Tumoră spinală cervicală asociată sarcinii
Pregnancy-related cervical spinal cord tumor
Abstract
Spinal cord tumors are rare in pregnancy, but when extensive, they can cause serious problems because of their rapidly progressive neurological involvement due to compression. Schwann cell tumors are the most common benign peripheral sheath nerve tumors. They may affect both sexes. Although they are slow-growing masses, the hormonal, biochemical and hemodynamic changes of pregnancy can trigger an accelerated growth of these tumors, with severe consequences for both mother and fetus. We report the case of a 24-year-old woman who presented at 34 weeks of gestation with a rapidly progressive pyramidal syndrome with paresis of arms and legs. The MRI exam revealed an extensive cervical spinal cord schwannoma with cord compression for which the patient required both obstetrical and neurosurgical interventions.Keywords
spinal cord tumorspregnancyschwannomaRezumat
Tumorile spinale sunt rar întâlnite în sarcină, dar atunci când sunt extinse, pot cauza probleme grave prin efectele neurologice rapid progresive date de compresia medulară. Tumorile cu celule Schwann sunt cele mai frecvente tumori derivate din teaca nervilor periferici şi pot afecta ambele sexe. Cu toate că sunt tumori cu o creştere lentă, modificările hormonale, biochimice şi hemodinamice din sarcină pot accelera creşterea acestor tumori, ducând la apariţia unor consecinţe severe pentru mamă şi făt. Prezentăm cazul unei paciente în vârstă de 24 de ani, care s-a prezentat la 34 de săptămâni de sarcină cu sindrom piramidal rapid progresiv şi tetrapareză. Examenul IRM a relevat un schwannom cervical extins, cu compresie medulară, pentru care pacienta a necesitat intervenţie chirurgicală obstetricală şi neurochirurgicală.Cuvinte Cheie
tumori spinalesarcinăschwannomIntroduction
Spinal schwannoma is a peripheral nerve sheath tumor comprised of neoplastic Schwann cells. Schwannomas are generally considered benign tumors, although some malignant subtypes exist(1). The main part of nerve sheath tumors is confined to the intradural extramedullary space, but some extend into the extradural compartment or to the spinal cord. Schwannomas are typically found eccentrically, attached to the nerve.
Schwannomas are usually encapsulated slow-growing solitary tumors which affect both males and females, mostly between 25 and 60 years of age. The incidence of spinal schwannoma is 0.3-0.4/100.000 cases per year, either as solitary tumors, or in a syndromic form(2).
Schwann cell tumors are reported in pregnant women, although their incidence is rare. It appears that hormonal changes in pregnancy may interfere with tumor growth, therefore these tumors are sometimes either revealed by the physiological pregnancy changes, or their symptoms are exacerbated by other coexisting conditions. A pregnancy-related spinal tumor occurs in about 1 in 1000 to 2000 pregnancies, and is diagnosed during the gravid state or within a year after childbirth(3). Common types of pregnancy-related spinal tumors are giant cell tumors, hemangiomas, schwannomas and metastases. The clinical symptoms may be absent or vague for months or years. Pain and paresthesia are frequent findings; sphincter function alteration or motor deficit can also be found depending on tumor location. The neurological deficit is generally progressive, but once the tumor reaches a critical size, spinal cord compression occurs and progresses rapidly. Although rare, spinal cord tumors diagnosed during pregnancy raise serious concerns in terms of continuation of pregnancy, anesthesia and neurosurgery(4).
We present the case of a 24-year-old pregnant patient who was transferred to our multidisciplinary hospital, with an ongoing 34-week pregnancy, progressive pyramidal syndrome with paresis of arms and legs, and an MRI image suggestive for a cervical spinal tumor.
Case report
A 24-year-old secundigravida was referred to our hospital presenting with increased motor weakness, back pain, numbness and aggravated paresthesia in her limbs. She had a 34-week ongoing pregnancy and was recently diagnosed with a cervical spinal mass. Her pregnancy medical history was scarce, with only two appointments to an obstetrician up to the third trimester. In the second trimester, she was diagnosed with pregnancy-induced hypertension, but has not continued further follow-up. She has been experiencing progressive back pain, headache, paresthesia and numbness in her arms and legs since 28 weeks of gestation. The symptoms aggravated at 33 weeks, when she was admitted to a local maternity hospital. Pregnancy monitoring showed no fetal distress. A cerebral and a spinal MRI were performed, and the patient was given a cervical collar to ease neck pain.
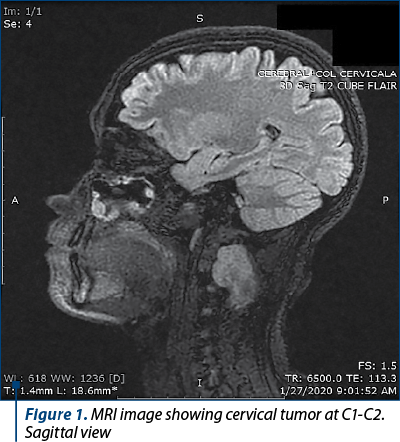
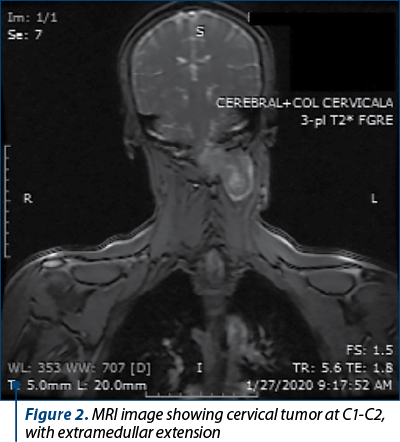
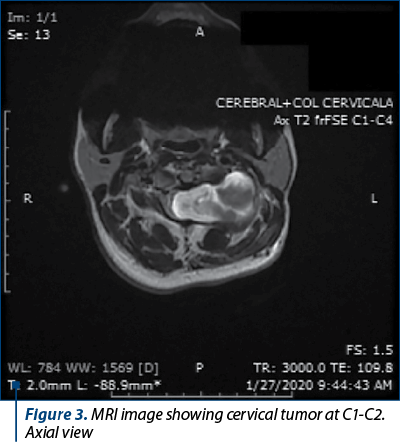
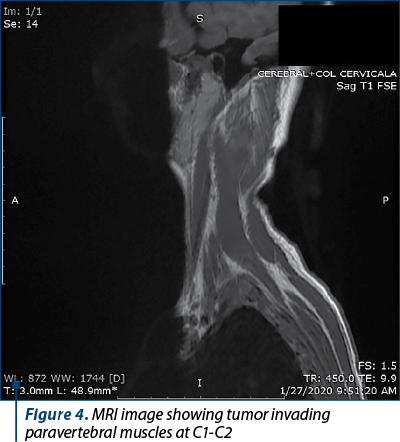
The MRI showed an extramedullar “dumbbell shaped” spinal tumor situated at C1-C2 level. The tumor measured 31/22/23 mm, had an inhomogeneous structure and extended in the paravertebral muscles on both sides, having a total diameter of 44/30/32 mm in both extensions. The entire encapsulated mass invaded the spinal cervical canal. Also, the tumor pushed the cervical spinal cord at C1-C2 level, causing compression and stenosis at C2 level on the left side. The tumor mass wrapped the root of the left spinal C2 nerve from its origin and engulfed the left lateral recess of the dural sac (Figures 1-4). The aspect suggested a benign cervical tumor, possibly a schwannoma. Next, the patient was transferred to our multidisciplinary unit in order to receive a complete management of her medical conditions.
At the admission to our hospital, the patient was hemodynamically stable, conscious, with a blood pressure of 140-150 mmHg, and SaO2 98%. She had an increased motor weakness, paresis and numbness in her limbs. The fetal monitoring and fetal ultrasound showed a live 34-week fetus, with no acute fetal distress. The patient was evaluated by the neurosurgery specialist and the obstetrician, and she was placed in the obstetrics and gynecology department for further fetal evaluation. She was given corticosteroids for fetal lung maturation and was closely monitored. As her neurologic symptoms aggravated, a caesarean section was required. A special attention was paid by the anesthesiology team, which had to prepare for intubation and ventilation difficulties. A premature, but otherwise healthy baby, with mild signs of intrauterine growth restriction, was extracted. Postoperatively, the patient was transferred to the intensive care unit for stabilization. The neurosurgery team intervened 48 hours later and performed the complete tumor resection. The pathology exam revealed that the encapsulated mass was a Schwann-cell benign tumor. The patient was discharged after recovery, with good neurological prognosis.
Discussion
The occurrence of spinal tumors in pregnancy is a relatively rare event. Most tumors exist prior to pregnancy, but are revealed by physiological changes of the gravid state or are diagnosed during pregnancy, because the patient refers to medical specialists more often. The most frequent types of pregnancy-related spine tumors are metastases of breast cancer, dermatological malignancies, hematological cancers, but also primary tumors like hemangioma, schwannoma and giant cell tumors(5). The treatment of such tumors poses diagnostic and therapeutic challenges, with regard to the maternal and fetal well-being.
The mechanism throughout which pregnancy affects tumor growth is still in debate. Many authors have stated that elevated estrogen and progesterone levels accelerate tumor growth. Also, elevated levels of angiogenic and growth factors trigger tumor growth in certain types, such as schwannomas. Hemodynamic changes in pregnancy are also involved in revealing tumor symptomatology. The increased blood flow volume through the vertebral venous plexus secondary to uterine compression of the vena cava can cause spinal cord compression(6).
The diagnostic and therapeutic approach involves a multidisciplinary discussion between neurosurgeons, obstetricians, anesthesiologists, oncologists and orthopedists. The decisions are made according to tumor biology, stage, gestational age, degree of spinal cord compression and fetal risks. There are three possible therapeutic scenarios during pregnancy(7).
1. Ideal case: adhere to standard treatment as for nonpregnant patients.
2. Immediate treatment needed: medication or surgery may put pregnancy at risk and may need termination of pregnancy; or terminate pregnancy and then start treatment.
3. In the later stages of pregnancy: delivery followed by treatment.
The surgical removal of most pregnancy-related spinal tumors can be delayed until postpartum, except for malignancies. Conservative treatment is the first choice for pregnant patients with benign adolescent tumors, but pain control is very important. Muscle relaxants and NSAIDs are not recommended in pregnancy. Some authors reported having successfully used acetaminophen(8).
The sudden deterioration of symptoms can be found during pregnancy, therefore close surveillance is required. MRI reexamination at three months during conservative approach is recommended and surgical treatment is applied according to gestational age(3). According to literature studies, if patients at 32 to 36 weeks of gestation or later had a sudden deterioration and required immediate treatment, the induction of delivery or elective caesarean section can be performed. Many authors recommend elective caesarean section in order to avoid the sudden deterioration during vaginal delivery(9).
Spinal surgery can be performed in the postpartum, but in some cases prepartum surgery is needed, with the risk of preterm labor or fetal damage. The neurological deficit due to rapid tumor growth during pregnancy is difficult to recover even in the postpartum, but in severe cases pregnant women may die if a highly malignant tumor is not timely treated during pregnancy(10).
Conclusions
Schwann cell tumor is the most common intradural tumor found in both male and female patients. It can be diagnosed as a pregnancy-related spinal tumor, its symptoms being triggered by physiological and pathological changes during pregnancy. The incidence is rare, but rapid growth due to hormonal and hemodynamical fluctuations lead to spinal cord compression with severe outcomes.
Our case illustrates how pregnancy complicated by even a mild degree of pregnancy-induced hypertension can unmask a preexisting, otherwise silent, schwannoma by causing severe symptoms of spinal cord compression. Moreover, our case highlights the importance of a multidisciplinary management of patients with pregnancy-related spinal tumors.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
Antinheimo J, Sankila R, Carpen O, Pukkala E, Sainio M, Jääskeläinen J. Population-based analysis of sporadic and type 2 neurofibromatosis-associated meningiomas and schwannomas. Neurology. 2000; 54(1):71-1.
-
Chamberlain MC, Tredway TL. Adult primary intradural spinal cord tumors: a review. Curr Neurol Neurosci Rep. 2011; 11(3):320-8.
-
Meng T, Yin H, Zhou W, Wang J, Xiao J. Therapeutic strategy and outcome of spine tumors in pregnancy: a report of 21 cases and literature review. Spine (Phila Pa 1976). 2015; 40(3):146-53.
-
Samii M, Giordano M. Spinal Schwannomas. In: Arnautović KI, Gokaslan ZL(Eds), Spinal Cord Tumors. Springer. 2019; 161-69.
-
Pikis S, Cohen JE, Rosenthal G, Barzilay Y, Kaplan L, Shoshan Y, Itshayek E. Spinal meningioma becoming symptomatic in the third trimester of pregnancy. J Clin Neurosci. 2013; 20(12):1797-9.
-
Hilton DA, Hanemann CO. Schwannomas and their pathogenesis. Brain Pathology. 2014; 24(3):205-20.
-
Moran BJ, Yano H, Al Zahir N, Farquharson M. Conflicting priorities in surgical intervention for cancer in pregnancy. Lancet Oncol. 2007; 8(6):536-44.
-
Vijay K, Shetty AP, Rajasekaran S. Symptomatic vertebral hemangioma in pregnancy treated antepartum. A case report with review of literature. Eur Spine J. 2008; Suppl 2:S299-303.
-
Cardonick E, Dougherty R, Grana G, Gilmandyar D, Ghaffar S, Usmani A. Breast cancer during pregnancy: maternal and fetal outcomes. Cancer J. 2010; 16(1):76-82.
-
Dham BS, Kwa DM, Campellone JV. Postpartum paraparesis from spinal neurofibroma. Spine J. 2012; 12(7):e5-8.