano P, Zhang C, Desoye G, Mathiesen ER, Damm P. Gestational diabetes mellitus. Nat Rev Dis Primers. 2019;5(1):47.
-
Saeedi P, Petersohn I, Salpea P, Malanda B,Karuranga S, Unwin N. Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: results from the International Diabetes Federation Diabetes Atlas. Diabetes Research and Clinical Practice. 9th ed. 2019;157:107843.
-
Metzger BE, Lowe LP, Dyer AR, et al. HAPO Study Cooperative Research Group. Hyperglycemia and adverse pregnancy outcomes. N Engl J Med. 2008;358(19):1991-2002.
-
Gomes D, von Kries R, Delius M, Mansmann U, Nast M, Stubert M, et al. Late-pregnancy dysglycemia in obese pregnancies after negative testing for gestational diabetes and risk of future childhood overweight: An interim analysis from a longitudinal mother-child cohort study. PLoS Med. 2018;15(10):e1002681.
-
Yogev Y, Xenakis EM, Langer O. The association between preeclampsia and the severity of gestational diabetes: the impact of glycemic control. Am J Obstet Gynecol. 2004;191(5):1655-60.
-
Gabbe SG, Niebyl JR, Simpson JL. Diabetes mellitus complicating pregnancy. Obstetrics, normal and problem pregnancies. Philadelphia, Churchill, Livingstone, 5th ed., 2007;976–1005.
-
Wenrui Y, Cong L, Jing H, Chenglong L, Zhixiong L, Fangkun L. Gestational diabetes mellitus and adverse pregnancy outcomes: systematic review and meta-analysis. BMJ. 2022;377:e067946.
-
Yuen L, Saeedi P, Riaz M, Karuranga S, Divakar H, Levitt N, Yang X, Simmons D. Projections of the prevalence of hyperglycemia in pregnancy in 2019 and beyond: Results from the International Diabetes Federation Diabetes Atlas, 9th edition. Diabetes Res Clin Pract. 2019;157:107841.
-
American Diabetes Association. Professional Practice Committee: Standards of Medical Care in Diabetes - 2022. Diabetes Care. 2022;45 (Suppl 1):S3.
-
Yefet E, Schwartz N, Sliman B, Ishay A, Nachum Z. Good glycemic control of gestational diabetes mellitus is associated with the attenuation of future maternal cardiovascular risk: a retrospective cohort study. Cardiovasc Diabetol. 2019;18:75.
-
Najafi F, Hasani J, Izadi N, Hashemi-Nazari SS, Namvar Z, Shamsi H, Erfanpoor S. Risk of gestational diabetes mellitus by pre-pregnancy body mass index: A systematic review and meta-analysis. Diabetes Metab Syndr. 2021;15(4):102181.
-
Cha E, Smart MJ, Braxter BJ, Faulkner MS. Preconception care to reduce the risks of overweight and obesity in women of reproductive age: an integrative review. Int J Environ Res Public Health. 2021;18(9):4582.
-
Saravanan P. Gestational diabetes: opportunities for improving maternal and child health. Lancet Diabetes Endocrinol. 2020;8(9):793-800.
-
Bellamy L, Casas JP, Hingorani AD, Williams D. Type 2 diabetes mellitus after gestational diabetes: a systematic review and meta-analysis. Lancet. 2009;373(9677):1773-9.
-
Yessoufou A, Moutairou K. Maternal diabetes in pregnancy: early and long-term outcomes on the offspring and the concept of “metabolic memory”. Exp Diabetes Res. 2011;2011:218598.





