Conduita chirurgicală adoptată în cazul unei formaţiuni tumorale pediculate gigante prolabate din cavitatea uterină – prezentare de caz
Surgical approach adopted in the case of a giant pediculated tumor prolabated from the uterine cavity – case report
Abstract
The uterine leiomyoma is a benign mesenchymal tumor of the smooth muscle tissue of the uterus, in parallel with the proliferation of fibroconjunctive stroma, and is found in 20% of the female population aged 35-50 years old. The treatment for each patient is individual and multifactorial. Fibroids can grow anywhere in the uterus, and their size varies from microscopic to giant. Uterine fibroids can be located in different parts of the muscle cavity. Depending on the areas where growth occurs, they are classified into intramural, subserous and submucosal. The prolapsed uterine fibromatous nodule is a pedunculated submucosal fibromatous uterine nodule that migrates from the uterine cavity through the cervical canal into the vagina. This article presents the clinical case of the patient H.E., aged 45 years old, who was diagnosed and treated at the “Elena Doamna” Clinical Hospital of Obstetrics and Gynecology, from Iaşi, in the gynecology department, being diagnosed with hemorrhagic fibromatous uterus and giant uterine fibromatous node prolapsed from the uterine cavity into the vagina. This case presents difficulties in making the decision, which refers to the volume and character of the surgical intervention due to the particularity of the case. Uterine leiomyomas are the most common tumors of the female genital tract. The massive pediculated uterine fibromatous nodule prolapsed through the cervical canal is a very rare tumor and is a major diagnostic and therapeutic challenge.Keywords
leiomyomapediculated fibromatous nodulehysterectomyRezumat
Leiomiomul uterin este o tumoră benignă mezenchimală din ţesutul muscular neted al uterului, în paralel cu proliferarea stromei fibroconjunctive, şi se întâlneşte la 20% din populaţia feminină cu vârsta cuprinsă între 35 şi 50 de ani. Tratamentul pentru fiecare pacientă este individual şi multifactorial. Fibroamele pot creşte oriunde în uter, iar dimensiunea lor variază, de la microscopice la gigante. Fibromul uterin se poate localiza în diferite porţiuni ale cavităţii musculare. În funcţie de zonele unde apare excrescenţa, acestea se clasifică în intramurale, subseroase şi submucose. Nodulul fibromatos uterin prolabat este un nodul uterin fibromatos submucos pediculat care migrează din cavitatea uterină, prin canalul cervical, în vagin. În acest articol este prezentat cazul clinic al pacientei H.E., în vârstă de 45 de ani, care a fost diagnosticată şi tratată în cadrul Spitalului Clinic de Obstetrică şi Ginecologie „Elena Doamna” din Iaşi, secţia de ginecologie, cu diagnosticul de uter fibromatos hemoragic şi nodul fibromatos uterin gigant prolabat din cavitatea uterină, vaginal. Acest caz prezintă dificultăţi în luarea deciziei, care se referă la volumul şi caracterul operaţiei din cauza particularităţii cazului. Leiomioamele uterine sunt cele mai frecvente tumori ale tractului genital feminin. Nodulul fibromatos uterin pediculat masiv şi prolabat prin canalul cervical este o tumoră foarte rară şi reprezintă o mare provocare diagnostică si terapeutică.Cuvinte Cheie
leiomiomnodul fibromatos pediculathisterectomieI. Introduction
Uterine leiomyomas are smooth, benign muscle tumors of the uterus. These are found in almost half of women over the age of 40 years old; the prevalence increases during reproduction and decreases after menopause(5,6).
Originating from the myometrium, leiomyomas contain a variable percentage of fibrous tissue. The size of leiomyomas varies from microscopic to giant tumors. They are usually multiple and the fibroids can be: submucosal, intramural, subserous and/or pediculated(7).
The reason for the appearance of fibroids has not been fully clarified, but many of the studies showed that the factors involved in their development were represented by fluctuating hormone concentrations (estrogen and progesterone)(10).
Etiopathogenetically, there are several theories: hormonal theory (hyperestrogenemia); Conheim’s hereditary congenital theory; Klebs-Pillot’s vascular theory; Virchow’s infectious theory(10).
Uterine leiomyomas are often asymptomatic, but large tumors often produce abnormal genital bleeding, pelvic discomfort (pressure and pain), dysmenorrhea, infertility, pollakiuria, dysuria, constipation, “myomatous erythrocytosis syndrome” or Meigs pseudosyndrome(8).
The clinical examination (enlargement of the uterus with regular or irregular contour and firm consistency) is the initial step in the diagnosis of uterine leiomyoma(5-7).
The preferred method of visualization for the initial assessment is ultrasonography, being the least invasive and the most cost-effective. The relative echogenicity of leiomyoma depends on the correlation of the fibrous tissue with the uterine smooth muscle, the extent of degeneration and the presence of dystrophic calcification(10).
A CT scan may be required; however, leiomyoma cannot be distinguished from the healthy myometrium unless when it is calcified or necrotic(4,9).
Magnetic resonance imaging is often useful in defining the number, size and location of fibroids(4-6,9).
The treatment options include: expectant management, drug therapy (gonadotropin-releasing hormone agonists), interventional procedure (uterine artery embolization), and surgical treatment(5,6,10).
The surgical management includes myomectomy, myolysis and hysterectomy(1,10).
Myomectomy (performed by laparotomy, laparoscopy or hysteroscopy) is an option for symptomatic women who refuse a hysterectomy or who want to maintain fertility(1,10).
Hysterectomy (performed vaginally, abdominally or laparoscopically) is the definitive surgical approach(10).
The surgical approach is most commonly preferred for the management of giant leiomyoma. Intraoperatively, the patient should be positioned so as to allow adequate ventilation and to reduce compression of the vena cava. The surgical approach should allow for easy manipulation of the formation and exploration of the upper abdomen(1,2,5,10).
Myolysis (including mono or bipolar cauterization, Nd-YAG laser vaporization, or cryotherapy) is currently experimental(1,5,10).
II. The purpose of the presentation
The purpose of the presentation is to evaluate the clinical, diagnostic and treatment features of the hemorrhagic polyfibromatous uterus, but especially the surgical treatment technique chosen by us for the fibromatous uterus and the giant fibromatous pediculated nodule prolapsed from the uterine cavity, through the cervix, into the vagina.
III. Materials and method
The patient H.E., aged 45, nonsmoker, was hospitalized in the gynecology department with a personal history of irregular menstrual cycles, hypermenorrhea, fatigue, abdominal heaviness and regular moderate pain in the hypogastric region that appeared six months prior to hospitalization.
One month before the total hysterectomy surgery with bilateral adnexectomy and enucleation of the fibromatous nodule prolapsed from the uterine cavity into the vagina, there were done uterine hemostatic and biopsy curettage due to massive genital bleeding, which revealed a proliferating endometrium.
The physical examination revealed a massive, semi-mobile, hard, painful abdominal tumor that caused abdominal enlargement with hypogastric pain and initially occupied the entire lower abdominal floor (before hemostatic uterine curettage), later decreasing in volume (after hemostatic uterine curettage).
Gynecological examination: as a peculiarity of the case, there were two different gynecological examinations at one-month intervals (gynecological examination before hemostatic and biopsic uterine curettage/gynecological examination after biopsy and hemostatic uterine curettage).
Before performing biopsy and hemostatic uterine curettage, the gynecological examination revealed the existence of a giant tumor that occupied the lower abdominal floor which was hard and painful.
At the vaginal examination with the valves, we noticed massive bleeding on the external genitalia with fluid blood and clots and an elevated cervix, without lesions.
At the digital vaginal examination associated with abdominal palpation, we found the following elements: the cervix had uniform elastic consistency with open external orifice; through the lateral vaginal sac a tumor was detected, occupying the lower abdominal floor up to subumbilical level, with irregular surface, reduced mobility, hard-elastic consistency, painful and impalpable appendages due to the voluminous tumor that occupied the entire lower abdominal floor.
A biopsy and hemostatic uterine curettage were performed to stop the bleeding, treatment with vitamins and iron-based products (to reduce anemia) was administered, and the patient was scheduled for surgery one month after the curettage. The post-curettage evolution was favorable.
When the patient returned to the hospital after 30 days, when she was admitted, a new gynecological consultation was performed, which was different from the gynecological consultation performed before uterine curettage. At this second gynecological consultation performed after uterine curettage, in the vagina we noticed the existence of a pearly tumor, with a large volume (120/90 mm), that completely dilated the cervix and prolapsed in the vagina, and the initial formation that occupied the lower abdominal floor was no longer found in the abdominal cavity at the digital vaginal examination associated with the palpation of the abdominal cavity.
The abdominal formation was much diminished (70/60 mm), which led us to conclude that the uterine curettage performed for hemostatic purposes favored the migration of the giant pedunculated fibromatous nodule from the uterine cavity into the vagina through the cervix.
The laboratory tests, including serum electrolytes, liver tests, and kidney functions, were normal. Secondary anemia was detected, with hemoglobin 10.1 g/dl and hematocrit 29.33%.
Paraclinical investigations
Transabdominal ultrasound: uterus with a size of 70/60 mm, hyperechoic, inhomogeneous echostructure. Submucosal fibromatous nodule of 120/90 mm pediculated and prolapsed into the vagina through the cervix. Right ovary 39/20 mm, with a normal appearance, left ovary 49/17 mm, dystrophic. Periadnexal fluid blade: 10 mm.
The patient was informed, counseled, and the consent was obtained for surgery.
Was made a median subumbilical incision, which was extended paraumbilically to have more space for intervention.
During the laparotomy, we detected a much larger uterus with a volume of about 70/60 mm; at the level of the anterior wall towards the uterine fundus, a hard fibromatous node was found, with an irregular surface of 5/4 cm (Figure 1).
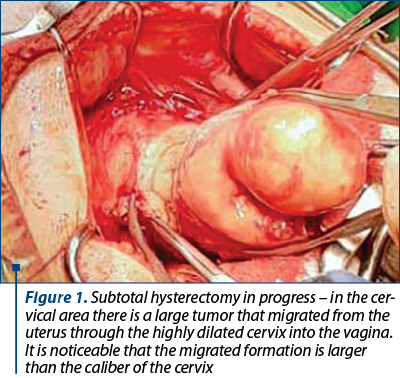
Subtotal hysterectomy and bilateral adnexectomy were performed (initially), followed by enucleation of the pedunculated nodule and totalization of the hysterectomy.
After removing the uterus, in the area of the highly dilated cervix, we detected a hard and voluminous tumor of approximately 120/90 mm, with the space of cleavage towards the cervix, a reason why the enucleation of the tumor and its vaginal extraction were performed (Figure 2).
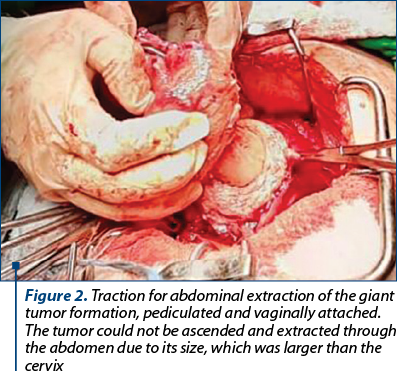
The tumor was hard, regular, of about 120/90 mm, semimobile, with space for cleavage from the cervix that allowed us to enucleate.
The prolapsed fibromatous nodule was enucleated and extracted from the cervix through the vagina with a sterile Pozzi forceps (Figures 3 and 4).
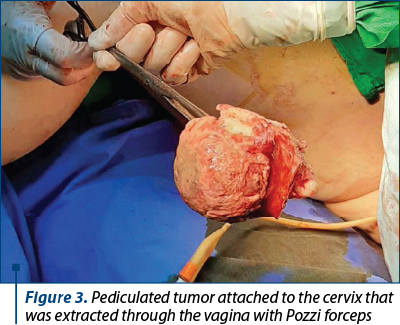
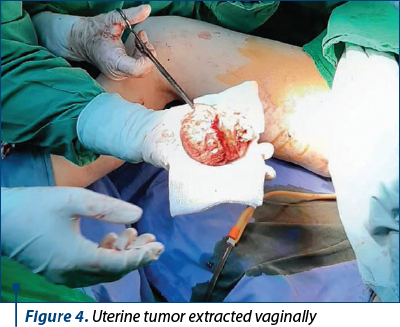
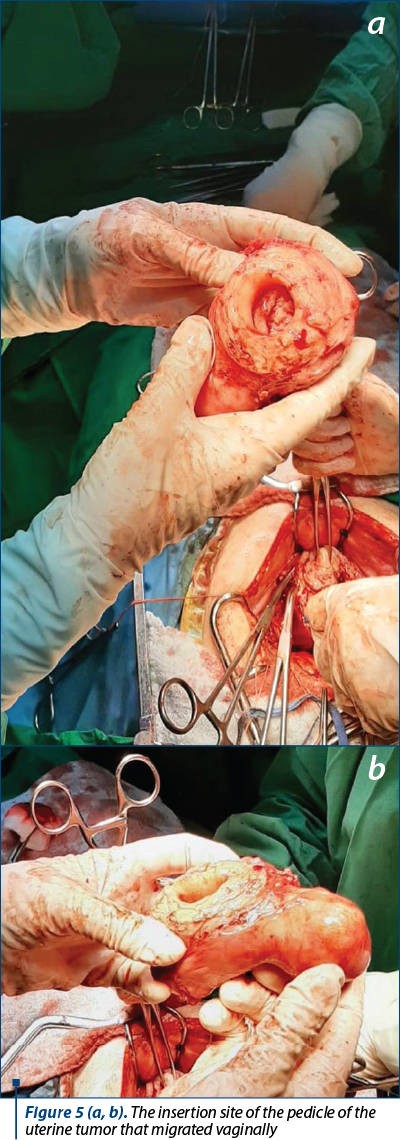
After enucleation of the cervical tumor (Figure 5), the hysterectomy was totalized.
A drainage tube was placed in the pelvis after hemostasis and was removed on the third day postoperatively. The patient was discharged on the seventh day after surgery in a stable condition with a primary scarred wound.
The patient was monitored for one month postoperatively, the evolution being favorable.
Histopathologically, we detected a leiomyoma with hyaline areas, secretory endometrium, fragments of cervix – muscle-fibrous tissue, with hemorrhagic areas, both ovaries with yellow hemorrhagic body and endometriosis, left fallopian tube – paratubal cyst. No histological signs of malignancy were detected (Figure 6).

The final histopathological diagnosis was: uterine leiomyoma, bilateral ovarian endometriosis, bilateral chronic salpingitis.
IV. Discussion
The case presented is interesting due to:
1. Difficulties in clinical diagnosis, in terms of the origin and character of the tumor (benign or malignant).
2. Difficulties in the aspect of taking decisions, which refer to the volume and character of the operation; we consider that the correct decision was taken, in the sense of performing a total hysterectomy with bilateral adnexectomy for a better quality of life of the patient (the presence of multiple and repetitive metrorrhagia with the risk of iron deficiency anemia).
3. Numerous technical difficulties can arise in the evaluation and removal of these tumors, therefore a professional was needed to properly solve the case.
4. The extremely small number of cases, especially the lack of reports in the literature, also reflects the rarity of this pathology.
5. One of the peculiarities of the case is represented by the tumor, the way the pediculated uterine tumor behaved after the biopsic and hemostatic uterine curettage and its migration from the uterine cavity through the cervix (completely dilated) to the vagina, fully occupying it.
6. Another peculiarity of the case is represented by the fact that the migrated vaginal tumor was much larger than the cervical canal, which made it impossible to elevate it from the vagina by abdominal extraction, the operating team being put in a position to take off and enucleate the giant tumor prolapsed through the cervix into the vagina through the existing cleavage space (major risk of bleeding) and to extract it vaginally.
V. Conclusions
The literature about vaginal extraction of the fibromatous nodule places a strong emphasis on the size of the fibroid as a predictor of the success of vaginal myomectomies.
Although there is no specific threshold size of the tumor, gynecological surgeons know that the surgical difficulties increase with its size.
In our opinion, the other two factors that are often ignored – the degree of mobility of the tumor in the cervical area and the surgeon’s ability to run a finger around the prolapsed tumor – are good predictors of a successful vaginal extraction, although we must not ignore the existing risk of bleeding.
The success of vaginal extraction of the pedunculated and prolapsed tumor through the cervix into the vagina not only depends on its size and the existence of the cleavage space, but also on the laxity of the remaining cervix, the risk of bleeding and the surgical skills of the surgeon.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Corton M, Cunningham F, Gala R, Hoffman B. Aspect of gynecologic surgery. In: Schorge J, et al, editors. Williams Gynecology, Ed. McGraw-Hill Companies, 2008;38-40:773-865.
- Courbiere B. Carcopino X. Fibromesuterins. In: Gynecologie Obstetrique. Ed. Vernazobres-Greco, 2006-2007:359-65.
- Grapsa D. A giant uterine leiomyoma simulating an ovarian mass in a 16-year-old girl: a case report and review of the literature. Eur J Gynaecol Oncol. 2006;27(3):294-6.
- Hadden W. Ultrasound and the use of imaging in gynecology – Uterine pathology. In: Rosevear S, Handbook of gynaecology management. Ed. Blackwell Science, 2002:173-6.
- Hoffman B. Pelvic mass. In: Schorge J, et al, Editors. Williams Gynecology, Ed. McGraw-Hill Companies, 2008;9:197-224.
- Jonas HS. Giant uterine tumors: case report and review of the literature. Obstet Gynecol. 1977;50(1 Suppl):2s-4s.
- Panayotidis C. Giant uterine leiomyomas: dilemmas in surgical management. Gynecol Surg. 2006;3:37-40.
- Van Voorhis B. A 41-year-old woman with menorrhagia, anemia, and fibroids: Review of treatment of uterine fibroids. JAMA. 2009;301(1):82-93.
- Wladimiroff J. Uterine fibroids. In: Ultrasound in obstetrics and gynaecology. Elsevier; 2009:303-6.
- Word L, Hoffman B. Surgeries for benign gynecologic conditions. In: Schorge J, et al, Editors. Williams Gynecology, Chapter 41. Ed. McGraw-Hill Companies. 2008:867-8; 905-10.





