Suicide prevention is an ongoing concern of public health policies, and a pressing requirement both in regular times, and especially during exceptional social contexts. Suicide prevention becomes a challenge and requires a special focus during the management of the COVID-19 pandemic. In the context of overall uncertainty and insecurity, preserving mental health and implementing suicide prevention strategies are valid and confirmed concerns. The role of media in triggering or precipitating suicide risk has been repeatedly outlined. The current article succinctly reviews the protective role of media and the risk factors for suicide which mass media can influence, to the benefit or detriment of persons at risk for suicide. Starting from the most widely known cases of suicide contagion in fiction or printed press, from Goethe to the Vienna case, this article outlines landmarks for mental health promotion and suicide prevention, myths concerning suicide, and the recommendations of World Health Organization for media reporting of suicide. Fact checking, abandoning sensationalistic and dramatic styles of reporting, providing contact information for available help and accurate information for readers are some of the listed recommendations. The current article emphasizes the preventive role of a responsible approach to information and accurate reporting in the media, especially in the context of the COVID-19 pandemic.
Mass-media – factor de risc şi de protecţie pentru comportamentul suicidar în timpul pandemiei de COVID-19
Mass media – risk and protective factor against suicidal behaviour in the COVID-19 pandemic
First published: 20 noiembrie 2020
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Psih.63.4.2020.3952
Abstract
Rezumat
Prevenţia suicidului constituie o preocupare constantă a politicilor de sănătate publică şi o nevoie reală atât în perioadele obişnuite, dar mai ales în cele marcate de situaţii sociale excepţionale. În managementul pandemiei de COVID-19, prevenţia suicidului devine provocatoare şi necesită o atenţie aparte. Pe fondul insecurităţii, păstrarea sănătăţii mintale şi adoptarea unor strategii de prevenţie a suicidului sunt justificate şi confirmate. Rolul mass-mediei în declanşarea sau catalizarea riscului de suicid a fost subliniat în mai multe rânduri. Articolul de faţă prezintă într-o formă succintă rolul protectiv şi factorii de risc ai suicidului asupra cărora mass-media poate acţiona, în avantajul sau în dezavantajul persoanelor cu risc suicidar. Plecând de la raportarea celor mai cunoscute cazuri de contagiune suicidară, din literatură sau din presa scrisă, de la Goethe la cazul Viena, în articol sunt sintetizate date statistice ce constituie repere în abordarea sănătăţii mintale şi prevenţiei suicidului, alături de miturile legate de suicid, dar şi recomandările Organizaţiei Mondiale a Sănătăţii de abordare a raportării suicidului în mass-media. Validarea informaţiei, abandonarea senzaţionalului, lipsa dramatizării în relatările din mass-media, oferirea de informaţii de contact şi informarea corectă a cititorilor sunt câteva din recomandările indicate. Tratarea informaţiei cu responsabilitate şi raportarea corectă în mass-media, în condiţiile actuale ale pandemiei de COVID-19, rezidă şi din abordarea acestui articol.
Introduction
The management of the COVID‑19 pandemic is a global public health challenge, and also an ensuing global crisis of the health care system.
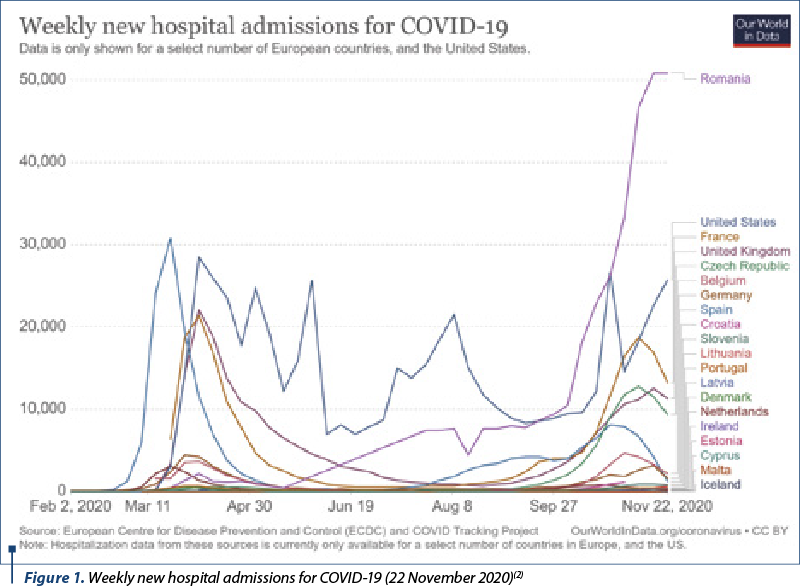
The COVID-19 pandemic, emerging at the end of 2019 and officially declared as pandemic in March 2020, continues to affect populations on a global scale, spreading in almost all countries, except some island states where containment was facilitated by geography. Currently (23.11.2020), there are approximately 59 million confirmed cases (0.75% of the world population), but the World Health Organization (WHO) estimates that approximately 10% of the global population is infected, the highest percentage consisting in asymptomatic persons. The number of deaths is also on the rise, with a fatality rate of 2.37% of confirmed patients(1). There are approximately 430,000 confirmed cases in Romania until now, representing 2.2% of the country population, with a fatality rate of 2.4% of the confirmed cases – i.e., 10,177 deaths until now (10 November 2020). The alarming issue is the recent significant rise of infections, with an impressive increase of hospitalizations and an overwhelming pressure on health care system, most of the times extending more than the emergency units, intensive care units, infectious diseases and pulmonology hospitals (Figure 1).
Preserving mental health becomes a requirement in this context, for optimal coping with this new type of somatic and emotional trauma. The management of the anxiety and stress levels is the greatest challenge. The main sources of stress during the pandemic are: fear of getting sick with COVID-19 or illnesses requiring emergency medical care, the effect of pshysical distancing on social relationships, increased level of family discord, family violence, changes in daily habits and routines due to remote work, online school, decreased opportunities for leisure activities (sports, entertainment, trips, vacations), financial issues generated by the economic crisis, unemployment, decreased income, bankruptcy, uncertainty regarding medical, financial, social future of the person and the group of close ones.
The specific population groups, with increased vulnerability for mental health issues, perceive a greater impact of stress. These vulnerable groups are: persons with preexisting mental health problems, patients infected with SARS-CoV-2, bereaved persons, medical staff, senior citizens, migrants, inmates.
Recent data from the UK outline that 80% of young persons with preexisting mental health disorders report the worsening of mental health, increased anxiety, sleep disorders, panic attacks, and self-harm in those with prior suicide attempts.
The Chinese researchers report that 20% of patients experienced a worsening of mental health and also stopping medication, while 32% experienced typical post-traumatic stress disorder (PTSD) symptoms. Approximately 12% of patients experienced moderate or severe suicidal ideation(3).
The impact of SARS-CoV-2 infection involves not only the patients diagnosed with COVID-19, but also those who came in contact with these patients. COVID-19 patients and their contacts are affected by legally imposed quarantine measures, which generate negative affective states. Thus, 96.2% of COVID-19 patients reported PTSD(4), and 10-20% of bereaved survivors develop pathological bereavement(5).
Depression, suicide and psychological contagion continue to represent a problem during the COVID-19 pandemic. Psychological contagion generating suicide is not a new fact; it has been reported historically in Antiquity (ex.: the Milet virgins suicide), the news of the fatal gesture being spread through oral reports. Also, psychological contagion may spread via texts, such as W. Goethe’s novel Young Werther’s Sufferings, and, currently, quick dissemination of information via online media and social media.
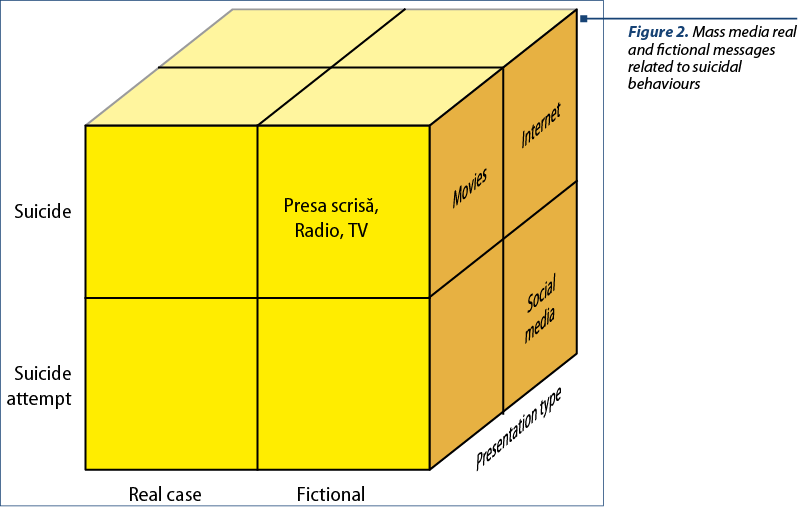
Various sources of dissemination of information related to suicide may trigger or promote suicide of the persons at risk for suicidal behaviours. These sources may be direct, such as people around the at-risk person, or indirect, such as novels, plays, music lyrics, movies, printed media, radio, TV, internet (including social media). Mass media spread news regarding the suicide of public figures, VIPs and socially relevant person, and become an action trigger for suicidal persons. The media messages which influence suicidal behaviour are remarkably notorious in volume and extent (Figure 2).
The way in which mass media presents suicide-related news may negatively impact the suicide risk and may lead to contagion in acting out suicidal behaviour.
The media dilemma consists in presenting news in a language as appealing as possible, emphasizing sensationalistic elements, faced with constraints imposed by confidentiality, which might decrease the public interest for that news. Certain types of presentations end up as becoming extremely harmful, acting like a catalyst, triggering self-harming behaviours by imitation in people at risk for suicide.
Several myths regarding suicide are promoted via mass media, such as:
-
“The ones who talk about suicide are the ones who least attempt suicide.”
-
“If someone wishes to kill himself, there is nothing that can be done to stop him.”
-
“Suicidal persons are determined to die.”
-
“If someone repeats «cry for help» behaviours, they will not kill themselves.”
-
“Talking about suicide with the suicidal person encourages suicidal behaviour.”
-
“Only persons with mental illness will truly attempt suicide.”
-
“A gastric lavage will teach those who commit reckless gestures to stop repeating them.”
-
“A person who is now at risk for suicide will forever remain at risk.”
-
“Suicide may be a relief, not only for the person, but also for the ones around.”
Mass media has the capacity to become a protective factor against suicide, even in the times of pandemic, by communicating and disseminating a wide array of information about: online self-help programs, the importance of psychological hygiene and mental health, the importance of decreasing harmful alcohol use, news about facilitating access to mental health services through telepsychiatry, campaigns to reduce stigma attached to persons with COVID-19 and, last but not least, abandoning emphatic news about suicide and replacing this way of communicating with balanced, responsible media accounts.
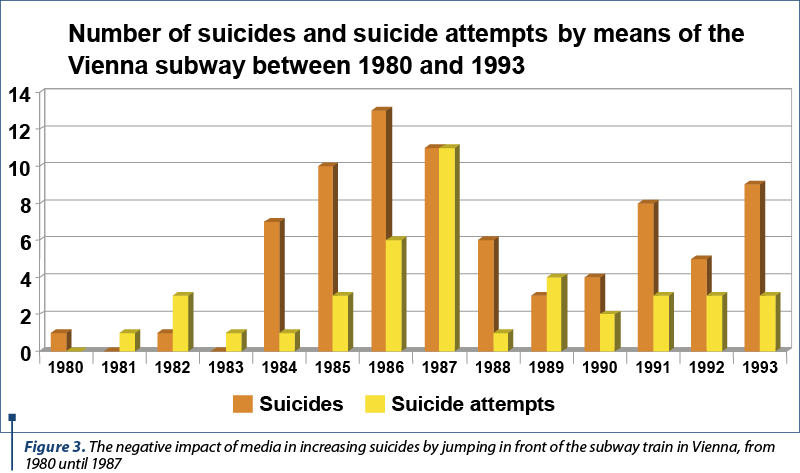
Mental health professionals are aware of the power of media in shaping people’s beliefs, ways of interpreting new information, and – in the case of persons with mental health-related vulnerabilities – triggering disfunctional behaviours. Such a negative media impact was identified in Vienna, around 1984, when many suicides by jumping in front of the subway train were recorded. The press widely presented these situations, in a dramatic manner, as sensationalistic events. Therefore, a significant increase of this means of suicide in Austrians was recorded. The implementation in 1987 of recommendations for suicide reporting via the partnership of the Association of Austrian Psychiatrists and journalists led to a significant decrease of suicides by this means (Figure 3)(6).
We can currently talk about a copycat effect, a psychological contagion via social media, similar with the effect generated by dissemination of news via printed media, radio, TV or internet. The number of persons who post messages with suicidal content on social media and are livestreaming suggest that this type of behaviour is on the rise.
Therefore, Facebook took several actions in order to mitigate this effect which is detrimental to the mental health of network users. In 2015, Facebook launched a program which identifies messages/posts with suicidal content, by implementing algorhythms to search and report these posts by the network of friends. Moreover, Facebook recommends a quick response and allerting an emergency service for intervention. The company declared that it develops a software to monitor and respond, with the help of artificial intelligence, when suicidal intent is reported “on a global scale” via Facebook.
Fears regarding health, one’s own and of loved ones, and concerns regarding social and economical consequences of the global medical crisis generated by the COVID-19 pandemic are amplified through daily exposure to news received by all media channels. The frequent exposure to negative media accounts or negative social media interactions may increase stress, anxiety and depression. Suicide presented by media accounts during the pandemic needs to be nuanced and complex. In no shape or form, the connection between suicide and the pandemic should be presented as a unique or main cause of suicide. It is known that suicide has multiple causes, including psychological issues prior to the pandemic. Also, the proximal risk factors, such as personal (breakups, conflicts) or social crisis (economic loss, unemployment) may also be involved. Therefore, the international experts recommend promoting information which helps the public understand suicidal phenomenon(1). This is best achieved through promoting perspectives of experts in mental health and suicidology, especially by discussing the risk factors for the suicidal behaviour.
Disseminating information about how to recognize a person with suicidal thoughts and how to optimally approach these situations is very important. Media also has the power to fight off myths about suicide. Thus, accounts avoiding simplistic approaches of suicidal acts (emphasis on a single cause or coincidences) and avoiding glorification of “suicide as an act of courage” are highly appreciated. Accounts that break the confidentiality regarding identity, address, profession, social status of the person in question, and give away details about the suicide method are NOT permitted.
In describing public fatal events, journalists are advised not to use terms such as successful or unsuccessful suicide attempt, victim of suicide, committing suicide, person with suicidal tendencies, person predisposed to suicide. It is preferable to use terms such as: suicide, death due to suicide, suicide attempt, person with suicide risk, help to prevent suicide.
As a general principle, WHO recommends approaching suicide through many angles: suicide as public health issue, not a sensational account; reporting comparative statistical data on suicide according to geographical area, age groups or sex. Strategies to include suicide prevention in international and national public health policies has become a long-term plan of the World Health Organization. According to this global perspective, media accounts of suicide are significant for influencing the good practices for communicating medical and social issues on a populational level.
WHO outlines the proposed good practices to be followed in reporting suicide deaths during the pandemic. As a general remark, deaths of other nature than those caused by the pandemic are noticeably ignored.
During these uncertain times, if a suicide becomes a media account, it is indicated that the journalists respect the WHO good practices guideline:
-
Suicide is NOT to be attributed to the pandemic; the speculations regarding medical causes of death should be avoided if there is no clear evidence.
-
The news should be clear and fair, not blaming the medical staff by promoting the opinion that suicide could have been prevented with professional help, even without hospitalization.
-
Will the news educate, inform, clarify facts, and help prevent other suicides?
-
Precautions should be used in deciding to include statements of bereaved survivors, especially if the pandemic is incriminated as the main cause of suicide.
-
Messages of hope should be often added, by reporting successful stories of healing and recovery.
-
Mass media should include contact data of crisis lines (local, national, international) in news about suicides, as a professional obligation, and also emergency lines for medical issues. As a moral obligation, media professionals should respect the death of a person and the suffering of the family, should consider the impact of the news on vulnerable persons, and present with extreme caution the suicide of celebrities and especially the methods used.
Conclusions
In order to become a protective factor against suicide, mass media needs to follow specific directions and good practices in presenting the suicidal events. Presenting news about persons who effectively deal with the suicidal crisis is beneficial for those who are desperate during the pandemic. Such news must end with national and international resources of suicidal crisis intervention and prevention of risk factors for suicidal behaviour. Mass media can and should instill hope for life.
Bibliografie
-
WHO (2020). Suicide. Available at: https://www.who.int/news-room/fact-sheets/detail/suicide
-
https://www.OurWorldinData.org/coronavirus
-
Hao F, Tan W, Jiang L, Zhang L, Zhao X, Zou Y, Hu Y, Luo X, Jiang X, McIntyre RS, Tran B, Sun J, Zhang Z, Ho R, Ho C, Tam W. Do psychiatric patients experience more psychiatric symptoms during COVID-19 pandemic and lockdown? A case-control study with service and research implications for immunopsychiatry. Brain, Behavior, and Immunity. 2020;87:100–106. https://doi.org/10.1016/j.bbi.2020.04.069
-
Mukaetova-Ladinska EB, Kronenberg G. Psychological and neuropsychiatric implications of COVID-19. Eur Arch Psychiatry Clin Neurosci. 2020 Nov 22;1-14. https://doi.org/10.1007/s00406-020-01210-2
-
Comtesse H, Vogel A, Kersting A, Rief W, Steil R, Rosner R. When does grief become pathological? Evaluation of the ICD-11 diagnostic proposal for prolonged grief in a treatment-seeking sample. European Journal of Psychotraumatology. 2020;11(1):1694348.
-
Sonneck G, Etzersdorfer E, Nagel-Kuess S. Imitative suicide on the Viennese subway. Soc Sci Med.1994 Feb;38(3):453-7.
Articole din ediţiile anterioare
Comorbidităţile asociate depresiei
Depresia este una dintre cauzele care duc la declin în funcţionarea socioprofesională şi la scăderea calităţii vieţii. De multe ori, depresia este ...
New psychopathologies in the digital age: orthorexia and cyberchondria
Într-o eră digitală în continuă evoluţie, preocuparea pentru sănătate a luat o nouă formă, generând noi psihopatologii, printre care şi „ortorexia...
Particularităţi ale comportamentului suicidar în tulburările depresive la tineri
În ultima perioadă, patologia psihiatrică este tot mai frecventă în rândul adolescenţilor şi al adulţilor tineri. Depresia, ideaţia suicidară, dar ...
Internările consumatorilor de droguri în spitalele de psihiatrie din România (2018-2021)
Substanţele psihoactive reprezintă o problemă importantă de sănătate publică, în special ţinând cont de trendul ascendent al numărului de cazuri di...