Objective. The aim of our study was to establish if high-field post-mortem MRI at 7T can perform three-dimensional measurements of the fetal heart, and retrieve results comparable to post-mortem macroscopic measurements performed at autopsy, in fetuses with whole body weight below 500 g. Methodology. Twelve second-trimester fetuses with gestational ages ranging from 13 to 19 weeks of gestation were considered. All fetuses resulted from therapeutic termination of pregnancy (TOP) due to plurimalformative syndromes or chromosomal anomalies. All cases were immersed in 10% formalin solution, and after proper fixation they were examined using high-field MRI at 7T. After post-mortem imagistic examination, all cases were submitted to conventional autopsy. Three-axis cardiac measurements were performed by both examination methods, using the same landmarks. Results. We observed a strong correlation between post-mortem MRI measurements at 7T and post-mortem macroscopic measurements at autopsy, with p<0.001. The coefficient of correlation (r) for all three axes was above or equal to 0.90. Bland Altman plots showed overall good agreement between measurements performed by both methods. Conclusions. Using 7T post-mortem MRI for three-dimensional morphometric evaluation of the fetal heart in the second-trimester fetuses with a body weight less than 500 g, the obtained results are comparable to the macroscopic measurements performed during conventional autopsy.
Evaluarea RMN-ului post-mortem de 7T în comparaţie cu autopsia convenţională: un studiu morfometric
Evaluation of post-mortem high-field MRI at 7T compared to conventional autopsy: a morphometric study
First published: 28 octombrie 2021
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/ObsGin.69.3.2021.5552
Abstract
Rezumat
Obiective. Scopul studiului nostru a fost de a stabili dacă RMN-ul post-mortem la 7T poate efectua măsurători tridimensionale ale inimii fetale şi dacă poate obţine rezultate comparabile cu ale măsurătorilor macroscopice post-mortem efectuate la autopsie, la feţii cu greutate corporală mai mică de 500 g. Metodologie. Au fost luaţi în considerare 12 feţi de trimestrul al doilea, cu vârsta gestaţională cuprinsă între 13 şi 19 săptămâni de amenoree. Toţi feţii au rezultat în urma întreruperii terapeutice a sarcinii (TOP) din cauza unor sindroame plurimalformative sau a prezenţei anomaliilor cromozomiale. Toate cazurile au fost fixate corespunzător în soluţie de formaldehidă 10%, iar ulterior au fost examinate folosind un aparat RMN de 7T. După examinarea imagistică post-mortem, toate cazurile au fost supuse autopsiei convenţionale. Măsurătorile cardiace pe trei axe au fost efectuate prin ambele metode de examinare, folosind aceleaşi repere. Rezultate. S-a observat o corelaţie puternică între măsurătorile RMN post-mortem la 7T şi măsurătorile efectuate la autopsie, cu p<0,001. Coeficientul de corelaţie (r) pentru toate cele trei axe măsurate a fost mai mare sau egal cu 0,90. Graficele Bland Altman au arătat o asociere în general bună între măsurătorile efectuate prin ambele metode. Concluzii. Utilizând RMN-ul post-mortem de 7T pentru evaluarea morfometrică tridimensională a cordului fetal la feţii de trimestrul al doilea, cu greutate corporală mai mică de 500 g, se obţin rezultate comparabile cu cele ale măsurătorilor macroscopice efectuate în timpul autopsiei convenţionale.
Introduction
Congenital heart disease continues to be a frequent cause of mortality and morbidity among children(1), with a prevalence of 81.70 (80.87-82.54)/10.000 births, according to EUROCAT data(2). Autopsy continues to be the gold standard for post-mortem examination. Though challenging, currently worldwide fetal cardiac dissection techniques can successfully follow the sequential segmental analysis system and visualize any structural abnormalities(3,4).
However, a sustained decline in autopsy consent rates has been observed worldwide in the last decade, due to either religious or personal concerns of the parents regarding the autopsy process(5). A complete post-mortem diagnosis is required for the proper counseling of future pregnancies. This has led to the development of numerous noninvasive post-mortem examination techniques, such as post-mortem magnetic resonance imaging (MRI), post-mortem ultrasound, and various techniques involving computed tomography (CT)(6) and microcomputed tomography for cardiac structural evaluation(7,8).
In the last decades, numerous small studies have reported post-mortem MRI as a potential alternative to conventional autopsy(9). For cardiac examination, conventional post-mortem MRI at 1.5T or 3T proved to be a good diagnostic tool even for complex congenital heart disease in fetuses with a gestational age beyond 16 weeks or with a body weight below 500 grams(10-12). For smaller fetuses, in the latest years, the significant advances in high-field MRI have shown better results for the visualization of cardiac structures, even in embryos, when compared to conventional autopsy(13-15).
Along with post-mortem evaluation, several studies were published using high-field MRI at 7T for in vivo evaluation, thus giving new usage for high-power magnets(16-18). For fetal cardiac examination, apart from fetal heart weight, morphometric studies regarding cardiac dimensions according to gestational age are lacking. An important question is whether cardiac measurements obtained by post-mortem MRI at 7T are comparable with those performed during autopsy in small fetuses. We considered that this could be an important aid tool for the future development of normal value charts regarding cardiac development, considering the decreasing rate of fetal autopsies worldwide. Post-mortem studies such as ours could be a starting point for future in vivo morphometric studies that would have a great impact in the more detailed evaluation of the fetal heart.
The aim of our study was to evaluate the accuracy of high-field post-mortem MRI at 7T in performing three-dimensional measurements of the fetal heart, compared to post-mortem macroscopic measurements at autopsy, in second-trimester fetuses.
Materials and method
General considerations
This study comprised 12 second-trimester fetuses with gestational ages ranging from 13 to 19 weeks of gestation (WG), calculated from the day of the last menstrual cycle, and with a weight below 500 g. All fetuses resulted from therapeutic termination of pregnancy (TOP) due to plurimalformative syndromes or chromosomal anomalies carried out using prostaglandins, administered locally and orally in the First Clinic of Obstetrics and Gynecology of the Emergency County Clinical Hospital of Cluj-Napoca, Romania, according to the internal protocol of the department.
All cases were referred to IMOGEN – the medical research institute within the Emergency County Clinical Hospital of Cluj-Napoca, between January 2015 and December 2017, for imagistic post-mortem assessment and autopsy. The study protocol was approved by the “Iuliu Haţieganu” University of Medicine and Pharmacy Ethics Committee, Romania (REG. 306/ 12.07.2017). The written informed parental consent for the scientific use of patient data was obtained before the imagistic and conventional autopsy procedures. All cases were handled according to the Human Tissue Act (2004).
The inclusion criteria were: second-trimester gestational age fetuses, whole body weight below 500 g, and interpretable post-mortem MRI scans at 7T.
We excluded second-trimester fetuses with whole body weight above 500 g, without post-mortem MRI scans at 7T, severe maceration, or presenting traumatic lesions.
After proper formalin fixation in 10% buffered formalin solution, all cases that fulfilled the aforementioned criteria were scanned using a 7-Tesla Bruker BioSpec machine, with high magnetic field gradient unit (BGA 9 S HP) and turbo spin-echo high-resolution T2-weighted imaging (T2 WI) protocol. The details on the preparation of the fetuses and the scanning protocol used have been described in previous papers(19).
Following the post-mortem MRI examination, all fetuses were submitted to conventional autopsy, carried out according to the French Society of Fetal Pathology guidelines for invasive autopsies(20).
Three-axis cardiac measurements were performed first by pm-MRI at 7T and secondly by classic autopsy using the same landmarks. Transverse axis measurements were performed on the maximum width of both ventricles. The base-apex axis measurement started at the apex and till the most distal point of the atriums. The highest value was taken into consideration. The third measurement, on the antero-inferior axis, followed a perpendicular line to the one corresponding to base-apex axis, that crossed the base of the ventricles (Figure 1).
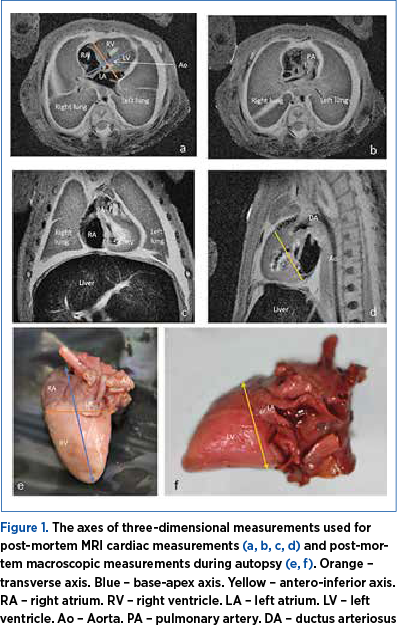
Post-mortem MRI measurements were performed on multiple sections, and the highest value was taken into consideration (Figure 1).
For statistical analysis, Microsoft Excel 2016 was used. To evaluate the relationship between macroscopic measurements and post-mortem MRI measurements, we used the Pearson’s correlation coefficient r. A level of p value below a=0.05 was considered to indicate a statistically significant result. The numerical data were presented as arithmetic means ± standard deviation (SD) if normally distributed or median (25th-75th percentile) if not.
To compare the differences (Delta) obtained between post-mortem MRI measurements and conventional autopsy measurements, a Student’s t-test for independent sample was used. To establish the agreement between the two types of quantitative measurements we used the Bland Altman plots using Bland Altman Confidence calculator attached to Carkeet A(21).
Results
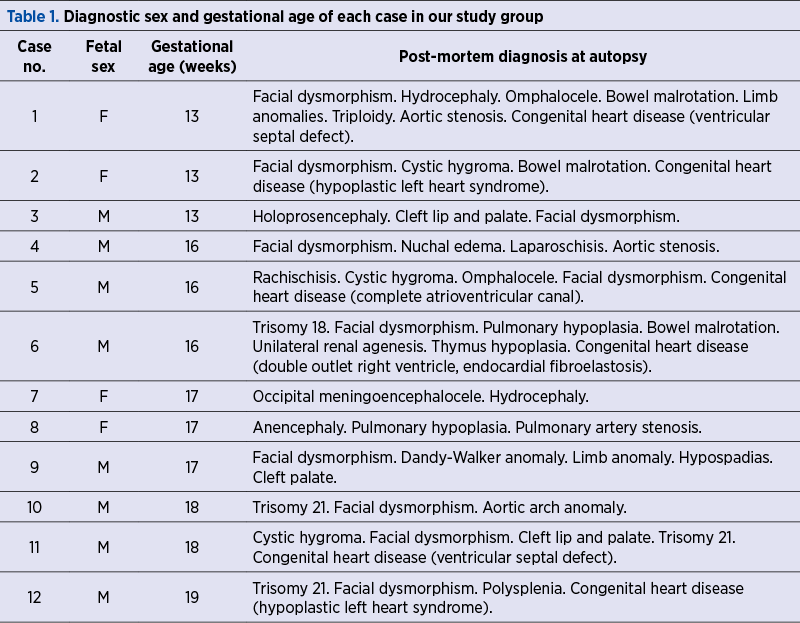
The mean whole-body weight of the fetuses considered was 118.33 g, with a median of 89 g (52.5;160.5). The mean gestational age was 16.5 WG (15.25;17.25). Eight fetuses (67%) had male genital differentiation, and four (33%) had female genital differentiation. All included cases presented various structural abnormalities, described in detail in Table 1.
The descriptive analysis for numerical data is presented in Table 2.
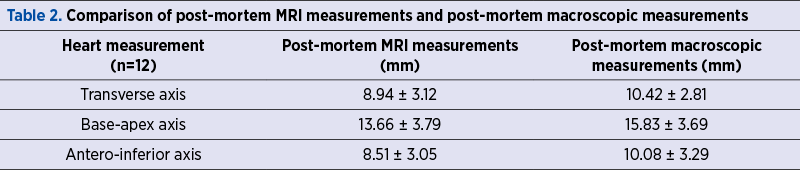
We observed a strong correlation between both measurements, with p<0.001 for all considered axes. The coefficient of correlation (r) for transverse axis measurements was 0.98, for base-apex axis measurements it was 0.90, and for antero-inferior axis measurements it was 0.93.
We observed small differences between post-mortem MRI measurements and their corresponding conventional autopsy measurements, this being evidentiated as follows. For transverse axis measurements, the mean of differences was 1.48 ± 1.72 mm, p=0.2; for base-apex axis measurements, the mean of differences was 2.17 ± 1.66 mm, p=0.81; and for antero-inferior axis measurements, the mean of differences was 1.57 ± 1.23 mm, p=0.33.
The agreement between the two examination methods was highlighted by using Bland Altman plots, which showed an overall good agreement between post-mortem macroscopic measurements and post-mortem MRI measurements, as all plot markers were located between the upper and lower limits of agreement and their standard deviations (±2 SD) for each measured structure (Figure 2).
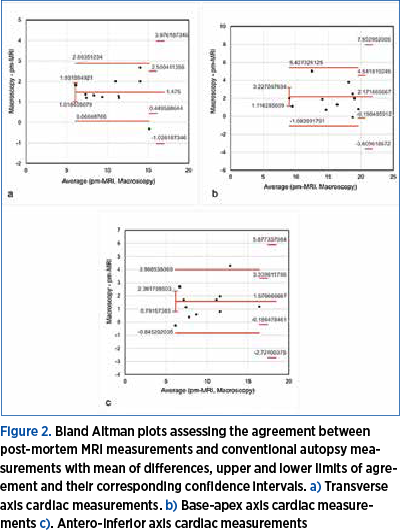
Out of all measurements, we observed two cases in which the corresponding marks in the plots were outside the limit of agreement, but still inside the corresponding standard deviation interval.
In the first case (Figure 2a), the point at the highest distance from the limit of agreement corresponds to Case no. 7, in which we observed that post-mortem MRI measurement was higher than post-mortem macroscopic measurement by 0.3 mm. Hence, all post-mortem MRI measurements were generally smaller than post-mortem macroscopic measurements, this case being pointed out by the analysis. In the other case (Case no. 12), observed in Figure 2c, post-mortem pathological measurements were higher than post-mortem MRI by 4 mm, and the standard deviation for antero-inferior axis measurements was 3.28 mm. In both cases, the different values were less than 1 millimeter and were the result of the measuring techniques.
The best agreement was observed for transverse axis measurements, this being highlighted by the higher degree of clustering around the line of agreement in the corresponding plot, compared to the other two plots.
Discussion
The present study proposes a simple and reproducible method for the morphometric evaluation of the fetal heart using post-mortem MRI at 7T. The imagistic post-mortem three-dimensional measurements performed are comparable to those performed at autopsy, in fetuses with mean gestational age of 16.5 weeks and mean fetal weight of 118.33 g. We observed a very strong correlation between post-mortem MRI at 7T measurements and macroscopic measurements at autopsy, especially for transverse axis measurements of the fetal heart (correlation coefficient r of 0.98, p<0.001).
As expected, the differences between measurements existed and they can be explained by the fact that post-mortem MRI measurements were performed in situ and the post-mortem measurements were performed after opening the thoracic cavity during conventional autopsy and after organ removal from the thoracic cavity. Formalin fixation is known to have an impact on the volume of examined tissues(22).
Also, post-mortem MRI measurements and conventional autopsy measurements were performed at different time points after 10% formalin fixation. The duration of this fixation process is known to cause morphometric changes in cardiac muscle, as an increased thickness of the cardiac muscle(23). However, there were no statistically significant differences between the two measurement methods.
Studies evaluating post-mortem MRI measurements of the heart compared to traditional autopsy measurements are scarce in the literature and were conducted only on adult populations(24-30).
Even though our study refers to fetal population, we also found a good correlation between measurements, in concordance with data previously published(26,27). Still, as opposed to previous studies, our post-mortem MRI measurements were slightly smaller than the post-mortem macroscopic measurements(27). To our best knowledge, this is the first study comparing fetal cardiac post-mortem MRI measurements with conventional autopsy measurements.
The good accuracy of the images obtained using 7T high-field MRI may recommend its use for post-mortem fetal investigation, particularly if specialists in fetal pathology are lacking or when parents refuse fetal autopsy. Considering the continuous development of MRI machines and protocols, in vivo fetal cardiac examination is now possible, even though only for research purposes(31). In this context, post-mortem MRI imaging morphometric studies could be useful for cardiac evaluation not only in the case of virtual autopsy, but also for the in vivo assessment of the fetus.
The main limitation of our study is the small number of cases. Our study group comprised second-trimester fetuses with whole body gestational age below 500 g. The median body weight was 89 g (52.5;160.5), and this could explain the discordance between our study and those previously published. Further studies on larger fetal populations are required to better evaluate the ability of high-field post-mortem MRI to perform measurements of the fetal heart comparable with conventional autopsy.
Conclusions
Our study shows that post-mortem MRI at 7T can be a useful tool in performing cardiac three-dimensional measurements that are comparable with macroscopic measurements performed during conventional autopsy in second-trimester fetuses with whole body weight below 500 g.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
REFERENCES
-
Srivastava D, Olson EN. A genetic blueprint for cardiac development. Nature. 2000 Sep 14;407(6801):221-6. https://pubmed.ncbi.nlm.nih.gov/11001064/
-
Prevalence charts and tables. EU RD Platform [Internet]. [cited 2021 Jul 10]. Available at: https://eu-rd-platform.jrc.ec.europa.eu/eurocat/eurocat-data/prevalence_en
-
Anderson R, Shirali G. Sequential segmental analysis. Annals of Pediatric Cardiology. 2009 Jan-Jun; 2(1):24–35.
-
Erickson LK. An Approach to the Examination of the Fetal Congenitally Malformed Heart at Autopsy. Journal of Fetal Medicine. 2015 Sep 4;2(3):135–41.
-
Addison S, Arthurs OJ, Thayyil S. Post-mortem MRI as an alternative to non-forensic autopsy in foetuses and children: From research into clinical practice. British Journal of Radiology. 2014 Apr;87(1036):20130621.
-
Shelmerdine SC, Hutchinson JC, Arthurs OJ, Sebire NJ. Latest developments in post-mortem foetal imaging. Prenatal Diagnosis. 2020 Jan 1;40(1):28–37.
-
Lombardi CM, Zambelli V, Botta G, Moltrasio F, Cattoretti G, Lucchini V, et al. Postmortem microcomputed tomography (micro-CT) of small fetuses and hearts. Ultrasound in Obstetrics & Gynecology. 2014 Nov 1;44(5):600–9.
-
Hutchinson JC, Arthurs OJ, Ashworth MT, Ramsey AT, Mifsud W, Lombardi CM, et al. Clinical utility of postmortem microcomputed tomography of the fetal heart: Diagnostic imaging vs macroscopic dissection. Ultrasound in Obstetrics and Gynecology. 2016 Jan 1;47(1):58–64.
-
Thayyil S, Sebire NJ, Chitty LS, Wade A, Olsen O, Gunny RS, et al. Post mortem magnetic resonance imaging in the fetus, infant and child: A comparative study with conventional autopsy (MaRIAS Protocol). BMC Pediatrics. 2011 Dec 22;11(1):120.
-
Kang X, Cannie MM, Arthurs OJ, Segers V, Fourneau C, Bevilacqua E, et al. Post-mortem whole-body magnetic resonance imaging of human fetuses: a comparison of 3-T vs. 1.5-T MR imaging with classical autopsy. European Radiology. 2017 Aug 1;27(8):3542–53.
-
Jawad N, Sebire NJ, Wade A, Taylor AM, Chitty LS, Arthurs OJ. Body weight lower limits of fetal postmortem MRI at 1.5 T. Ultrasound in Obstetrics & Gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2016 Jul 1;48(1):92–7.
-
Sandaite I, Dymarkowski S, de Catte L, Moerman P, Gewillig M, Fedele L, et al. Fetal heart pathology on postmortem 3-T magnetic resonance imaging. Prenatal Diagnosis. 2014 Mar;34(3):223–9.
-
Votino C, Jani J, Verhoye M, Bessieres B, Fierens Y, Segers V, et al. Postmortem examination of human fetal hearts at or below 20 weeks’ gestation: A comparison of high-field MRI at 9.4 T with lower-field MRI magnets and stereomicroscopic autopsy. Ultrasound in Obstetrics and Gynecology. 2012 Oct;40(4):437–44.
-
Kose K. Magnetic Resonance Microscopy of Chemically Fixed Human Embryos Performed in University of Tsukuba Since 1999 to 2015. The Anatomical Record. 2018 Jun 1;301(6):987–97.
-
Tyszka JM, Fraser SE, Jacobs RE. Magnetic resonance microscopy: Recent advances and applications. Current Opinion in Biotechnology. 2005 Feb;16(1):93-9.
-
Federau C, Gallichan D. Motion-Correction Enabled Ultra-High Resolution In-Vivo 7T-MRI of the Brain. PLoS One. 2016 May 1;11(5):e0154974.
-
Veluw SJ van, Zwanenburg JJM, Engelen-Lee J, Spliet WGM, Hendrikse J, Luijten PR, et al. In vivo detection of cerebral cortical microinfarcts with high-resolution 7T MRI. Journal of Cerebral Blood Flow & Metabolism. 2013 Mar 9;33(3):322.
-
Thomas BP, Welch EB, Niederhauser BD, Whetsell WO, Jr, Anderson AW, et al. High-Resolution 7T MRI of the Human Hippocampus In Vivo. Journal of Magnetic Resonance Imaging. 2008 Nov;28(5):1266.
-
Staicu A, Albu C, Popa-Stanila R, Chiriac L, Boitor-Borza D, Bondor C, et al. Potential clinical benefits and limitations of fetal virtopsy using high-field MRI at 7 Tesla versus stereomicroscopic autopsy to assess first trimester fetuses. Prenatal Diagnosis. 2019 Jun 1;39(7):505–18.
-
Férechté ER. Pathologie foetale & placentaire pratique/ouvrage collectif de la Société française de foetopathologie, SOFFOET; coordonateurs Férechté E-Razavi, Dominique Carles; sous la direction de Raymonde Bouvier, Dominique Carles, Marie-Christine Dauge, et al. Sauramps médical. 2008.
-
Carkeet A. A Review of the Use of Confidence Intervals for Bland-Altman Limits of Agreement in Optometry and Vision Science. Optometry and Vision Science. 2020 Jan;97(1):3-8.
-
Weisbecker V. Distortion in formalin-fixed brains: Using geometric morphometrics to quantify the worst-case scenario in mice. Brain Structure and Function. 2012 Apr;217(2):677–85.
-
Hołda MK, Klimek-Piotrowska W, Koziej M, Piątek K, Hołda J. Influence of different fixation protocols on the preservation and dimensions of cardiac tissue. Journal of Anatomy. 2016 Aug 1;229(2):334.
-
Jakobsen LS, Lundemose S, Banner J, Lynnerup N, Jacobsen C. Forensic postmortem computed tomography: volumetric measurement of the heart and liver. Forensic Sci Med Pathol. 2016;12(4):510–6.
-
Troxler R, Minoiu C, Vaucher P, Michaud K, Doenz F, Ducrot K, et al. The role of angiography in the congruence of cardiovascular measurements between autopsy and postmortem imaging. Int J Legal Med. 2018;132(1):249–62.
-
Chatzaraki V, Thali MJ, Schweitzer W, Ampanozi G. Left myocardial wall measurements on postmortem imaging compared to autopsy. Cardiovasc Pathol. 2019;43:107149.
-
Ampanozi G, Hatch GM, Flach PM, Thali MJ, Ruder TD. Postmortem magnetic resonance imaging: reproducing typical autopsy heart measurements. Leg Med (Tokyo). 2015;17(6):493–8.
-
Gheorghe AG, Fuchs A, Jacobsen C, Kofoed KF, Møgelvang R, Lynnerup N, et al. Cardiac left ventricular myocardial tissue density, evaluated by computed tomography and autopsy. BMC Med Imaging. 2019;19(1):29.
-
Okuma H, Gonoi W, Ishida M, Shintani Y, Takazawa Y, Fukayama M, et al. Heart wall is thicker on postmortem computed tomography than on antemortem [corrected] computed tomography: the first longitudinal study. PLoS One. 2013;8(9):e76026.
-
Ampanozi G, Hatch GM, Flach PM, Thali MJ, Ruder TD. Postmortem magnetic resonance imaging: Reproducing typical autopsy heart measurements. Legal Medicine (Tokyo, Japan). 2015;17(6):493–8.
-
Roy CW, Amerom JFP van, Marini D, Seed M, Macgowan CK. Fetal Cardiac MRI: A Review of Technical Advancements. Topics in Magnetic Resonance Imaging. 2019 Oct 1;28(5):235.