Managementul unui paciente cu hemofilie, formă dobândită gestaţional – prezentare de caz
The management of a patient with pregnancy-acquired hemophilia – a case report
Abstract
Acquired hemophilia A (AHA) is a rare and severe hemorrhagic disorder in which the body produces specific antibodies against factor VIII of coagulation. AHA is an important coagulation disorder because it develops suddenly and it can be life-threatening due to fulminant bleeding. In women, AHA affects 20-30-year-olds, because of the relationship with pregnancy and puerperal period. Managing acquired hemophilia A during pregnancy or postpartum period can be a challenge, because the signs and symptoms can be confused with hemostasis disorders related to postpartum bleeding, such as coagulation factors deficiency, HELLP syndrome, Von Willebrand disease and others. Also, obstetrical causes for bleeding should be excluded, such as uterine atony, placental remnants or birth canal lesion. The treatment should be prompt and personalized according to each case, but the most important measures are to control the bleeding and to eradicate the inhibitors.Keywords
pregnancyacquired hemophilia Acompartment syndromeRezumat
Hemofilia A dobândită este o patologie hemoragică rară şi severă în care organismul produce anticorpi specifici împotriva factorului VIII al coagulării. Hemofilia A dobândită reprezintă o patologie hematologică importantă, deoarece apare spontan şi poate pune în pericol viaţa mamei din cauza sângerării fulminante. La femei, hemofilia A dobândită afectează grupa de vârstă 20-30 de ani, din cauza incidenţei crescute a sarcinii sau a perioadei puerperale la această categorie populaţională. Managementul hemofiliei A pe parcursul sarcinii poate fi o provocare, din cauza semnelor şi simptomelor care pot fi confundate cu cele ale altor patologii hemoragice asociate sângerării post-partum, precum deficitul factorilor de coagulare, sindromul HELLP, boala Von Willedbrand şi altele. De asemenea, cauzele obstetricale de sângerare ar trebui excluse, precum atonia uterină, resturi placentare sau laceraţii ale canalului de naştere. Tratamentul trebuie să fie prompt şi personalizat, în funcţie de fiecare caz, dar cele mai importante măsuri sunt controlul hemostazei şi eradicarea anticorpilor.Cuvinte Cheie
sarcinăhemofilia A dobândităsindromul de compartimentIntroduction
Acquired hemophilia A (AHA) is a rare autoimmune disease, in which the body produces specific antibodies against factor VIII of coagulation(1-5). The certain etiology of AHA is not completely known. Drugs and malignant neoplasms can be responsible for the cause of AHA in elderly population. Possible etiologies associated with pregnancy and postpartum period can be: autoimmune diseases, such as systemic lupus erythematosus, rheumatoid arthritis, multiple sclerosis, Sjögren’s syndrome, autoimmune hemolytic anemia, myasthenia gravis, autoimmune hypothyroidism, or hematological diseases, such as Waldestron’s disease, leukemia, Hodgkin disease or multiple myeloma(1).
AHA affects 1.2 to 1.4 million people a year, being more common in men over 60 years old and very rare during childhood(1,6). The disease occurs in all ethnic groups and is spread all over the world; in women, it appears in fertile age and is related to pregnancy and puerperal period, with a frequency of 7-21%(1). The rate of mortality in AHA is estimated to be over 20% in patients over 65 years old and in those with underlying malignancies, but the deaths from bleeding are less common (3.2%)(7-9).
The most important sign in AHA is the bleeding. The most common bleeding in AHA is the subcutaneous bleeding (>80%), followed by muscle bleeding (>40%) and gastrointestinal bleeding (>20%); genitourinary, retroperitoneal and other sites of bleeding represent less than 10%(7,9-11). In pregnancy, AHA typically appears in the first pregnancy and it is usually diagnosed several days to months postpartum, but it can also manifest peripartum(7,9-17). Despite other AHA, in the disorder associated with pregnancy, the important uterine or vaginal bleeding is frequent(17).
The diagnosis of AHA should be suspected in elderly patients and in peri- or postpartum women, with recent onset of abnormal bleeding and increased activated partial time, without changes in platelet count, prothrombin time and thrombin time(1,7). Factor VIII of coagulation has a decreased level in plasma and the presence of the inhibitors against this factor is confirmed using a blood clotting assay called the Bethesda Inhibitor Assay(1).
The treatment of AHA requires a multidisciplinary management, because it is important to control the bleeding, to remove the trigger and to eradicate the inhibitors(1). Bleeding can be controlled by using coagulation factors and for the eradication of the inhibitors immunosuppressants such as corticosteroids are usually used; however, these drugs can be associated with other cytotoxic agents(1).
Women with pregnancy-associated AHA respond very well to immunosuppressive therapy, with the effect of substantially reducing hemorrhagic complications(1).
Case report
We report the case of a 31-year-old Caucasian patient who was admitted in the Intensive Care Unit of the Bucharest University Emergency Hospital, Romania, transferred from a regional maternity for forearm compartment syndrome. The patient had delivered (first pregnancy) 33 days prior to that. Regarding the general information about her lifestyle, the family medical history and the personal pathological history, we noticed no significant data. She had a Body Mass Index of 26.6, and she was non-smoker and non-hypertensive.
She began investigating her pregnancy at 5-6 weeks of amenorrhea. She had an unremarkable medical history. The patient underwent regular gynecological examinations, ultrasound scans, and all the blood and urine tests recommended by her physician. Her unique problem during pregnancy, at 7-8 weeks of pregnancy, was a urinary infection with Enterococcus faecalis, which was treated.
At 40 weeks of gestation, she delivered spontaneously, at the maternity unit where her pregnancy was supervised, giving birth to a masculine fetus of 3000 grams, with an Apgar score of 7 at one minute, and 8 at five minutes. The deliverance of the placenta was natural, its weight was approximately 500 grams, and it looked macroscopically normal, therefore no manual or instrumental uterine exploration was needed. After two days of hospitalization, she was discharged with a favorable general status, with the involution of the uterus in normal parameters, with serosanguinous lochia and breastfeeding.
In the next three weeks, the patient presented three episodes of abundant vaginal bleeding, for which she referred to the emergency room of the maternity where she delivered. Each time a haemostatic uterine curettage was performed. After the third episode the bleeding could not be controlled anymore by the haemostatic uterine curettage, and total hysterectomy was performed. Erythrocyte concentrate was administrated for post-hemorrhagic anemia. During the hospitalization, numerous bruises appeared at venipuncture sites. After a week from surgery, at an arterial puncture site, the patient developed a hematoma complicated with forearm compartment syndrome. The patient was transferred to our hospital and multiple fasciotomy surgeries were practiced in the Department of Plastic and Reconstructive Surgery (Figure 1). We performed an abdominopelvic computed tomography and we detected two hematomas: one at the level of rectus abdominis, with an unorganized characteristic, of 14/5/14 cm in diameters, and one deep intraperitoneal hematoma with the same characteristics, but with reduced diameters of approximately 7/4/8 cm (Figure 2).
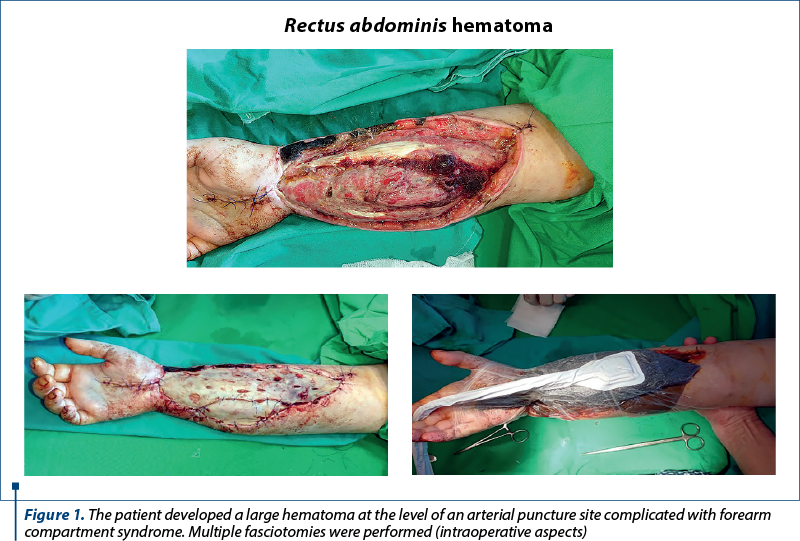
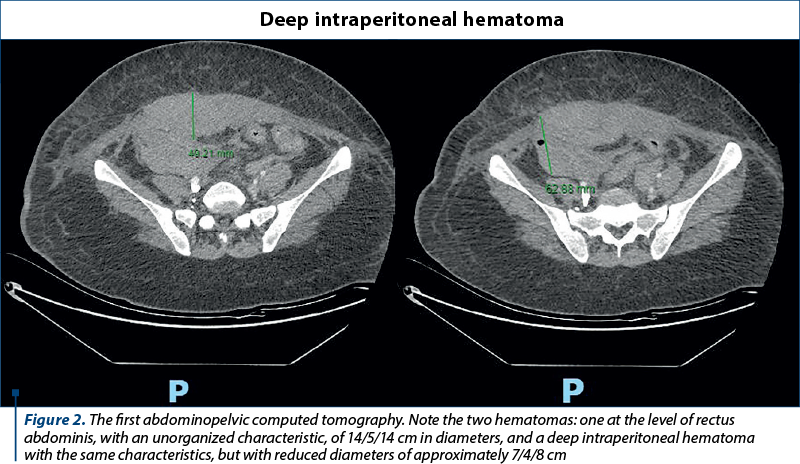
The blood samples from our hospital revealed an increased activated partial time and plasmatic levels of factor VIII under 1%. Therefore, the diagnosis of acquired hemophilia A was suspected, and therapy with recombinant factor VIIa was recommended.
The certain diagnosis was established in the next two days: severe form of acquired hemophilia A, with factor VIII under 1% and inhibitors over 220 Bethesda units. Systemic lupus erythematosus was excluded. The patient continued the therapy with recombinant factor VIIa and corticosteroids and rituximab were also recommended. She also received erythrocyte concentrates for severe anemia and antibiotic therapy. Another fasciotomy and surgical debridement were performed in order to control the hemostasis and to alleviate the compartment syndrome. A transvaginal drainage was also performed. The following computed tomography disclosed decreased diameters of hematomas (Figure 3).
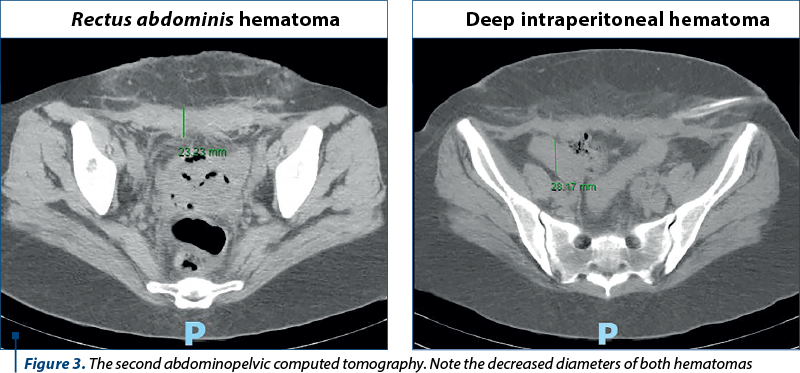
After a week of hospitalization and specific therapy, blood samples demonstrated an improvement: an increased factor VIII from under 1% to 7.21%, and a decrease of inhibitors of factor VIII from 220 to 180 Bethesda units.
During the hospitalization, the patient continued the antibiotic and antifibrinolytic therapy and the treatment with corticosteroids and iron. The therapy with recombinant factor VIIa was used just in case of acute bleeding.
After almost two months of hospitalizations and multiple surgical interventions (Figure 4) and complex treatments, the patient was discharged with a favorable status regarding the hematological, gynecological and plastic surgery disorders. The patient will need at least one year of medical supervision, to exclude the possibility of other complications.
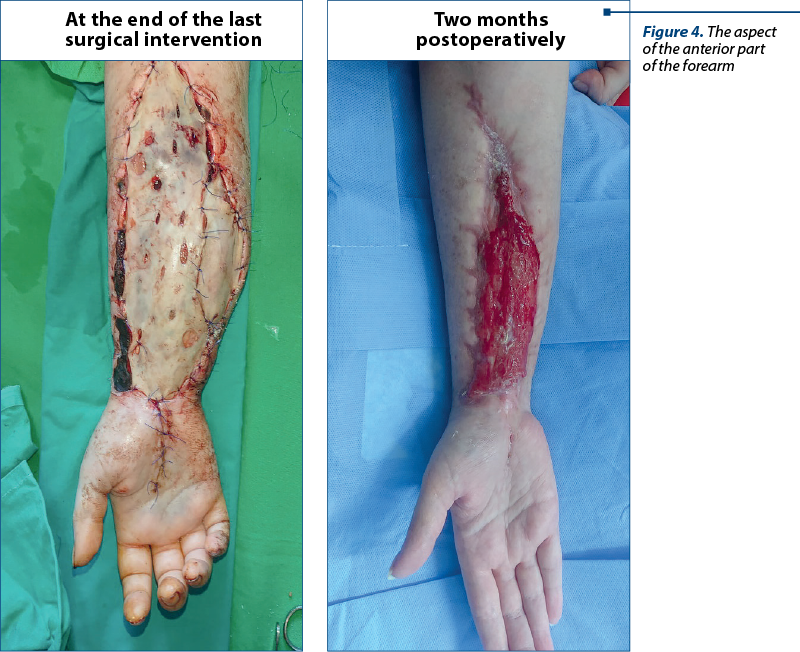
Discussion
Acquired hemophilia A is a rare autoimmune disease caused by the spontaneous production of neutralizing immunoglobulin G autoantibodies targeting endogenous factor VIII of coagulation(7,18,19).
Pregnancy-related AHA appears in 7% to 11% of cases of this disease, and is most common within 1 to 4 months after delivery(20-22). AHA mainly manifests as hemorrhages in the skin, mucous, membranes, muscles or joint(20), but in our case the first signs were the repeated abundant vaginal bleeding in the first three weeks after birth and the forearm compartment syndrome. It is important to remark that an autoimmune disease was not found in this patient, and she had no personal or family history of abnormal bleedings.
In our case, the lack of manual or instrumental uterine exploration could have been a cause of undiagnosed AHA. Also, the repeated abundant vaginal bleeding and the repeated uterine curettage should have raised a question.
Regarding the forearm compartment syndrome, the etiology includes trauma – which is the most common cause –, burns, bleeding disorders, arterial injuries and intravenous drug administration(23,24). In our case, the trigger of the compartment syndrome was the arterial injury on a background of an unknown bleeding disorder. The prompt management in compartment syndrome has the most important prognostic value. The treatment of acute compartment syndrome is represented by the urgent forearm compartment fasciotomies, which are critical and limb saving(23,25,26). As presented, in our cause the management was correctly applied, as soon as possible, therefore the patient had a full recovery. Because of her AHA, she needed more fasciotomies, but the final result was a success.
The goal in the AHA treatment is to control the bleeding and suppress the inhibitors(20). Fortunately, in our case the patient received the prompt and the correct treatment and the evolution was good.
Women with AHA during pregnancy or peripartum period may present a spontaneous resolution of the condition, but they should be followed-up to one year after the remission of the disease, because of the risk of recurrence(1,27,28).
Conclusions
Pregnancy-related acquired hemophilia A is a rare coagulation disease which is important to be diagnosed in a very short time. The patients diagnosed with this condition require a multidisciplinary management in order to decrease morbidity and even mortality.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Rodrigues DO, Júnior I, Ferreira AA, Sudário LC, Rocha Maciel BA. Postpartum acquired hemophilia A: case report and literature review. J Blood Disord Med. 2017;2(1).
- Burish MJ, Aysenne A, Singh V. Multifocal subdural hematomas as the presenting sign of acquired hemophilia A: a case report. BMC Research Notes. 2014;7(1):134.
- Collins P, Baudo F, Knoebl P, Lévesque H, Nemes L, Pellegrini F, Huth-Kühne A. Immunosuppression for acquired hemophilia A: results from the European Acquired Haemophilia Registry (EACH2). Blood. 2012;120(1):47-55.
- Collins PW. Therapeutic challenges in acquired factor VIII deficiency. Hematology Am Soc Hematol Educ Program. 2012;2012(1): 369–74.
- Kyaw TZ, Jayaranee S, Bee PC, Chin EFM. Acquired factor VIII inhibitors: three cases. Turkish J Hematol. 2013;30(1):76-80.
- Barg AA, Livnat T, Kenet G. An extra X does not prevent acquired hemophilia – Pregnancy-associated acquired hemophilia A. Thrombosis Research. 2017;151:S82-S85.
- Kruse‐Jarres R, Kempton CL, Baudo F, Collins PW, Knoebl P, Leissinger CA, Kessler CM. Acquired hemophilia A: updated review of evidence and treatment guidance. Am J Hematol. 2017;92(7):695-705.
- Bitting RL, Bent S, Li Y, Kohlwes J. The prognosis and treatment of acquired hemophilia: a systematic review and meta-analysis. Blood Coagul Fibrinolysis. 2009;20(7):517-23.
- Collins PW, Hirsch S, Baglin TP, Dolan G, Hanley J, Makris M, Hay CR. Acquired hemophilia A in the United Kingdom: a 2-year national surveillance study by the United Kingdom Haemophilia Centre Doctors’ Organisation. Blood. 2007;109(5):1870-77.
- Delgado J, Jimenez‐Yuste V, Hernandez‐Navarro F, Villar A. Acquired haemophilia: review and meta‐analysis focused on therapy and prognostic factors. Brit J Haematol. 2003;121(1):21-35.
- Knoebl P, Marco P, Baudo F, Collins P, Huth‐Kühne A, Nemes L, EACH2 Registry Contributors. Demographic and clinical data in acquired hemophilia A: results from the European Acquired Haemophilia Registry (EACH2). J Thromb Haemost. 2012;10(4):622-31.
- Green D, Lechner K. A survey of 215 non-hemophilic patients with inhibitors to factor VIII. Thromb Haemost. 1981;45(03): 200-3.
- Tay L, Duncan E, Singhal D, Al-Qunfoidi R, Coghlan D, Jaksic W, Lloyd J. Twelve years of experience of acquired hemophilia A: trials and tribulations in South Australia. Semin Thromb Hemost. 2009;35(8):769-77.
- Borg JY, Guillet B, Le Cam‐Duchez V, Goudemand J, Lévesque H, SACHA Study Group. Outcome of acquired haemophilia in France: the prospective SACHA Haemophilia. 2013;19(4):564-70.
- Huang SY, Tsay W, Lin SY, Hsu SC, Hung MH, Shen MC. A study of 65 patients with acquired hemophilia A in Taiwan. J Formos Med Assoc. 2015;114(4):321-7.
- Gheisari R, Bomke B, Hoffmann T, Scharf RE. Clinical features and outcome of acquired haemophilia A. Hämostaseologie. 2010;30(03):156-61.
- Tengborn L, Baudo F, Huth‐Kühne A, Knoebl P, Lévesque H, Marco P, EACH2 registry contributors. Pregnancy‐associated acquired haemophilia A: results from the European Acquired Haemophilia (EACH2) registry. BJOG. 2012;119(12):1529-37.
- Oldenburg J, Zeitler H, Pavlova A. Genetic markers in acquired haemophilia. Haemophilia. 2010;16(suppl 3):41-5.
- Ma AD, Carrizosa D. Acquired factor VIII inhibitors: pathophysiology and treatment. Hematology Am Soc Hematol Educ Program. 2006;432-7.
- Qian L, Ge H, Hu P, Zhu N, Chen J, Shen J, Zhang Y. Pregnancy-related acquired hemophilia A initially manifesting as pleural hemorrhage: A case report. Medicine (Baltimore). 2019;98(3): e14119.
- Bossi P, Cabane J, Ninet J, Dhote R, Hanslik T, Chosidow O, Pouchot J. Acquired hemophilia due to factor VIII inhibitors in 34 patients. Am J Med. 1998;105(5):400-8.
- Michiels JJ. Acquired hemophilia A in women postpartum: clinical manifestations, diagnosis, and treatment. Clin Appl Thromb/Hemost. 2000;6(2):82-6.
- Jimenez A, Marappa-Ganeshan R. Forearm compartment syndrome. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020.
- Lee YK, Lee SH, Kwon TY. Acute compartment syndrome of the forearm associated with transradial coronary intervention. J Hand Surg (Eur Vol). 2020;1753193419899007.
- Hanandeh A, Mani VR, Bauer P, Ramcharan A, Donaldson B. Identification and surgical management of upper arm and forearm compartment syndrome. Cureus. 2019;11(10):e5862.
- Gondolini G, Schiavi P, Pogliacomi F, Ceccarelli F, Antonetti T, Zasa M. Long-term outcome of mini-open surgical decompression for chronic exertional compartment syndrome of the forearm in professional motorcycling riders. Clin J Sport Med. 2019;29(6):476-81.
- Almagro Vázquez D. Hemofilia A adquirida. Rev Cubana Hematol Inmunol Hemoter. 2010;26(3):174-85.
- Freire M, Teodoro RB, Nogueira DA, Rita DPC, Ribeiro Filho E, Sousa LVD. Acquired hemophilia associated with rheumatoid arthritis. Bras J Reumatol. 2009;49(3):302-7.





