Suplimentele dietetice în practica pediatrică – prieteni sau duşmani pentru afecţiunile hepatice?
Dietary supplements in the pediatric populations – friends or enemies in the liver disease?
Abstract
Liver pathology is one of the most challenging tasks in the pediatric population, due to the increased risk of malnutrition, which is an independent predictor of mortality and morbidity. People affected by this pathology require fat-soluble vitamins and other minerals as part of their disease management and, therefore, there is an increased consumption of dietary supplements among these patients. However, many reports showed that these supplements may interact with the levels of some prescribed drugs, such as immunosuppressants. On the one hand, recent studies have revealed that some herbal and dietary supplements have a characteristic clinical fingerprint, that may help to identify herbal and dietary supplements which induce liver injury. On the other hand, dietary supplements are known for their properties such as insulin sensitizer, antioxidant and antiinflammatory capacities, involved in several liver pathologies. Pediatricians need to be fully advised when prescribing supplements for liver disease, in order to discuss both the benefits and the risks with their patients.Keywords
liver diseasemalnutritionherbal medicinedietary supplementsRezumat
Patologia hepatică cronică implică un management de caz extins, asociind frecvent un risc crescut de malnutriţie, ceea ce reprezintă un predictor independent de mortalitate şi morbiditate la populaţia pediatrică. Pacienţii afectaţi de această patologie necesită terapie nutriţională susţinută, reprezentată de vitamine liposolubile, adaos de calorii şi minerale, acestea făcând parte din managementul ameliorării simptomatologiei bolii, explicând astfel un consum crescut de suplimente alimentare în rândul acestor pacienţi. Unele suplimente pot interacţiona cu unele medicamente, cum ar fi imunosupresoarele, iar studii recente au indicat faptul că unele suplimente alimentare pe bază de plante au o amprentă clinică specifică, ce poate ajuta la identificarea leziunilor hepatice induse de acestea. Pe de altă parte, suplimentele alimentare sunt cunoscute pentru proprietăţile lor, cum ar fi insulinosensibilizarea, capacităţi antioxidante şi antiinflamatoare, implicate în patologii hepatice severe. Medicii pediatri trebuie să fie pe deplin informaţi atunci când prescriu suplimente pentru afecţiunile hepatice, pentru a putea discuta atât despre beneficiile, cât şi despre posibilele riscuri, împreună cu pacienţii lor.Cuvinte Cheie
boli hepaticemalnutriţieremedii din plantesuplimente dieteticeIntroduction
Liver plays a key role in the anabolism, catabolism and storage of macronutrients and micronutrients. In diseased liver, the fine balance between anabolism, catabolism and storage of nutrients is heavily disturbed(1). Malnutrition affects the function and recovery of every organ system, so we can say that is a complication of cholestatic and end-stage liver diseases, which together may increase the morbidity and mortality of individual patients(2). Severe malnutrition in children can cause fatty liver which is generally fully reversible upon refeeding. In children with kwashiorkor, there seems to be a maladaptation associated with less efficient breakdown of fat and oxidation of fatty acids compared to children with marasmus. Dietary supplements are frequently administered in infants and children. Most dietary supplements used by children are not under the recommendation of a healthcare provider. It is important to mention that dietary supplements cannot be marketed for the treatment or prevention of disease; they are often taken to treat symptoms or illnesses, as well as to maintain or improve the overall health and to increase school or sports performance(3). Therefore, this review summarizes the complications caused by the liver pathology in the pediatric population and also the importance of awareness on the risks to which patients are exposed by taking dietary supplements without the consent of a specialist.
Definitions and reports
According to Food and Drug Administration (FDA), dietary supplements represent a large category of products based on herbs and botanicals, as well as their metabolites and extracts, and also vitamins, minerals and aminoacids(4). Studies from a large representative sample of children in the United States of America and Japan showed that the use of dietary supplements has been increasing in the last years(1). Vitamins and minerals are the most popular ingredients, and the main common reasons for dietary supplement use in order to improve or maintain health and to increase the school performance. In addition to vitamins and minerals, people also use non-vitamin and non-mineral supplements such as fish oil, probiotics, and herbal products, and what is concerning is that most users of dietary supplements do not consult health professionals(5). Some reports showed that the consuming of these dietary supplements can cause some adverse events, usually mild or moderate, but in some cases it has been report liver injury(6). When the parents were asked if they knew about the side effects of these products, many of them said that they didn’t know about them or that they took it as well, and that they were perfectly fine and didn’t believe these side effects truly existed(7).
Despite the excessive use of dietary supplements in the healthy pediatric population, their use should not be ignored in the pediatric population with liver disease. These patients often require fat-soluble vitamins and other minerals as part of their disease management. However, these dietary supplements may be metabolized by the liver and their use may conduct to underlying or exacerbating liver disease(1). Unfortunately, patients often fail to disclose their use with their healthcare providers and sometimes they are rushed to the hospital due to the side effects caused by them.
Dietary supplements in pediatric population
Dietary supplements use is widespread amongst the general population, including in children and adolescents, and has been increasing worldwide. They come in a variety of forms, including tablets, capsules, gummies and powders, as well as drinks and energy bars. Popular supplements include multivitamins like vitamins B12, D and C and minerals like calcium and iron. Also, herbs such as Echinacea, green tea and garlic are very popular.
The most recently released data from the National Health and Nutrition Examination Survey (NHANES) during 2017-2018 were used to estimate the prevalence of use among U.S. children and adolescents of any dietary supplement, of two or more dietary supplements, and specific dietary supplement product types(5). The trends were calculated for dietary supplement use from 2009-2010 to 2017-2018. During 2017-2018, 34% of children and adolescents used any dietary supplement in the past 30 days, with no significant change since 2009-2010. The use of two or more dietary supplements increased from 4.3% during 2009-2010 to 7.1% during 2017-2018. Multivitamin-mineral products were used by 23.8% of children and adolescents, making these the most commonly used products(5).
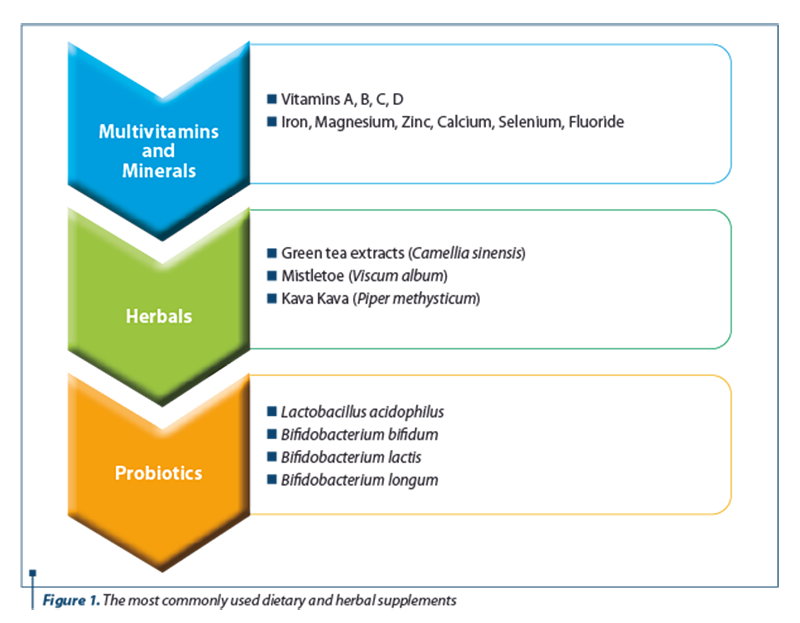
A study commissioned by the Food and Drug Administration estimated that the Food and Drug Administration is notified of less than 1% of all adverse events associated with dietary supplements(5). A summary of the most used liver supplements is shown in Figure 1.
Vitamin A is a fat-soluble vitamin which has two forms/source options for the human diet: retinoids or preformed vitamin A, and carotenoids or provitamin A. It is useful for the immune system function, fertility and is also an antioxidant. It is also involved in healthy vision, including low light vision – the formation of rhodopsin.
Vitamin B group is represented by a diversity of substances: B1 (thiamine), B2 (riboflavin), B3 (niacin), B5 (pantothenic acid), B6 (pyridoxine), B7 (biotin), B9 (folic acid or folate) and B12 (cobalamin). As a collective, the B vitamins provide energy and can help the body through short bursts of stress. The metabolism of macronutrients is also a key activity for this group, with the additional benefits for the following: B6 aids in blood, central nervous system and skin metabolism, in the synthesis of heme (iron) and nucleic acid; B9 is useful for red blood cells, the development of the foetal nervous system (in pregnancy); B12 is useful in the formation of normal red blood cells.
Vitamin C is a water-soluble vitamin that the human body cannot synthesis. It is involved in a large number of biological processes: collagen synthesis for skin, joints and bones and also in anti-aging, in healing (it speeds up wound healing), red blood cell formation and for preventing bleeding, at the level of the immune system it helps the white blood cell activity, it is a natural antihistamine, and offers free radical protection.
Vitamin D is a fat-soluble vitamin essential for bone health, calcium absorption and blood clotting. It has two important forms for humans: vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol). Vitamin D helps the bones and muscle function and in general health.
Iron is an important mineral which is found in the body in the hemoglobin of the red cells and in the myoglobin of muscle cells. It is needed for transporting oxygen and carbon dioxide.
Magnesium is a mineral which contributes to the metabolism of aminoacids, cholesterol, glucose and carbohydrates. The potential health benefits of this mineral are: it provides antioxidants, it supports bone health associated with other nutrients, such as calcium and vitamin D, it reduce blood sugar and inflammation.
Calcium is a mineral which is an essential part of bones and teeth. The heart, nerves and blood-clotting systems also need calcium to work. It is also used in muscle cramps, osteoporosis, rickets and osteomalacia.
Zinc is considered an essential mineral because of its role in the immune system. It is required for numerous processes, including gene expression, enzymatic reactions, protein synthesis, DNA synthesis, wound healing, growth and development.
Selenium is a mineral with many antioxidant properties.
Green tea extracts are made from the Camellia sinensis plant. It can promote blood sugar regulation, it reduces blood fat levels and improves brain health. It is also used for weight loss.
Kava kava is used as a ceremonial drink to promote a state of relaxation. It has been shown that consuming kava kava may reduce anxiety, protect neurons from damage and reduce pain sensations.
Probiotics are healthful strains of live bacteria and yeast. Studies suggest that consuming probiotics can provide more beneficial bacteria, which may help restore the balance of the gut microbiota. The most common are Bifidobacterium and Lactobacillus bacteria.
Dietary supplements in pediatric non-alcoholic fatty liver disease
Now and in the near future, non-alcoholic fatty liver disease will be the most common chronic liver disease in children. Due to lack of exercise, physical activity and the consumption of fast-food, sweets and snacks, children risk of becoming overweight, up to obesity(8). As we know, obesity is associated with an increased risk of non-alcoholic fatty liver through different mechanisms, such as intensification of insulin resistance and increased levels of inflammatory markers. Unfortunately, there is no specific treatment approved for this pathology, the only strategy approved being lifestyle change. However, recent studies have shown that dietary supplements play an important role in pediatric management through insulin sensitizer, antioxidant and antiinflammatory properties(9).
For example, it seems that omega-3 fatty acids supplementation has beneficial effects on pediatric non-alcoholic fatty liver disease, through its antiinflammatory and insulin sensitizer effects. Also, several studies showed that vitamin E could significantly reduce the ALT levels at weeks 24 and 48, and on the other hand, it significantly improves the histopathological characteristics of the disease at week 96(1).
It is worth mentioning that the effects of probiotics and prebiotics have been studied for some time and the researchers came to the conclusions that probiotics can modify some risk factors, such as insulin resistance, liver fat and oxidative stress, while prebiotics such as lactulose and galacto-oligosaccharides can promote the growth of certain intestinal bacteria such as Lactobacillus and downregulate the levels of inflammatory factors. Further studies should be conducted to find the best combination of probiotics and prebiotics for achieving the best results from supplementation(10).
In the end, we must not forget to mention the herbal medicines which have been used in the traditional medicine, such as cinnamon, curcumin and ginger. They can improve the insulin sensitivity and lipid profile and are proposed for the treatment of non-alcoholic fatty liver disease, but studies have not been conducted to examine the effects of these supplements on the pediatric population. Also, in this category, we have polyphenols, which are plant-derived compounds with important antiinflammatory and antioxidant properties. For exemplification, we have the most important member of the polyphenols family: resveratrol. The supplementation with resveratrol has been shown to be useful in the reduction of the disease severity, attenuating hepatic steatosis and reducing the level of liver enzymes and inflammatory cytokines(10).
Supplements for malnutrition
Malnutrition is a common complication of cholestatic and end-stage liver diseases. Nutrition support is a key aspect of the management of these patients, as it has an impact on their quality of life, on morbidity and mortality. Malnutrition may be caused initially by maldigestion and malabsorption of nutrients, along with an increased metabolic demand. The pathophysiology of malnutrition seen in chronic and end-stage liver disease is very complex and the main causes for malnutrition in liver disease are: increased nutritional requirement due to increased resting energy expenditure and total energy expenditure, bile salts are required to activate lipase, and in their absence (as in chronic cholestasis), a large proportion of fat is excreted and unabsorbed, decreased nutritional intake due to early satiety, nausea and vomiting, decreased absorption due to intestinal mucosal oedema secondary to portal hypertension(1).
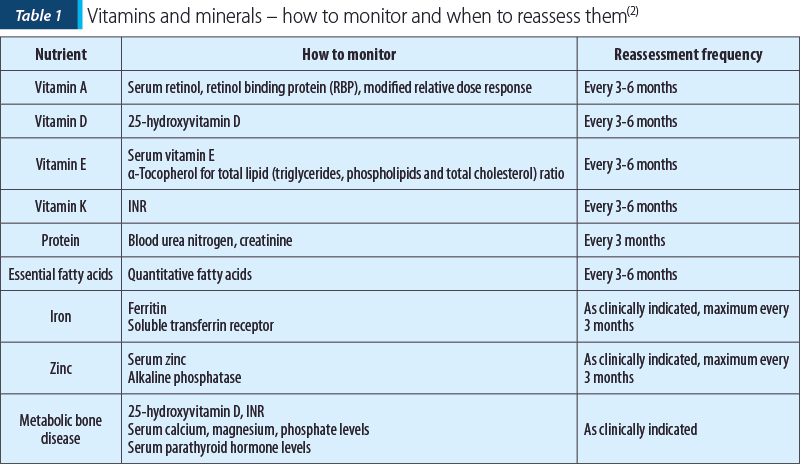
This is why children with chronic cholestatic and/or end-stage liver disease must be observed closely by the specialist to identify nutritional deficiencies early and to initiate nutritional interventions to both optimize the appropriate development and prevent further complications. These patients have a huge deficiency in proteins, vitamins, minerals and essential fatty acids and this is why they should be screened for nutritional deficiencies.
Over-the-counter dietary supplements
Patients with chronic liver disease frequently take dietary supplements which can react with the levels of prescribed drugs and often fail to disclose their use with their specialists. A study showed that only about one-third of adult liver transplant patients who use supplements consulted with their medical team regarding their use(11).
Because of the irrational use of herbal and dietary supplements on the long term, a study showed that, from 2408 adult cases, 625 were characterized as a drug-induced liver injury and 21 were produced after taking dietary supplements and herbs. This was due to the recent outbreak of acute liver failure caused by herbal/dietary supplements in Hawaii patients who underwent emergency liver transplantation in the United States(12).
Conclusions
Dietary supplements can also bring benefits, as well as serious side effects. On the bright side, they play a pivotal role in pediatric management through insulin sensitizer, antioxidant and antiinflammatory properties. They are important in the management of malnutrition, the supplementation of micronutrient deficiencies, including fat-soluble vitamins, and may prevent the further complications of the disease. On the other hand, if they are taken without the recommendation of the specialist, they can produce adverse reactions, such as liver injury, which can cause acute liver failure, leading to liver transplantation. We must remember that the most commonly involved products include bodybuilding and weight loss products, and that some herbal products do have a clear clinical signature that can make the diagnosis almost certain. In the future, we hope to publish as many studies and researches on these supplements in order to be able to establish concretely to whom, when and under what conditions we can grant them.
Bibliografie
-
Korotkaya Y, Conner K, Lau J, Mullin G, Harpavat S, Miloh T, et al. Use of Dietary Supplements in Pediatric Liver Disease and Transplantation. J Pediatr Gastroenterol Nutr. 2021 Jan 1;72(1):e10-e14.
-
Mouzaki M, Bronsky J, Gupte G, Hojsak I, Jahnel J, Pai N, et al. Nutrition Support of Children With Chronic Liver Diseases: A Joint Position Paper of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition and the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition. J Pediatr Gastroenterol Nutr. 2019 Oct;69(4):498-511.
-
Agostoni C, Esposito S, Nobili A. Dietary supplements in infants and children: only beneficial? Journal of Pediatric Gastroenterology and Nutrition. 2016 Aug;63(Issue 2):177-180.
-
Commissioner of the Food and Drug Administration. August 16, 2019. Dietary Supplements. https://www.fda.gov/food/dietary-supplements.
-
Gardiner P, Buettner C, Davis RB, et al. Factors and common conditions associated with adolescent dietary supplement use: an analysis of the National Health and Nutrition Examination Survey (NHANES). BMC Complement Altern Med. 2008 Mar 31;8(1):9.
-
Hillman L, Gottfried M, Whitsett M, et al. Clinical features and outcomes of complementary and alternative medicine induced acute liver failure and injury. Am J Gastroenterol. 2016;111:958–65.
-
de Boer YS, Sherker AH. Herbal and dietary supplement induced liver injury. Clin Liver Dis. 2017 Feb;21(1):135-49.
-
McCullough AJ. The clinical features, diagnosis and natural history of nonalcoholic fatty liver disease. Clin Liver Dis. 2004 Aug;8(3):521-533.
-
Rahimlou M, Ahmadnia H, Hekmatdoost A. Dietary supplements and pediatric non-alcoholic fatty liver disease: Present and the future. World J Hepatol. 2015; 7(25):2597–602.
-
Kobayashi E, Sato Y, Nishijima C, et al. Concomitant use of dietary supplements and medicines among preschool and school-aged children in Japan. Nutrients. 2019 Dec 4;11(12):2960.
-
Neff WG, O’Brien C, Montalnono M, DeManno A, Kahn S, et al. Consumption of dietary supplements in a liver transplant population. Liver Transplantation. 2004;10(7):881-885.
-
Wong LL, Lacar L, Roytman M, Orloff SL. Urgent Liver Transplantation for Dietary Supplements: An Under-Recognized Problem. Transplant Proc. 2017 Mar;49(2):322-325.