Prognosticul neonatal al sarcinilor complicate cu anemie la adolescente
Neonatal outcome of adolescent pregnancies complicated with anemia
Abstract
Pregnancy among teenagers represents a public health problem which has a huge impact for the mother, newborn, society and even for the new generations. When it comes to pregnancy in adolescents, we see that obstetrical complications represent the main cause of death in this population. Also, the newborns may have complications like premature birth or intrauterine growth restriction. Because the increase incidence of pregnant adolescents occurs in low- and middle-income countries, the nutritional status has a negative impact on the mother and the fetus. We performed a retrospective study in the Department of Obstetrics and Gynecology of the University Emergency Hospital, Bucharest, between the15th of April 2020 and the 15th of April 2022 that included 258 adolescents who gave birth in our unit. The aim of the study was to analyze the risk of premature birth in newborns from adolescent mother with anemia compared to adolescent patients without anemia, so we divided the patients into two groups. The premature birth was established by the gestational age and the neonatal status was evaluated using the Apgar score at 1 minute. Regarding the results, adolescent patients with anemia had a higher risk of premature birth compared to those who were not diagnosed with anemia.Keywords
adolescentspregnancyanemiafetal outcomeRezumat
Sarcina în rândul adolescentelor reprezintă o problemă de sănătate publică, având un impact deosebit asupra mamei, nou-născutului, societăţii, dar şi pentru viitoarele generaţii. Când vorbim despre sarcina în rândul adolescentelor, putem observa că principala cauză de deces în rândul acestei populaţii este reprezentată de complicaţiile obstetricale. De asemenea, complicaţiile neonatale sunt mai frecvente, iar acestea includ prematuritatea şi restricţia de creştere intrauterină. Deoarece majoritatea cazurilor de adolescente gravide apar în ţările în curs de dezvoltare, statusul nutriţional al pacientelor are un impact negativ atât pentru mamă, cât şi pentru nou-născut. Am efectuat un studiu retrospectiv în Clinica de obstetrică şi ginecologie a Spitalului Universitar de Urgenţă Bucureşti, în perioada 15 aprilie 2020 – 15 aprilie 2022, care a inclus 258 de paciente adolescente ce au născut în clinica noastră. Scopul studiului a fost de a analiza riscul de naştere prematură la pacientele adolescente cu anemie comparativ cu cele fără anemie, astfel încât acestea au fost împărţite în două grupe. Prematuritatea a fost stabilită în funcţie de vârsta gestaţională, iar statusul neonatal a fost evaluat cu ajutorul scorului Apgar calculat la 1 minut. În ceea ce priveşte rezultatele, putem concluziona că pacientele adolescente care au fost diagnosticate cu anemie au avut un risc mai mare de naştere prematură, comparativ cu celelalte adolescente.Cuvinte Cheie
adolescentesarcinăanemiaprognostic neonatalIntroduction
Pregnancy during adolescent period represents a public health problem all over the world. World Health Organization (WHO) estimates that 11% of the world’s births result from adolescent patients and the global rate represents 46 births per 1000 women(1,2). An important issue is that 95% of all these births are in low- and middle-income countries, while Romania occupies the second place in Europe regarding adolescent pregnancies(3,4). One of the explanations consists in the fact that the background in these countries is represented by poverty and low formal education levels(5).
The main problem of pregnant women during adolescent period is that, most of the time, the pregnancy is unwanted and many teenagers resort to abortion. It is important to mention that the leading cause of death in adolescent population is related to pregnancy. The most frequent cause of death in pregnant adolescents is spontaneous delivery, followed by other complications of pregnancy, maternal care of the newborn or due to abortion. All these represent 61% of deaths related to pregnancy in adolescents(1,6-8). Even when the pregnancy is wanted, there are consequences concerning the mental and psychological health or for society(9,10).
Regarding the neonatal and obstetrical complications, there are more often in adolescent patients than in women between 20 and 30 years old, and it is also estimated that pregnant adolescents have twice the chances to die from complications in pregnancy or childbirth than older women(1). Besides this major complication, teenagers are more likely to have more complications such as preeclampsia, eclampsia, anemia and induced or spontaneous abortion(1,11).
When it comes to nutritional health in adolescents, it is clear that pregnancy may have serious consequences, from this point of view. The explanation is that teenagers are not prepared for pregnancy, and in the moment they are pregnant, their nutritional status is inadequate(12). Also, there are studies which reveal that pregnant adolescents do not gain weight during the follow-up period compared to never-pregnant adolescents(12,13). Regarding the adolescents’ health, we can add that they are more exposed to develop anemia during pregnancy and also this complication may have serious negative effects for the newborn. There is a study that took place between January 2015 and December 2015 which included 241 adolescents. In this study, more than 33% of patients had anemia and, also, it was concluded that anemia, along to poor antenatal care, is associated with high rates for fetal distress at birth and preterm delivery(14).
Materials and method
We performed a retrospective study in the Department of Obstetrics and Gynecology of the University Emergency Hospital, Bucharest, during two years, between the 15th of April 2020 and the 15th of April 2022. We analyzed adolescent patients who gave birth in our hospital, the ones who had associated anemia and the correlation between them and the neonatal outcome. The neonatal outcome was evaluated by weight of the newborn and the Apgar score at 1 minute. The maternal anemia was analyzed by hemoglobin concentration below 10 g/dL. This study included 258 newborns and their adolescent mothers. The patients who had anemia were 102, representing 39% of all adolescents who gave birth in our hospital. The inclusion criteria were represented by adolescent mothers from 13 to 19 years old who were admitted and gave birth in our unit and the ones who had anemia diagnosed during hospitalization.
The information regarding pregnancy and neonatal data were retrieved from the hospitalization sheets and the Database System of the University Emergency Hospital, Bucharest. Maternal age was defined as that recorded at the time of delivery and the anemia criterium was established at <10 g/dL, as in our laboratory hospital.
We analyzed the pregnant adolescents with anemia and the neonatal status compared to pregnant adolescents who didn’t have anemia and their newborns.
We mention that the adolescents who gave birth in our hospital represented 6% of all births.
Results
A total of 258 patients were included in the study. One hundred and fifty-six patients, aged 14-19 years old, were included in Group A – pregnant adolescents without anemia, and one hundred and two patients, aged 13-19 years old, were included in Group B – pregnant adolescents with anemia. We mention that in the first group there were three patients with multiple pregnancy, while in the second group there were two patients with twin pregnancy.
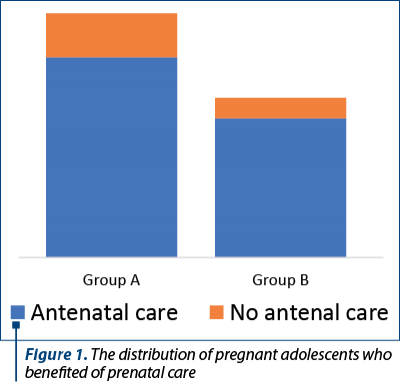
It was also evaluated if the patients in both groups underwent antenatal care (Figure 1). It is important to say that a huge number of adolescent patients did not undergo any routine medical visit in both groups – more than 80%. In group A, 82% of adolescents did not have any antenatal care, while in group B the percentage was 87%.
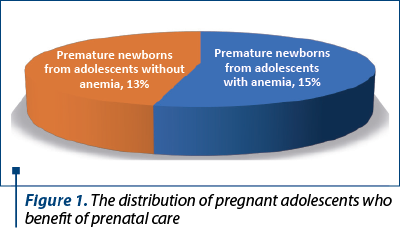
Analyzing the neonatal status in pregnant adolescents with anemia, we concluded that they had an increased risk of preterm birth than adolescents who gave birth and did not have anemia. Thus, in Group A (156 patients without anemia), there were born 21 premature newborns (13%), while in the Group B (102 patients with anemia), there were born 18 premature newborns (15%) – Figure 2. Also, we noticed that 3% (n=3) of patients with anemia had a severe form, with a value of hemoglobin <7 g/dL, and they needed blood transfusion. Regarding these aspects, the newborn status was affected too, and all of them were born premature, with a weight under 1000 grams, and all needed neonatal intensive care.
We specify that in Group B there were two patients with hepatitis B, one with hepatitis C, one with active herpes simplex and one with AIDS plus hepatitis C. None of these viral infections were seen in the patients from Group A. All the children born from mothers with these viral infections were premature and they had an Apgar score at 1 minute below 7.
As it can be seen in Figure 2, there were more premature newborns from adolescent patients with anemia than those without anemia. We must mention that, in the analyzed period of time, we had two cases of maternal death in adolescents with anemia. In one case it was a cerebral pathology in an 18-year-old adolescent who died one month after she gave birth to the third child, and the other case was also an 18-years-old teenager who died due to AIDS 3 weeks after she gave birth to her first child. In both cases, the fetuses were born premature. Both patients did not undergo any antenatal care. There had not been any maternal death in adolescent patients without anemia.
Because the analyzed period corresponds to the COVID-19 pandemic time, we also evaluated the impact of SARS-CoV-2 infection in pregnant adolescents with anemia. The data show that patients with anemia have been more affected by COVID-19 compared to the ones without anemia, with a percentage of 6%, respectively 5%.
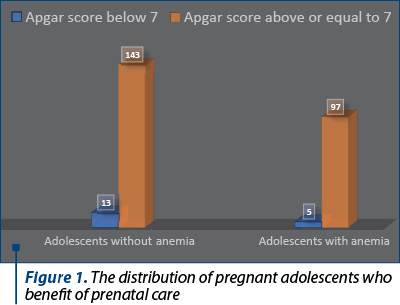
Regarding the neonatal status, in Group A, in adolescent patients without anemia, there have been more newborns who had an Apgar score below 7 compared to the newborns from mothers with anemia (Figure 3). The reason may be the fact that a high number of patients had no antenatal medical care and maybe the newborn status was poor due to other complications that had not been diagnosed previously.
Discussion
Our study included 258 adolescents who gave birth in our hospital, representing 6% of all births in our unit. Also, we noticed a high rate of no antenatal medical visits in these patients. As other studies show, our findings seem to be consistent with international reported ranges about pregnancy among teenagers(14).
Almost 40% of pregnant adolescents were diagnosed with anemia. In these cases, we noticed a higher rate of premature newborns compared to adolescent patients who had no anemia and gave birth. Even though studies show that teenagers have an increased risk of premature birth, we can conclude that anemia during pregnancy and the nutritional status can have an additional negative impact on newborns from adolescent mothers. Even in adult populations, anemia during pregnancy has adverse neonatal outcomes(15). In our study, we can conclude that anemia in adolescent pregnant patients had an additional negative impact and a higher risk of preterm birth. Furthermore, we noticed that the risk of prematurity was directly proportional to the severity of anemia. All the newborns from mothers with severe anemia suffered from extreme prematurity.
Regarding the neonatal status evaluated by the Apgar score, we can conclude that anemia does not affect the newborn more than the young maternal age does. Although we concluded that anemia is a risk factor for premature birth, we cannot ignore the fact that in the group of patients with anemia there had been five cases of mothers with viral infections that affected the newborns. However, the reason that in the group of adolescent patients without anemia there was a higher incidence of low neonatal status may be due to the fact that an important number of patients did not undergo any medical care, so we could not know if they had any pathologies associated. Most of the patients who gave birth in our hospital (more than 87%) had the first medical evaluation when they had been hospitalized.
Conclusions
The current retrospective study shows a higher risk of preterm birth in adolescent population who associate anemia. Due to a poor antenatal care, pregnant teenagers present more risks. We should improve this problem with new educational programs. The adolescent population should be aware of the importance of antenatal care, nutritional status and the obstetrical and neonatal outcome at this age.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
González-Andrade F, Saeteros-Cordero X. Pregnancy in adolescence and adverse neonatal outcomes in Ecuadorian mestizo newborns. Pediatr Neonatol. 2020;61(2): 216-23.
-
Ganchimeg T, Ota E, Morisaki N, Laopaiboon M, Lumbiganon P, Zhang J, et al. WHO Multicountry Survey on Maternal Newborn Health Research Network. Pregnancy and childbirth outcomes among adolescent mothers: a World Health Organization multicountry study. BJOG. 2014;121 Suppl 1:40-8.
-
Uzunov AV, Bohîlţea RE, Munteanu O, Nemescu D, Cîrstoiu MM. A retrospective study regarding the method of delivery of adolescents in a Romanian Hospital. Exp Ther Med. 2020;20(3):2444-8.
-
Cook SM, Cameron ST. Social issues of teenage pregnancy. Obstet Gynecol Reprod Med. 2015;25:243‐8.
-
Monteiro DLM, Martins JAFDS, Rodrigues NCP, Miranda FRDD, Lacerda IMS, Souza FMD, et al. Adolescent pregnancy trends in the last decade. Rev Assoc Méd Bras. 2019;65(9):1209-15.
-
Sánchez-Gómez A, Cevallos W, Grijalva MJ, Silva-Ayçaguer LC, Tamayo S, Jacobson JO, et al. Social factors associated with use of prenatal care in Ecuador. Pan Am J Public Health. 2016;40(5):341-6.
-
Parra-Pingel PE, Quisiguiña-Avellán LA, Hidalgo L, Chedraui P, Pérez-López FR. Pregnancy outcomes in younger and older adolescent mothers with severe preeclampsia. Adolescent Health, Medicine and Therapeutics. 2017;8:81.
-
Svanemyr J, Guijarro S, Riveros BB, Chandra-Mouli V. The health status of adolescents in Ecuador and the country’s response to the need for differentiated healthcare for adolescents. Reprod Health. 2017;14:29.
-
Buratto J, Kretzer MR, Freias PF, Traebert J, Nunes RD. Temporal trend of adolescent pregnancy in Brasil. Rev Assoc Méd Bras. 2019;65(6):880-5.
-
Victora CG, Aquino EM, do Carmo Leal M, Monteiro CA, Barros FC, Szwarcwald CL. Maternal and child health in Brazil: progress and challenges. Lancet. 2011;377(9780):1863-76.
-
Mesenburg MA, Restrepo-Mendez MC, Amigo H, Balandrán AD, Barbosa-Verdun MA, Caicedo-Velásquez B, et al. Ethnic group inequalities in coverage with reproductive, maternal and child health interventions: cross-sectional analyses of national surveys in 16 Latin American and Caribbean countries. Lancet Glob Health. 2018;6(8):e902-e913.
-
Christian P, Smith ER. Adolescent undernutrition: global burden, physiology, and nutritional risks. Ann Nutr Metab. 2018;72(4):316-28.
-
Rah JH, Christian P, Shamim AA, Arju UT, Labrique AB, Rashid M. Pregnancy and lactation hinder growth and nutritional status of adolescent girls in rural Bangladesh. J Nutr. 2008;138(8):1505-11.
-
Baş EK, Bülbül A, Uslu S, Baş V, Elitok GK, Zubarioğlu U. Maternal characteristics and obstetric and neonatal outcomes of singleton pregnancies among adolescents. Med Sci Monitor. 2020;26:e919922-1.
-
Iqbal S, Ekmekcioglu C. Maternal and neonatal outcomes related to iron supplementation or iron status: a summary of meta-analyses. J Matern Fetal Neonatal Med. 2019;32(9):1528-40.





